Abstract
Purpose
Leptomeningeal collaterals play a pivotal role in acute ischemic stroke. While most collateral scores rely on subjective visual analysis, an objective quantification is possible using dynamic computed tomography (CT) angiography (dynCTA). The aim was to determine the value of collateral filling delay (CFD) as assessed by dynCTA for predicting subacute stroke complications.
Methods
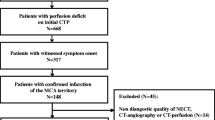
All subjects with isolated prebifurcation middle cerebral artery M1 occlusions were selected from an initial cohort of 2635 patients who underwent multiparametric CT for suspected stroke. The CFD was defined as the difference in time to peak enhancement between M2 segments of both hemispheres. Logistic regression analysis of CFD for space-occupying infarction (≥5 mm shift of brain tissue over the midline), parenchymal hematoma, and hemorrhagic transformation on follow-up imaging was performed.
Results
In this study 78 patients (47 female, median age 74 years) were included. The median CFD was 6.31 s (interquartile range [IQR] 4.00–8.64). The CFD values were correlated with qualitative collateral scores (p < 0.05). Higher CFD was associated with the development of space-occupying infarction in univariable (odds ratio, OR = 1.28; p = 0.002) and multivariable regression analysis (OR = 1.48; p = 0.004). The CFD had no association with parenchymal hematoma or hemorrhagic transformation (p > 0.05).
Conclusion
A high CFD may serve as reproducible measure for collateralization and indicate development of increased risk of space-occupying infarction.



Similar content being viewed by others

References
Balami JS, Chen RL, Grunwald IQ, Buchan AM. Neurological complications of acute ischaemic stroke. Lancet Neurol. 2011;10:357–71.
Vahedi K, Hofmeijer J, Juettler E, Vicaut E, George B, Algra A, Amelink GJ, Schmiedeck P, Schwab S, Rothwell PM, Bousser MG, van der Worp HB, Hacke W; DECIMAL, DESTINY, and HAMLET investigators. Early decompressive surgery in malignant infarction of the middle cerebral artery: a pooled analysis of three randomised controlled trials. Lancet Neurol. 2007;6:215–22.
Krieger DW, Demchuk AM, Kasner SE, Jauss M, Hantson L. Early clinical and radiological predictors of fatal brain swelling in ischemic stroke. Stroke. 1999;30:287–92.
Menon BK, Qazi E, Nambiar V, Foster LD, Yeatts SD, Liebeskind D, Jovin TG, Goyal M, Hill MD, Tomsick TA, Broderick JP, Demchuk AM; Interventional Management of Stroke III Investigators. Differential effect of baseline computed tomographic angiography collaterals on clinical outcome in patients enrolled in the Interventional Management of Stroke III trial. Stroke. 2015;46:1239–44.
van den Wijngaard IR, Boiten J, Holswilder G, Algra A, Dippel DW, Velthuis BK, Wermer MJ, van Walderveen MA. Impact of collateral status evaluated by dynamic computed tomographic angiography on clinical outcome in patients with ischemic stroke. Stroke. 2015;46:3398–404.
Tan IY, Demchuk AM, Hopyan J, Zhang L, Gladstone D, Wong K, Martin M, Symons SP, Fox AJ, Aviv RI. CT angiography clot burden score and collateral score: correlation with clinical and radiologic outcomes in acute middle cerebral artery infarct. AJNR Am J Neuroradiol. 2009;30:525–31.
Menon BK, d’Esterre CD, Qazi EM, Almekhlafi M, Hahn L, Demchuk AM, Goyal M. Multiphase CT angiography: a new tool for the imaging triage of patients with acute Ischemic stroke. Radiology. 2015;275:510–20.
Martinon E, Lefevre PH, Thouant P, Osseby GV, Ricolfi F, Chavent A. Collateral circulation in acute stroke: assessing methods and impact: a literature review. J Neuroradiol. 2014;41:97–107.
Beyer SE, von Baumgarten L, Thierfelder KM, Rottenkolber M, Janssen H, Dichgans M, Johnson TR, Straube A, Ertl-Wagner B, Reiser MF, Sommer WH. Predictive value of the velocity of collateral filling in patients with acute ischemic stroke. J Cereb Blood Flow Metab. 2015;35:206–12.
Horsch AD, Dankbaar JW, Stemerdink TA, Bennink E, van Seeters T, Kappelle LJ, Hofmeijer J, de Jong HW, van der Graaf Y, Velthuis BK; DUST investigators. Imaging findings associated with space-occupying edema in patients with large middle cerebral artery infarcts. AJNR Am J Neuroradiol. 2016;37:831–7.
Berger C, Fiorelli M, Steiner T, Schäbitz WR, Bozzao L, Bluhmki E, Hacke W, von Kummer R. Hemorrhagic transformation of ischemic brain tissue: asymptomatic or symptomatic? Stroke. 2001;32:1330–5.
R Development Core Team, R Core Team. R: a language and environment for statistical computing. Vienna; 2008. Available online at https://www.R-project.org/.
Kovács P, Petres T, Tóth L. A new measure of multicollinearity in linear regression models. Int Stat Rev. 2005;73:405–12.
Hacke W, Schwab S, Horn M, Spranger M, De Georgia M, Von Kummer R. ‘Malignant’middle cerebral artery territory infarction: clinical course and prognostic signs. Arch Neurol. 1996;53:309–15.
Berrouschot J, Sterker M, Bettin S, Köster J, Schneider D. Mortality of space-occupying (‘malignant’) middle cerebral artery infarction under conservative intensive care. Intensive Care Med. 1998;24:620.
Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, Biller J, Brown M, Demaerschalk BM, Hoh B, Jauch EC, Kidwell CS, Leslie-Mazwi TM, Ovbiagele B, Scott PA, Sheth KN, Southerland AM, Summers DV, Tirschwell DL; American Heart Association Stroke Council. 2018 guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American stroke association. Stroke. 2018;49:e46-110.
Hom J, Dankbaar JW, Soares BP, Schneider T, Cheng SC, Bredno J, Lau BC, Smith W, Dillon WP, Wintermark M. Blood-brain barrier permeability assessed by perfusion ct predicts symptomatic hemorrhagic transformation and malignant edema in acute ischemic stroke. AJNR Am J Neuroradiol. 2011;32:41–8.
Heiss WD. Malignant MCA infarction: pathophysiology and imaging for early diagnosis and management decisions. Cerebrovasc Dis. 2016;41:1–7.
Campbell BC, Christensen S, Tress BM, Churilov L, Desmond PM, Parsons MW, Barber PA, Levi CR, Bladin C, Donnan GA, Davis SM; EPITHET Investigators. Failure of collateral blood flow is associated with infarct growth in ischemic stroke. J Cereb Blood Flow Metab. 2013;33:1168–72.
Tong E, Patrie J, Tong S, Evans A, Michel P, Eskandari A, Wintermark M. Time-resolved CT assessment of collaterals as imaging biomarkers to predict clinical outcomes in acute ischemic stroke. Neuroradiology. 2017;59:1101–9.
Maas MB, Lev MH, Ay H, Singhal AB, Greer DM, Smith WS, Harris GJ, Halpern E, Kemmling A, Koroshetz WJ, Furie KL. Collateral vessels on CT angiography predict outcome in acute ischemic stroke. Stroke. 2009;40:3001–5.
Menon BK, O’Brien B, Bivard A, Spratt NJ, Demchuk AM, Miteff F, Lu X, Levi C, Parsons MW. Assessment of leptomeningeal collaterals using dynamic CT angiography in patients with acute ischemic stroke. J Cereb Blood Flow Metab. 2013;33:365–71.
Agarwal S, Bivard A, Warburton E, Parsons M, Levi C. Collateral response modulates the time–penumbra relationship in proximal arterial occlusions. Baillieres Clin Neurol. 2018;90:e316–22.
Irvine HJ, Ostwaldt AC, Bevers MB, Dixon S, Battey TW, Campbell BC, Davis SM, Donnan GA, Sheth KN, Jahan R, Saver JL, Kidwell CS, Kimberly WT. Reperfusion after ischemic stroke is associated with reduced brain edema. J Cereb Blood Flow Metab. 2018;38:1807-17.
Kimberly WT, Dutra BG, Boers AMM, Alves HCBR, Berkhemer OA, van den Berg L, Sheth KN, Roos YBWEM, van der Lugt A, Beenen LFM, Dippel DWJ, van Zwam WH, van Oostenbrugge RJ, Lingsma HF, Marquering H, Majoie CBLM; MR CLEAN Investigators. Association of reperfusion with brain edema in patients with acute ischemic stroke. JAMA Neurol. 2018;75:453-61.
Berkhemer OA, Jansen IG, Beumer D, Fransen PS, van den Berg LA, Yoo AJ, Lingsma HF, Sprengers ME, Jenniskens SF, Lycklama À, Nijeholt GJ, van Walderveen MA, van den Berg R, Bot JC, Beenen LF, Boers AM, Slump CH, Roos YB, van Oostenbrugge RJ, Dippel DW, van der Lugt A, van Zwam WH, Marquering HA, Majoie CB; MR CLEAN Investigators. Collateral status on baseline computed tomographic angiography and intra-arterial treatment effect in patients with proximal anterior circulation stroke. Stroke. 2016;47:768–76.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
M.F. Froelich, K.M. Thierfelder, L.T. Rotkopf, M.P. Fabritius, L. Kellert, S. Tiedt, W.H. Sommer, F.A. Wollenweber, F. Dorn, T. Liebig, P. Reidler and W.G. Kunz declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Froelich, M.F., Thierfelder, K.M., Rotkopf, L.T. et al. Impact of Collateral Filling Delay on the Development of Subacute Complications After Acute Ischemic Stroke. Clin Neuroradiol 30, 331–337 (2020). https://doi.org/10.1007/s00062-019-00760-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00062-019-00760-w