Abstract
Objective
Previous research has indicated a relation between obsessive–compulsive disorder (OCD), childhood traumatic experiences and higher levels of dissociation that appears to relate to negative treatment outcome for OCD. The aim of the present study is to investigate whether childhood trauma and dissociation are related to severity of OCD in adulthood. We also intend to examine the association between treatment resistance, dissociation, and each form of trauma.
Methods
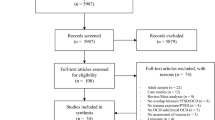
Participants included 120 individuals diagnosed with OCD; 58 (48.3 %) of them met the criteria for treatment-resistant OCD (resistant group), whereas the other 62 (51.7 %) were labeled as responder group. The intensity of obsessions and compulsions was evaluated using Yale-brown obsessive–compulsive scale (Y-BOCS). All patients were assessed with the traumatic experiences checklist, dissociative experiences scale, beck depression inventory, and beck anxiety inventory.
Results
Controlling for clinical variables, resistant group had significantly higher general OCD severity, anxiety, depression, trauma, and dissociation scores than the responders. Correlation analyses indicated that Y-BOCS scores were significantly related to severity of dissociation, anxiety, depression, and traumatic experiences. In a logistic regression analysis with treatment resistance as a dependent variable, high dissociation levels, long duration of illness, and poor insight emerged as relevant predictors, but gender, levels of anxiety, depression, and traumatic experiences did not.
Conclusions
Our results suggest that dissociation may be a predictor of poorer treatment outcome in patients with OCD; therefore, a better understanding of the mechanisms that underlie this phenomenon may be useful. Future longitudinal studies are warranted to verify if this variable represents predictive factors of treatment non-response.
Similar content being viewed by others
References
Husted DS, Shapira NA (2004) A review of the treatment for refractory obsessive-compulsive disorder: from medicine to deep brain stimulation. CNS Spectr 9:833–847
Bloch MH, Landeros-Weisenberger A, Kelmendi B, Coric V, Bracken MB, Leckman JF (2006) A systematic review: antipsychotic augmentation with treatment refractory obsessive-compulsive disorder. Mol Psychiatry 11:622–632
Goodman WK, Ward HE, Kablinger AS, Murphy TK (2000) Biological approaches to treatment-resistant obsessive-compulsive disorder. In: Goodman WK, Rudorfer MV, Maser JD (eds) Obsessive-compulsive disorder: contemporary issues in management. Lawrence Erlbaum Associates, London, pp 333–369
Ravizza L, Barzega G, Bellino S, Bogetto F, Maina G (1995) Predictors of drug treatment response in obsessive-compulsive disorder. J Clin Psychiatry 56:368–373
Shetti CN, Reddy YC, Kandavel T, Kashyap K, Singisetti S, Hiremath AS, Siddequehusen MU, Raghunandanan S (2005) Clinical predictors of drug nonresponse in obsessive-compulsive disorder. J Clin Psychiatry 66:1517–1523
Pigott TA, Seay S (1997) Pharmacotherapy of obsessive-compulsive disorder. Int Rev Psychiatry 9:133–147
Hantouche EG, Bouhassira M, Lancrenon S (2000) Prospective follow-up over a 12 month period of a cohort of 155 patients with obsessive-compulsive disorder: phase III National DRT-TOC Study. Encephale 26:73–83
Alonso P, Menchon JM, Pifarre J, Mataix-Cols D, Torres L, Salgado P, Vallejo J (2001) Long-term follow-up and predictors of clinical outcome in obsessive-compulsive patients treated with serotonin reuptake inhibitors and behavioral therapy. J Clin Psychiatry 62:535–540
Lochner C, duToit PL, Zungu-Dirwayi N, Marais A, vanKradenburg J, Seedat S, Niehaus DJH, Stein DJ (2002) Childhood trauma in obsessive-compulsive disorder, trichotillomania, and controls. Depress Anxiety 15:66–68
Burnam MA, Stein JA, Golding JM, Siegel JM, Sorenson SB, Forsythe AB (1988) Sexual assault and mental disorders in a community population. J Consult Clin Psychol 56:843–850
Caspi A, Vishne T, Sasson Y, Gross R, Livne A, Zohar J (2008) Relationship between childhood sexual abuse and obsessive-compulsive disorder: case control study. Isr J Psychiatry Rel Sci 45:177–182
Gershuny BS, Baer L, Wilson KA, Radomsky AS, Jenike MA (2003) Connections among symptoms of obsessive-compulsive disorder and posttraumatic stress disorder: a case series. Behav Res Ther 41:1029–1041
Pitman RK (1993) Posttraumatic obsessive-compulsive disorder: a case study. Compr Psychiatry 34:102–107
Gershuny BS, Baer L, Parker H, Gentes EL, Infield AL, Jenike MA (2008) Trauma and posttraumatic stress disorder in treatment-resistant obsessive-compulsive disorder. Depress Anxiety 25:69–71
Goff DC, Olin JA, Jenike MA, Baer L, Buttolph ML (1992) Dissociative symptoms in patients with obsessive-compulsive disorder. J Nerv Ment Dis 180:332–337
Praško J, Raszka M, Adamcová K, Grambal A, Kopřivová J, Kudrnovská H, Látalová K, Vyskočilová J (2009) Predicting the therapeutic response to cognitive behavioural therapy in patients with pharmacoresistant obsessive-compulsive disorder. Neuroendocrinol Lett 30:615–623
Draijer N, Langeland W (1999) Childhood trauma and perceived parental dysfunction in the etiology of dissociative symptoms in psychiatric inpatients. Am J Psychiatry 156:379–385
Lochner C, Seedat S, Hemmings SM, Kinnear CF, Corfield VA, Niehaus DJ, Moolman-Smook JC, Stein DJ (2004) Dissociative experiences in obsessive-compulsive disorder and trichotillomania: clinical and genetic findings. Compr Psychiatry 45:384–391
Lochner C, Seedat S, Hemmings SM, Moolman-Smook JC, Kidd M, Stein DJ (2007) Investigating the possible effects of trauma experiences and 5-HTT on the dissociative experiences of patients with OCD using path analysis and multiple regression. Neuropsychobiology 56:6–13
Rufer M, Held D, Cremer J, Fricke S, Moritz S, Peter H, Hand I (2006) Dissociation as a predictor of cognitive behavior therapy outcome in patients with obsessive-compulsive disorder. Psychother Psychosom 75:40–46
First MB, Spitzer RL, Gibbon M, Williams JBW (1997) Structured clinical interview for DSM-IV Axis I disorders: clinical version (SCIDCV). American Psychiatric Press, Washington, DC
Goodman WK, Price LH, Rasmussen SA, Mazure C, Fleischmann RL, Hill CL, Heninger GR, Charney DS (1989) The Yale-brown obsessive-compulsive scale I: development, use, and reliability. Arch Gen Psychiatry 46:1006–1011
Tek C, Ulug B, Rezaki BG, Tanrivedi N, Mercan S, Demir B, Vargel S (1995) Yale-brown obsessive compulsive scale and US national institute of mental health global obsessive compulsive scale in Turkish: reliability and validity. Acta Psychiatr Scand 91:410–413
Nijenhuis ERS, Van der Hart O, Kruger K (2002) The psychometric characteristics of the traumatic experiences questionnaire (TEC): first findings among psychiatric outpatients. Clin Psychol Psychother 9:200–210
Semiz UB, Basoglu C, Ebrinc C, Ergun BM, Noyan CO, Cetin M (2005) Body dysmorphic disorder, trauma, and dissociation in patients with borderline personality disorder: a preliminary study. Bull Clin Psychopharmacol 15:65–70
Hisli N (1989) Reliability and validity of BECK depression inventory among university students. J Turk Psychol 7:3–13 (in Turkish)
Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J (1961) An inventory for measuring depression. Arch Gen Psychiatry 4:561–571
Beck AT, Epstein N, Brown G, Steer RA (1988) An inventory for measuring clinical anxiety: psychometric properties. J Consult Clin Psychol 56:893–897
Ulusoy M, Erkmen H, Sahin N (1998) Turkish version of the beck anxiety inventory: psychometric properties. J Cogn Psychother 12:163–172
Yargic LI, Tutkun H, Sar V (1995) The reliability and validity of the Turkish version of the dissociative experiences scale. Dissociation 8:10–13
Bernstein EM, Putnam FW (1986) Development, reliability, and validity of a dissociation scale. J Nerv Ment Dis 174:727–735
Mathews CA, Kaur N, Stein MB (2008) Childhood trauma and obsessive-compulsive symptoms. Depress Anxiety 25:742–751
Briggs ES, Price IR (2009) The relationship between adverse childhood experience and obsessive-compulsive symptoms and beliefs: the role of anxiety, depression and experiential avoidance. J Anxiety Disord 23:1037–1046
Cromer KR, Schmidt NB, Murphy DL (2006) An investigation of traumatic life events and obsessive-compulsive disorder. Behav Res Ther 4:1683–1691
Carpenter L, Chung MC (2011) Childhood trauma in obsessive compulsive disorder: the roles of alexithymia and attachment. Psychol Psychother 84:367–388
Gershuny BS, Baer L, Jenike MA, Minichiello WE, Wilhelm S (2002) Comorbid posttraumatic stress disorder: impact on treatment outcome for obsessive-compulsive disorder. Am J Psychiatry 159:852–854
Selvi Y, Besiroglu L, Aydin A, Gulec M, Atli A, Boysan M, Celik C (2012) Relations between childhood traumatic experiences, dissociation, and cognitive models in obsessive compulsive disorder. Int J Psychiatry Clin Pract 16:53–59
Michelson L, June K, Vives A, Testa S, Marchione N (1998) The role of trauma and dissociation in cognitive-behavioral psychotherapy outcome and maintenance for panic disorder with agoraphobia. Behav Res Ther 36:1011–1050
Spitzer C, Barnow S, Freyberger HJ, Grabe HJ (2007) Dissociation predicts symptom-related treatment outcome in short-term inpatient psychotherapy. Aust N Z J Psychiatry 41:682–687
Fontenelle LF, Domingues AM, Souza WF, Mendlowicz MV, de Menezes GB, Figueira IL, Versiani M (2007) History of trauma and dissociative symptoms among patients with obsessive-compulsive disorder and social anxiety disorder. Psychiatr Q 78:241–250
Ball S, Robinson A, Shekhar A, Walsh K (1997) Dissociative symptoms in panic disorder. J Nerv Ment Dis 185:755–760
Lipinski JF Jr, Pope HG Jr (1994) Do “flashbacks” represent obsessional imagery? Compr Psychiatry 35:245–247
Grabe HJ, Goldschmidt F, Lehmkuhl L, Gänsicke M, Spitzer C, Freyberger HJ (1999) Dissociative symptoms in obsessive-compulsive dimensions. Psychopathology 32:319–324
Kluft RP (1993) Multiple personality disorder. In: Spiegel DA (ed) Dissociative disorders: a clinical review. Sidran Press, Lutherville, pp 17–44
McNevin SH, Rivera M (2001) Obsessive compulsive spectrum disorders in individuals with dissociative disorders. J Trauma Dissociation 2:117–131
Ross CA, Anderson G (1988) Phenomenological overlap of multiple personality disorder and obsessive compulsive disorder. J Nerv Ment Dis 176:295–299
Belli H, Ural C, Vardar MK, Yesılyurt S, Oncu F (2012) Dissociative symptoms and dissociative disorder comorbidity in patients with obsessive-compulsive disorder. Compr Psychiatry 53:975–980
Medford N, Sierra M, Baker D, David AS (2005) Understanding and treating depersonalisation disorder. Adv Psychiatr Treat 11:92–100
Hollander E, Benzaquen SD (1997) The obsessive-compulsive spectrum disorders. Int Rev Psychiatry 9:99–110
Hollander E, Carrasco JL, Mullen LS, Trungold S, De-Caria CM, Towey J (1992) Left hemispheric activation in depersonalization disorder: a case report. Biol Psychiatry 31:1157–1162
Pica M, Beere D, Maurer L (1997) The overlap between dissociative and obsessive-compulsive disorders: a theoretical link. Dissociation 10:38–43
West M, Adam K, Spreng S, Rose S (2001) Attachment disorganization and dissociative symptoms in clinically treated adolescents. Can J Psychiatry 46:627–631
Meyer B, Pilkonis PA, Proietti JM, Heape CL, Egan M (2001) Attachment styles and personality disorders as predictors of symptom course. J Pers Disord 15:371–389
Saxena S, Maidment KM, Vapnik T, Golden G, Rishwain T, Rosen RM, Tarlow G, Bystritsky A (2002) Obsessive-compulsive hoarding: symptom severity and response to multimodal treatment. J Clin Psychiatry 63:21–27
Eisen JL, Rasmussen SA, Phillips KA, Price LH, Davidson J, Lydiard RB, Ninan P, Piggott T (2001) Insight and treatment outcome in obsessive-compulsive disorder. Compr Psychiatry 42:494–497
Hardt J, Rutter M (2004) Validity of adult retrospective reports of adverse childhood experiences: review of the evidence. J Child Psychol Psychiatry 45:260–273
Sar V, Akyuz G, Kugu N, Ozturk E, Ertem-Vehid H (2006) Axis I dissociative disorder comorbidity in borderline personality disorder and reports of childhood trauma. J Clin Psychiatry 10:1583–1590
Conflict of interest
On behalf of all the authors, the corresponding author states that there is no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Semiz, U.B., Inanc, L. & Bezgin, C.H. Are trauma and dissociation related to treatment resistance in patients with obsessive–compulsive disorder?. Soc Psychiatry Psychiatr Epidemiol 49, 1287–1296 (2014). https://doi.org/10.1007/s00127-013-0787-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-013-0787-7