Abstract
Purpose
This study aimed to develop and validate machine-learning models for the prediction of recurrent infection in patients following revision total knee arthroplasty for periprosthetic joint infection.
Methods
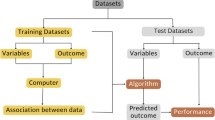
A total of 618 consecutive patients underwent revision total knee arthroplasty for periprosthetic joint infection. The patient cohort included 165 patients with confirmed recurrent periprosthetic joint infection (PJI). Potential risk factors including patient demographics and surgical characteristics served as input to three machine-learning models which were developed to predict recurrent periprosthetic joint. The machine-learning models were assessed by discrimination, calibration and decision curve analysis.
Results
The factors most significantly associated with recurrent PJI in patients following revision total knee arthroplasty for PJI included irrigation and debridement with/without modular component exchange (p < 0.001), > 4 prior open surgeries (p < 0.001), metastatic disease (p < 0.001), drug abuse (p < 0.001), HIV/AIDS (p < 0.01), presence of Enterococcus species (p < 0.01) and obesity (p < 0.01). The machine-learning models all achieved excellent performance across discrimination (AUC range 0.81–0.84).
Conclusion
This study developed three machine-learning models for the prediction of recurrent infections in patients following revision total knee arthroplasty for periprosthetic joint infection. The strongest predictors were previous irrigation and debridement with or without modular component exchange and prior open surgeries. The study findings show excellent model performance, highlighting the potential of these computational tools in quantifying increased risks of recurrent PJI to optimize patient outcomes.
Level of evidence
IV.





Similar content being viewed by others
Data availability
Data are available upon request.
Code availability
Only standard software was used for analysis.
References
Abdelaziz H, Gruber H, Gehrke T, Salber J, Citak M (2019) What are the factors associated with re-revision after one-stage revision for periprosthetic joint infection of the hip? A case–control study. Clin Orthop Relat Res 10:2258–2263
Aggarwal V, Bakhshi H, Ecker N, Parvizi J, Gehrke T, Kendoff D (2014) Organism profile in periprosthetic joint infection: pathogens differ at two arthroplasty infection referral centers in Europe and in the United States. J Knee Surg 27:399–406
Allahbakhshi K, Khorasani-Zavareh D, Jazani RK, Ghomian Z (2019) Preparedness components of health systems in the Eastern Mediterranean Region for effective responses to dust and sand storms: a systematic review. F1000Research 8:146–152
Bilimoria KY, Liu Y, Paruch JL, Zhou L, Kmiecik TE, Ko CY, Cohen ME (2013) Development and evaluation of the universal ACS NSQIP surgical risk calculator: a decision aid and informed consent tool for patients and surgeons. J Am Coll Surg 217:833–841
Bozic KJ, Ong K, Lau E, Berry DJ, Vail TP, Kurtz SM, Rubash HE (2013) Estimating risk in Medicare patients with THA: an electronic risk calculator for periprosthetic joint infection and mortality. Clin Orthop Relat Res 471:574–583
Van Calster B, McLernon DJ, van Smeden M, Wynants L, Steyerberg EW, Bossuyt P, Collins GS, Macaskill P, McLernon DJ, Moons KGM, Steyerberg EW, Van Calster B, van Smeden M, Vickers AJ, initiative O behalf of TG ‘Evaluating diagnostic tests and prediction models’ of the S (2019) Calibration: the Achilles heel of predictive analytics. BMC Med 17:230–237
Ching T, Zhu X, Garmire LX (2018) Cox-nnet: an artificial neural network method for prognosis prediction of high-throughput omics data. PLoS Comput Biol 14:e1006076
Citak M, Friedenstab J, Abdelaziz H, Suero EM, Zahar A, Salber J, Gehrke T (2019) Risk factors for failure after 1-stage exchange total knee arthroplasty in the management of periprosthetic joint infection. J Bone Jt Surg Am 101:1061–1069
Darst BF, Malecki KC, Engelman CD (2018) Using recursive feature elimination in random forest to account for correlated variables in high dimensional data. BMC Genet 19:1–6
Ferro CAT (2007) Comparing probabilistic forecasting systems with the Brier score. Weather Forecast 22:1076–1088
Haeberle HS, Helm JM, Navarro SM, Karnuta JM, Schaffer JL, Callaghan JJ, Mont MA, Kamath AF, Krebs VE, Ramkumar PN (2019) Artificial intelligence and machine learning in lower extremity arthroplasty: a review. J Arthroplasty 34:2201–2203
Harris AHS, Kuo AC, Weng Y, Trickey AW, Bowe T, Giori NJ (2019) Can machine learning methods produce accurate and easy-to-use prediction models of 30-day complications and mortality after knee or hip arthroplasty? Clin Orthop Relat Res 477:452–460
Huang R, Hu C-C, Adeli B, Mortazavi J, Parvizi J (2012) Culture-negative periprosthetic joint infection does not preclude infection control. Clin Orthop Relat Res 470:2717–2723
Ibrahim MS, Twaij H, Haddad FS (2018) Two-stage revision for the culture-negative infected total hip arthroplasty: a comparative study. Bone Jt J 100B:3–8
Jamthikar A, Gupta D, Saba L, Khanna NN, Araki T, Viskovic K, Mavrogeni S, Laird JR, Pareek G, Miner M, Sfikakis PP, Protogerou A, Viswanathan V, Sharma A, Nicolaides A, Kitas GD, Suri JS (2020) Cardiovascular/stroke risk predictive calculators: a comparison between statistical and machine learning models. Cardiovasc Diagn Ther 10:919–938
Karhade AV, Schwab JH, Bedair HS (2019) Development of machine learning algorithms for prediction of sustained postoperative opioid prescriptions after total hip arthroplasty. J Arthroplasty 34:2272–2277
Kieboom J, Tirumala V, Box H, Oganesyan R, Klemt C, Kwon Y-M (2021) One-stage revision is as effective as two-stage revision for chronic culture-negative periprosthetic joint infection after total hip and knee arthroplasty. Bone Jt J 103-B:515–521
Klemt C, Smith EJ, Tirumala V, Bounajem G, van den Kieboom J, Kwon Y-M (2021) Outcomes and risk factors associated with 2-stage reimplantation requiring an interim spacer exchange for periprosthetic joint infection. J Arthroplasty 36:1094–1100
Klemt C, Tirumala V, Oganesyan R, Xiong L, van den Kieboom J, Kwon Y-M (2021) Single-stage revision of the infected total knee arthroplasty is associated with improved functional outcomes: a propensity score-matched cohort study. J Arthroplasty 36:298–304
Klemt C, Tirumala V, Smith EJ, Padmanabha A, Kwon Y-M (2020) Development of a preoperative risk calculator for re-infection following revision surgery for periprosthetic joint infection. J Arthroplasty 2:693–699
Klemt C, Tirumala V, Smith EJ, Padmanabha A, Kwon Y-M (2021) Development of a preoperative risk calculator for reinfection following revision surgery for periprosthetic joint infection. J Arthroplasty 36:693–699
Kurtz SM, Lau E, Schmier J, Ong KL, Zhao KE, Parvizi J (2008) Infection burden for hip and knee arthroplasty in the United States. J Arthroplasty 23:984–991
Ma C, Lu Y, Bell KL, Wang J, Ko J, Wang C, Kuo F (2019) Predictors of treatment failure after 2-stage reimplantation for infected total knee arthroplasty: a 2- to 10-year follow-up. J Arthroplasty 33:2234–2239
Panesar SS, D’Souza RN, Yeh F-C, Fernandez-Miranda JC (2019) Machine learning versus logistic regression methods for 2-year mortality prognostication in a small, heterogeneous glioma database. World Neurosurg 2:100012
Parvizi J, Tan TL, Goswami K, Higuera C, Della Valle C, Chen AF, Shohat N (2018) The 2018 definition of periprosthetic hip and knee infection: an evidence-based and validated criteria. J Arthroplasty 33:1309–1314
Parvizi J, Zmistowski B, Berbari EF, Bauer TW, Springer BD, Della Valle CJ, Garvin KL, Mont MA, Wongworawat MD, Zalavras CG (2011) New definition for periprosthetic joint infection: from the Workgroup of the Musculoskeletal Infection Society. Clin Orthop Relat Res 469:2992–2994
Shohat N, Goswami K, Tan TL, Fillingham Y, Parvizi J (2019) Increased failure after irrigation and debridement for acute hematogenous periprosthetic joint infection. J Bone Jt Surg Am 101:696–703
Shohat N, Goswami K, Tan TL, Yayac M, Soriano A, Sousa R, Wouthuyzen-Bakker M, Parvizi J (2020) 2020 Frank Stinchfield Award: identifying who will fail following irrigation and debridement for prosthetic joint infection: a machine learning-based validated tool. Bone Jt J 102:11–19
Sniderman J, Stark RB, Schwartz CE, Imam H, Finkelstein JA, Nousiainen M (2021) Patient factors that matter in predicting hip arthroplasty outcomes: a machine-learning approach. J Arthroplasty 6:2024–2032
Steyerberg EW, Vergouwe Y (2014) Towards better clinical prediction models: seven steps for development and an ABCD for validation. Eur Heart J 35:1925–1931
Tan TL, Maltenfort MG, Chen AF, Shahi A, Higuera CA, Siqueira M, Parvizi J (2018) Development and evaluation of a preoperative risk calculator for periprosthetic joint infection following total joint arthroplasty. J Bone Jt Surg Am 100:777–785
Vickers AJ, Elkin EB (2006) Decision curve analysis: a novel method for evaluating prediction models. Int J Soc Med 26:565–574
Funding
The study did not receive any funding.
Author information
Authors and Affiliations
Contributions
CK: data collection, analysis, write-up. SL: data collection, analysis, write-up. ACU: write-up. JCB: data collection. TGC: write-up. IY: data collection. YH: data collection. Y-MK: analysis, write-up.
Corresponding author
Ethics declarations
Conflict of interest
All authors report no conflict of interest or financial disclosures.
Ethical approval
This study was approved by the Institutional Review Board (IRB).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Klemt, C., Laurencin, S., Uzosike, A.C. et al. Machine learning models accurately predict recurrent infection following revision total knee arthroplasty for periprosthetic joint infection. Knee Surg Sports Traumatol Arthrosc 30, 2582–2590 (2022). https://doi.org/10.1007/s00167-021-06794-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06794-3