Abstract
Rationale
Memory plays a central role in the psychedelic experience. The spontaneous recall and immersive reliving of autobiographical memories has frequently been noted by researchers and clinicians as a salient phenomenon in the profile of subjective effects of classic psychedelic drugs such as psilocybin, LSD, and ayahuasca. The ability for psychedelics to provoke vivid memories has been considered important to their clinical efficacy.
Objective
This review aims to examine and aggregate the findings from experimental, observational, and qualitative studies on the acute modulation of memory by classic psychedelics in humans.
Method
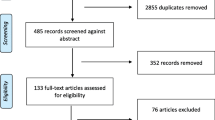
A literature search was conducted using PubMed and PsycInfo as well as manual review of references from eligible studies. Publications reporting quantitative and/or qualitative findings were included; animal studies and case reports were excluded.
Results
Classic psychedelics produce dose-dependently increasing impairments in memory task performance, such that low doses produce no impairment and higher doses produce increasing levels of impairment. This pattern has been observed in tasks assessing spatial and verbal working memory, semantic memory, and non-autobiographical episodic memory. Such impairments may be less pronounced among experienced psychedelic users. Classic psychedelics also increase the vividness of autobiographical memories and frequently stimulate the recall and/or re-experiencing of autobiographical memories, often memories that are affectively intense (positively or negatively valenced) and that had been avoided and/or forgotten prior to the experience.
Conclusions
Classic psychedelics dose-dependently impair memory task performance but may enhance autobiographical memory. These findings are relevant to the understanding of psychological mechanisms of action of psychedelic-assisted psychotherapy.
Similar content being viewed by others
References
Anderson MC (2006) Repression: a cognitive neuroscience approach. In: Mancia M (ed) Psychoanalysis and Neuroscience. Springer Milan, Milano, pp 327–349
Axmacher N, Do Lam ATA, Kessler H, Fell J (2010) Natural memory beyond the storage model: repression, trauma, and the construction of a personal past. Front Hum Neurosci 4. https://doi.org/10.3389/fnhum.2010.00211
Barrett FS, Griffiths RR (2018) Classic hallucinogens and mystical experiences: phenomenology and neural correlates. Curr Top Behav Neurosci 36:393–430. https://doi.org/10.1007/7854_2017_474
Barrett FS, Carbonaro TM, Hurwitz E et al (2018) Double-blind comparison of the two hallucinogens psilocybin and dextromethorphan: effects on cognition. Psychopharmacology 235:2915–2927. https://doi.org/10.1007/s00213-018-4981-x
Belouin SJ, Henningfield JE (2018) Psychedelics: Where we are now, why we got here, what we must do. Neuropharmacology 142:7–19. https://doi.org/10.1016/j.neuropharm.2018.02.018
Belser AB, Agin-Liebes G, Swift TC et al (2017) Patient experiences of psilocybin-assisted psychotherapy: an interpretative phenomenological analysis. J Humanist Psychol. https://doi.org/10.1177/0022167817706884
Bershad AK, Schepers ST, Bremmer MP et al (2019) Acute subjective and behavioral effects of microdoses of lysergic acid diethylamide in healthy human volunteers. Biol Psychiatry 86:792–800. https://doi.org/10.1016/j.biopsych.2019.05.019
Bogenschutz MP, Forcehimes AA (2017) Development of a Psychotherapeutic Model for Psilocybin-Assisted Treatment of Alcoholism. Journal of Humanistic Psychology 57:389–414. https://doi.org/10.1177/0022167816673493
Bogenschutz MP, Ross S (2018) Therapeutic Applications of Classic Hallucinogens. Curr Top Behav Neurosci 36:361–391. https://doi.org/10.1007/7854_2016_464
Bogenschutz MP, Forcehimes AA, Pommy JA et al (2015) Psilocybin-assisted treatment for alcohol dependence: a proof-of-concept study. J Psychopharmacol 29:289–299. https://doi.org/10.1177/0269881114565144
Bouso JC, Riba J (2014) Ayahuasca and the treatment of drug addiction. The therapeutic use of ayahuasca 95–109. https://doi.org/10.1007/978-3-642-40426-9_6
Bouso JC, Fábregas JM, Antonijoan RM et al (2013) Acute effects of ayahuasca on neuropsychological performance: differences in executive function between experienced and occasional users. Psychopharmacology 230:415–424. https://doi.org/10.1007/s00213-013-3167-9
Buckman J (1967) Theoretical aspects of L.S.D. therapy. Int J Soc Psychiatry 13:126–138. https://doi.org/10.1177/002076406701300205
Busch AK, Johnson WC (1950) L.S.D. 25 as an aid in psychotherapy; preliminary report of a new drug. Dis Nerv Syst 11:241–243
Cameron LP, Nazarian A, Olson DE (2020) Psychedelic microdosing: prevalence and subjective effects. J Psychoactive Drugs:1–10. https://doi.org/10.1080/02791072.2020.1718250
Carhart-Harris RL, Friston KJ (2010) The default-mode, ego-functions and free-energy: a neurobiological account of Freudian ideas. Brain 133:1265–1283. https://doi.org/10.1093/brain/awq010
Carhart-Harris RL, Friston KJ (2019) REBUS and the anarchic brain: toward a unified model of the brain action of psychedelics. Pharmacol Rev 71:316–344. https://doi.org/10.1124/pr.118.017160
Carhart-Harris RL, Erritzoe D, Williams T et al (2012a) Neural correlates of the psychedelic state as determined by fMRI studies with psilocybin. Proc Natl Acad Sci U S A 109:2138–2143. https://doi.org/10.1073/pnas.1119598109
Carhart-Harris RL, Leech R, Williams TM et al (2012b) Implications for psychedelic-assisted psychotherapy: functional magnetic resonance imaging study with psilocybin. Br J Psychiatry 200:238–244. https://doi.org/10.1192/bjp.bp.111.103309
Carhart-Harris RL, Leech R, Hellyer PJ et al (2014) The entropic brain: a theory of conscious states informed by neuroimaging research with psychedelic drugs. Front Hum Neurosci 8. https://doi.org/10.3389/fnhum.2014.00020
Carhart-Harris RL, Kaelen M, Whalley MG et al (2015) LSD enhances suggestibility in healthy volunteers. Psychopharmacology 232:785–794. https://doi.org/10.1007/s00213-014-3714-z
Carhart-Harris RL, Bolstridge M, Rucker J et al (2016a) Psilocybin with psychological support for treatment-resistant depression: an open-label feasibility study. Lancet Psychiatry 3:619–627. https://doi.org/10.1016/S2215-0366(16)30065-7
Carhart-Harris RL, Muthukumaraswamy S, Roseman L et al (2016b) Neural correlates of the LSD experience revealed by multimodal neuroimaging. Proc Natl Acad Sci U S A 113:4853–4858. https://doi.org/10.1073/pnas.1518377113
Carhart-Harris RL, Roseman L, Haijen E et al (2018) Psychedelics and the essential importance of context. J Psychopharmacol 32:725–731. https://doi.org/10.1177/0269881118754710
Carter OL, Burr DC, Pettigrew JD et al (2005) Using psilocybin to investigate the relationship between attention, working memory, and the serotonin 1A and 2A receptors. J Cogn Neurosci 17:1497–1508. https://doi.org/10.1162/089892905774597191
Chai WJ, Abd Hamid AI, Abdullah JM (2018) Working memory from the psychological and neurosciences perspectives: a review. Front Psychol 9. https://doi.org/10.3389/fpsyg.2018.00401
Chandler AL, Hartman MA (1960) Lysergic acid diethylamide (LSD-25) as a facilitating agent in psychotherapy. AMA Arch Gen Psychiatry 2:286–299. https://doi.org/10.1001/archpsyc.1960.03590090042008
Cohen S, Eisner BG (1959) Use of lysergic acid diethylamide in a psychotherapeutic setting. AMA Arch NeurPsych 81:615–619. https://doi.org/10.1001/archneurpsyc.1959.02340170081008
Curran HV, Nutt D, de Wit H (2018) Psychedelics and related drugs: therapeutic possibilities, mechanisms and regulation. Psychopharmacology 235:373–375. https://doi.org/10.1007/s00213-017-4822-3
Cutner M (1959) Analytic work with LSD 25. Psych Quar 33:715–757. https://doi.org/10.1007/BF01562041
Davis AK, Clifton JM, Weaver EG et al (2020) Survey of entity encounter experiences occasioned by inhaled N, N-dimethyltryptamine: phenomenology, interpretation, and enduring effects. J Psychopharmacol. https://doi.org/10.1177/0269881120916143
Domínguez-Clavé E, Soler J, Elices M et al (2016) Ayahuasca: pharmacology, neuroscience and therapeutic potential. Brain Res Bull 126:89–101. https://doi.org/10.1016/j.brainresbull.2016.03.002
Eisner BG, Cohen S (1958) Psychotherapy with lysergic acid diethylamide. J Nerv Ment Dis 127:528–539. https://doi.org/10.1097/00005053-195812000-00006
Foa EB, Hembree EA, Rothbaum BO (2007) Prolonged exposure therapy for PTSD: emotional processing of traumatic experiences: Therapist guide. Oxford University Press, New York
Frecska E, Bokor P, Winkelman M (2016) The therapeutic potentials of ayahuasca: possible effects against various diseases of civilization. Front Pharmacol 7. https://doi.org/10.3389/fphar.2016.00035
Frederking W (1955) Intoxicant drugs (mescaline and lysergic acid diethylamide) in psychotherapy. J Nerv Ment Dis 121:262–266. https://doi.org/10.1097/00005053-195503000-00010
Freud S (1915) Repression. In: Papers on Metapsychology. The Standard Edition of the Complete Works of Sigmund Freud. Vol. XIV (trans: Strachey J). The Hogarth Press, London
Garcia-Romeu A, Richards WA (2018) Current perspectives on psychedelic therapy: use of serotonergic hallucinogens in clinical interventions. Int Rev Psychiatry 30:291–316. https://doi.org/10.1080/09540261.2018.1486289
Gasser P, Holstein D, Michel Y et al (2014) Safety and efficacy of lysergic acid diethylamide-assisted psychotherapy for anxiety associated with life-threatening diseases. J Nerv Ment Dis 202:513–520. https://doi.org/10.1097/NMD.0000000000000113
Gasser P, Kirchner K, Passie T (2015) LSD-assisted psychotherapy for anxiety associated with a life-threatening disease: a qualitative study of acute and sustained subjective effects. J Psychopharmacol (Oxford) 29:57–68. https://doi.org/10.1177/0269881114555249
Gleaves DH, Smith SM, Butler LD, Spiegel D (2004) False and recovered memories in the laboratory and clinic: a review of experimental and clinical evidence. Clin Psychol Sci Pract 11:3–28. https://doi.org/10.1093/clipsy.bph055
González D, Carvalho M, Cantillo J et al (2019) Potential use of ayahuasca in grief therapy. Omega (Westport) 79:260–285. https://doi.org/10.1177/0030222817710879
Griffiths RR, Johnson MW, Carducci MA et al (2016) Psilocybin produces substantial and sustained decreases in depression and anxiety in patients with life-threatening cancer: a randomized double-blind trial. J Psychopharmacol 30:1181–1197. https://doi.org/10.1177/0269881116675513
Griffiths RR, Johnson MW, Richards WA et al (2018) Psilocybin-occasioned mystical-type experience in combination with meditation and other spiritual practices produces enduring positive changes in psychological functioning and in trait measures of prosocial attitudes and behaviors. J Psychopharmacol 32:49–69. https://doi.org/10.1177/0269881117731279
Haijen ECHM, Kaelen M, Roseman L et al (2018) Predicting Responses to Psychedelics: A Prospective Study. Front Pharmacol 9. https://doi.org/10.3389/fphar.2018.00897
Hartogsohn I (2016) Set and setting, psychedelics and the placebo response: an extra-pharmacological perspective on psychopharmacology. J Psychopharmacol 30:1259–1267. https://doi.org/10.1177/0269881116677852
Hartogsohn I (2017) Constructing drug effects: a history of set and setting. Drug Sci Policy Law 3:2050324516683325. https://doi.org/10.1177/2050324516683325
Horák M, Hasíková L, Verter N (2018) Therapeutic potential ascribed to ayahuasca by users in the Czech Republic. J Psychoactive Drugs 50:430–436. https://doi.org/10.1080/02791072.2018.1511878
Hutten NRPW, Mason NL, Dolder PC, Kuypers KPC (2019) Motives and side-effects of microdosing with psychedelics among users. Int J Neuropsychopharmacol 22:426–434. https://doi.org/10.1093/ijnp/pyz029
Huxley A (1956) Mescaline and the “other world.” In: Cholden L (ed) Proceedings of the round table on lysergic acid diethylamide and mescaline in experimental psychiatry. Grune & Stratton, New York
Inserra A (2018) Hypothesis: The psychedelic ayahuasca heals traumatic memories via a sigma 1 receptor-mediated epigenetic-mnemonic process. Front Pharmacol 9:330. https://doi.org/10.3389/fphar.2018.00330
Jarvik ME, Abramson HA, Hirsch MW (1955) Lysergic acid diethylamide (LSD-25): VI. Effect upon recall and recognition of various stimuli. J Psychol 39:443–454. https://doi.org/10.1080/00223980.1955.9916194
Johnson MW, Garcia-Romeu A, Cosimano MP, Griffiths RR (2014) Pilot study of the 5-HT2AR agonist psilocybin in the treatment of tobacco addiction. J Psychopharmacol 28:983–992. https://doi.org/10.1177/0269881114548296
Kjellgren A, Eriksson A, Norlander T (2009) Experiences of encounters with ayahuasca--"the vine of the soul". J Psychoactive Drugs 41:309–315. https://doi.org/10.1080/02791072.2009.10399767
Langs RJ (1967) Stability of earliest memories under LSD-25 and placebo. J Nerv Ment Dis 144:171–184. https://doi.org/10.1097/00005053-196703000-00002
Lebedev AV, Lövdén M, Rosenthal G et al (2015) Finding the self by losing the self: Neural correlates of ego-dissolution under psilocybin. Hum Brain Mapp 36:3137–3153. https://doi.org/10.1002/hbm.22833
Letheby C, Gerrans P (2017) Self unbound: ego dissolution in psychedelic experience. Neurosci Conscious. https://doi.org/10.1093/nc/nix016
Leuner HC (1967) Present state of psycholytic therapy and its possibilities. In: Abramson HA (ed) The use of LSD in psychotherapy and alcoholism. The Bobbs-Merrill, Indianapolis
Levine J, Ludwig AM (1964) The LSD controversy. Compr Psychiatry 5:314–321. https://doi.org/10.1016/S0010-440X(64)80010-9
Levine A, Abramson HA, Abramson HA, Markham S (1955) Lysergic Acid Diethylamide (Lsd-25): Xvi. the Effect on Intellectual Functioning as Measured By the Wechsler-Bellevue Intelligence Scale. J Psychol 40:385–395. https://doi.org/10.1080/00223980.1955.9712992
Lienert G (1966) Mental age regression induced by lysergic acid diethylamide. Aust J Psychol 63:3–11. https://doi.org/10.1080/00223980.1966.10544806
Ling TM, Buckman J (1960) The Use of Lysergic Acid in Individual Psychotherapy. Proc R Soc Med 53:927–929
MacLean KA, Johnson MW, Griffiths RR (2011) Mystical experiences occasioned by the hallucinogen psilocybin lead to increases in the personality domain of openness. J Psychopharmacol 25:1453–1461. https://doi.org/10.1177/0269881111420188
Majić T, Schmidt TT, Gallinat J (2015) Peak experiences and the afterglow phenomenon: when and how do therapeutic effects of hallucinogens depend on psychedelic experiences? J Psychopharmacol (Oxford) 29:241–253. https://doi.org/10.1177/0269881114568040
Mak LE, Minuzzi L, MacQueen G et al (2016) The default mode network in healthy individuals: a systematic review and meta-analysis. Brain Connect 7:25–33. https://doi.org/10.1089/brain.2016.0438
Malone TC, Mennenga SE, Guss J et al (2018) Individual experiences in four cancer patients following psilocybin-assisted psychotherapy. Front Pharmacol 9:256. https://doi.org/10.3389/fphar.2018.00256
Martin AJ (1957) L.S.D. (Lysergic Acid Diethylamide) Treatment of chronic psychoneurotic patients under day-hospital conditions. Int J Soc Psychiatry. https://doi.org/10.1177/002076405700300304
Millière R, Carhart-Harris RL, Roseman L et al (2018) Psychedelics, meditation, and self-consciousness. Front Psychol 9. https://doi.org/10.3389/fpsyg.2018.01475
Müller F, Dolder PC, Schmidt A et al (2018) Altered network hub connectivity after acute LSD administration. Neuroimage Clin 18:694–701. https://doi.org/10.1016/j.nicl.2018.03.005
Nielson JL, Megler JD (2014) Ayahuasca as a candidate therapy for PTSD. In: Labate BC, Cavnar C (eds) The Therapeutic Use of Ayahuasca. Springer, Berlin, pp 41–58
Noorani T, Garcia-Romeu A, Swift TC et al (2018) Psychedelic therapy for smoking cessation: qualitative analysis of participant accounts. J Psychopharmacol (Oxford) 32:756–769. https://doi.org/10.1177/0269881118780612
Nour MM, Evans L, Nutt D, Carhart-Harris RL (2016) Ego-dissolution and psychedelics: validation of the ego-dissolution inventory (EDI). Front Hum Neurosci 10. https://doi.org/10.3389/fnhum.2016.00269
Nutt D, Erritzoe D, Carhart-Harris R (2020) Psychedelic psychiatry’s brave new world. Cell 181:24–28. https://doi.org/10.1016/j.cell.2020.03.020
Oram M (2018) The trials of psychedelic therapy: LSD psychotherapy in America, 1st edn. Johns Hopkins University Press, Baltimore
Palhano-Fontes F, Andrade KC, Tofoli LF et al (2015) The psychedelic state induced by ayahuasca modulates the activity and connectivity of the default mode network. PLoS ONE 10:e0118143. https://doi.org/10.1371/journal.pone.0118143
Pokorny T, Duerler P, Seifritz E, et al (2019) (undefined/ed) LSD acutely impairs working memory, executive functions, and cognitive flexibility, but not risk-based decision-making. Psychol Med 1–10. https://doi.org/10.1017/S0033291719002393
Pollan M (2018) How to change your mind: what the new science of psychedelics teaches us about consciousness, dying, addiction, depression, and transcendence, Softcover large print edition edition. Penguin Press, New York
Porter LS, Lane RC (1996) Iatrogenic creation of false childhood sexual abuse memories: Controversy, dynamics, fantasy, and reality. J Contemp Psychother 26:23–42. https://doi.org/10.1007/BF02307703
Preller KH, Burt JB, Ji JL et al (2018) Changes in global and thalamic brain connectivity in LSD-induced altered states of consciousness are attributable to the 5-HT2A receptor. eLife 7:e35082. https://doi.org/10.7554/eLife.35082
Rabin AI, Guertin WH (1951) Research with the Wechsler-Bellevue test: 1945-1950. Psychol Bull 48:211–248. https://doi.org/10.1037/h0059554
Raichle ME (2015) The Brain’s Default Mode Network. Annu Rev Neurosci 38:433–447. https://doi.org/10.1146/annurev-neuro-071013-014030
Renelli M, Fletcher J, Tupper KW et al (2020) An exploratory study of experiences with conventional eating disorder treatment and ceremonial ayahuasca for the healing of eating disorders. Eat Weight Disord 25:437–444. https://doi.org/10.1007/s40519-018-0619-6
Riba J, Rodríguez-Fornells A, Urbano G et al (2001) Subjective effects and tolerability of the South American psychoactive beverage Ayahuasca in healthy volunteers. Psychopharmacology 154:85–95. https://doi.org/10.1007/s002130000606
Richards WA (2017) Psychedelic psychotherapy: insights from 25 years of research. J Humanist Psychol 57:323–337. https://doi.org/10.1177/0022167816670996
Rizzolatti G, Semi AA, Fabbri-Destro M (2014) Linking psychoanalysis with neuroscience: the concept of ego. Neuropsychologia 55:143–148. https://doi.org/10.1016/j.neuropsychologia.2013.10.003
Robinson JT, Davies LS, Sack ELNS, Morrissey JD (1963) a controlled trial of abreaction with lysergic acid diethylamide (Lsd-25). Br J Psychiatry 109:46–53. https://doi.org/10.1192/bjp.109.458.46
Roseman L, Nutt DJ, Carhart-Harris RL (2018) Quality of acute psychedelic experience predicts therapeutic efficacy of psilocybin for treatment-resistant depression. Front Pharmacol 8. https://doi.org/10.3389/fphar.2017.00974
Ross S, Bossis A, Guss J et al (2016) Rapid and sustained symptom reduction following psilocybin treatment for anxiety and depression in patients with life-threatening cancer: a randomized controlled trial. J Psychopharmacol 30:1165–1180. https://doi.org/10.1177/0269881116675512
Sandison RA (1954) Psychological aspects of the LSD treatment of the neuroses. J Ment Sci 100:508–515. https://doi.org/10.1192/bjp.100.419.508
Sandison RA (1963) Certainty and uncertainty in the LSD treatment of psychoneurosis. In: Crocket RW, Sandison RA, Walk A (eds) Hallucinogenic drugs and their psychotherapeutic use. H. K. Lewis, London
Sandison RA, Whitelaw JD (1957) Further studies in the therapeutic value of lysergic acid diethylamide in mental illness. J Ment Sci 103:332–343. https://doi.org/10.1192/bjp.103.431.332
Sandison RA, Spencer AM, Whitelaw JD (1954) The therapeutic value of lysergic acid diethylamide in mental illness. J Ment Sci 100:491–507. https://doi.org/10.1192/bjp.100.419.491
Santangelo V, Bordier C (2019) Large-scale brain networks underlying successful and unsuccessful encoding, maintenance, and retrieval of everyday scenes in visuospatial working memory. Front Psychol 10. https://doi.org/10.3389/fpsyg.2019.00233
Savage C (1952) Lysergic acid diethylamide (LSD-25): a clinical-psychological study. Am J Psychiatry 108:896–900. https://doi.org/10.1176/ajp.108.12.896
Savage C (1957) The resolution and subsequent remobilization of resistance by LSD in psychotherapy. J Nerv Ment Dis 125:434–437. https://doi.org/10.1097/00005053-195707000-00015
Schmiege GR (1963) LSD as a therapeutic tool. J Med Soc N J 60:203–207
Schoen SM (1964) LSD in psychotherapy. Am J Psychother 18:35–51. https://doi.org/10.1176/appi.psychotherapy.1964.18.1.35
Shapiro F (2018) Eye movement desensitization and reprocessing (EMDR) therapy: basic principles, protocols, and procedures, 3rd edn. Guilford Press, New York
Sherwood JN, Stolaroff MJ, Harman WW (1968) The psychedelic experience - a new concept in psychotherapy. J Psychedelic Drugs 1:96–111. https://doi.org/10.1080/02791072.1968.10524522
Silverstein AB, Klee GD (1958) Effects of lysergic acid diethylamide (LSD-25) on intellectual functions. AMA Arch NeurPsych 80:477–480. https://doi.org/10.1001/archneurpsyc.1958.02340100077018
Silverstein AB, Klee GD (1960) The effect of lysergic acid diethylamide on digit span. J Clin Exp Psychopathol Quart 21:11–14
Sloane B, Doust JW (1954) Psychophysiological investigations in experimental psychoses; results of the exhibition of d-lysergic acid diethylamide to psychiatric patients. J Ment Sci 100:129–144. https://doi.org/10.1192/bjp.100.418.129
Speth J, Speth C, Kaelen M et al (2016) Decreased mental time travel to the past correlates with default-mode network disintegration under lysergic acid diethylamide. J Psychopharmacol. https://doi.org/10.1177/0269881116628430
Swift TC, Belser AB, Agin-Liebes G et al (2017) Cancer at the dinner table: experiences of psilocybin-assisted psychotherapy for the treatment of cancer-related distress. J Humanist Psychol 57:488–519. https://doi.org/10.1177/0022167817715966
Turton S, Nutt DJ, Carhart-Harris RL (2014) A qualitative report on the subjective experience of intravenous psilocybin administered in an FMRI environment. Curr Drug Abuse Rev 7:117–127. https://doi.org/10.2174/1874473708666150107120930
Unger SM (1963) Mescaline, LSD, psilocybin, and personality change. Psychiatry 26:111–125. https://doi.org/10.1080/00332747.1963.11023344
Vollenweider FX, Kometer M (2010) The neurobiology of psychedelic drugs: implications for the treatment of mood disorders. Nat Rev Neurosci 11:642–651. https://doi.org/10.1038/nrn2884
Vollenweider FX, Vollenweider-Scherpenhuyzen MFI, Bäbler A et al (1998) Psilocybin induces schizophrenia-like psychosis in humans via a serotonin-2 agonist action. NeuroReport 9:3897–3902
Watts R, Day C, Krzanowski J et al (2017) Patients’ accounts of increased “Connectedness” and “Acceptance” after psilocybin for treatment-resistant depression. J Humanist Psychol 57:520–564. https://doi.org/10.1177/0022167817709585
Wittmann M, Carter O, Hasler F et al (2007) Effects of psilocybin on time perception and temporal control of behaviour in humans. J Psychopharmacol. https://doi.org/10.1177/0269881106065859
Zhang G, Stackman RW (2015) The role of serotonin 5-HT2A receptors in memory and cognition. Front Pharmacol 6:225. https://doi.org/10.3389/fphar.2015.00225
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declares that there is no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Healy, C.J. The acute effects of classic psychedelics on memory in humans. Psychopharmacology 238, 639–653 (2021). https://doi.org/10.1007/s00213-020-05756-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00213-020-05756-w