Abstract
Objectives
To determine the best compromise between low radiation dose and suitable image quality for the detection of lytic and sclerotic bone lesions of the lumbar spine and pelvis.
Methods
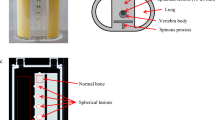
A phantom was scanned using the routine protocol (STD, 13 mGy) and six decreasing dose levels. Raw data were reconstructed using level 3 of iterative reconstruction (IR3) with 1-mm slice thickness for the STD protocol and highest IR levels with 3-mm slice thickness for the others. CTDIvol was used for radiation dose assessment. Quantitative criteria (noise power spectrum [NPS], task-based transfer function [TTF], and the detectability index [d′]), as well as qualitative analysis, were used to compare protocols. NPS and TTF were computed using specific software (imQuest). d′ was computed for two imaging tasks: lytic and sclerotic bone lesions. A subjective analysis was performed to validate the image quality obtained on the anthropomorphic phantom with the different dose values.
Results
Similar d′ values were found for CTDIvol from 3 to 4 mGy with IR4 and from 1 to 2 mGy for IR5 compared with d′ values using the STD protocol. Image quality was validated subjectively for IR4 but rejected for IR5 (image smoothing). Finally, for the same d′, the dose was reduced by 74% compared with the STD protocol, with the CTDIvol being 3.4 mGy for the lumbar spine and for the pelvis.
Conclusion
A dose level as low as 3.4 mGy, in association with high levels of IR, provides suitable image quality for the detection of lytic and sclerotic bone lesions of the lumbar spine and pelvis.
Key Points
• A CTDI vol of 3.4 mGy, in association with high iterative reconstruction level, provides suitable image quality for the detection of lytic and sclerotic bone lesions, both at objective and subjective analysis.
• Compared with the standard protocol, radiation dose can be reduced up to 74% for the lumbar spine and pelvis.
• A task-based image quality assessment using the detectability index represents an objective method for the assessment of image quality and bridges the gap between complex physical metrics and subjective image analysis.

Similar content being viewed by others
Abbreviations
- CT:
-
Computed tomography
- CTDIvol :
-
Volume-computed tomography dose index
- d′:
-
Detectability index
- DLP:
-
Dose length product
- E:
-
Effective dose
- ESF:
-
Edge-spread function
- FBP:
-
Filtered back projection
- IR:
-
Iterative reconstruction
- LSF:
-
Line-spread function
- NPS:
-
Noise power spectrum
- NPWE:
-
Nonprewhitening observer model with eye filter
- ROI:
-
Region of interest
- SAFIRE:
-
Sinogram-affirmed iterative reconstruction
- STD:
-
Standard protocol
- TTF:
-
Task-based transfer function
References
Brenner DJ, Hall EJ (2007) Computed tomography--an increasing source of radiation exposure. N Engl J Med 357:2277–2284
Laurent G, Villani N, Hossu G et al (2019) Full model-based iterative reconstruction (MBIR) in abdominal CT increases objective image quality, but decreases subjective acceptance. Eur Radiol 29:4016–4025
Racine D, Ryckx N, Ba A et al (2018) Task-based quantification of image quality using a model observer in abdominal CT: a multicentre study. Eur Radiol 28:5203–5210
Greffier J, Macri F, Larbi A et al (2016) Dose reduction with iterative reconstruction in multi-detector CT: what is the impact on deformation of circular structures in phantom study? Diagn Interv Imaging 97:187–196
Larbi A, Orliac C, Frandon J et al (2018) Detection and characterization of focal liver lesions with ultra-low dose computed tomography in neoplastic patients. Diagn Interv Imaging 99:311–320
Suntharalingam S, Mikat C, Wetter A et al (2018) Whole-body ultra-low dose CT using spectral shaping for detection of osteolytic lesion in multiple myeloma. Eur Radiol 28:2273–2280
Park JH, Jeon JJ, Lee SS et al (2018) Can we perform CT of the appendix with less than 1 mSv? A De-escalating dose-simulation study. Eur Radiol 28:1826–1834
Fingerle AA, Noël PB (2018) Dose reduction in abdominal CT: the road to submillisievert imaging. Eur Radiol 28:2743–2744
Omoumi P, Verdun FR, Becce F (2015) Optimization of radiation dose and image quality in musculoskeletal CT: emphasis on iterative reconstruction techniques (part 2). Semin Musculoskelet Radiol 19:422–430
Samei E, Richard S (2015) Assessment of the dose reduction potential of a model-based iterative reconstruction algorithm using a task-based performance metrology. Med Phys 42:314–323
Solomon J, Zhang Y, Wilson J, Samei E (2018) An automated software tool for task-based image quality assessment and matching in clinical CTusing the TG-233 framework. AAPM 2018, Nashville TN
Gervaise A, Gervaise-Henry C, Pernin M, Naulet P, Junca-Laplace C, Lapierre-Combes M (2016) How to perform low-dose computed tomography for renal colic in clinical practice. Diagn Interv Imaging 97:393–400
Acknowledgements
We are deeply grateful to Dr. J. Solomon for support regarding the use of the imQuest software.
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Jean Paul Beregi.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was not required for this study because this is a phantom study.
Ethical approval
Institutional Review Board approval was not required because this is a phantom study.
Methodology
• experimental
• Performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 11.6 MB)
Rights and permissions
About this article
Cite this article
Greffier, J., Frandon, J., Pereira, F. et al. Optimization of radiation dose for CT detection of lytic and sclerotic bone lesions: a phantom study. Eur Radiol 30, 1075–1078 (2020). https://doi.org/10.1007/s00330-019-06425-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-019-06425-z