Abstract
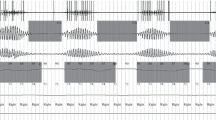
The recent SERVE HF study concluded that patients with chronic heart failure (CHF) and Cheyne–Stokes respiration (CSR) have increased mortality when treated with adaptive servo-ventilation (ASV). We, therefore, wanted to explore if these patients tolerated discontinuation of ASV treatment. The study was a prospective post-ASV treatment observational design with a 3-month follow-up period. 14 patients from our outpatient clinic, all male, were originally diagnosed with CHF and Cheyne–Stokes respiration, which is a clinical form of central sleep apnea. Left ventricular ejection fraction (LVEF) was ≤45% when ASV treatment was initiated. Median machine use was 68 (42–78) months when the patients were instructed to terminate ASV treatment. The patients were then followed during conventional CHF treatment for 3 months. Study baseline was set the last ASV treatment day. Sleep data were collected from the machine the last day of use. Apnea–hypopnea index (AHI), LVEF, 6-min walk test and 24-h ambulatory electrocardiogram recordings were performed at baseline and at study end. Life quality data were obtained using The Minnesota Living with Heart Failure Questionaire (MLHFQ). New York Heart Association Functional Classification (NYHA) was registered. An ambulatory sleep screening was performed at study end. AHI increased significantly after 3 months without ASV treatment [from 1.6 (0.8–3.2) to 39.2 (24.3–44.1, p = 0.001)]. Quality of life (QOL) decreased significantly: 30 (13–54) at discontinuation of ASV vs. 46 (24–67) (MLHFQ) at study end, p = 0.04. Though there was no significant change in NYHA functional class, patients especially reported increased shortness of breath, reduced concentration and reduced memory after discontinuation of ASV treatment. There were no significant differences in LVEF, heart rhythm data and physical capacity. Left ventricular function was preserved indicating that discontinuation of ASV in heart failure patients does not affect cardiac capacity. There was a significant decrement in QOL that must be considered in further treatment of these patients.

Similar content being viewed by others
References
Jaffe LM, Kjekshus J, Gottlieb SS (2013) Importance and management of chronic sleep apnoea in cardiology. Eur Heart J 34(11):809–815
Miyata M, Yoshihisa A, Yamauchi H, Owada T, Sato T, Suzuki S, Sugimoto K, Yamaki T, Kunii H, Nakazato K, Suzuki H, Saitoh S, Takeishi Y (2015) Impact of sleep-disordered breathing on myocardial damage and metabolism in patients with chronic heart failure. Heart Vessels 30(3):318–324
Bitter T, Westerheide N, Prinz C, Hossain MS, Vogt J, Langer C, Horstkotte D, Oldenburg O (2011) Cheyne-stokes respiration and obstructive sleep apnoea are independent risk factors for malignant ventricular arrhythmias requiring appropriate cardioverter-defibrillator therapies in patients with congestive heart failure. Eur Heart J 32(1):61–74
Wang Y, Cao J, Feng J, Chen BY (2015) Cheyne-stokes respiration during sleep: mechanisms and potential interventions. Br J Hosp Med (Lond) 76(7):390–396
Sands SA, Owens R (2015) Congestive heart failure and central sleep apnea. Crit Care Clin 31(3):473–495
Yumino D, Wang H, Floras JS, Newton GE, Mak S, Ruttanaumpawan P, Parker JD, Bradley TD (2009) Relationship between sleep apnoea and mortality in patients with ischaemic heart failure. Heart 95(10):819–824
Bradley TD, Floras JS (2003) Sleep apnea and heart failure: part I: obstructive sleep apnea. Circulation 107(12):1671–1678
Kasai T, Usui Y, Yoshioka T, Yanagisawa N, Takata Y, Narui K, Yamaguchi T, Yamashina A, Momomura S (2010) Effect of flow-triggered adaptive servo-ventilation compared with continuous positive airway pressure in patients with chronic heart failure with coexisting obstructive sleep apnea and Cheyne-Stokes respiration. Circ Heart Fail 3(1):140–148
Oldenburg O, Lamp B, Faber L, Teschler H, Horstkotte D, Topfer V (2007) Sleep-disordered breathing in patients with symptomatic heart failure: a contemporary study of prevalence in and characteristics of 700 patients. Eur J Heart Fail 9(3):251–257
Hanly PJ, Zuberi-Khokhar NS (1996) Increased mortality associated with Cheyne-Stokes respiration in patients with congestive heart failure. Am J Respir Crit Care Med 153(1):272–276
Naughton MT (1998) Pathophysiology and treatment of Cheyne-stokes respiration. Thorax 53(6):514–518
Bradley TD (2000) Continuous positive airway pressure for congestive heart failure. CMAJ 162(4):535–536
Teschler H, Dohring J, Wang YM, Berthon-Jones M (2001) Adaptive pressure support servo-ventilation: a novel treatment for Cheyne-Stokes respiration in heart failure. Am J Respir Crit Care Med 164(4):614–619
Bradley TD, Logan AG, Kimoff RJ, Series F, Morrison D, Ferguson K, Belenkie I, Pfeifer M, Fleetham J, Hanly P, Smilovitch M, Tomlinson G, Floras J (2005) Continuous positive airway pressure for central sleep apnea and heart failure. N Engl J Med 353(19):2025–2033
Arzt M, Floras JS, Logan AG, Kimoff RJ, Series F, Morrison D, Ferguson K, Belenkie I, Pfifer M, Fleetham J, Hanly P, Smilovitch M, Ryan C, Tomlinson G, Bradley TD (2007) Suppression of central sleep apnea by continuous positive airway pressure and transplant-free survival in heart failure: a post hoc analysis of the canadian continuous positive airway pressure for patients with central sleep apnea and heart failure trial (CANPAP). Circulation 115(25):3173–3180
Javaheri S, Brown LK, Randerath WJ (2014) Clinical applications of adaptive servoventilation devices: part 2. Chest 146(3):858–868
Yoshihisa A, Suzuki S, Owada T, Iwaya S, Yamauchi H, Miyata M, Yamaki T, Sugimoto K, Kunii H, Nakazato K, Suzuki H, Saitoh S, Takeishi Y (2013) Short-term use of adaptive servo ventilation improves renal function in heart failure patients with sleep-disordered breathing. Heart Vessels 28(6):728–734
Philippe C, Stoica-Herman M, Drouot X, Raffestin B, Escourrou P, Hittinger L, Michel PL, Roualt S, d’Ortho MP (2006) Compliance with and effectiveness of adaptive servoventilation versus continuous positive airway pressure in the treatment of Cheyne-Stokes respiration in heart failure over a six month period. Heart 92(3):337–342
Tomita Y, Kasai T, Kisaka T, Rossiter HB, Kihara Y, Wasserman K, Daida H (2015) Altered breathing syndrome in heart failure: newer insights and treatment options. Curr Heart Fail Rep 12(2):158–165
Cowie MR, Woehrle H, Wegscheider K, Angermann C, d’Ortho MP, Erdmann E, Levy P, Simonds A, Somers V, Zannad F, Teschler H (2015) Adaptive servo-ventilation for central sleep apnea in systolic heart failure. N Engl J Med 373(12):1095–1105
Emdin M, Passino C, Giannoni A (2015) After the SERVE-HF trial, is there still a need for treatment of central apnea? J Card Fail 21(11):903–905
Hetland A, Haugaa KH, Olseng M, Gjesdal O, Ross S, Saberniak J, Jacobsen M, Edvardsen T (2013) Three-month treatment with adaptive servoventilation improves cardiac function and physical activity in patients with chronic heart failure and cheyne-stokes respiration: a prospective randomized controlled trial. Cardiology 126(2):81–90
Dingli K, Coleman EL, Vennelle M, Finch SP, Wraith PK, Mackay TW, Douglas NJ (2003) Evaluation of a portable device for diagnosing the sleep apnoea/hypopnoea syndrome. Eur Respir J 21(2):253–259
Oldenburg O, Schmidt A, Lamp B, Bitter T, Muntean BG, Langer C, Horstkotte D (2008) Adaptive servoventilation improves cardiac function in patients with chronic heart failure and Cheyne-Stokes respiration. Eur J Heart Fail 10(6):581–586
Schiller NB, Shah PM, Crawford M, DeMaria A, Devereux R, Feigenbaum H, Gutgesell H, Reichek N, Sahn D, Schnittger I, Silverman N, Tajik AJ (1989) Recommendations for quantitation of the left ventricle by two-dimensional echocardiography. American society of echocardiography committee on standards, subcommittee on quantitation of two-dimensional echocardiograms. J Am Soc Echocardiogr 2(5):358–367
Nagueh SF, Smiseth OA, Appleton CP, Byrd III BF, Dokainish H, Edvardsen T, Flachskampf FA, Gillebert TC, Klein AL, Lancellotti P, Marino P, Oh JK, Popescu BA, Waggoner AD (2016) Recommendations for the evaluation of left ventricular diastolic function by echocardiography: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging. doi:10.1093/ehjci/jew082
Enright PL (2003) The six-minute walk test. Respir Care 48(8):783–785
Carmona-Bernal C, Ruiz-Garcia A, Villa-Gil M, Sanchez-Armengol A, Quintana-Gallego E, Ortega-Ruiz F, Baron-Esquivias G, Capote F (2008) Quality of life in patients with congestive heart failure and central sleep apnea. Sleep Med 9(6):646–651
Edvardsen T, Haugaa KH (2011) Imaging assessment of ventricular mechanics. Heart 97(16):1349–1356
Haugaa KH, Smedsrud MK, Steen T, Kongsgaard E, Loennechen JP, Skjaerpe T, Voigt JU, Willems R, Smith G, Smiseth O, Amlie J, Edvardsen T (2010) Mechanical dispersion assessed by myocardial strain in patients after myocardial infarction for risk prediction of ventricular arrhythmia. JACC Cardiovasc Imaging 3(3):247–256
Zhang XL, Yin KS, Li XL, Jia EZ, Su M (2006) Efficacy of adaptive servoventilation in patients with congestive heart failure and Cheyne-Stokes respiration. Chin Med J (Engl) 119(8):622–627
Hanly P, Zuberi-Khokhar N (1995) Daytime sleepiness in patients with congestive heart failure and Cheyne-Stokes respiration. Chest 107(4):952–958
Lupon J, Gastelurrutia P, de Antonio M, Gonzalez B, Cano L, Cabanes R, Urrutia A, Diez C, Coll R, Altimir S, Bayes-Genis A (2013) Quality of life monitoring in ambulatory heart failure patients: temporal changes and prognostic value. Eur J Heart Fail 15(1):103–109
Damy T, Margarit L, Noroc A, Bodez D, Guendouz S, Boyer L, Drouot X, Lamine A, Paulino A, Rappeneau S, Stoica MH, Dubois-Rande JL, Adnot S, Hittinger L, d’Ortho MP (2012) Prognostic impact of sleep-disordered breathing and its treatment with nocturnal ventilation for chronic heart failure. Eur J Heart Fail 14(9):1009–1019
Pepperell JC, Maskell NA, Jones DR, Langford-Wiley BA, Crosthwaite N, Stradling JR, Davies J (2003) A randomized controlled trial of adaptive ventilation for Cheyne-Stokes breathing in heart failure. Am J Respir Crit Care Med 168(9):1109–1114
Acknowledgements
This study was supported by The Hospital of Østfold, Fredrikstad, Norway.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Disclosures
None.
Rights and permissions
About this article
Cite this article
Hetland, A., Lerum, T.V., Haugaa, K.H. et al. Patients with Cheyne–Stokes respiration and heart failure: patient tolerance after three-month discontinuation of treatment with adaptive servo-ventilation. Heart Vessels 32, 909–915 (2017). https://doi.org/10.1007/s00380-017-0951-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-017-0951-1