Abstract
Purpose
To estimate the prevalence of metabolic syndrome (MetS) and its components in adults and older adults residents of São Paulo, the association of MetS with the glycemic index (GI) and glycemic load (GL) and the foods that contribute to dietary GI and GL in this population.
Methods
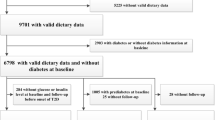
Data from 591 adults and older adults participants in the Health Survey of São Paulo were used. This is a cross-sectional, population-based study with a complex multistage sample design of residents in the urban area of the municipality. Dietary consumption data, anthropometric measurements, blood pressure and blood samples were collected. The associations between GI, GL and MetS and its components were tested using logistic regression models, considering the sample design of the study.
Results
The prevalence of MetS in the adult and older adults residents of São Paulo was 30.3%. There was no association between GI, GL and MetS. GI and GL were positively associated with low high-density lipoprotein cholesterol (HDL-c), OR = 1.113 (95% CI 1.007–1.230) and OR = 1.019 (95% CI 1.002–1.037), respectively. GL was inversely associated with high blood pressure and this association differed by age group (OR = 0.981; 95% CI 0.964–0.998). Foods that most contributed to dietary GI and GL were sugar, white rice and French bread.
Conclusions
Considering the high prevalence of low HDL-c in the population of São Paulo, GI and GL may contribute to the nutritional therapy of this dyslipidemia. However, findings should be treated with caution, considering several conflicting results between studies.
Similar content being viewed by others
References
International Diabetes Federation (2006) The IDF consensus worldwide definition of the Metabolic Syndrome 2006, Brussels
Vidigal FC, Bressan J, Babio N, Salas-Salvadó J (2013) Prevalence of metabolic syndrome in Brazilian adults: a systematic review. BMC Public Health 33:1198
Aguilar M, Bhuket T, Torres S, Liu B, Wong RJ (2015) Prevalence of the Metabolic Syndrome in the United States, 2003–2012. JAMA 313(19):1973–1974
World Health Organization (2014) Global status report on noncommunicable diseases 2014, Geneva
Brasil. Ministério da Saúde (2014) VIGITEL Brasil 2013—Vigilância de fatores de risco e proteção para doenças crônicas por inquérito telefônico, Brasília
Alberti KG, Eckel RH, Grundy SM, Zimmet PZ, Cleeman JI, Donato KA et al (2009) Harmonizing the metabolic syndrome: a joint interim statement of the International Diabetes Federation Task Force on Epidemiology and Prevention; National Heart, Lung, and Blood Institute; American Heart Association; World Heart Federation; International Atherosclerosis Society and International Association for the Study of Obesity. Circulation 120(16):1640–1645
Institute of Medicine, Food and Nutrition Board (2002) Dietary reference intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids. National Academy Press, Washington (DC)
Jenkins DJ, Wolever TM, Taylor RH, Barker HM, Fielden H, Baldwin JM et al (1981) Glycemic index of foods: a physiological basis for carbohydrate exchange. Am J Clin Nutr 34(3):362–366
Salmerón J, Manson JE, Stampfer MJ, Colditz GA, Wing AL, Willett WC (1997) Dietary fiber, glycemic load, and risk of non-insulin-dependent diabetes mellitus in women. JAMA 277(6):472–477
Augustin LS, Kendall CW, Jenkins DJ, Willett WC, Astrup A, Barclay AW et al (2015) Glycemic index, glycemic load and glycemic response: An International Scientific Consensus Summit from the International Carbohydrate Quality Consortium (ICQC). Nutr Metab Cardiovasc Dis 25(9):795–815
Finley CE, Barlow CE, Halton TL, Haskell WL (2010) Glycemic index, glycemic load, and prevalence of the metabolic syndrome in the Cooper Center Longitudinal Study. J Am Diet Assoc 110(12):1820–1829
Kim K, Yun HS, Choi BY, Kim MK (2008) Cross-sectional relationship between dietary carbohydrate, glycaemic index, glycaemic load and risk of the metabolic syndrome in a Korean population. Br J Nutr 100:576–584
Klemsdal TO, Holme I, Nerland H, Pedersen TR, Tonstad S (2010) Effects of a low glycemic load diet versus a low-fat diet in subjects with and without the metabolic syndrome. Nutr Metab Cardiovasc Dis 20:195–201
Juanola-Falgarona M, Salas-Salvadó J, Buil-Cosiales P, Corella D, Estruch R, Ros E et al (2015) Dietary glycemic index and glycemic load are positively associated with risk of developing metabolic syndrome in middle-aged and elderly adults. J Am Geriatr Soc 63:1991–2000
Cullberson A, Kafai MR, Ganji V (2009) Glycemic load is associated with HDL cholesterol but not with the other components and prevalence of metabolic syndrome in the third National Health and Nutrition Examination Survey, 1988–1994. Int Arch Med 2(1):3
Vrolix R, Mensink RP (2010) Effects of glycemic load on metabolic risk markers in subjects at increased risk of developing metabolic syndrome. Am J Clin Nutr 92(2):366–374
Craig CL, Marshall AL, Sjöström M, Bauman AE, Booth ML, Ainsworth BE et al (2003) International physical activity questionnaire: 12-country reliability and validity. Med Sci Sports Exerc 35:1381–1395
World Health Organization (1998) Consultation on Obesity: Preventing and managing the global epidemic, Report, Geneva
Lebrão ML, Duarte YAO (2003) SABE—Saúde, Bem-estar e Envelhecimento—O Projeto Sabe no município de São Paulo: uma abordagem inicial, 1rst ed. Brasília: Organização Pan-Americana da Saúde
Sociedade Brasileira de Cardiologia (2007) V Diretrizes Brasileiras de Hipertensão Arterial. Arq Bras Cardiol 89(3):24–79
Guenther PM, DeMaio TJ, Ingwersen LA, Berlin M (1995) The multiple-pass approach for the 24-hour recall in the continuing survey of food intakes by individuals (CSFII) 1994-96. International Conference on Dietary Assessment Methods, Boston
Flood A, Subar AF, Hull SG, Zimmerman TP, Jenkins DJ, Schatzkin A (2006) Methodology for adding glycemic load values to the National Cancer Institute Diet History Questionnaire database. J Am Diet Assoc 106(3):393–402
Tabela Brasileira de Composição de Alimentos-USP. Versão 5.0, Resposta glicêmica de alimentos brasileiros. São Paulo: Universidade de São Paulo, Faculdade de Ciências Farmacêuticas, Departamento de Alimentos e Nutrição Experimental, 2008. http://www.intranet.fcf.usp.br/tabela/lista.asp?base=r. Accessed 5 Nov 2014
Haubrock J, NÓ§thlings U, Volatier J, Dekkers A, Ocke M, Harttig U (2011) Estimating usual food intake distributions by using the Multiple Source Method in the EPIC-Potsdam Calibration Study. J Nutr 141:914–920
Willett WC, Howe GR, Kushi LW (1997) Adjustment for total energy intake in epidemiologic studies. Am J Clin Nutr 65:1220S–1228S
Block G, Dresser CM, Hartman AM, Carroll MD (1985) Nutrient sources in the American diet: quantitative data from the NHANESII survey. II. Macronutrients and fats. Am J Epidemiol 122:27–40
Alkerwi A, Donneau A, Sauvageot N, Lair ML, Scheen A, Albert A et al (2011) Prevalence of the metabolic syndrome in Luxembourg according to the Joint Interim Statement definition estimated from the ORISCAV-LUX study. BMC Public Health 11(1):4
Fernández-Bergés D, Cabrera de León A, Sanz H, Elosua R, Guembe MJ, Alzamora M et al (2012) Metabolic syndrome in Spain: prevalence and coronary risk associated with harmonized definition and WHO proposal. DARIOS study. Rev Esp Cardiol 65(3):241–248
Barbosa PJB, Lessa I, de Almeida Filho N, Magalhães LBNC, Araújo J (2006) Criteria for Central Obesity in a Brazilian Population: Impact on the Metabolic Syndrome. Arq Bras Cardiol 87:407–414
Vianna CA, da Silva Linhares R, Bielemann RM, Machado EC, González-Chica DA, Matijasevich AM et al (2014) Accuracy and adequacy of waist circumference cut-off points currently recommended in Brazilian adults. Public Health Nutr 17(4):861–869
Vrolix R, Mensink RP (2010) Effects of glycemic load on metabolic risk markers in subjects at increased risk of developing metabolic syndrome. JAMA 92:366–374
Song S, Paik HY, Song WO, Park M, Song Y (2014) Three distinct clustering patterns in metabolic syndrome abnormalities are differentially associated with dietary factors in Korean adults. Nutr Res 34(5):383–390
Shikany JM, Tinker LF, Neuhouser ML, Ma Y, Patterson RE, Phillips LS et al (2010) Association of glycemic load with cardiovascular disease risk factors: the Women’s Health Initiative Observational Study. Nutrition 26(6):641–647
Recio-Rodriguez JI, Gomez-Marcos MA, Patino-Alonso MC, Rodrigo-De Pablo E, Cabrejas-Sánchez A, Arietaleanizbeaskoa MS et al (2015) Glycemic index, glycemic load, and pulse wave reflection in adults. Nutr Metab Cardiovasc Dis 25(1):68–74
Song M, Fung TT, Hu FB, Willett WC, Longo VD, Chan AT et al (2016) Association of Animal and Plant Protein Intake With All-Cause and Cause-Specific Mortality JAMA. Intern Med 176(10):1453–1463
Ludwig DS (2002) The glycemic index: physiological mechanisms relating to obesity, diabetes, and cardiovascular disease. JAMA 287(18):2414–2423
Pawlak DB, Kushner JA, Ludwig DS (2004) Effects of dietary glycaemic index on adiposity, glucose homoeostasis, and plasma lipids in animals. Lancet 364(9436):778–785
Blaak EE, Antoine J-M, Benton D, Bjork I, Bozzetto L, Brouns F et al (2012) Impact of postprandial glycaemia on health and prevention of disease—Etiology and Pathophysiology. Obes Rev 13(10):923–984
Atkinson FS, Foster-Powell K, Brand-Miller JC (2008) International tables of glycemic index and glycemic load values: 2008. Diabetes Care 31(12):2281–2283
Fabricatore AN, Ebbeling CB, Wadden TA, Ludwig DS (2011) Continuous glucose monitoring to assess the ecologic validity of dietary glycemic index and glycemic load. Am J Clin Nutr 94(6):1519–1524
Dodd H, Williams S, Brown R, Venn B (2011) Calculating meal glycemic index by using measured and published food values compared with directly measured meal glycemic index. Am J Clin Nutr 94(4):992–996
Brand-Miller JC (2009) Glycaemic index and glycaemic load: crunch time? Nutr Diet 66, 136–137.
Salmeron J, Ascherio A, Rimm E, Colditz GA, Spiegelman D, Jenkins DJ et al (1997) Dietary fiber, glycemic load, and risk of NIDDM in men. Diabetes Care 20:545–550
Salmeron J, Manson J, Stampfer M, Colditz G, Wing A, Willett W (1997) Dietary fiber, glycemic load, and risk of non-insulin-dependent diabetes mellitus in women. JAMA 277:472–477
Brasil. Ministério do Planejamento, Orçamento e Gestão (2011) Indicadores Sociais Municipais – Uma análise dos resultados do universo do Censo Demográfico 2010, Rio de Janeiro
Acknowledgements
We are grateful to Prof. Dr. Chester Luiz Galvão Cesar, Prof. Dr. Moisés Goldbaum, Maria Cecilia Goi Porto Alves, and all Health Survey of São Paulo staff for conception and design of the study and to the Food Consumption Research Group (GAC) for their support. The São Paulo Municipal Health Department (no grant number), National Council for Scientific and Technological Development (CNPq; Process # 481176/2008-0 e 473100/2009-6), Foundation for Research Support of the State of Paulo (FAPESP; Process # 2009/15831-0 and # 2012/22113-9) and Higher Education Personnel Training Coordination (CAPES; no grant numbers) supported this study.
Author contributions
MMF was involved in the analysis and interpretation of the data and drafting the article. CHS and AAFC were involved in the analysis and interpretation of the data, drafting the article, and revising it critically for important intellectual content. DMM was involved in the conception and design of the study and revising it critically for important intellectual content. RMF was involved in the conception and design of the study, interpretation of the data, and revising the manuscript critically for important intellectual content. All authors approved the final version to be submitted.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
de Mello Fontanelli, M., Sales, C.H., Carioca, A.A.F. et al. The relationship between carbohydrate quality and the prevalence of metabolic syndrome: challenges of glycemic index and glycemic load. Eur J Nutr 57, 1197–1205 (2018). https://doi.org/10.1007/s00394-017-1402-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-017-1402-6