Abstract
Purpose
Several studies in recent years have investigated the relationship between alcohol intake and melanoma risk, with conflicting results. To help clarify this issue, we conducted a literature review and dose–response meta-analysis of studies published until June 30th, 2017, that examined the association between alcohol intake (overall and by beverage type) and melanoma risk.
Methods
We used random effect models with maximum likelihood estimation to calculate summary relative risk (SRR) and 95% confidence intervals (95%CI).
Results
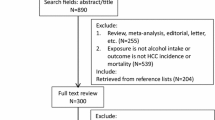
We included 20 independent studies (encompassing 10,555 melanoma cases and over 1.6 million non-cases/controls) published during 1986–2016, of which six had a prospective cohort study design. Adjustment for phenotypic characteristics and sunlight exposure was performed in 11 and nine studies, respectively. Alcohol intake was moderately associated with melanoma risk: the SRR were 1.29 (95% CI 1.14–1.45) for those in the highest vs. lowest category of current alcohol intake, and 1.96 (95% CI 1.02–3.76, I2 = 0%) for cumulative intake. In the dose–response analysis, the increase in risk associated with a 10 g increment in daily alcohol intake was 1.07 (95% CI 1.03–1.11). Risk estimates did not differ by gender, study design and adjustment for confounders; between-studies heterogeneity was acceptable, and there was no evidence of publication bias.
Conclusions
Our findings suggest that alcohol drinking may be moderately associated with increased melanoma risk, although residual confounding and bias cannot be ruled out. Further research is needed to confirm these findings, clarify the role of the different alcohol sources, and investigate the interaction with known melanoma risk factors.





Similar content being viewed by others
Abbreviations
- UV:
-
Ultraviolet
- IARC:
-
International Agency for Research on Cancer
- RR:
-
Relative risk
- SRR:
-
Summary relative risk
- WCRF:
-
World Cancer Research Fund
References
Erdmann F, Lortet-Tieulent J, Schüz J, Zeeb H, Greinert R, Breitbart EW, Bray F (2013) International trends in the incidence of malignant melanoma 1953–2008 are recent generations at higher or lower risk? Int J Cancer 132(2):385–400
Ferlay J, Soerjomataram I, Dikshit R, Eser S, Mathers C, Rebelo M, Parkin DM, Forman D, Bray F (2012) Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 136(5):E359–E386
Gandini S, Sera F, Cattaruzza MS, Pasquini P, Abeni D, Boyle P, Melchi CF (2005) Meta-analysis of risk factors for cutaneous melanoma: I. Common and atypical naevi. Eur J Cancer 41(1):28–44
Gandini S, Sera F, Cattaruzza MS, Pasquini P, Zanetti R, Masini C, Boyle P, Melchi CF (2005) Meta-analysis of risk factors for cutaneous melanoma: III. Family history, actinic damage and phenotypic factors. Eur J Cancer 41(14):2040–2059
Gandini S, Sera F, Cattaruzza MS, Pasquini P, Picconi O, Boyle P, Melchi CF (2005) Meta-analysis of risk factors for cutaneous melanoma: II. Sun exposure. Eur J Cancer 41(1):45–60
International Agency for Research on Cancer (IARC) (2012) IARC Monographs on the evaluation of carcinogenic risks to humans. Radiation, vol 100D. IARC, Lyon, France
de Waure C, Quaranta G, Gualano MR, Cadeddu C, Jovic-Vranes A, Djikanovic B, La Torre G, Ricciardi W (2015) Systematic review of studies investigating the association between dietary habits and cutaneous malignant melanoma. Public Health 129(8):1099–113
Caini S, Masala G, Saieva C, Kvaskoff M, Savoye I, Sacerdote C, Hemmingsson O, Hammer Bech B, Overvad K, Tjønneland A, Petersen KE, Mancini FR, Boutron-Ruault MC, Cervenka I, Kaaks R, Kühn T, Boeing H, Floegel A, Trichopoulou A, Valanou E, Kritikou M, Tagliabue G, Panico S, Tumino R, Bueno-de-Mesquita HB, Peeters PH, Veierød MB, Ghiasvand R, Lukic M, Quirós JR, Chirlaque MD, Ardanaz E, Salamanca Fernández E, Larrañaga N, Zamora-Ros R, Maria Nilsson L, Ljuslinder I, Jirström K, Sonestedt E, Key TJ, Wareham N, Khaw KT, Gunter M, Huybrechts I, Murphy N, Tsilidis KK, Weiderpass E, Palli D (2017) Coffee, tea and melanoma risk: findings from the European Prospective Investigation into Cancer and Nutrition. Int J Cancer 140(10):2246–2255
Noel SE, Stoneham AC, Olsen CM, Rhodes LE, Green AC (2014) Consumption of omega-3 fatty acids and the risk of skin cancers: a systematic review and meta-analysis. Int J Cancer 135(1):149–56
Donat-Vargas C, Berglund M, Glynn A, Wolk A, Åkesson A (2017) Dietary polychlorinated biphenyls, long-chain n-3 polyunsaturated fatty acids and incidence of malignant melanoma. Eur J Cancer 72:137–143
Saladi RN, Nektalova T, Fox JL (2010) Induction of skin carcinogenicity by alcohol and ultraviolet light. Clin Exp Dermatol 35(1):7–11
Rota M, Pasquali E, Bellocco R, Bagnardi V, Scotti L, Islami F, Negri E, Boffetta P, Pelucchi C, Corrao G, La Vecchia C (2014) Alcohol drinking and cutaneous melanoma risk: a systematic review and dose-risk meta-analysis. Br J Dermatol 170(5):1021–1028
Kubo JT, Henderson MT, Desai M, Wactawski-Wende J, Stefanick ML, Tang JY (2014) Alcohol consumption and risk of melanoma and non-melanoma skin cancer in the Women’s Health Initiative. Cancer Causes Control 25(1):1–10
Rivera A, Nan H, Li T, Qureshi A, Cho E (2016) Alcohol intake and risk of incident melanoma: a pooled analysis of three prospective studies in the United States. Cancer Epidemiol Biomark Prev 25(12):1550–1558
Miura K, Zens MS, Peart T, Holly EA, Berwick M, Gallagher RP, Mack TM, Elwood JM, Karagas MR, Green AC (2015) Alcohol consumption and risk of melanoma among women: pooled analysis of eight case-control studies. Arch Dermatol Res 307(9):819–28
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of observational studies in epidemiology (MOOSE) group. JAMA 283(15):2008–2012
Tønnesen H, Møller H, Andersen JR, Jensen E, Juel K (1994) Cancer morbidity in alcohol abusers. Br J Cancer 69:327–332
Sigvardsson S, Hardell L, Przybeck TR, Cloninger R (1996) Increased cancer risk among Swedish female alcoholics. Epidemiology 7(2):140–143
Greenland S (1987) Quantitative methods in the review of epidemiologic literature. Epidemiol Rev 9:1–30
van Houwelingen HC, Arends LR, Stijnen T (2002) Advanced methods in meta-analysis: multivariate approach and meta-regression. Stat Med 21(4):589–624
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558
Macaskill P, Walter SD, Irwig L (2001) A comparison of methods to detect publication bias in meta-analysis. Stat Med 20(4):641–54
Begg CB, Mazumdar M (1994) Operating characteristics of a rank correlation test for publication bias. Biometrics 50(4):1088–101
Greenland S, Longnecker MP (1992) Methods for trend estimation from summarized dose–response data, with applications to meta-analysis. Am J Epidemiol 135(11):1301–1309
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P The Newcastle–Ottawa Scale for assessing the quality of nonrandomised studies in meta-analyses. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed 22 Dec 2017
Holman CD, Armstrong BK, Heenan PJ, Blackwell JB, Cumming FJ, English DR, Holland S, Kelsall GR, Matz LR, Rouse IL et al (1986) The causes of malignant melanoma: results from the West Australian Lions Melanoma Research Project. Recent Results Cancer Res 102:18–37
Stryker WS, Stampfer MJ, Stein EA, Kaplan L, Louis TA, Sober A, Willett WC (1990) Diet, plasma levels of beta-carotene and alpha-tocopherol, and risk of malignant melanoma. Am J Epidemiol 131:597–611
Bain C, Green A, Siskind V, Alexander J, Harvey P (1993) Diet and melanoma. An exploratory case-control study. Ann Epidemiol 3(3):235–238
Westerdahl J, Olsson H, Måsbäck A, Ingvar C, Jonsson N (1996) Risk of malignant melanoma in relation to drug intake, alcohol, smoking and hormonal factors. Br J Cancer 73(9):1126–1131
Rolón PA, Kramárová E, Rolón HI, Khlat M, Parkin DM (1997) Plantar melanoma: a case-control study in Paraguay. Cancer Causes Control 8(6):850–856
Veierød MB, Thelle DS, Laake P (1997) Diet and risk of cutaneous malignant melanoma: a prospective study of 50,757 Norwegian men and women. Int J Cancer 71(4):600–604
Freedman DM, Sigurdson A, Doody MM, Rao RS, Linet MS (2003). Risk of melanoma in relation to smoking, alcohol intake, and other factors in a large occupational cohort. Cancer Causes Control 14(9):847–57
Millen AE, Tucker MA, Hartge P, Halpern A, Elder DE, Guerry D 4th, Holly EA, Sagebiel RW, Potischman N (2004) Diet and melanoma in a case-control study. Cancer Epidemiol Biomark Prev 13(6):1042–1051
Naldi L, Gallus S, Tavani A, Imberti GL, La Vecchia C; Oncology Study Group of the Italian Group for Epidemiologic Research in Dermatology (2004) Risk of melanoma and vitamin A, coffee and alcohol: a case-control study from Italy. Eur J Cancer Prev 13(6):503–508
Vinceti M, Pellacani G, Malagoli C, Bassissi S, Sieri S, Bonvicini F, Krogh V, Seidenari S (2005) A population-based case-control study of diet and melanoma risk in northern Italy. Public Health Nutr 8(8):1307–1314
Le Marchand L, Saltzman BS, Hankin JH, Wilkens LR, Franke AA, Morris SJ, Kolonel LN (2006) Sun exposure, diet, and melanoma in Hawaii Caucasians. Am J Epidemiol 164(3):232–45
Gogas H, Trakatelli M, Dessypris N, Terzidis A, Katsambas A, Chrousos GP, Petridou ET (2008) Melanoma risk in association with serum leptin levels and lifestyle parameters: a case-control study. Ann Oncol 19:384–389
Fortes C, Mastroeni S, Melchi F, Pilla MA, Antonelli G, Camaioni D, Alotto M, Pasquini P (2008) A protective effect of the Mediterranean diet for cutaneous melanoma. Int J Epidemiol 37(5):1018–1029
Allen NE, Beral V, Casabonne D, Kan SW, Reeves GK, Brown A, Green J, Million Women Study Collaborators (2009) Moderate alcohol intake and cancer incidence in women. J Natl Cancer Inst 101(5):296–305
Benedetti A, Parent ME, Siemiatycki J (2009) Lifetime consumption of alcoholic beverages and risk of 13 types of cancer in men: results from a case-control study in Montreal. Cancer Detect Prev 32:352–362
Asgari MM, Brasky TM, White E (2012) Association of vitamin A and carotenoid intake with melanoma risk in a large prospective cohort. J Invest Dermatol 132(6):1573–1582
de Vries E, Trakatelli M, Kalabalikis D, Ferrandiz L, Ruiz-de-Casas A, Moreno-Ramirez D, Sotiriadis D, Ioannides D, Aquilina S, Apap C, Micallef R, Scerri L, Ulrich M, Pitkänen S, Saksela O, Altsitsiadis E, Hinrichs B, Magnoni C, Fiorentini C, Majewski S, Ranki A, Stockfleth E, Proby C; EPIDERM Group (2012) Known and potential new risk factors for skin cancer in European populations: a multicentre case-control study. Br J Dermatol 167(Suppl 2):1–13
International Agency for Research on Cancer (IARC) (2010) IARC monographs on the evaluation of carcinogenic risks to humans. Alcohol consumption and ethyl carbamate, vol 96. IARC, Lyon, France
World Cancer Research Fund/American Institute for Cancer Research (2007) Food, nutrition, physical activity, and the prevention of cancer: a global perspective. AICR, Washington
World Cancer Research Fund/American Institute for Cancer Research. Continuous Update Project Report (2016) Diet, nutrition, physical activity, and oesophageal cancer. World Cancer Research Fund, London
World Cancer Research Fund/American Institute for Cancer Research. Continuous Update Project Report (2011) Food, nutrition, physical activity, and the prevention of colorectal cancer. World Cancer Research Fund, London
World Cancer Research Fund/American Institute for Cancer Research. Continuous Update Project Report (2015) Diet, nutrition, physical activity, and liver cancer. World Cancer Research Fund, London
World Cancer Research Fund/American Institute for Cancer Research. Continuous Update Project Report (2017) Diet, nutrition, physical activity, and breast cancer. World Cancer Research Fund, London
World Cancer Research Fund/American Institute for Cancer Research. Continuous Update Project Report (2016) Diet, nutrition, physical activity, and stomach cancer. World Cancer Research Fund, London
Roswall N, Weiderpass E (2015) Alcohol as a risk factor for cancer: existing evidence in a global perspective. J Prev Med Public Health 48(1):1–9
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The Authors declare that they have no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Gandini, S., Masala, G., Palli, D. et al. Alcohol, alcoholic beverages, and melanoma risk: a systematic literature review and dose–response meta-analysis. Eur J Nutr 57, 2323–2332 (2018). https://doi.org/10.1007/s00394-018-1613-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-018-1613-5