Abstract
Purpose
The relationship between menarche age and endometriosis has been studied extensively; however, the results were inconsistent due to differences in study dates, populations, and methodology. The goal of this meta-analysis was to see how different research populations, dates, and types affected the estimated risk of endometriosis in early menarche.
Methods
The terms “endometriosis”, “early menarche”, and other pertinent terms were searched in PubMed, Medline, and Embase. This meta-analysis comprised 16 papers published between 2000 and 2020, with a start year ranging from 1989 to 2017. Random effects were used to examine endometriosis risks in these articles. Study start years, countries, types (case–control and cohort studies), and quality (Newcastle–Ottawa scale, NOS) were all taken into account in further stratified analysis and meta-regression analyses.
Results
Early menarche (< 12 years) was associated with a significant pooled risk of endometriosis with high heterogeneity (OR = 1.34, 95% CI 1.16–1.54, I2 = 72.0%). Stratified analysis showed that this risk was increased in studies started after 2000 (OR = 1.62, 95% CI 0.96–1.35, I2 = 74.4%), compared to those before 2000 (OR = 1.13, 95% CI 1.16–1.54, I2 = 40.7%); additionally, this risk was higher in low-income countries (OR = 2.11, 95% CI 1.55–2.87, I2 = 0%) than in other countries (OR = 1.25, 95% CI 1.09–1.43, I2 = 70.6%). These results were further confirmed by meta-regression analysis (both P values < 0.1). No significant differences were found between different study types and NOS scores.
Conclusion
Our results suggested an increasing risk of endometriosis with early menarche, which was more noticeable in low-income countries. Large-scale studies are warranted.



Similar content being viewed by others
Availability of data and materials
Not applicable.
Code availability
Not applicable.
References
Armour M, Lawson K, Wood A, Smith CA, Abbott J (2019) The cost of illness and economic burden of endometriosis and chronic pelvic pain in Australia: a national online survey. PLoS ONE 14:e0223316. https://doi.org/10.1371/journal.pone.0223316
Roomaney R, Kagee A (2018) Salient aspects of quality of life among women diagnosed with endometriosis: a qualitative study. J Health Psychol 23:905. https://doi.org/10.1177/1359105316643069
Soliman AM, Surrey E, Bonafede M, Nelson JK, Castelli-Haley J (2018) Real-world evaluation of direct and indirect economic burden among endometriosis patients in the United States. Adv Ther 35:408. https://doi.org/10.1007/s12325-018-0667-3
Lin YH, Chen YH, Chang HY, Au HK, Tzeng CR, Huang YH (2018) Chronic niche inflammation in endometriosis-associated infertility: current understanding and future therapeutic strategies. Int J Mol Sci. https://doi.org/10.3390/ijms19082385
Practice Committee of the American Society for Reproductive M (2012) Endometriosis and infertility: a committee opinion. Fertil Steril 98:591. https://doi.org/10.1016/j.fertnstert.2012.05.031
Farland LV, Missmer SA, Bijon A, Gusto G, Gelot A, Clavel-Chapelon F et al (2017) Associations among body size across the life course, adult height and endometriosis. Hum Reprod 32:1732. https://doi.org/10.1093/humrep/dex207
Holoch KJ, Lessey BA (2010) Endometriosis and infertility. Clin Obstet Gynecol 53:429. https://doi.org/10.1097/GRF.0b013e3181db7d71
Zullo F, Spagnolo E, Saccone G, Acunzo M, Xodo S, Ceccaroni M et al (2017) Endometriosis and obstetrics complications: a systematic review and meta-analysis. Fertil Steril 108:667. https://doi.org/10.1016/j.fertnstert.2017.07.019
Nicolaus K, Brauer D, Sczesny R, Buhler K, Diebolder H, Runnebaum IB (2020) A two-third majority of infertile women exhibit endometriosis in pre-ART diagnostic hysteroscopy and laparoscopic chromopertubation: only one-third have a tubal obstruction. Arch Gynecol Obstet 301:1081. https://doi.org/10.1007/s00404-020-05479-5
von Theobald P, Cottenet J, Iacobelli S, Quantin C (2016) Epidemiology of endometriosis in france: a large, nation-wide study based on hospital discharge data. Biomed Res Int 2016:3260952. https://doi.org/10.1155/2016/3260952
Burney RO, Giudice LC (2012) Pathogenesis and pathophysiology of endometriosis. Fertil Steril 98:511. https://doi.org/10.1016/j.fertnstert.2012.06.029
Lagana AS, Garzon S, Gotte M, Vigano P, Franchi M, Ghezzi F et al (2019) The pathogenesis of endometriosis: molecular and cell biology insights. Int J Mol Sci. https://doi.org/10.3390/ijms20225615
Peterson CM, Johnstone EB, Hammoud AO, Stanford JB, Varner MW, Kennedy A et al (2013) Risk factors associated with endometriosis: importance of study population for characterizing disease in the ENDO Study. Am J Obstet Gynecol 208(451):e1. https://doi.org/10.1016/j.ajog.2013.02.040
Parazzini F, Esposito G, Tozzi L, Noli S, Bianchi S (2017) Epidemiology of endometriosis and its comorbidities. Eur J Obstet Gynecol Reprod Biol 209:3. https://doi.org/10.1016/j.ejogrb.2016.04.021
Wei M, Cheng Y, Bu H, Zhao Y, Zhao W (2016) Length of menstrual cycle and risk of endometriosis: a meta-analysis of 11 case-control studies. Medicine (Baltimore) 95:e2922. https://doi.org/10.1097/MD.0000000000002922
Gaudineau A, Ehlinger V, Vayssiere C, Jouret B, Arnaud C, Godeau E (2010) Factors associated with early menarche: results from the French Health Behaviour in School-aged Children (HBSC) study. BMC Public Health 10:175. https://doi.org/10.1186/1471-2458-10-175
Forman MR, Mangini LD, Thelus-Jean R, Hayward MD (2013) Life-course origins of the ages at menarche and menopause. Adolesc Health Med Ther 4:1. https://doi.org/10.2147/AHMT.S15946
Emons G, Grundker C, Hanf V (2002) Are estrogens carcinogens? Zentralbl Gynakol 124:559. https://doi.org/10.1055/s-2002-40168
Nnoaham KE, Webster P, Kumbang J, Kennedy SH, Zondervan KT (2012) Is early age at menarche a risk factor for endometriosis? A systematic review and meta-analysis of case-control studies. Fertil Steril 98:702. https://doi.org/10.1016/j.fertnstert.2012.05.035
Papadimitriou A (2016) The evolution of the age at menarche from prehistorical to modern times. J Pediatr Adolesc Gynecol 29:527. https://doi.org/10.1016/j.jpag.2015.12.002
Parent AS, Teilmann G, Juul A, Skakkebaek NE, Toppari J, Bourguignon JP (2003) The timing of normal puberty and the age limits of sexual precocity: variations around the world, secular trends, and changes after migration. Endocr Rev 24:668. https://doi.org/10.1210/er.2002-0019
Magnus MC, Guyatt AL, Lawn RB, Wyss AB, Trajanoska K, Kupers LK et al (2020) Identifying potential causal effects of age at menarche: a Mendelian randomization phenome-wide association study. BMC Med 18:71. https://doi.org/10.1186/s12916-020-01515-y
Hiatt RA, Stewart SL, Hoeft KS, Kushi LH, Windham GC, Biro FM et al (2017) Childhood socioeconomic position and pubertal onset in a cohort of multiethnic girls: implications for breast cancer. Cancer Epidemiol Biomark Prev 26:1714. https://doi.org/10.1158/1055-9965.EPI-17-0496
Deardorff J, Abrams B, Ekwaru JP, Rehkopf DH (2014) Socioeconomic status and age at menarche: an examination of multiple indicators in an ethnically diverse cohort. Ann Epidemiol 24:727. https://doi.org/10.1016/j.annepidem.2014.07.002
Toppari J, Juul A (2010) Trends in puberty timing in humans and environmental modifiers. Mol Cell Endocrinol 324:39. https://doi.org/10.1016/j.mce.2010.03.011
Fisher MM, Eugster EA (2014) What is in our environment that effects puberty? Reprod Toxicol 44:7. https://doi.org/10.1016/j.reprotox.2013.03.012
Iavazzo C, Vrachnis N, Gkegkes ID (2022) Peritoneal bacteria contamination and endometriosis pathogenesis. Arch Gynecol Obstet. https://doi.org/10.1007/s00404-022-06467-7
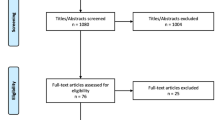
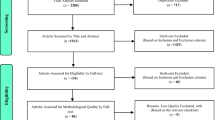
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097. https://doi.org/10.1371/journal.pmed.1000097
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283:2008. https://doi.org/10.1001/jama.283.15.2008
Burghaus S, Klingsiek P, Fasching PA, Engel A, Haberle L, Strissel PL et al (2011) Risk factors for endometriosis in a German case-control study. Geburtshilfe Frauenheilkd 71:1073. https://doi.org/10.1055/s-0031-1280436
Mollazadeh S, Sadeghzadeh Oskouei B, Kamalifard M, Mirghafourvand M, Aminisani N, Shobeiri MJ (2019) Association between sexual activity during menstruation and endometriosis: a case-control study. Int J Fertil Steril. 13:230. https://doi.org/10.22074/ijfs.2019.5601
Bouzari Z, Yazdani S, Ahangarkolaee ZH, Zeinalzadeh M, Hajian K (2016) The comparison of menstrual characteristics and BMI in women with endometriosis and without endometriosis. 6:20. https://scientonline.org/open-access/the-comparison-of-menstrual-characteristics-and-bmi-in-women-with-endometriosis-and-without-endometriosis.pdf
Kvaskoff M, Bijon A, Clavel-Chapelon F, Mesrine S, Boutron-Ruault MC (2013) Childhood and adolescent exposures and the risk of endometriosis. Epidemiology 24:261. https://doi.org/10.1097/EDE.0b013e3182806445
Mamdouh HM, Mortada MM, Kharboush IF, Abd-Elateef HA (2011) Epidemiologic determinants of endometriosis among Egyptian women: a hospital-based case-control study. J Egypt Public Health Assoc 86:21. https://doi.org/10.1097/01.EPX.0000395322.91912.56
Saha R, Kuja-Halkola R, Tornvall P, Marions L (2017) Reproductive and lifestyle factors associated with endometriosis in a large cross-sectional population sample. J Womens Health (Larchmt) 26:152. https://doi.org/10.1089/jwh.2016.5795
Treloar SA, Bell TA, Nagle CM, Purdie DM, Green AC (2010) Early menstrual characteristics associated with subsequent diagnosis of endometriosis. Am J Obstet Gynecol 202(534):e1. https://doi.org/10.1016/j.ajog.2009.10.857
Hemmings R, Rivard M, Olive DL, Poliquin-Fleury J, Gagne D, Hugo P et al (2004) Evaluation of risk factors associated with endometriosis. Fertil Steril 81:1513. https://doi.org/10.1016/j.fertnstert.2003.10.038
Flores I, Abreu S, Abac S, Fourquet J, Laboy J, Rios-Bedoya C (2008) Self-reported prevalence of endometriosis and its symptoms among Puerto Rican women. Int J Gynaecol Obstet 100:257. https://doi.org/10.1016/j.ijgo.2007.08.010
Gallagher JS, DiVasta AD, Vitonis AF, Sarda V, Laufer MR, Missmer SA (2018) The impact of endometriosis on quality of life in adolescents. J Adolesc Health 63:766. https://doi.org/10.1016/j.jadohealth.2018.06.027
Johnson CY, Grajewski B, Lawson CC, Whelan EA, Bertke SJ, Tseng CY (2016) Occupational risk factors for endometriosis in a cohort of flight attendants. Scand J Work Environ Health 42:52. https://doi.org/10.5271/sjweh.3538
Matalliotakis IM, Cakmak H, Fragouli YG, Goumenou AG, Mahutte NG, Arici A (2008) Epidemiological characteristics in women with and without endometriosis in the Yale series. Arch Gynecol Obstet 277:389. https://doi.org/10.1007/s00404-007-0479-1
Missmer SA, Hankinson SE, Spiegelman D, Barbieri RL, Malspeis S, Willett WC et al (2004) Reproductive history and endometriosis among premenopausal women. Obstet Gynecol 104:965. https://doi.org/10.1097/01.AOG.0000142714.54857.f8
Templeman C, Marshall SF, Ursin G, Horn-Ross PL, Clarke CA, Allen M et al (2008) Adenomyosis and endometriosis in the California Teachers Study. Fertil Steril 90:415. https://doi.org/10.1016/j.fertnstert.2007.06.027
Buck Louis GM, Hediger ML, Pena JB (2007) Intrauterine exposures and risk of endometriosis. Hum Reprod 22:3232. https://doi.org/10.1093/humrep/dem338
Deeks JJ (2001) Systematic reviews of evaluations of diagnostic and screening tests. BMJ 323:157
Sterne JA, Egger M (2001) Funnel plots for detecting bias in meta-analysis: guidelines on choice of axis. J Clin Epidemiol 54:1046. https://doi.org/10.1016/s0895-4356(01)00377-8
Lin L, Chu H (2018) Quantifying publication bias in meta-analysis. Biometrics 74:785. https://doi.org/10.1111/biom.12817
Begg CB, Mazumdar M (1994) Operating characteristics of a rank correlation test for publication bias. Biometrics 50:1088
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629. https://doi.org/10.1136/bmj.315.7109.629
Vigano P, Somigliana E, Panina P, Rabellotti E, Vercellini P, Candiani M (2012) Principles of phenomics in endometriosis. Hum Reprod Update 18:248. https://doi.org/10.1093/humupd/dms001
Sampson JA (1927) Metastatic or embolic endometriosis, due to the menstrual dissemination of endometrial tissue into the venous circulation. Am J Pathol 3:93
Marcellin L, Santulli P, Pinzauti S, Bourdon M, Lamau MC, Borghese B et al (2019) Age at menarche does not correlate with the endometriosis phenotype. PLoS ONE 14:e0219497. https://doi.org/10.1371/journal.pone.0219497
Herman-Giddens ME (2006) Recent data on pubertal milestones in United States children: the secular trend toward earlier development. Int J Androl 29:241. https://doi.org/10.1111/j.1365-2605.2005.00575.x
Piekarski DJ, Johnson CM, Boivin JR, Thomas AW, Lin WC, Delevich K et al (2017) Does puberty mark a transition in sensitive periods for plasticity in the associative neocortex? Brain Res 1654:123. https://doi.org/10.1016/j.brainres.2016.08.042
Anderson SE, Must A (2005) Interpreting the continued decline in the average age at menarche: results from two nationally representative surveys of U.S. girls studied 10 years apart. J Pediatr 147:753. https://doi.org/10.1016/j.jpeds.2005.07.016
Bougie O, Yap MI, Sikora L, Flaxman T, Singh S (2019) Influence of race/ethnicity on prevalence and presentation of endometriosis: a systematic review and meta-analysis. BJOG 126:1104. https://doi.org/10.1111/1471-0528.15692
Cramer DW, Missmer SA (2002) The epidemiology of endometriosis. Ann N Y Acad Sci 955:11. https://doi.org/10.1111/j.1749-6632.2002.tb02761.x
Pierce MB, Leon DA (2005) Age at menarche and adult BMI in the Aberdeen children of the 1950s cohort study. Am J Clin Nutr 82:733. https://doi.org/10.1093/ajcn/82.4.733
Funding
This work was supported by Research Foundation of Shenzhen Baoan Women’s and Children’s Hospital, Jinan University to BL (BAFY 2020005).
Author information
Authors and Affiliations
Contributions
MYL: data collection, data analysis, and manuscript writing. JLN: data collection and data analysis. BL: protocol/project development and manuscript writing/editing.
Corresponding author
Ethics declarations
Conflict of interests
The authors have no conflicts of interest to declare.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
This manuscript is approved by all the authors for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.

404_2022_6541_MOESM1_ESM.jpg
Supplementary file1 Linear analysis between NOS score and log(OR) for 16 included studies. NOS, Newcastle-Ottawa scale. Circle size means the reported OR and its 95% CI. Red Line and grey band means the predicted OR and its 95% CI (JPG 92 KB)

404_2022_6541_MOESM2_ESM.jpg
Supplementary file2 Meta-analysis of included studies presented by the subgroups of study countries: Asia & Africa vs. Europe & Oceania vs. North America (JPG 199 KB)

404_2022_6541_MOESM3_ESM.jpg
Supplementary file3 Meta-analysis of included studies presented by the subgroups of study area: low-income countries vs. others (JPG 172 KB)

404_2022_6541_MOESM4_ESM.jpg
Supplementary file4 Meta-analysis of included studies presented by the subgroups of study type: Case-control studies vs. Cohort studies (JPG 174 KB)

404_2022_6541_MOESM5_ESM.jpg
Supplementary file5 Meta-analysis of included studies presented by the subgroups of NOS score: ≤5 vs. >5. NOS, Newcastle-Ottawa scale (JPG 181 KB)

404_2022_6541_MOESM6_ESM.png
Supplementary file6 Funnel plot of the publication bias in this meta-analyses. (A)Funnel plot with pseudo 95% CI of 16 included studies. (B), Begg’s test for small-study effects (PNG 88 KB)



404_2022_6541_MOESM9_ESM.jpg
Supplementary file9 Forest plot of the association between early menarche and endometriosis in studies with different quality on the ascertainment of exposure (age at menarche): 2(top), studies with poor quality on the ascertainment of exposure. 1(bottom), and studies with higher quality on the ascertainment of exposure (JPG 179 KB)

404_2022_6541_MOESM10_ESM.jpg
Supplementary file10 Forest plot of the association between early menarche and endometriosis in 13 included studies, when removing 3 studies with inadequately controlled for potential confounders (JPG 164 KB)
Appendix
Appendix
-
A.
PRISMA 2009 CHECKLIST Online Supplementary Material.
-
B.
MOOSE CHECKLIST Online Supplementary Material.
Rights and permissions
About this article
Cite this article
Lu, MY., Niu, JL. & Liu, B. The risk of endometriosis by early menarche is recently increased: a meta-analysis of literature published from 2000 to 2020. Arch Gynecol Obstet 307, 59–69 (2023). https://doi.org/10.1007/s00404-022-06541-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-022-06541-0