Abstract
Purpose
To describe characteristics of recurrent intermittent exotropia after bilateral lateral rectus (BLR) recession, and identify factors associated with poor outcome after unilateral medial rectus (MR) resection for recurrent intermittent exotropia.
Methods
We retrospectively reviewed 124 patients who have undergone unilateral MR resection for recurrent intermittent exotropia after BLR recession. Patients were followed for at least 2 years after MR resection. Clinical characteristics and risk factors associated with poor outcome after unilateral MR resection were evaluated. Successful outcome was defined as distant deviation within the range of 4 prism diopters (PD) esotropia and 10 PD exotropia at last visit after MR resection.
Results
Among 124 patients, 50 patients (41.1%) were male, and the mean age at the time of MR resection was 9.5 ± 3.1 years. The average follow-up period after MR resection was 43.8 ± 23.7 months. Forty-seven patients (37.9%) were classified to have poor outcome at last visit, and 29 patients (23.4%) underwent third operation. None of the patients was overcorrected after MR resection. Multiple logistic regression analyses showed that distant deviation at post-operative 3 months and male gender were associated with poor outcome (OR 1.49; 95% CI 1.27–1.73; P < 0.001, and OR 5.19; 95% CI 1.42–18.98; P = 0.013, respectively).
Conclusion
Ocular deviation at 3 months after unilateral MR resection for recurrent intermittent exotropia may play a valuable role in anticipating poor outcome. Patients whose exotropia exceeded 9 PD at distance at 3 months’ follow-up tended to recur while those whose exotropia remained below 9 PD at distance showed a stable disease course.

Similar content being viewed by others
References
Ing MR, Pang SW (1974) The racial distribution of strabismus. A statistical study. Hawaii Med J 33:22–23
Lee JY, Lee GI, Park KA, Oh SY (2017) Long-term evaluation of two reoperation groups for intermittent exotropia. J AAPOS 21:349–353. https://doi.org/10.1016/j.jaapos.2017.05.031
Nusz KJ, Mohney BG, Diehl NN (2006) The course of intermittent exotropia in a population-based cohort. Ophthalmology 113:1154–1158. https://doi.org/10.1016/j.ophtha.2006.01.033
Choi J, Chang JW, Kim SJ, Yu YS (2012) The long-term survival analysis of bilateral lateral rectus recession versus unilateral recession-resection for intermittent exotropia. Am J Ophthalmol 153(343–351):e341. https://doi.org/10.1016/j.ajo.2011.06.024
Lee BJ, Kim SJ, Yu YS (2014) Factors associated with the angle of exodeviation in patients with recurrent exotropia. Br J Ophthalmol 98:1414–1419. https://doi.org/10.1136/bjophthalmol-2014-304876
Lim SH, Hwang BS, Kim MM (2012) Prognostic factors for recurrence after bilateral rectus recession procedure in patients with intermittent exotropia. Eye (Lond) 26:846–852. https://doi.org/10.1038/eye.2012.55
Mims JL 3rd (2003) Outcome of 5 mm resection of one medial rectus extraocular muscle for recurrent exotropia. Binocul Vis Strabismus Q 18:143–150
Hahm IR, Yoon SW, Baek SH, Kong SM (2005) The clinical course of recurrent exotropia after reoperation for exodeviation. Korean J Ophthalmol 19:140–144. https://doi.org/10.3341/kjo.2005.19.2.140
Farzavandi KWWAS (2007) Color atlas of strabismus surgery strategies and techniques. Springer Science Business Media, New York
Olitsky SE, Kelly C, Lee H, Nelson LB (2001) Unilateral rectus resection in the treatment of undercorrected or recurrent strabismus. J Pediatr Ophthalmol Strabismus 38:349–353
Chae SH, Chun BY, Kwon JY (2008) The effect of unilateral medial rectus muscle resection in patients with recurrent exotropia. Korean J Ophthalmol 22:174–177. https://doi.org/10.3341/kjo.2008.22.3.174
Kim JH, Kim HJ, Choi DG (2013) Contralateral lateral rectus recession versus recess-resect for recurrent exotropia after unilateral recess-resect. Br J Ophthalmol 97:752–756. https://doi.org/10.1136/bjophthalmol-2013-303171
Sung JY, Yang HK, Hwang JM (2019) Long-term surgical outcomes of bilateral vs. unilateral medial rectus resection for recurrent exotropia. Eye (Lond). https://doi.org/10.1038/s41433-019-0379-1
Luk AS, Yam JC, Lau HH, Yip WW, Young AL (2015) Surgical outcome of medial rectus resection in recurrent exotropia: a novel surgical formula. J Ophthalmol 2015:758463. https://doi.org/10.1155/2015/758463
Ren MY, Wang T, Wang Q, Guo JL, Wang LH (2015) Unilateral medial rectus resection for the treatment of recurrent exotropia in children. Jpn J Ophthalmol 59:341–345. https://doi.org/10.1007/s10384-015-0393-1
Yang HK, Hwang JM (2009) Bilateral vs unilateral medial rectus resection for recurrent exotropia after bilateral lateral rectus recession. Am J Ophthalmol 148:459–465. https://doi.org/10.1016/j.ajo.2009.04.017
Wang L, Nelson LB (2010) One muscle strabismus surgery. Curr Opin Ophthalmol 21:335–340. https://doi.org/10.1097/ICU.0b013e32833bd953
Koklanis K, Georgievski Z (2009) Recurrence of intermittent exotropia: factors associated with surgical outcomes. Strabismus 17:37–40. https://doi.org/10.1080/09273970802678750
Lim SH, Hong JS, Kim MM (2011) Prognostic factors for recurrence with unilateral recess-resect procedure in patients with intermittent exotropia. Eye (Lond) 25:449–454. https://doi.org/10.1038/eye.2011.12
Bateman JB, Parks MM, Wheeler N (1983) Discriminant analysis of acquired esotropia surgery. Predictor variables for short- and long-term outcomes. Ophthalmology 90:1154–1159
Repka MX, Connett JE, Scott WE (1996) The one-year surgical outcome after prism adaptation for the management of acquired esotropia. Ophthalmology 103:922–928
Thorn F, Gwiazda J, Cruz AA, Bauer JA, Held R (1994) The development of eye alignment, convergence, and sensory binocularity in young infants. Invest Ophthalmol Vis Sci 35:544–553
McNeer KW, Tucker MG, Spencer RF (1997) Botulinum toxin management of essential infantile esotropia in children. Arch Ophthalmol 115:1411–1418
Yam JC, Chong GS, Wu PK, Wong US, Chan CW, Ko ST (2014) Predictive factors affecting the short term and long term exodrift in patients with intermittent exotropia after bilateral rectus muscle recession and its effect on surgical outcome. Biomed Res Int 2014:482093. https://doi.org/10.1155/2014/482093
Scott WE, Keech R, Mash AJ (1981) The postoperative results and stability of exodeviations. Arch Ophthalmol 99:1814–1818
Kim WJ, Kim MM (2014) The clinical course of recurrent intermittent exotropia following one or two surgeries over 24 months postoperatively. Eye (Lond) 28:819–824. https://doi.org/10.1038/eye.2014.93
Choi YM, Lee JY, Jung JH, Kim SH, Cho YA (2013) Risk factors predicting the need for additional surgery in consecutive esotropia. J Pediatr Ophthalmol Strabismus 50:335–339. https://doi.org/10.3928/01913913-20130903-01
Moore S (1969) The prognostic value of lateral gaze measurements in intermittent exotropia. Am Orthopt J 19:69–71
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Supplementary figure 1
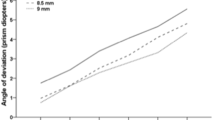
The course of post-operative angle of deviation following BLR for intermittent exotropia. The two groups did not show significant differences in exodrift during the 2 years of follow-up in both near deviation (A) and distant deviation (B) except for post-operative 1 year. (*P value <0.05.) (PPTX 1085 kb)
Rights and permissions
About this article
Cite this article
Lee, J.S., Han, J. & Han, SH. Risk factors associated with poor outcome after medial rectus resection for recurrent intermittent exotropia. Graefes Arch Clin Exp Ophthalmol 258, 445–450 (2020). https://doi.org/10.1007/s00417-019-04510-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-019-04510-z