Abstract
Background
Symptoms may be unreliable to diagnose gastroesophageal reflux disease (GERD) in patients with minor psychiatric disorders (MPD). This study aims to evaluate the influence of MPD in the diagnosis of GERD.
Methods
We prospectively studied 245 patients (based on a sample size calculation) with suspected GERD. All patients underwent manometry and pH monitoring and MPD evaluation based on the Hospital Anxiety and Depression Scale (HADS).
Results
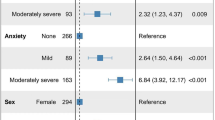
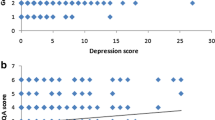
Based on the results of the pH monitoring, patients were classified as GERD + (n = 136, 55% of the total, mean age 46 years, 47% females) or GERD − (n = 109, 45% of the total, mean age 43 years, 60% females). The mean HADS score for GERD + and GERD − for anxiety was 7.8 and 8.5, respectively (p = 0.8) and for depression was 5.4 and 6.1, respectively (p = 0.1). DeMeester score (DS) did not correlate with total HADS score (p = 0.08) or depression domain (p = 0.9) but there was a negative correlation between DS and anxiety level (p < 0.001). A significant threshold accuracy value for HADS to diagnose GERD was not found on receiver operating characteristics curve analysis.
Conclusion
Almost half of the patients evaluated for GERD did not have the disease on objective evaluation. GERD + and GERD − patients had similar levels of MPD. However, the amount of reflux correlated negatively with the severity of anxiety. Symptoms and HADS cannot accurately diagnose or exclude GERD. pH monitoring should be more liberally used especially in patients with high levels of anxiety.


Similar content being viewed by others
References
Vakil N et al (2006) The Montreal definition and classification of gastroesophageal reflux disease: a global evidence-based consensus. Am J Gastroenterol 101(8):1900–1920. (quiz 1943)
El-Serag HB et al (2014) Update on the epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut 63(6):871–880
Dent J et al (2010) Accuracy of the diagnosis of GORD by questionnaire, physicians and a trial of proton pump inhibitor treatment: the Diamond Study. Gut 59(6):714–721
Nasi A et al (2001) Gastroesophageal reflux disease: comparison between patients with and without esophagitis, concerning age, gender and symptoms. Arq Gastroenterol 38(2):109–115
Moraes-Filho JP et al (2010) Guidelines for the diagnosis and management of gastroesophageal reflux disease: an evidence-based consensus. Arq Gastroenterol 47(1):99–115
Andolfi C et al (2016) Importance of esophageal manometry and pH monitoring in the evaluation of patients with refractory gastroesophageal reflux disease: a multicenter study. J Laparoendosc Adv Surg Tech A 26(7):548–550
Olden KW (2008) Psychosocial factors in functional gastrointestinal disorders: an evolving phenomenon. Neurogastroenterol Motil 20(Suppl 1):114–120
Aziz Q et al (2016) Functional esophageal disorders. Gastroenterology. https://doi.org/10.1053/j.gastro.2016.02.012
Nunez-Rodriguez MH, Miranda A, Sivelo (2008) Psychological factors in gastroesophageal reflux disease measured by scl-90-R questionnaire. Dig Dis Sci 53(12):3071–3075
Lee KJ et al (2009) Demographic, clinical, and psychological characteristics of the heartburn groups classified using the Rome III criteria and factors associated with the responsiveness to proton pump inhibitors in the gastroesophageal reflux disease group. Digestion 79(3):131–136
Wiklund I et al (2006) Psychological factors as a predictor of treatment response in patients with heartburn: a pooled analysis of clinical trials. Scand J Gastroenterol 41(3):288–293
Velanovich V, Karmy-Jones R (2001) Psychiatric disorders affect outcomes of antireflux operations for gastroesophageal reflux disease. Surg Endosc 15(2):171–175
Del Grande LM, Herbella FA, Bigatao AM, Abrao H, Jardim JR, Patti MG (2016) Pathophysiology of gastroesophageal reflux in patients with chronic pulmonary obstructive disease is linked to an increased transdiaphragmatic pressure gradient and not to a defective esophagogastric barrier. J Gastrointest Surg 20(1):104–110
DeMeester TR et al (1980) Technique, indications, and clinical use of 24 hour esophageal pH monitoring. J Thorac Cardiovasc Surg 79(5):656–670
Zigmond AS, Snaith RP (1983) The hospital anxiety and depression scale. Acta Psychiatr Scand 67(6):361–370
Andrade LH et al (2012) Mental disorders in megacities: findings from the Sao Paulo megacity mental health survey, Brazil. PLoS ONE 7(2):e31879
Avidan B et al (2001) Reflux symptoms are associated with psychiatric disease. Aliment Pharmacol Ther 15(12):1907–1912
Martin-Merino E et al (2010) Depression and treatment with antidepressants are associated with the development of gastro-oesophageal reflux disease. Aliment Pharmacol Ther 31(10):1132–1140
Hartono JL, Mahadeva S, Goh KL (2012) Anxiety and depression in various functional gastrointestinal disorders: do differences exist? J Dig Dis 13(5):252–257
Jansson C et al (2007) Severe gastro-oesophageal reflux symptoms in relation to anxiety, depression and coping in a population-based study. Aliment Pharmacol Ther 26(5):683–691
Baker LH, Lieberman D, Oehlke M (1995) Psychological distress in patients with gastroesophageal reflux disease. Am J Gastroenterol 90(10):1797–1803
Mykletun A et al (2010) Prevalence of mood and anxiety disorder in self reported irritable bowel syndrome (IBS). An epidemiological population based study of women. BMC Gastroenterol 10:88
Kessing BF et al (2015) Effects of anxiety and depression in patients with gastroesophageal reflux disease. Clin Gastroenterol Hepatol 13(6):1089–195.e1
Neto SC et al (2014) Ratio between proximal/distal gastroesophageal reflux does not discriminate abnormal proximal reflux. World J Surg 38(4):890–896
Oh JH et al (2009) Relationship between psychological factors and quality of life in subtypes of gastroesophageal reflux disease. Gut Liver 3(4):259–265
O’Boyle CJ et al (2002) Preoperative prediction of long-term outcome following laparoscopic fundoplication. ANZ J Surg 72(7):471–475
Taft TH et al (2018) Validation of the oesophageal hypervigilance and anxiety scale for chronic oesophageal disease. Aliment Pharmacol Ther 47(9):1270–1277
Boltin D et al (2013) Psychological distress is not associated with treatment failure in patients with gastroesophageal reflux disease. J Psychosom Res 75(5):462–466
Yang XJ et al (2015) Anxiety and depression in patients with gastroesophageal reflux disease and their effect on quality of life. World J Gastroenterol 21(14):4302–4309
Kimura Y et al (2016) Persistent reflux symptoms cause anxiety, depression, and mental health and sleep disorders in gastroesophageal reflux disease patients. J Clin Biochem Nutr 59(1):71–77
Bilgi MM et al (2017) Prevalence of psychiatric comorbidity in symptomatic gastroesophageal reflux subgroups. Dig Dis Sci 62(4):984–993
Okuyama M et al (2017) Associations among gastroesophageal reflux disease, psychological stress, and sleep disturbances in Japanese adults. Scand J Gastroenterol 52(1):44–49
Javadi S, Shafikhani AA (2017) Anxiety and depression in patients with gastroesophageal reflux disorder. Electron Physician 9(8):5107–5112
Acknowledgements
We are indebted to Dr. Sun Rein Lin to allow his patients to be included in the study; Ms. Eliane Francisco for her invaluable assistance with IRB bureaucracy and Edkerly Noronha, NP and her team for priceless help to perform the esophageal functions tests.
Author information
Authors and Affiliations
Contributions
RMLN: Protocol/project development; data collection or management; data analysis; manuscript writing/editing. FAMH: Protocol/project development; data collection or management; data analysis; manuscript writing/editing. AZ: Protocol/project development. VV: Protocol/project development; data collection or management; manuscript writing/editing. BM: Data collection or management. FS: Manuscript writing/editing. MGP: Manuscript writing/editing. All authors contributed sufficiently to be named as authors and are responsible for the manuscript. No professional or ghost writer was hired.
Corresponding author
Ethics declarations
Disclosures
Rafael Melillo Laurino Neto, Fernando A. M. Herbella, Andre Zugman, Vic Velanovich, Beth Montera, Francisco Schlottmann, and Marco G. Patti, MD have no conflicts of interest or financial ties to disclose.
Ethical approval
The study protocol was approved by the local Ethics Committee, and written informed consent was obtained from each subject.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Neto, R.M.L., Herbella, F.A.M., Zugman, A. et al. Minor psychiatric disorders and objective diagnosis of gastroesophageal reflux disease. Surg Endosc 33, 4116–4121 (2019). https://doi.org/10.1007/s00464-019-06716-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-06716-y