Abstract
Background
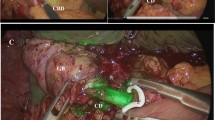
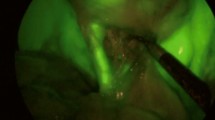
The aim is to evaluate safety and efficacy of near infra-red (NIR) indocyanine green (ICG) fluorescence structural imaging during laparoscopic cholecystectomy (LC) (Group A) and to compare perioperative data, including operative time, with a series of patients who underwent LC with routine traditional intraoperative cholangiography (IOC) (Group B).
Methods
Forty-four patients with acute or chronic cholecystitis underwent NIR-ICG fluorescent cholangiography during LC. ICG was administered intravenously at different time intervals or by direct gallbladder injection during surgery. Fluorescence intensity and anatomy identification were scored according to a visual analogue scale between 1 (least accurate) and 5 (most accurate). Group B patients (n = 44) were chosen from a prospectively maintained database of patients who underwent LC with routine IOC, matched for age, sex, body mass index, and diagnosis with group A patients.
Results
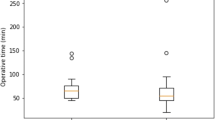
No adverse reactions were recorded. In group A, mean time between intravenous administration of ICG and surgery was 10.7 ± 8.2 (range 2–52) h. Administered doses ranged from 3.5 to 13.5 mg. Fluorescence was present in all cases, scoring ≥ 3 in 41 patients. Mean operative time was 86.9 ± 36.9 (30–180) min in group A and 117.9 ± 43.4 (40–220) min in group B (p = 0.0006). No conversion to open surgery nor bile duct injuries were observed in either group.
Conclusions
LC with NIR-ICG fluorescent cholangiography is safe and effective for early recognition of anatomical landmarks, reducing operative time as compared to LC with IOC, even when residents were the main operator. NIR-ICG fluorescent cholangiography was effective in patients with acute cholecystitis and in the obese. Data collection into large registries on the results of NIR-ICG fluorescent cholangiography during LC should be encouraged to establish whether this technique might set a new safety standard for LC.


Similar content being viewed by others
References
Pucher PH, Brunt LM, Davies N, Linsk A, Munshi A, Rodriguez HA, Fingerhut A, Fanelli RD, Asbun H, Aggarwal R, SAGES Safe Cholecystectomy Task Force (2018) Outcome trends and safety measures after 30 years of laparoscopic cholecystectomy: a systematic review and pooled data analysis. Surg Endosc 32(5):2175–2183. https://doi.org/10.1007/s00464-017-5974-2
National Center for Health Statistics. Health, United States, 2009. In Brief—medical technology (2010). https://www.cdc.gov/nchs/data/hus/hus09_InBrief_MedicalTech.pdf. Accessed 4 Jan 2019
Flum DR, Dellinger EP, Cheadle A, Chan L, Koepsell T (2003) Intraoperative cholangiography and risk of common bile duct injury during cholecystectomy. JAMA 289(13):1639–1644
Gartland RM, Bloom JP, Fong ZV, DeRoo C, Dwyer K, Quinn G, Lillemoe K, Mort E (2018) What have we learned from malpractice claims involving the surgical management of benign biliary disease?: A 128 million dollar question. Ann Surg. https://doi.org/10.1097/sla.0000000000003155
Harboe KM, Bardram L (2011) The quality of cholecystectomy in Denmark: outcome and risk factors for 20,307 patients from the national database. Surg Endosc 25(5):1630–1641. https://doi.org/10.1007/s00464-010-1453-8
Navez B, Ungureanu F, Michiels M, Claeys D, Muysoms F, Hubert C, Vanderveken M, Detry O, Detroz B, Closset J, Devos B, Kint M, Navez J, Zech F, Gigot JF, Belgian Group for Endoscopic Surgery (BGES) and the Hepatobiliary and Pancreatic Section (HBPS) of the Royal Belgian Society of Surgery (2012) Surgical management of acute cholecystitis: results of a 2-year prospective multicenter survey in Belgium. Surg Endosc 26(9):2436–2445
Törnqvist B, Strömberg C, Akre O, Enochsson L, Nilsson M (2015) Selective intraoperative cholangiography and risk of bile duct injury during cholecystectomy. Br J Surg 102(8):952–958. https://doi.org/10.1002/bjs.9832
Törnqvist B, Strömberg C, Persson G, Nilsson M (2012) Effect of intended intraoperative cholangiography and early detection of bile duct injury on survival after cholecystectomy: population based cohort study. BMJ 345:e6457. https://doi.org/10.1136/bmj.e6457
Waage A, Nilsson M (2006) Iatrogenic bile duct injury: a population- based study of 152 776 cholecystectomies in the Swedish inpatient registry. Arch Surg 141(12):1207–1213
Dolan JP, Diggs BS, Sheppard BC, Hunter JG (2005) Ten-year trend in the national volume of bile duct injuries requiring operative repair. Surg Endosc 19(7):967–973
Landman MP, Feurer ID, Moore DE, Zaydfudim V, Pinson CW (2013) The long-term effect of bile duct injuries on health-related quality of life: a meta-analysis. HPB (Oxford) 15(4):252–259. https://doi.org/10.1111/j.1477-2574.2012.00586.x
Fletcher DR, Hobbs MS, Tan P, Valinsky LJ, Hockey RL, Pikora TJ, Knuiman MW, Sheiner HJ, Edis A (1999) Complications of cholecystectomy: risks of the laparoscopic approach and protective effects of operative cholangiography: a population-based study. Ann Surg 229(4):449–457
Fingerhut A, Dziri C, Garden OJ, Gouma D, Millat B, Neugebauer E, Paganini A, Targarona E (2013) ATOM, the all-inclusive, nominal EAES classification of bile duct injuries during cholecystectomy. Surg Endosc 27(12):4608–4619. https://doi.org/10.1007/s00464-013-3081-6
Rystedt JML, Tingstedt B, Montgomery F, Montgomery AK (2017) Routine intraoperative cholangiography during cholecystectomy is a cost-effective approach when analysing the cost of iatrogenic bile duct injuries. HPB (Oxford) 19(10):881–888. https://doi.org/10.1016/j.hpb.2017.06.004
Dip FD, Asbun D, Rosales-Velderrain A, Lo Menzo E, Simpfendorfer CH, Szomstein S, Rosenthal RJ (2014) Cost analysis and effectiveness comparing the routine use of intraoperative fluorescent cholangiography with fluoroscopic cholangiogram in patients undergoing laparoscopic cholecystectomy. Surg Endosc 28(6):1838–1843. https://doi.org/10.1007/s00464-013-3394-5
Strasberg SM, Hertl M, Soper NJ (1995) An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surg 180(1):101–125
Booij KA, de Reuver PR, Nijsse B, Busch OR, van Gulik TM, Gouma DJ (2014) Insufficient safety measures reported in operation notes of complicated laparoscopic cholecystectomies. Surgery 155(3):384–389. https://doi.org/10.1016/j.surg.2013.10.010.epub
Deal SB, Stefanidis D, Telem D, Fanelli RD, McDonald M, Ujiki M, Michael Brunt L, Alseidi AA (2017) Evaluation of crowd-sourced assessment of the critical view of safety in laparoscopic cholecystectomy. Surg Endosc 31(12):5094–5100. https://doi.org/10.1007/s00464-017-5574-1
Boni L, David G, Mangano A, Dionigi G, Rausei S, Spampatti S, Cassinotti E, Fingerhut A (2015) Clinical applications of indocyanine green (ICG) enhanced fluorescence in laparoscopic surgery. Surg Endosc 29(7):2046–2055. https://doi.org/10.1007/s00464-014-3895-x
van den Bos J, Schols RM, Luyer MD, van Dam RM, Vahrmeijer AL, Meijerink WJ, Gobardhan PD, van Dam GM, Bouvy ND, Stassen LP (2016) Near-infrared fluorescence cholangiography assisted laparoscopic cholecystectomy versus conventional laparoscopic cholecystectomy (FALCON trial): study protocol for a multicentre randomised controlled trial. BMJ Open 6(8):e011668. https://doi.org/10.1136/bmjopen-2016-011668
Schols RM, Bouvy ND, van Dam RM, Masclee AA, Dejong CH, Stassen LP (2013) Combined vascular and biliary fluorescence imaging in laparoscopic cholecystectomy. Surg Endosc 27(12):4511–4517. https://doi.org/10.1007/s00464-013-3100-7
Ishizawa T, Bandai Y, Ijichi M, Kaneko J, Hasegawa K, Kokudo N (2010) Fluorescent cholangiography illuminating the biliary tree during laparoscopic cholecystectomy. Br J Surg 97(9):1369–1377. https://doi.org/10.1002/bjs.7125
Daskalaki D, Fernandes E, Wang X, Bianco FM, Elli EF, Ayloo S, Masrur M, Milone L, Giulianotti PC (2014) Indocyanine green (ICG) fluorescent cholangiography during robotic cholecystectomy: results of 184 consecutive cases in a single institution. Surg Innov 21(6):615–621. https://doi.org/10.1177/1553350614524839
European Fluorescence Imaging-Guided Surgery (EURO-FIGS registry). http://www.euro-figs.eu. Accessed 16 Jan 2019
Lezoche E, Paganini A, Guerrieri M, Carlei F, Lomanto D, Sottili M, Nardovino M (1994) Technique and results of routine dynamic cholangiography during 528 consecutive laparoscopic cholecystectomies. Surg Endosc 8(12):1443–1447
Graves C, Ely S, Idowu O, Newton C, Kim S (2017) Direct gallbladder indocyanine green injection fluorescence cholangiography during laparoscopic cholecystectomy. J Laparoendosc Adv Surg Tech A 27(10):1069–1073. https://doi.org/10.1089/lap.2017.0070
Quaresima S, Balla A, Guerrieri M, Campagnacci R, Lezoche E, Paganini AM (2017) A 23 year experience with laparoscopic common bile duct exploration. HPB (Oxford) 19(1):29–35. https://doi.org/10.1016/j.hpb.2016.10.011
Quaresima S, Balla A, Guerrieri M, Lezoche G, Campagnacci R, D’Ambrosio G, Lezoche E, Paganini AM (2016) Results of medium seventeen years’ follow-up after laparoscopic choledochotomy for ductal stones. Gastroenterol Res Pract 2016:9506406. https://doi.org/10.1155/2016/9506406
Takada T, Strasberg SM, Solomkin JS, Pitt HA, Gomi H, Yoshida M, Mayumi T, Miura F, Gouma DJ, Garden OJ, Büchler MW, Kiriyama S, Yokoe M, Kimura Y, Tsuyuguchi T, Itoi T, Gabata T, Higuchi R, Okamoto K, Hata J, Murata A, Kusachi S, Windsor JA, Supe AN, Lee S, Chen XP, Yamashita Y, Hirata K, Inui K, Sumiyama Y, Committee Tokyo Guidelines Revision (2013) TG13: Updated Tokyo Guidelines for the management of acute cholangitis and cholecystitis. J Hepatobiliary Pancreat Sci 20(1):1–7. https://doi.org/10.1007/s00534-012-0566-y
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibañes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250(2):187–196. https://doi.org/10.1097/SLA.0b013e3181b13ca2
Diana M, Soler L, Agnus V, D’Urso A, Vix M, Dallemagne B, Faucher V, Roy C, Mutter D, Marescaux J, Pessaux P (2017) Prospective evaluation of precision multimodal gallbladder surgery navigation: virtual reality, near-infrared fluorescence, and X-ray-based intraoperative cholangiography. Ann Surg 266(5):890–897. https://doi.org/10.1097/SLA.0000000000002400
Roy M, Dip F, Nguyen D, Simpfendorfer CH, Menzo EL, Szomstein S, Rosenthal RJ (2017) Fluorescent incisionless cholangiography as a teaching tool for identification of Calot’s triangle. Surg Endosc 31(6):2483–2490. https://doi.org/10.1007/s00464-016-5250-x
Way LW, Stewart L, Gantert W, Liu K, Lee CM, Whang K, Hunter JG (2003) Causes and prevention of laparoscopic bile duct injuries: analysis of 252 cases from a human factors and cognitive psychology perspective. Ann Surg 237(4):460–469
Ford JA, Soop M, Du J, Loveday BP, Rodgers M (2012) Systematic review of intraoperative cholangiography in cholecystectomy. Br J Surg 99(2):160–167. https://doi.org/10.1002/bjs.7809
Vlek SL, van Dam DA, Rubinstein SM, de Lange-de Klerk ESM, Schoonmade LJ, Tuynman JB, Meijerink WJHJ, Ankersmit M (2017) Biliary tract visualization using near-infrared imaging with indocyanine green during laparoscopic cholecystectomy: results of a systematic review. Surg Endosc 31(7):2731–2742. https://doi.org/10.1007/s00464-016-5318-7
Zroback C, Chow G, Meneghetti A, Warnock G, Meloche M, Chiu CJ, Panton ON (2016) Fluorescent cholangiography in laparoscopic cholecystectomy: the initial Canadian experience. Am J Surg 211(5):933–937. https://doi.org/10.1016/j.amjsurg.2016.01.013
Dip F, LoMenzo E, Sarotto L, Phillips E, Todeschini H, Nahmod M, Alle L, Schneider S, Kaja L, Boni L, Ferraina P, Carus T, Kokudo N, Ishizawa T, Walsh M, Simpfendorfer C, Mayank R, White K, Rosenthal RJ (2019) Randomized trial of near-infrared incisionless fluorescent cholangiography. Ann Surg. https://doi.org/10.1097/sla.0000000000003178
Millat B, Atger J, Deleuze A, Briandet H, Fingerhut A, Guillon F, Marrel E, De Seguin C, Soulier P (1997) Laparoscopic treatment for choledocholithiasis: a prospective evaluation in 247 consecutive unselected patients. Hepatogastroenterology 44(13):28–34
Tranter SE, Thompson MH (2003) A prospective single-blinded controlled study comparing laparoscopic ultrasound of the common bile duct with operative cholangiography. Surg Endosc 17(2):216–219
Dili A, Bertrand C (2017) Laparoscopic ultrasonography as an alternative to intraoperative cholangiography during laparoscopic cholecystectomy. World J Gastroenterol 23(29):5438–5450. https://doi.org/10.3748/wjg.v23.i29.5438
Eikermann M, Siegel R, Broeders I, Dziri C, Fingerhut A, Gutt C, Jaschinski T, Nassar A, Paganini AM, Pieper D, Targarona E, Schrewe M, Shamiyeh A, Strik M, Neugebauer EA, European Association for Endoscopic Surgery (2012) Prevention and treatment of bile duct injuries during laparoscopic cholecystectomy: the clinical practice guidelines of the European Association for Endoscopic Surgery (EAES). Surg Endosc 26(11):3003–3039. https://doi.org/10.1007/s00464-012-2511-1
Pucher PH, Brunt LM, Fanelli RD, Asbun HJ, Aggarwal R (2015) SAGES expert Delphi consensus: critical factors for safe surgical practice in laparoscopic cholecystectomy. Surg Endosc 29(11):3074–3085. https://doi.org/10.1007/s00464-015-4079-z
Balla A, Quaresima S, Corona M, Lucatelli P, Fiocca F, Rossi M, Bezzi M, Catalano C, Salvatori FM, Fingerhut A, Paganini AM (2018) ATOM classification of bile duct injuries during laparoscopic cholecystectomy: analysis of a single institution experience. J Laparoendosc Adv Surg Tech A. https://doi.org/10.1089/lap.2018.0413
Strasberg SM, Brunt LM (2017) The critical view of safety: why it is not the only method of ductal identification within the standard of care in laparoscopic cholecystectomy. Ann Surg 265(3):464–465. https://doi.org/10.1097/SLA.0000000000002054
Kawaguchi Y, Ishizawa T, Miyata Y, Yamashita S, Masuda K, Satou S, Tamura S, Kaneko J, Sakamoto Y, Aoki T, Hasegawa K, Sugawara Y, Kokudo N (2013) Portal uptake function in veno-occlusive regions evaluated by real-time fluorescent imaging using indocyanine green. J Hepatol 58(2):247–253. https://doi.org/10.1016/j.jhep.2012.09.028
Verbeek FP, Schaafsma BE, Tummers QR, van der Vorst JR, van der Made WJ, Baeten CI, Bonsing BA, Frangioni JV, van de Velde CJ, Vahrmeijer AL, Swijnenburg RJ (2014) Optimization of near-infrared fluorescence cholangiography for open and laparoscopic surgery. Surg Endosc 28(4):1076–1082
Gutt CN, Encke J, Köninger J, Harnoss JC, Weigand K, Kipfmüller K, Schunter O, Götze T, Golling MT, Menges M, Klar E, Feilhauer K, Zoller WG, Ridwelski K, Ackmann S, Baron A, Schön MR, Seitz HK, Daniel D, Stremmel W, Büchler MW (2013) Acute cholecystitis: early versus delayed cholecystectomy, a multicenter randomized trial (ACDCstudy, NCT00447304). Ann Surg 258(3):385–393. https://doi.org/10.1097/SLA.0b013e3182a1599b
Boni L, Cassinotti EC, David G, Marzorati AM, Fingerhut A (2015) Indocyanine green-enhanced fluorescence cholangiography in laparoscopic cholecystectomy: experience from 100 cases. J Am Coll Surg 221(4):S71
Osayi SN, Wendling MR, Drosdeck JM, Chaudhry UI, Perry KA, Noria SF, Mikami DJ, Needleman BJ, Muscarella P 2nd, Abdel-Rasoul M, Renton DB, Melvin WS, Hazey JW, Narula VK (2015) Nera-infrared fluorescent cholangiography facilitates identification of biliary anatomy during laparoscopic cholecystectomy. Surg Endosc 29(2):368–375. https://doi.org/10.1007/s00464-014-3677-5
Dip F, Nguyen D, Montorfano L, Szretter Noste ME, Lo Menzo E, Simpfendorfer C, Szomstein S, Rosenthal R (2016) Accuracy of near infrared-guided surgery in morbidly obese subjects undergiong laparoscopic cholecystectomy. Obes Surg 26(3):525–530. https://doi.org/10.1007/s11695-015-1781-9
Liu YY, Kong SH, Diana M, Lègner A, Wu CC, Kameyama N, Dallemagne B, Marescaux J (2016) Near-infrared cholecysto-cholangiography with indocyanine green may secure cholecystectomy in difficult clinical situations: proof of the concept in a porcine model. Surg Endosc 30(9):4115–4123. https://doi.org/10.1007/s00464-015-4608-9
Ankersmit M, van Dam DA, van Rijswijk AS, van den Heuvel B, Tuynman JB, Meijerink WJHJ (2017) Fluorescent imaging with indocyanine green during laparoscopic cholecystectomy in patients at increased risk of bile duct injury. Surg Innov 24(3):245–252. https://doi.org/10.1177/1553350617690309
Bergamaschi R, Ignjatovic D (2000) More than two structures in Calot’s triangle. A postmortem study. Surg Endosc 14(4):354–357
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Silvia Quaresima, Andrea Balla, Livia Palmieri, Ardit Seitaj, Abe Fingerhut, Pietro Ursi, and Alessandro M. Paganini declare that they have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Quaresima, S., Balla, A., Palmieri, L. et al. Routine near infra-red indocyanine green fluorescent cholangiography versus intraoperative cholangiography during laparoscopic cholecystectomy: a case-matched comparison. Surg Endosc 34, 1959–1967 (2020). https://doi.org/10.1007/s00464-019-06970-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-06970-0