Abstract
Background
Rapid weight loss is associated with a high incidence of cholelithiasis.
Objectives
To identify the incidence of gallstone formation after weight loss surgery and to detect the efficacy of 6 months regimen of prophylactic Ursodeoxycholic acid (UDCA).
Methods
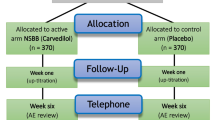
RCT included a total of 1530 morbid obese patients who were subjected to either laparoscopic one anastomosis gastric bypass (OAGB), sleeve gastrectomy (SG), or greater curve plication (GCP). Patients with previous or concomitant cholecystectomy and missed follow-up were excluded, leaving 1432 patients to analyze. They were randomly allocated into two groups receiving either UDCA or placebo with a minimum follow-up of one year for assessment of cholelithiasis and weight loss.
Results
The overall incidence of cholelithiasis after surgery was 9.7%. There was a significant decrease in the incidence of gallstone formation from 22% in placebo to 6.5% in treated group with UDCA. The mean percentage of excess weight loss (%EWL) was significantly higher in those who develop gallstones than others. Of those developing gallstones, there was 64.7 % with SG versus 28.1% and 7.2% in OAGB and GCP, respectively, which is statistically significant. NNT to prevent cholelithiasis is six, AR% is 70.4%, and RR is 3.4%.
Conclusions
Cholelithiasis after SG and OAGB was higher than GCP. %EWL was rapid and higher in OAGB and SG contributing to the higher rate of symptomatic cholelithiasis and could be predictive for post-bariatric cholelithiasis. A 6-month use of UDCA is an effective prophylaxis decreasing gallstone formation after bariatric surgery at short-term follow-up.

Similar content being viewed by others
References
Sunyer FX (1996) A review of long-term studies evaluating the efficacy in weight loss ameliorating disorders associated with obesity. Clin Ther 18:1006–1035
Buchwald H, Avidor Y, Braunwald E, Jensen MD, Pories W, Fahrbach K (2004) Bariatric surgery: a systematic review and meta-analysis. JAMA 292(14):1724–1737
De Maria EJ (2007) Bariatric surgery for morbid obesity. N Engl J Med 356(21):2176–2183
Holst JJ, Madsbad S, Bojsen-Møller KN, Svane MS, Jørgensen NB, Carsten D et al (2018) Mechanisms in bariatric surgery: gut hormones, diabetes resolution, and weight loss. Surg Obes Relat Dis 14:708–714
Dimitriadis GK, Randeva MS, Miras AD (2017) Potential hormone mechanisms of bariatric surgery. Curr Obes Rep 6:253–265
Brody F (2004) Minimally invasive surgery for morbid obesity. Clevel Clin J Med 71(4):289–298
Miller K, Hell E, Lang B, Lengauer E (2003) Gallstone formation prophylaxis after gastric restrictive procedures for weight loss: a randomized double-blind placebo-controlled trial. Ann Surg 238:697–702
Shiffman ML, Sugerman HJ, Kellum JM, Moore EW (1992) Changes in gallbladder bile composition following gallstone formation and weight reduction. Gastroenterology 103:214–221
Boerlage TCC, Haal S, de Brauw LM, Acherman YIZ, Bruin S, Van de Laar AW et al (2017) Ursodeoxycholic acid for the prevention of symptomatic gallstone disease after bariatric surgery: study protocol for a randomized controlled trial (UPGRADE trial). BMC Gastroenterol 17(1):164. https://doi.org/10.1186/s12876-017-0674-x
Deitel M, Petrov I (1987) Incidence of symptomatic gallstones after bariatric operations. Surg Gynecol Obstet 164:549–552
International Federation for the Surgery of Obesity (1997) Statement on patient selection for bariatric surgery. Obes Surg 7:41
Mason EE (2002) Gallbladder management in obesity surgery. Obes Surg 12(2):222–229
Wattchow DA, Hall JC, Whiting MJ, Bradley B, Iannos J, Watts JM (1983) Prevalence and treatment of gallstones after gastric bypass surgery for morbid obesity. Br Med J Clin Res 286:763
Angrisani L, Lorenzo M, De Palma G, Sivero L, Catanzano C, Tesauro B et al (1995) Laparoscopic cholecystectomy in obese patients compared with nonobese patients. Surg Laparosc Endosc 5:197–201
Festi D, Colecchia A, Larocca A, Villanova N, Mazzella G, Petroni ML et al (2000) Review: low caloric intake and gall-bladder motor function. Aliment Pharmacol Ther 14(2):51–53
Everhart JE (1993) Contributions of obesity and weight loss to gallstone disease. Ann Intern Med 119:1029–1035
Shiffman ML, Shamburek RD, Schwartz CC, Sugerman HJ, Kellum JM, Moore EW (1993) Gallbladder mucin, arachidonic acid, and bile lipids in patients who develop gallstones during weight reduction. Gastroenterology 105:1200–1208
Shiffman ML, Sugerman HJ, Kellum JH, Brewer WH, Moore EW (1993) Gallstones in patients with morbid obesity. Relationship to body weight, weight loss and gallbladder bile cholesterol solubility. Int J Obes Relat Metab Disord 17:153–158
Dittrick GW, Thompson JS, Campos D, Bremers D, Sudan D (2005) Gallbladder pathology in morbid obesity. Obes Surg 15(2):238–242
Tucker ON, Fajnwaks P, Szomstein S, Rosenthal RJ (2008) Is concomitant cholecystectomy necessary in obese patients undergoing laparoscopic gastric bypass surgery? Surg Endosc 22(11):2450–2454
Portenier DD, Grant JP, Blackwood HS, Pryor A, McMahon RL, DeMaria E (2007) Expectant management of the asymptomatic gallbladder at Roux-en-Y gastric bypass. Surg Obes Relat Dis 3(4):476–479
Papasavas PK, Gagné DJ, Ceppa FA, Caushaj PF (2006) Routine gallbladder screening not necessary in patients undergoing laparoscopic Roux-en-Y gastric bypass. Surg Obes Relat Dis 2(1):41–46
Villegas L, Schneider B, Provost D, Chang C, Scott D, Sims T et al (2004) Is routine cholecystectomy required during laparoscopic gastric bypass? Obes Surg 14(2):206–211
Ryia MH, Abd-Allah HS, Khadrawy OH, Moussa GI (2014) Predictors of gallstone formation in morbidly obese patients after bariatric surgery: a retrospective observational study. Surg Sci 5:1–5
Oliveira CIB, Chaim EA, Silva BB (2003) Impact of rapid weight reduction on risk of cholelithiasis after bariatric surgery. Obes Surg 13(4):625–628
Yang H, Peterson GM, Roth MP, Schoenfield LJ, Marks JW (1992) Risk factors for gallstones formation during rapid loss of weight. Dig Dis Sci 37(6):912–918
Uy MC, Talingdan-Te MC, Espinosa WZ, Daez ML, Ong JP (2008) Ursodeoxycholic acid in the prevention of gallstone formation after bariatric surgery: a meta-analysis. Obes Surg 18(12):1532–1538
Wudel LJ, Wright JK, Debelak JP, Allos TM, Shyr Y, Chapman WC (2002) Prevention of gallstone formation in morbidly obese patients undergoing rapid weight loss: results of a randomized controlled pilot study. J Surg Res 102(1):50–56
Sugerman HJ, Brewer WH, Shiffman ML, Brolin RE, Fobi MA, Linner JH (1995) A multicenter, placebo-controlled, randomized, double-blind, prospective trial of prophylactic ursodiol for the prevention of gallstone formation following gastric-bypass-induced rapid weight loss. Am J Surg 169:91–96 (Discussion 96–97)
Li VK, Pulido N, Fajnwaks P, Szomstein S, Rosenthal R, Duartez P (2009) Predictors of gallstone formation after bariatric surgery: a multivariate analysis of risk factors comparing gastric bypass, gastric banding, and sleeve gastrectomy. Surg Endosc 23(7):1640–1644
Cirillo DJ, Wallace RB, Rodabough RJ, Greenland P, LaCroix AZ, Limacher MC (2005) Effect of estrogen therapy on gallbladder disease. JAMA 293:330–339
Schmidt JH, Hocking MP, Rout WR, Woodward ER (1988) The case for prophylactic cholecystectomy concomitant with gastric restriction for morbid obesity. Am Surg 54:269–272
Shiffman ML, Sugerman HJ, Kellum JM, Brewer WH, Moore EW (1991) Gallstone formation after rapid weight loss: a prospective study in patients undergoing gastric bypass surgery for treatment of morbid obesity. Am J Gastroentrol 86(8):1000–1005
Miller K, Höller E, Hell E (2002) Restrictive procedures in the treatment of morbid obesity: vertical banded gastroplasty vs. adjustable gastric banding. Zentralbl Chir 127:1038–1043
Jonas E, Marsk R, Rasmussen F, Freedman J (2010) Incidence of postoperative gallstone disease after antiobesity surgery: population-based study from Sweden. Surg Obes Relat Dis 6:54–58
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Ahmed Talha, Tamer Abdelbaki, Ayman Farouk, Ehab Hasouna, Eman Azzam, and Gihan Shehata have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Talha, A., Abdelbaki, T., Farouk, A. et al. Cholelithiasis after bariatric surgery, incidence, and prophylaxis: randomized controlled trial. Surg Endosc 34, 5331–5337 (2020). https://doi.org/10.1007/s00464-019-07323-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-07323-7