Abstract
Background
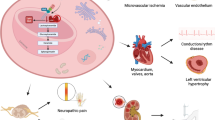
Pompe disease (PD) is a lysosomal glycogen storage disorder caused by a deficiency in acid α-glucosidase (GAA) activity. Various organs, including the skeletal muscle, cardiac muscle, and liver, are commonly involved. Early initiation of enzyme replacement therapy (ERT) with recombinant human α-glucosidase (rhGAA) can improve the outcome. However, some patients experience a poor clinical course despite ERT because of the emergence of anti-rhGAA antibodies that neutralize rhGAA. Treatment against anti-rhGAA antibodies is challenging.
Case–diagnosis/treatment
A 14-year-old boy with late-onset PD was referred to our hospital with proteinuria detected by school urinalysis screening. He was diagnosed with PD at the age of 4 years based on muscle biopsy and decreased GAA activity. Treatment with rhGAA was initiated, but anaphylaxis occurred frequently. Anti-rhGAA antibodies were detected and immune tolerance therapy was therefore given, but his antibody titer remained high. Kidney biopsy revealed stage II membranous nephropathy. Immunohistochemistry staining revealed anti-rhGAA antibody/rhGAA immune complexes along the glomerular capillary loop. Aggressive immunotherapy combined with bortezomib and rituximab was then initiated. Serum levels of anti-rhGAA antibodies decreased significantly and his proteinuria finally resolved.
Conclusions
There have been few reports of membranous nephropathy associated with ERT for PD. We clarified the cause in the current patient. Bortezomib and rituximab effectively suppressed anti-rhGAA antibody production resulting in the resolution of proteinuria and maintenance of ERT efficacy.


Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article.
References
Kishnani PS, Steiner RD, Bali D, Berger K et al (2006) Pompe disease diagnosis and management guideline. Genet Med 8:267–288. https://doi.org/10.1097/01.gim.0000218152.87434.f3
Kishnani PS, Corzo D, Nicolino M, Byrne B et al (2007) Recombinant human acid α-glucosidase: major clinical benefits in infantile-onset Pompe disease. Neurology 68:99–109. https://doi.org/10.1212/01.wnl.0000251268.41188.04
Chien YH, Lee NC, Thurberg BL, Chiang SC et al (2009) Pompe disease in infants: improving the prognosis by newborn screening and early treatment. Pediatrics 124:e1116–e1125. https://doi.org/10.1542/peds.2008-3667
Toscano A, Schoser B (2013) Enzyme replacement therapy in late-onset Pompe disease: a systematic literature review. J Neurol 260:951–959. https://doi.org/10.1007/s00415-012-6636-x
Hanna D, Vassili V, Olivia B, Laure-Helene N et al (2014) Allo-immune membranous nephropathy and recombinant aryl sulfatase replacement therapy: a need for tolerance induction therapy. J Am Soc Nephrol 25:675–680. https://doi.org/10.1681/ASN.2013030290
Hunley TE, Corzo D, Dudek M, Kishnani PS et al (2004) Nephrotic syndrome complicating alpha-glucosidase replacement therapy for Pompe disease. Pediatrics 114:e532–e535. https://doi.org/10.1542/peds.2003-0988-L
Banugaria SG, Prater SN, Ng YK, Kobori JA et al (2011) The impact of antibodies on clinical outcomes in diseases treated with therapeutic protein: lessons learned from infantile Pompe disease. Genet Med 13:729–736. https://doi.org/10.1097/GIM.0b013e3182174703
Banugaria SG, Patel TT, Mackey J, Das S et al (2012) Persistence of high sustained antibodies to enzyme replacement therapy despite extensive immuno-modulatory therapy in an infant with Pompe disease: need for agents to target antibody-secreting plasma cells. Mol Genet Metab 105:677–680. https://doi.org/10.1016/j.ymgme.2012.01.019
Kishnani PS, Goldenberg PC, DeArmey SL, Heller J et al (2010) Cross-reactive immunologic material status affects treatment outcomes in Pompe disease infants. Mol Genet Metab 99:26–33. https://doi.org/10.1016/j.ymgme.2009.08.003
Markic J, Polic B, Stricevic L, Metlicic V et al (2014) Effects of immune modulation therapy in the first Croatian infant diagnosed with Pompe disease: a 3-year follow-up study. Wien Klin Wochenschr 126:133–137. https://doi.org/10.1007/s00508-013-0475-3
Rohrbach M, Klein A, Kohli-Wiesner A, Veraguth D et al (2010) CRIM-negative infantile Pompe disease: 42-month treatment outcome. J Inherit Metab Dis 33:751–757. https://doi.org/10.1007/s10545-010-9209-0
van Kooten HA, Ditters IAM, Hoogeveen-Westerveld M, Jacobs EH (2022) Antibodies against recombinant human alpha-glucosidase do not seem to affect clinical outcome in childhood onset Pompe disease. Orpanet J Rare Dis 17:31. https://doi.org/10.1186/s13023-022-02175-2
Mendelsohn NJ, Messinger YH, Rosenberg AS, Kishnani PS (2009) Elimination of antibodies to recombinant enzyme in Pompe’s disease. N Engl J Med 360:194–195. https://doi.org/10.1056/NEJMc0806809
Everly MJ, Everly JJ, Susskind B, Brailey P et al (2008) Bortezomib provides effective therapy for antibody- and cell-mediated acute rejection. Transplantation 86:1754–1761. https://doi.org/10.1097/TP.0b013e318190af83
Stenger EO, Kazi Z, Lisi E, Gambello MJ, Kishnani PS (2015) Immune tolerance strategies in siblings with infantile Pompe disease-advantages for a preemptive approach to high-sustained antibody titers. Mol Genet Metab Rep 4:30–34. https://doi.org/10.1016/j.ymgmr.2015.05.004
Acknowledgements
We are grateful to Dr. Koji Muroya, Department of Endocrinology and Metabolism, Kanagawa Children’s Medical Center, for his medical advice, and to Professor Kenichi Ohashi, Jikei University School of Medicine, for providing the anti-rhGAA antibody. We thank Melissa Crawford, PhD, and Susan Furness, PhD, from Edanz (https://jp.edanz.com/ac) for editing drafts of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sasaki, K., Uchimura, T., Inaba, A. et al. Aggressive immunotherapy combined with bortezomib and rituximab for membranous nephropathy associated with enzyme replacement therapy in Pompe disease. Pediatr Nephrol 38, 921–925 (2023). https://doi.org/10.1007/s00467-022-05672-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-022-05672-5