Abstract
Background
Surgery has not been proven to be a better treatment option than non-operative management for limb paresis due to lumbar disc herniation. For the patients it will still be a concern, whether they will regain full strength after the operation or not.
Methods
A prospective cohort study of 91 patients with preoperative paresis due to disc herniation with 1-year follow up was carried out. The primary outcome was muscle strength in affected limb, and the secondary outcome was self-reported symptoms on back and leg pain, disability, health related quality of life, general health and working capability.
Results
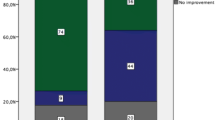
Seventy-five percent of patients had no paresis 1 year after the operation. The severity of the paresis was the only predictor for persistent paresis. Preoperative duration of the paresis did not influence the rate of full recovery. Non-recovery was associated with inferior outcomes and higher risk for reduced working capability.
Conclusions
The majority of patients with paresis were fully recovered 1 year after microdiscectomy for lumbar disc herniation. If the paresis was severe at baseline, there was a four times higher risk for non-recovery. Patients who did not recover had significantly worse outcomes.

Similar content being viewed by others
References
Cribb GL, Jaffray DC, Cassar-Pullicino VN (2007) Observations on the natural history of massive lumbar disc herniation. J Bone Joint Surg Br 89:782–784. doi:10.1302/0301-620X.89B6.18712
Dubourg G, Rozenberg S, Fautrel B, Valls-Bellec I, Bissery A, Lang T, Faillot T, Duplan B, Briançon D, Levy-Weil F, Morlock G, Crouzet J, Gatfosse M, Bonnet C, Houvenagel E, Hary S, Brocq O, Poiraudeau S, Beaudreuil J, de Sauverzac C, Durieux S, Levade M-H, Esposito P, Maitrot D, Goupille P, Valat J-P, Bourgeois P (2002) A pilot study on the recovery from paresis after lumbar disc herniation. Spine 27:1426–1431 (discussion 1431)
Weber H (1983) Lumbar disc herniation: a controlled, prospective study with ten years of observation. Spine 8:131–140
Barth M, Weiss C, Thomé C (2008) Two-year outcome after lumbar microdiscectomy versus microscopic sequestrectomy: part 1: evaluation of clinical outcome. Spine 33:265–272. doi:10.1097/BRS.0b013e318162018c
Eysel P, Rompe JD, Hopf C (1994) Prognostic criteria of discogenic paresis. Eur Spine J 3:214–218
Mariconda M, Galasso O, Secondulfo V, Cozzolino A, Milano C (2008) The functional relevance of neurological recovery after lumbar discectomy: a follow-up of more than 20 years. J Bone Joint Surg Br 90:622–628. doi:10.1302/0301-620X.90B5.20182
Postacchini F, Giannicola G, Cinotti G (2002) Recovery of motor deficits after microdiscectomy for lumbar disc herniation. J Bone Joint Surg Br 84:1040–1045
Hislop H, Montgomery J, H. Connolly B, Daniels L (2007) Daniels and Worthingham’s muscle testing: techniques of manual examination, 8th edn. p 437
Group TE (1990) EuroQol: a new facility for the measurement of health-related quality of life. Health Policy 16:199–208
Dolan P (1997) Modeling valuations for EuroQol health states. Med Care 35:1095–1108
Kind P, Dolan P, Gudex C, Williams A (1998) Variations in population health status: results from a United Kingdom national questionnaire survey. BMJ 316:736–741
Solberg TK, Olsen J-A, Ingebrigtsen T, Hofoss D, Nygaard OP (2005) Health-related quality of life assessment by the EuroQol-5D can provide cost-utility data in the field of low-back surgery. Eur Spine J 14:1000–1007. doi:10.1007/s00586-005-0898-2
Arts M, Brand R, van der Kallen B, Lycklama a Nijeholt G, Peul W (2011) Does minimally invasive lumbar disc surgery result in less muscle injury than conventional surgery? A randomized controlled trial. Eur Spine J 20:51–57. doi:10.1007/s00586-010-1482-y
Veresciagina K, Spakauskas B, Ambrozaitis KV (2010) Clinical outcomes of patients with lumbar disc herniation, selected for one-level open-discectomy and microdiscectomy. Eur Spine J 19:1450–1458. doi:10.1007/s00586-010-1431-9
Porchet F, Bartanusz V, Kleinstueck FS, Lattig F, Jeszenszky D, Grob D, Mannion AF (2009) Microdiscectomy compared with standard discectomy: an old problem revisited with new outcome measures within the framework of a spine surgical registry. Eur Spine J 18(3):360–366. doi:10.1007/s00586-009-0917-9
Brock M, Kunkel P, Papavero L (2008) Lumbar microdiscectomy: subperiosteal versus transmuscular approach and influence on the early postoperative analgesic consumption. Eur Spine J 17:518–522. doi:10.1007/s00586-008-0604-2
Silverplats K, Lind B, Zoega B, Halldin K, Rutberg L, Gellerstedt M, Brisby H (2010) Clinical factors of importance for outcome after lumbar disc herniation surgery: long-term follow-up. Eur Spine J 19:1459–1467. doi:10.1007/s00586-010-1433-7
Teli M, Lovi A, Brayda-Bruno M, Zagra A, Corriero A, Giudici F, Minoia L (2010) Higher risk of dural tears and recurrent herniation with lumbar micro-endoscopic discectomy. Eur Spine J 19:443–450. doi:10.1007/s00586-010-1290-4
Dewing CB, Provencher MT, Riffenburgh RH, Kerr S, Manos RE (2008) The outcomes of lumbar microdiscectomy in a young, active population: correlation by herniation type and level. Spine 33:33–38. doi:10.1097/BRS.0b013e31815e3a42
Jönsson B, Strömqvist B (1995) Motor affliction of the L5 nerve root in lumbar nerve root compression syndromes. Spine 20:2012–2015
Suzuki A, Matsumura A, Konishi S, Terai H, Tsujio T, Dozono S, Nakamura H (2011) Risk factor analysis for motor deficit and delayed recovery associated with L4/5 lumbar disc herniation. J Spinal Disord Tech 24:1–5. doi:10.1097/BSD.0b013e3181c5be1d
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lønne, G., Solberg, T.K., Sjaavik, K. et al. Recovery of muscle strength after microdiscectomy for lumbar disc herniation: a prospective cohort study with 1-year follow-up. Eur Spine J 21, 655–659 (2012). https://doi.org/10.1007/s00586-011-2122-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-011-2122-x