Abstract
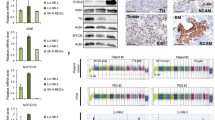
Neuroendocrine tumors are rare, and little is known about the existence of cancer stem cells in this disease. Identification of the tumorigenic population will contribute to the development of effective therapies targeting neuroendocrine tumors. Surgically resected brain metastases from a primary neuroendocrine tumor of unknown origin were dissociated and cultured in serum-free neurosphere medium. Stem cell properties, including self-renewal, differentiation potential, and stem cell marker expression, were examined. Tumor formation was evaluated using intracranial xenograft models. The effect of temozolomide was measured in vitro by cell viability assays. We established the neuroendocrine tumor sphere cell line ANI-27S, which displayed stable exponential growth, virtually unlimited expansion in vitro, and expression of stem-cell markers such as CD133, nestin, Sox2, and aldehyde dehydrogenase. FBS-induced differentiation decreased Sox2 and nestin expression. On the basis of real-time PCR, ANI-27S cells expressed the neuroendocrine markers synaptophysin and chromogranin A. Intracranial xenotransplanted brain tumors recapitulated the original patient tumor and temozolomide exhibited cytotoxic effects on tumor sphere cells. For the first time, we demonstrated the presence of a sphere-forming, stem cell-like population in brain metastases from a primary neuroendocrine tumor. We also demonstrated the potential therapeutic effects of temozolomide for this disease.





Similar content being viewed by others
References
Modlin IM, Lye KD, Kidd M (2003) A 5-decade analysis of 13,715 carcinoid tumors. Cancer 97:934–959
Jernman J, Valimaki MJ, Louhimo J, Haglund C, Arola J (2012) The novel WHO 2010 classification for gastrointestinal neuroendocrine tumours correlates well with the metastatic potential of rectal neuroendocrine tumours. Neuroendocrinology 95:317–324
Modlin IM, Oberg K, Chung DC, Jensen RT, de Herder WW, Thakker RV, Caplin M, Delle Fave G, Kaltsas GA, Krenning EP, Moss SF, Nilsson O, Rindi G, Salazar R, Ruszniewski P, Sundin A (2008) Gastroenteropancreatic neuroendocrine tumours. Lancet Oncol 9:61–72
Hallet J, Law CH, Cukier M, Saskin R, Liu N, Singh S (2015) Exploring the rising incidence of neuroendocrine tumors: a population-based analysis of epidemiology, metastatic presentation, and outcomes. Cancer 121:589–597
Yao JC, Hassan M, Phan A, Dagohoy C, Leary C, Mares JE, Abdalla EK, Fleming JB, Vauthey JN, Rashid A, Evans DB (2008) One hundred years after “carcinoid”: epidemiology of and prognostic factors for neuroendocrine tumors in 35,825 cases in the United States. J Clin Oncol 26:3063–3072
Hlatky R, Suki D, Sawaya R (2004) Carcinoid metastasis to the brain. Cancer 101:2605–2613
Kim SH, Ezhilarasan R, Phillips E, Gallego-Perez D, Sparks A, Taylor D, Ladner K, Furuta T, Sabit H, Chhipa R, Cho JH, Mohyeldin A, Beck S, Kurozumi K, Kuroiwa T, Iwata R, Asai A, Kim J, Sulman EP, Cheng SY, Lee LJ, Nakada M, Guttridge D, DasGupta B, Goidts V, Bhat KP, Nakano I (2016) Serine/threonine kinase MLK4 determines mesenchymal identity in glioma stem cells in an NF-kappa B-dependent manner. Cancer Cell 29:201–213
Lapidot T, Sirard C, Vormoor J, Murdoch B, Hoang T, Caceres-Cortes J, Minden M, Paterson B, Caligiuri MA, Dick JE (1994) A cell initiating human acute myeloid leukaemia after transplantation into SCID mice. Nature 367:645–648
Eramo A, Lotti F, Sette G, Pilozzi E, Biffoni M, Di Virgilio A, Conticello C, Ruco L, Peschle C, De Maria R (2008) Identification and expansion of the tumorigenic lung cancer stem cell population. Cell Death Differ 15:504–514
Gaur P, Sceusi EL, Samuel S, Xia L, Fan F, Zhou Y, Lu J, Tozzi F, Lopez-Berestein G, Vivas-Mejia P, Rashid A, Fleming JB, Abdalla EK, Curley SA, Vauthey JN, Sood AK, Yao JC, Ellis LM (2011) Identification of cancer stem cells in human gastrointestinal carcinoid and neuroendocrine tumors. Gastroenterology 141:1728–1737
Krampitz GW, George BM, Willingham SB, Volkmer JP, Weiskopf K, Jahchan N, Newman AM, Sahoo D, Zemek AJ, Yanovsky RL, Nguyen JK, Schnorr PJ, Mazur PK, Sage J, Longacre TA, Visser BC, Poultsides GA, Norton JA, Weissman IL (2016) Identification of tumorigenic cells and therapeutic targets in pancreatic neuroendocrine tumors. Proc Natl Acad Sci USA 113:4464–4469
Mitry E, Baudin E, Ducreux M, Sabourin JC, Rufie P, Aparicio T, Aparicio T, Lasser P, Elias D, Duvillard P, Schlumberger M, Rougier P (1999) Treatment of poorly differentiated neuroendocrine tumours with etoposide and cisplatin. Br J Cancer 81:1351–1355
Kunz PL (2015) Carcinoid and neuroendocrine tumors: building on success. J Clin Oncol 33:1855–1863
Ekeblad S, Sundin A, Janson ET, Welin S, Granberg D, Kindmark H, Dunder K, Kozlovacki G, Orlefors H, Sigurd M, Oberg K, Eriksson B, Skogseid B (2007) Temozolomide as monotherapy is effective in treatment of advanced malignant neuroendocrine tumors. Clin Cancer Res 13:2986–2991
Kulke MH, Stuart K, Enzinger PC, Ryan DP, Clark JW, Muzikansky A, Vincitore M, Michelini A, Fuchs CS (2006) Phase II study of temozolomide and thalidomide in patients with metastatic neuroendocrine tumors. J Clin Oncol 24:401–406
Chan JA, Stuart K, Earle CC, Clark JW, Bhargava P, Miksad R, Baszkowsky L, Enzinger PC, Meherhardt JA, Zheng H, Fuchs CS, Kulke MH (2012) Prospective study of bevacizumab plus temozolomide in patients with advanced neuroendocrine tumors. J Clin Oncol 30:2963–2968
De Divitiis C, von Arx C, Grimaldi AM, Cicala D, Tatangelo F, Arcella A, Romano GM, Simeone E, Iaffaioli RV, Ascierto PA, Tafuto S, European Neuroendocrine Tumor Society (ENETS) Center of Excellence-Multidisciplinary Group for Neuroendocrine Tumors in Naples (Italy) (2016) Metronomic temozolomide as second line treatment for metastatic poorly differentiated pancreatic neuroendocrine carcinoma. J Transl Med 14:113
Lin X, Saad RS, Luckasevic TM, Silverman JF, Liu Y (2007) Diagnostic value of CDX-2 and TTF-1 expressions in separating metastatic neuroendocrine neoplasms of unknown origin. Appl Immunohistochem Mol Morphol 15:407–414
Brandes AA, Franceschi E, Tosoni A, Benevento F, Scopece L, Mazzocchi V, Bacci A, Agati R, Calbucci F, Ermani M (2009) Temozolomide concomitant and adjuvant to radiotherapy in elderly patients with glioblastoma: correlation with MGMT promoter methylation status. Cancer 115:3512–3518
Flavahan WA, Wu Q, Hitomi M, Rahim N, Kim Y, Sloan AE, Weil RJ, Nakano I, Sarkaria JN, Stringer BW, Day BW, Li M, Lathia JD, Rich JN, Hjelmeland AB (2013) Brain tumor initiating cells adapt to restricted nutrition through preferential glucose uptake. Nat Neurosci 16:1373–1382
Okita Y, Nonaka M, Shofuda T, Kanematsu D, Yoshioka E, Kodama Y, Mano M, Nakajima S, Kanemura Y (2014) (11)C-methinine uptake correlates with MGMT promoter methylation in nonenhancing gliomas. Clin Neurol Neurosurg 125:212–216
Kanda Y (2013) Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transplant 48:452–458
Marcato P, Dean CA, Giacomantonio CA, Lee PW (2011) Aldehyde dehydrogenase: its role as a cancer stem cell marker comes down to the specific isoform. Cell Cycle 10:1378–1384
Ginestier C, Hur MH, Charafe-Jauffret E, Monville F, Dutcher J, Brown M, Jacquemier J, Viens P, Kleer CG, Lui S, Schott A, Haynes D, Birnbaum D, Wicha MS, Dontu G (2007) ALDH1 is a marker of normal and malignant human mammary stem cells and a predictor of poor clinical outcome. Cell Stem Cell 1:555–567
Douville J, Beaulieu R, Balicki D (2009) ALDH1 as a functional marker of cancer stem and progenitor cells. Stem Cells Dev 18:17–25
Reynolds BA, Weiss S (1992) Generation of neurons and astrocytes from isolated cells of the adult mammalian central nervous system. Science 255:1707–1710
Reynolds BA, Rietze RL (2005) Neural stem cells and neurospheres—re-evaluating the relationship. Nat Methods 2:333–336
Hong X, Chedid K, Kalkanis SN (2012) Glioblastoma cell line-derived spheres in serum containing medium versus serum-free medium: a comparison of cancer stem cell properties. Int J Oncol 41:1693–1700
Kulke MH, Hornick JL, Frauenhoffer C, Hooshmand S, Ryan DP, Enzinger PC, Meyerhardt JA, Clark JW, Stuart K, Fuchs CS, Redston MS (2009) O6-methylguanine DNA methyltransferase deficiency and response to temozolomide-based therapy in patients with neuroendocrine tumors. Clin Cancer Res 15:338–345
Hegi ME, Liu L, Herman JG, Stupp R, Wick W, Weller M, Mehta MP, Gilbert MR (2008) Correlation of O6-methylguanine methyltransferase (MGMT) promoter methylation with clinical outcomes in glioblastoma and clinical strategies to modulate MGMT activity. J Clin Oncol 26:4189–4199
Guo J, Cui Q, Jiang W, Liu C, Li D, Zeng Y (2013) Research on DNA methylation of human osteosarcoma cell MGMT and its relationship with cell resistance to alkylating agents. Biochem Cell Biol 91:209–213
Bai Y, Zhang QG, Wang XH (2014) Downregulation of TES by hypermethylation in glioblastoma reduces cell apoptosis and predicts poor clinical outcome. Eur J Med Res 19:66
Acknowledgements
We thank Ms. Hitomi Tatsumi and Ms. Akemi Mizushima for general technical assistance. This work was supported by JSPS KAKENHI Grant Number JP15K19983 and 15K10346.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Iwata, R., Maruyama, M., Ito, T. et al. Establishment of a tumor sphere cell line from a metastatic brain neuroendocrine tumor. Med Mol Morphol 50, 211–219 (2017). https://doi.org/10.1007/s00795-017-0160-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00795-017-0160-0