Abstract
Purpose
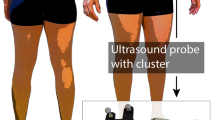
In dynamic musculoskeletal sonography, probe fixation can contribute to field of view (FOV) consistency, which is necessary for valid analysis of architectural parameters. In this volunteer study, the achieved FOV consistency in fixated ultrasonography was quantified and compared with freehand acquisition.
Methods
During five resting periods during cycling exercise, longitudinal B-mode images of the vastus lateralis (VL) muscle were acquired on one thigh with a fixated probe, and by two trained observers on the other thigh. In each acquisition, the structural similarity compared to the first resting period was determined using the complex wavelet structural similarity index (CW-SSIM). Also, the pennation angle of the VL was measured. Both CW-SSIM and pennation angle were compared between fixated and freehand acquisition. Furthermore, the compression of tissue by the probe fixation was measured.
Results
In fixated acquisition, a significantly higher structural similarity (p < 0.05) and an improved repeatability of pennation angle measurement were obtained compared to freehand acquisition. Probe fixation compressed muscle tissue by 12% on average.
Conclusions
Quantification of the structural similarity showed an increase in FOV consistency with sonography compared to freehand acquisition. The demonstrated feasibility of long-term fixated acquisition might be attractive in many medical fields and sports, and for reduction of work-related ergonomic problems among sonographers.







Similar content being viewed by others
References
Shung KK. Diagnostic ultrasound: imaging and blood flow measurements. 2nd ed. Boca Raton: CRC Press; 2015. p. 2–4.
Zamorani MP, Valle M. Muscle and Tendon. Ultrasound musculoskeletal system. Springer, Berlin 2007. p. 45–96. https://doi.org/10.1007/978-3-540-28163-4_3.
Pillen S, van Alfen N. Skeletal muscle ultrasound. Neurol Res. 2011;33:1016–24.
Peetrons P. Ultrasound of muscles. Eur Radiol. 2002;12:35–43.
Sikdar S, Wei Q, Cortes N. Dynamic ultrasound imaging applications to quantify musculoskeletal function. Exerc Sport Sci Rev. 2014;42:126–35.
Cronin NJ, Lichtwark G. The use of ultrasound to study muscle-tendon function in human posture and locomotion. Gait Posture. 2013;37:305–12.
Drakonaki EE, Allen GM, Wilson DJ. Ultrasound elastography for musculoskeletal applications. Br J Radiol. 2012;85:1435–45.
Konofagou EE, D’Hooge J, Ophir J. Myocardial elastography: a feasibility study in vivo. Ultrasound Med Biol. 2002;28:475–82.
Newman JS, Adler R, Rubin JM. Power doppler sonography: use in measuring alterations in muscle blood volume after exercise. J Diagn Med Sonogr. 1997;13:266.
Krix M, Weber M-A, Krakowski-Roosen H, et al. Assessment of skeletal muscle perfusion using contrast-enhanced ultrasonography. J Ultrasound Med. 2005;24:431–41.
Klimstra M, Dowling J, Durkin JL, et al. The effect of ultrasound probe orientation on muscle architecture measurement. J Electromyogr Kinesiol. 2007;17:504–14.
Shih Y-F. Active patellar tracking measurement: a novel device using ultrasound. Am J Sports Med. 2004;32:1209–17.
Peltonen J, Cronin NJ, Stenroth L, et al. Viscoelastic properties of the Achilles tendon in vivo. Springerplus. 2013;2:212.
Eranki A, Cortes N, Ferenček ZG, Sikdar S. A novel application of musculoskeletal ultrasound imaging. J Vis Exp. 2013. https://doi.org/10.3791/50595.
Hodges PW, Pengel LHM, Herbert RD, et al. Measurement of muscle contraction with ultrasound imaging. Muscle Nerve. 2003;27:682–92.
Aggeloussis N, Giannakou E, Albracht K, et al. Reproducibility of fascicle length and pennation angle of gastrocnemius medialis in human gait in vivo. Gait Posture. 2010;31:73–7.
Giannakou E, Aggeloussis N, Arampatzis A. Reproducibility of gastrocnemius medialis muscle architecture during treadmill running. J Electromyogr Kinesiol. 2011;21:1081–6.
Mairet S, Maïsetti O, Portero P. Homogeneity and reproducibility of in vivo fascicle length and pennation determined by ultrasonography in human vastus lateralis muscle. Sci Sport. 2006;21:268–72.
Fukunaga T, Ichinose Y, Ito M, et al. Determination of fascicle length and pennation in a contracting human muscle in vivo. J Appl Physiol. 1997;82:354–8.
Wang Z, Bovik AC, Sheikh HR, et al. Image quality assessment: from error visibility to structural similarity. IEEE Trans Image Process. 2004;13:600–12.
Zhou W, Simoncelli EP. Translation insensitive image similarity in complex wavelet domain. In: Proceedings (ICASSP’05) of IEEE international conferences on acoust speech, Signal Process 2005. IEEE; 2005; p. 573–6.
Renieblas GP, Nogués AT, González AM, et al. Structural similarity index family for image quality assessment in radiological images. J Med Imaging. 2017;4:035501.
Kowalik-Urbaniak I, Brunet D, Wang J, Koff D, et al. The quest for “diagnostically lossless” medical image compression: a comparative study of objective quality metrics for compressed medical images. SPIE Med Imaging. 2014;9037:903716–7.
Sampat MP, Zhou W, Gupta S, et al. Complex wavelet structural similarity: a new image similarity index. IEEE Trans Image Process. 2009;18:2385–401.
Portilla J, Simoncelli EP. A parametric texture model based on joint statistics of complex wavelet coefficients. Int J Comput Vis. 2000;40:49–70.
Jacobson JA. Musculoskeletal ultrasound: focused impact on MRI. Am J Roentgenol. 2009;193:619–27.
Bénard MR, Becher JG, Harlaar J, et al. Anatomical information is needed in ultrasound imaging of muscle to avoid potentially substantial errors in measurement of muscle geometry. Muscle Nerve. 2009;39:652–65.
Ema R, Akagi R, Wakahara T, et al. Training-induced changes in architecture of human skeletal muscles: current evidence and unresolved issues. J Phys Fit Sport Med. 2016;5:37–46.
Muraki S, Fukumoto K, Fukuda O. Prediction of the muscle strength by the muscle thickness and hardness using ultrasound muscle hardness meter. Springerplus. 2013;2:457.
Linder-Ganz E, Shabshin N, Itzchak Y, et al. Assessment of mechanical conditions in sub-dermal tissues during sitting: a combined experimental-MRI and finite element approach. J Biomech. 2007;40:1443–54.
Evans K, Roll S, Baker J. Work-related musculoskeletal disorders (WRMSD) among registered diagnostic medical sonographers and vascular technologists: a representative sample. J Diagn Med Sonogr. 2009;25:287–99.
Gremark Simonsen J, Axmon A, Nordander C, Arvidsson I. Neck and upper extremity pain in sonographers—associations with occupational factors. Appl Ergon. 2017;58:245–53.
Coffin C. Work-related musculoskeletal disorders in sonographers: a review of causes and types of injury and best practices for reducing injury risk. Reports Med Imaging. 2014;7:15.
Hecht HS, DeBord L, Sotomayor N, et al. Supine bicycle stress echocardiography: peak exercise imaging is superior to postexercise imaging. J Am Soc Echocardiogr. 1993;6:265–71.
Nakashiki K, Kisanuki A, Otsuji Y, et al. Usefulness of a novel ultrasound transducer for continuous monitoring treadmill exercise echocardiography to assess coronary artery disease. Circ J. 2006;70:1297–302.
Chandraratna PAN, Gajanayaka R, Makkena SM, Wijegunaratne K, Hafeez H, Vijayasekaran S, et al. “Hands-Free” continuous echocardiography during treadmill exercise using a novel ultrasound transducer. Echocardiography. 2010;27:563–6. https://doi.org/10.1111/j.1540-8175.2009.01056.x.
Acknowledgements
This study was funded by the European Community’s Seventh Framework Programme under Grant Agreement No. 318067.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The research proposal was reviewed by the local Medical Ethics Committee of the Máxima Medical Centre, Veldhoven, The Netherlands, and ethical approval was waived.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Heres, H.M., Sjoerdsma, M., Schoots, T. et al. Image acquisition stability of fixated musculoskeletal sonography in an exercise setting: a quantitative analysis and comparison with freehand acquisition. J Med Ultrasonics 47, 47–56 (2020). https://doi.org/10.1007/s10396-019-00983-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10396-019-00983-x