Abstract
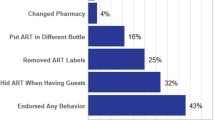
This study examined the relationship between HIV serostatus disclosure and adherence to antiretroviral therapy (ART). The study was conducted with 215 HIV-seropositive patients who demonstrated poor adherence (<80%) and who were in serodiscordant relationships. Participants completed self-report measures regarding HIV serostatus disclosure and reasons for missing ART doses, as well as electronic monitoring of ART adherence (MEMS caps). Overall, 19% of the sample reported missing medication doses in the last two months due to concerns regarding serostatus disclosure. Participants who reported greater serostatus disclosure to others demonstrated higher rates of adherence, and this relationship remained after controlling for other explanatory variables. The relationship between disclosure and adherence was not mediated by practical support for adherence from others. Interventions to improve ART adherence should address the role of serostatus disclosure by providing patients with skills to maintain adherence in contexts of non-disclosure and to make informed choices regarding selective disclosure.
Similar content being viewed by others
REFERENCES
Ammassari, A., Trotta, M. P., Murri, R., Castelli, F., Narciso, P., Noto, P., et al. (2002). Correlates and predictors of adherence to highly active antiretroviral therapy: Overview of published literature. Journal of Acquired Immune Deficiency Syndrome, 31, S123–S127.
Bangsberg, D. R., Hecht, F. M., Charlebois, E., Zolopa, A. R., Holodiny, M., Sheiner, L., et al. (2000). Adherence to protease inhibitors, HIV-1 viral load, and development of drug resistance in an indigent population. AIDS, 14, 357–366.
Bangsberg, D. R., Sharon, P., Charlebois, E. D., Clark, R. A., Roberston, M., Zolopa, A. R., et al. (2001). Non-adherence to highly active antiretroviral therapy predicts progression to AIDS. AIDS, 15, 1181–1183.
Baron, R. M., & Kenny, D. A. (1986). The moderator-mediator variable distinction in social psychological research: Conceptual, strategic, and statistical considerations. Journal of Personality and Social Psychology, 51, 1173–1182.
Beck, A. T., Steer, R. A., & Brown, G. K. (1996). Manual for the beck depression inventory-II. San Antonio, TX: Psychological Corporation.
Black, B. P., & Miles, M. S. (2002).Calculating the risks and benefits of disclosure in African American women who have HIV. Journal of Obstetric and Gynecological Neonatal Nursing, 31, 688–697.
Blaney, N. T., Fernandez, I., Ethier, K. A., Wilson, T. E., Walter, E., & Koenig, L. J., for the Perinatal Guidelines Evaluation Project Group. (2004). Psychosocial and behavioral correlates of depression among HIV-infected pregnant women. AIDS Patient Care and STDs, 18(7), 405–415.
Bozzette, S. A., Berry, S. H., Duan, N., Frankel, M. R., Leibowitz, A. A., Lefkowitz, D., et al. (1998). The care of HIV-infected adults in the United States. HIV Cost and Services Utilization Study Consortium. New England Journal of Medicine, 339(26), 1897–904.
Catz, S. L., Kelly, J. A., Bogart, L. M., Benotsch, E. G., & McAiliffe, T. L. (2000). Patterns, correlates and barriers to medication adherence among persons prescribed new treatments for HIV disease. Health Psychology, 19, 124–133.
Chesney, M. A., Chambers, D. B., Taylor, J. M., & Johnson, L. M. (2003). Social support, distress, and well-being in older men living with HIV infection. Journal of Acquired Immune Deficiency Syndromes, 33, S185 –S193.
Chesney, M. A., Ickovics, J. R., Chambers, D. B., Gifford, A. L., Neidig, J., Zwickl, B., et al. (2000). Self-reported adherence to antiretroviral medications among participants in HIV clinical trials: The AACTG adherence instruments. Patient Care Committee and Adherence Working Group of the Outcomes Committee of the Adult AIDS Clinical Trials Group (AACTG). AIDS Care, 12(3), 255–266.
Chesney, M. A., Ickovics, J., Hecht, F. M., Sikipa, G., & Rabkin, J. (1999). Adherence: a necessity for successful HIV combination therapy. AIDS, 12(Supp A), S271–S278.
Chesney, M. A., & Smith, A. W. (1999). Critical delays in HIV testing and care. American Behavioral Scientist, 42, 1162–1174.
Christensen, A., & Shenk, J. L. (1991). Communication, conflict, and psychological distance in nondistressed, clinic, and divorcing couples. Journal of Consulting and Clinical Psychology, 59, 458–463.
Clark, H. J., Lindner, G., Armistead, L., & Austin, B. (2003). Stigma, disclosure, and psychological functioning among HIV-infected and non-infected African-American women. Women and Health, 38(4), 57–71.
Clingerman, E. (2004). Physical activity, social support, and health-related quality of life among persons with HIV disease. Journal of Community Health Nursing, 21(3), 179–197.
Cohen, C. I., & Sokolovsky, J. (1978). General Social Survey network items. Connections, 8, 119–122.
D’Angelo, L. J., Abdalian, S. E., Sarr, M., Hoffman, N., Belzer, M., & the Adolescent Medicine HIV/AIDS Research Network. (2001). Disclosure of serostatus by HIV infected youth: The experience of the REACH study (Reaching for Excellence in Adolescent Care and Health). Journal of Adolescent Health, 29, 72–79.
Demas, P., Schoenbaum, E. E., Wills, T. A., Doll, L. S., & Klein, R. S. (1995). Stress, coping, and attitudes toward HIV treatment in injecting drug users: A qualitative study. AIDS Education and Prevention, 7(5), 429–442.
DiMatteo, M. R. (2004). Social support and patient adherence to medical treatment: A meta-analysis. Health Psychology, 23, 207–218.
Duran, S., Spire, B., Raffi, F., Walter, V., Bouhour, D., Journot, V., et al. (2001). Self-reported symptoms after initiation of a protease inhibitor in HIV-infected patients and their impact on adherence to HAART. HIV Clinical Trials, 2(1), 38–45.
El-Bassel, N., Cooper, D. K., Chen, D. R., & Schilling, R. F. (1998). Personal social networks and HIV status among women on methadone. AIDS Care, 10(6), 735–749.
Ewart, C. K. (1991). Social action theory for a public health psychology. American Psychologist, 46, 931–946.
Gibb, D. M., Goodall, R. L., Giacomet, V., McGee, L., Compagnucci, A., & Lyall, H,, for the Paediatric European Network for Treatment of AIDS Steering Committee (2003). Adherence to prescribed antiretroviral therapy in human immunodeficiency virus-infected children in the PENTA 5 trial. Pediatric Infectious Disease Journal, 22, 56–62.
Golin, C., Isasi, F., Bontempi, J. B., & Eng, E. (2002). Secret pills: HIV-positive patients’ experiences taking antiretroviral therapy in North Carolina. AIDS Education and Prevention, 14(4), 318–329.
Gonzalez, J. S., Penedo, F. J., Antoni, M. H., Duran, R. E., Fernandez, M. I., McPherson-Baker, S., et al. (2004). Social support, positive states of mind, and HIV treatment adherence in men and women living with HIV/AIDS. Health Psychology, 23, 413–418.
Gordillo, V., del Amo, J., Soriano, V., & Gonzalez-Lahoz, J. (1999). Sociodemographic and psychological variables influencing adherence to antiretroviral therapy. AIDS, 13, 1763–1769.
Heckman, T. G., Anderson, E. S., Sikkema, K. J., Kochman, A., Kalichman, S. C., & Anderson, T. (2004). Emotional distress in nonmetropolitan persons living with HIV disease enrolled in a telephone-delivered coping improvement group intervention. Health Psychology, 23, 94–100.
Herek, G. M., Capitanio, J. P., & Widaman, K. F. (2002). HIV-related stigma and knowledge in the United States: Prevalence and trends, 1991–1999. American Journal of Public Health, 92(3), 371–377.
Hoff, C. C. McKusick, L., Hillard, B., & Coates, T. J. (1992). The impact of HIV antibody status on gay men's partner preferences: A community perspective. AIDS Education and Prevention, 4, 197–204.
Horowitz, M., Adler, N., & Kegeles, S. (1988). A scale for measuring the occurrence of positive states of mind: A preliminary report. Psychosomatic Medicine, 50, 477–483.
Justice, A. C., Holmes, W., Gifford, A. L., Rabeneck, L., Zackin, R., Sinclair, G., et al. (2001). Development and validation of a self-completed HIV symptom index. Journal of Clinical Epidemiology, 54, S77–S90.
Kalichman, S. C., DiMarco, M., Austin, J., Luke, W., & DiFonzo, K. (2003). Stress, social support, and HIV-status disclosure to family and friends among HIV-positive men and women. Journal of Behavioral Medicine, 26(4), 315–332.
Kelly, J. A., Murphy, D. A., Bahr, G. R., & Kalichman, S. C. (1993). Outcome of cognitive-behavioral and support group brief therapies for depressed, HIV-infected persons. American Journal of Psychiatry, 150, 1679–1686.
Klitzman, R. L., Kirschenbaum, S. B., Dodge, B., Remien, R. H., Ehrhardt, A. A., Johnson, M. O., et al. (2004). Intricacies and inter-relationships between HIV disclosure and HAART: A qualitative study. AIDS Care, 16(5), 628–640.
Leserman, J., Jackson, E. D., Petitto, J. M., Golden, R. N., Silva, S. G., Perkins, D. O., et al. (1999). Progression to AIDS: The effects of stress, depressive symptoms, and social support. Psychosomatic Medicine, 61, 397–406.
Malcolm, S. E., Ng, J. J., Rosen, R. K., & Stone, V. E. (2003). An examination of HIV/AIDS patients who have excellent adherence to HAART. AIDS Care, 15, 251–261.
Mellins, C. A., Kang, E., Cheng-Shiun, L., Havens, J. F., & Chesney, M. A. (2003). Longitudinal study of mental health and psychosocial predictors of medical treatment adherence in mothers living with HIV disease. AIDS Patient Care and STDs, 17(8), 407–416.
Mellins, C. A., Brackis-Cott, E., Dolezal, C., & Abrams, E. J. (2004). The role of psychosocial and family factors in adherence to antiretroviral treatment in human immunodeficiency virus-infected children. Pediatric Infectious Disease Journal, 23, 1035–1041.
Morse, E. V., Simon, P. M., Coburn, M., Hyslop, N., Greenspan, D., & Balson, P. M. (1991). Determinants of subject compliance within an experimental anti-HIV drug protocol. Social Science & Medicine, 10, 1161–1167.
Mostashari, F., Riley, E., Selwyn, P. A., & Altice, F. L. (1998). Acceptance and adherence with antiretroviral therapy among HIV-infected women in a correctional facility. Journal of Acquired Immune Deficiency Syndromes, 18(4), 341–348.
Murphy, D. A., Steers, W. N., & Dello Stritto, M. E. (2001). Maternal disclosure of mother's HIV serostatus to their young children. Journal of Family Psychology, 15, 441–450.
Murri, R., Ammassari, A., Gallicano, K., De Luca, A., Cingolani, A., Jacobson, D., et al. (2000). Patient-reported nonadherence to HAART is related to protease inhibitor levels. Journal of Acquired Immune Deficiency Syndromes, 24, 123–128.
Ouette, M., Juretzko, P., Kroidl, A., Sagir, A., Wettstein, M., Siegrist, J., et al. (2002). Lipodystrophy syndrome and self-assessment of well-being and physical appearance in HIV-positive patients. AIDS Patient Care and STDs, 16(9), 413–417.
Paterson, D. L., Swindells, S., Mohr, J., Brester, M., Vergis, E. N., Squier, C., et al. (2000). Adherence to protease inhibitor therapy and outcomes in patients with HIV infection. Annals of Internal Medicine, 133, 21–30.
Prado, G., Feaster, D. J., Schwartz, S. J., Pratt, I. A., Smith, L., & Szapocznik, J. (2004). Religious involvement, coping, social support, and psychological distress in HIV-seropositive African American mothers. AIDS and Behavior, 8, 221–235.
Pugatch, D., Bennett, L., & Patterson, D. (2002). HIV medication adherence in adolescents: A qualitative study. Journal of HIV/AIDS Prevention and Education for Adolescents and Children, 5(1-2), 9–29.
Remien, R. H., Stirratt, M. J., Dolezal, C., Dognin, J. S., Wagner, G. J., Carballo-Dieguez, A., et al. (2005). Couple-focused support to improve HIV medication adherence: A randomized controlled trial. AIDS, 19, 807–814.
Safren, S. A., Radomsky, A. S., Otto, M. W., & Salomon, E. (2002). Predictors of psychological well-being in a diverse sample of HIV-positive patients receiving highly active antiretroviral therapy. Psychosomatics, 43, 478–485.
Serovich, J. M. (2001). A test of two HIV disclosure theories. AIDS Education and Prevention, 13, 355–364.
Siegel, K., Schrimshaw, E. W., & Raveis, V. H. (2000). Accounts for non-adherence to antiviral combination therapies among older HIV-infected adults. Psychology, Health & Medicine, 5(1), 29–42.
Stirratt, M. J. (2005). I have something to tell you: HIV serostatus disclosure strategies and sexual practices. In P. N. Halkitis, C. Gomez, & R. Wolitski (Eds.), HIV+ Sex: The psychological and interpersonal dynamics of HIV-seropositive gay and bisexual men's relationships. Washington, DC: American Psychological Association.
Swindells, S., Mohr, J., Justis, J. C., Berman, S., Squier, C., Wagener, M. M., et al. (1999). Quality of life in patients with human immunodeficiency virus infection: impact of social support, coping style and hopelessness. International Journal of STDs and AIDS, 10(6), 383–391.
Wills, T. A., & Fegan, M. F. (2001). Social networks and social support. In A. Baum, T. A. Revenson, & J. E. Singer (Eds.), Handbook of health psychology (pp. 209–234). Mahwah, NJ: Lawrence Erlbaum.
Wood, E., Hogg, R. S., Yip, B., Harrigan, P. R., O’Shaughnessy, M. V., & Montaner, J. S. (2003). Effect of medication adherence on survival of HIV-infected adults who start highly active antiretroviral therapy when the CD4+ cell count is 0.200 to 0.350 × 10(9) cells/L. Annals of Internal Medicine, 139, 810–816.
Wood, E., Hogg, R. S., Yip, B., Harrigan, P. R., O’Shaughnessy, M. V., & Montaner, J. S. (2004). The impact of adherence on CD4 cell count responses among HIV-infected patients. Journal of Acquired Immune Deficiency Syndromes, 35, 261–268.
Zea, M. C., Reisen, C. A., Poppen, P. J., Bianchi, F. T., & Echeverry, J. J. (2005). Disclosure of HIV status and psychological well-being among Latino gay and bisexual men. AIDS & Behavior, 9, 15–26.
Zierler, S., Cunningham, W. E., Andersen, R., Shapiro, M. F., Bozzette, S. A., Nakazono, T., et al. (2000). Violence victimization after HIV infection in a U.S. probability sample of adult patients in primary care. American Journal of Public Health, 90(2), 208–215.
Acknowledgement
This study was supported by the National Institute of Mental Health (R01 MH61173 Serodiscordant Couples, Medical Adherence, and HIV Risk; Robert H. Remien, Ph.D.). Michael J. Stirratt, Ph.D., is a post-doctoral fellow supported by a training grant from the National Institute of Mental Health (T32 MH19139 Behavioral Sciences Research in HIV Infection; Anke A. Ehrhardt, Ph.D.). The authors acknowledge the contributions of the SMART Couples Study Team: Nabila El Bassel, Ph.D., Robert Kertzner, Ph.D., Alex Carballo-Dieguez, Ph.D., and Joanna Dognin, Psy.D. We also thank Tiffany Jung, N. P., Robert Warford, N.P., Ernie Attah, Ph.D., and Ronit Epstein, B.A., for their assistance with the conduct of this study. We are grateful to Victoria Sharp, M.D., and the clinical staff at St. Luke’s-Roosevelt Hospital Center for their collaboration on this project and to the men and women who participated in this study
Author information
Authors and Affiliations
Consortia
Corresponding author
Rights and permissions
About this article
Cite this article
Stirratt, M.J., Remien, R.H., Smith, A. et al. The Role of HIV Serostatus Disclosure in Antiretroviral Medication Adherence. AIDS Behav 10, 483–493 (2006). https://doi.org/10.1007/s10461-006-9106-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-006-9106-6