Abstract
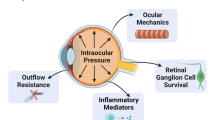
Estrogen is essential in maintaining various physiological features in women, and a decline in estrogen levels are known to give rise to numerous unfortunate symptoms associated with menopause. To alleviate these symptoms hormone replacement therapy with estrogen is often used, and has been shown to be fruitful in improving quality of life in women suffering from postmenopausal discomforts. An often forgotten condition associated with menopause is the optic nerve disorder, glaucoma. Thus, estrogen may also have an impact in maintaining the retinal ganglion cells (RGCs), which make up the optic nerve, thereby preventing glaucomatous neurodegeneration. This review aims to provide an overview of possible associations of estrogen and the glaucoma subtype, primary open-angle glaucoma (POAG), by evaluating the current literature through a PubMed-based literature search. Multiple in vitro and in vivo studies of RGC protection, as well as clinical and epidemiological data concerning the well-defined retinal neurodegenerative disorder POAG have been reviewed. Over all, deficiencies in retinal estrogen may potentially instigate RGC loss, visual disability, and eventual blindness. Estrogen replacement therapy may therefore be a beneficial future treatment. However, more studies are needed to confirm the relevance of estrogen in glaucoma prevention.



Similar content being viewed by others
References
Abegão Pinto L, Vandewalle E, De Clerck E, Marques-Neves C, Stalmans I (2013) Lack of spontaneous venous pulsation: possible risk indicator in normal tension glaucoma? ActaOphthalmol 91:514–520. https://doi.org/10.1111/j.1755-3768.2012.02472.x
Abramov Y, Borik S, Yahalom C, Fatum M, Avgil G, Brzezinski A, Banin E (2005) Does postmenopausal hormone replacement therapy affect intraocular pressure? J Glaucoma 14:271–275
Acharya M et al (2006) Primary role of CYP1B1 in Indian juvenile-onset POAG patients. Mol Vis 12:399–404
Akar ME, Taskin O, Yucel I, Akar Y (2004) The effect of the menstrual cycle on optic nerve head analysis in healthy women. ActaOphthalmolScand 82:741–745. https://doi.org/10.1111/j.1600-0420.2004.00351.x
Akar ME, Apaydin KC, Taskin O, Akar Y, Trak B (2005a) Menstrual cycle-dependent changes in white-on-white visual field analysis of diabetic women. GynecolObstet Invest 60:92–97. https://doi.org/10.1159/000085327
Akar ME, Yucel I, Erdem U, Taskin O, Ozel A, Akar Y (2005b) Effect of the menstrual cycle on the optic nerve head in diabetes: analysis by confocal scanning laser ophthalmoscopy. Can J Ophthalmol 40:175–182. https://doi.org/10.1016/S0008-4182(05)80029-8
Bailey JNC et al (2018) Testosterone pathway genetic polymorphisms in relation to primary open-angle glaucoma: an analysis in two large datasets. Invest Ophthalmol Vis Sci 59:629–636. https://doi.org/10.1167/iovs.17-22708
Banerjee A, Chakraborty S, Chakraborty A, Chakrabarti S, Ray K (2016) Functional and structural analyses of CYP1B1 variants linked to congenital and adult-onset glaucoma to investigate the molecular basis of these diseases. PLoS ONE 11:e0156252. https://doi.org/10.1371/journal.pone.0156252
Battaglia C, Mancini F, Regnani G, Persico N, Volpe A, De Aloysio D (2004) Hormone therapy and ophthalmic artery blood flow changes in women with primary open-angle glaucoma. Menopause 11:69–77. https://doi.org/10.1097/01.GME.0000079741.18541.92
Behl C, Skutella T, Lezoualc'h F, Post A, Widmann M, Newton CJ, Holsboer F (1997) Neuroprotection against oxidative stress by estrogens: structure-activity relationship. MolPharmacol 51:535–541
Bengtsson B (1981) The prevalence of glaucoma. Br J Ophthalmol 65:46–49. https://doi.org/10.1136/bjo.65.1.46
Brann DW, Dhandapani K, Wakade C, Mahesh VB, Khan MM (2007) Neurotrophic and neuroprotective actions of estrogen: basic mechanisms and clinical implications. Steroids 72:381–405. https://doi.org/10.1016/j.steroids.2007.02.003
Broman AT et al (2008) Estimating the rate of progressive visual field damage in those with open-angle glaucoma, from cross-sectional data. Invest Ophthalmol Vis Sci 49:66–76. https://doi.org/10.1167/iovs.07-0866
Cao W, Rajala RVS, Li F, Anderson RE, Wei N, Soliman CE, McGinnis JF (2003) Neuroprotective effect of estrogen upon retinal neurons in vitro. AdvExp Med Biol 533:395–402. https://doi.org/10.1007/978-1-4615-0067-4_50
Caprioli J et al (2016) Trabeculectomy can improve long-term visual function in glaucoma. Ophthalmology 123:117–128. https://doi.org/10.1016/j.ophtha.2015.09.027
Caulin-Glaser T, García-Cardeña G, Sarrel P, Sessa WC, Bender JR (1997) 17 beta-estradiol regulation of human endothelial cell basal nitric oxide release, independent of cytosolic Ca2+ mobilization. Circ Res 81:885–892. https://doi.org/10.1161/01.res.81.5.885
Cavalieri EL, Rogan EG (2016) Depurinating estrogen-DNA adducts, generators of cancer initiation: their minimization leads to cancer prevention. ClinTransl Med 5:12. https://doi.org/10.1186/s40169-016-0088-3
Chan KKW, Tang F, Tham CCY, Young AL, Cheung CY (2017) Retinal vasculature in glaucoma: a review. BMJ Open Ophthalmol 1:e000032. https://doi.org/10.1136/bmjophth-2016-000032
Charlson ME et al (2014) Nocturnal systemic hypotension increases the risk of glaucoma progression. Ophthalmology 121:2004–2012. https://doi.org/10.1016/j.ophtha.2014.04.016
Chen YY et al (2018) Association between normal tension glaucoma and the risk of Alzheimer's disease: a nationwide population-based cohort study in Taiwan. BMJ Open 8:e022987. https://doi.org/10.1136/bmjopen-2018-022987
Chistiakov DA, Sobenin IA, Revin VV, Orekhov AN, Bobryshev YV (2014) Mitochondrial aging and age-related dysfunction of mitochondria. Biomed Res Int 2014:238463. https://doi.org/10.1155/2014/238463
Choi J, Kook MS (2015) Systemic and ocular hemodynamic risk factors in glaucoma. Biomed Res Int 2015:141905. https://doi.org/10.1155/2015/141905
Choi J, Jeong J, Cho HS, Kook MS (2006) Effect of nocturnal blood pressure reduction on circadian fluctuation of mean ocular perfusion pressure: a risk factor for normal tension glaucoma. Invest Ophthalmol Vis Sci 47:831–836. https://doi.org/10.1167/iovs.05-1053
Choi J, Kim KH, Jeong J, Cho HS, Lee CH, Kook MS (2007) Circadian fluctuation of mean ocular perfusion pressure is a consistent risk factor for normal-tension glaucoma. Invest Ophthalmol Vis Sci 48:104–111. https://doi.org/10.1167/iovs.06-0615
Coca-Prados M, Escribano J, Ortego J (1999) Differential gene expression in the human ciliary epithelium. ProgRetin Eye Res 18:403–429. https://doi.org/10.1016/s1350-9462(98)00026-3
Coca-Prados M, Ghosh S, Wang Y, Escribano J, Herrala A, Vihko P (2003) Sex steroid hormone metabolism takes place in human ocular cells. J Steroid BiochemMolBiol 86:207–216. https://doi.org/10.1016/j.jsbmb.2003.08.001
Coffey M, Reidy A, Wormald R, Xian WX, Wright L, Courtney P (1993) Prevalence of glaucoma in the west of Ireland. Br J Ophthalmol 77:17–21. https://doi.org/10.1136/bjo.77.1.17
Collins P et al (1995) 17 beta-Estradiol attenuates acetylcholine-induced coronary arterial constriction in women but not men with coronary heart disease. Circulation 92:24–30. https://doi.org/10.1161/01.cir.92.1.24
de Voogd S, Wolfs RC, Jansonius NM, Uitterlinden AG, Pols HA, Hofman A, de Jong PT (2008) Estrogen receptors alpha and beta and the risk of open-angle glaucoma: the Rotterdam Study. Arch Ophthalmol 126:110–114. https://doi.org/10.1001/archopht.126.1.110
Delamere NA (2005) Ciliary body and ciliary epithelium. Adv Organ Biol 10:127–148. https://doi.org/10.1016/S1569-2590(05)10005-6
Deschênes MC et al (2010) Postmenopausal hormone therapy increases retinal blood flow and protects the retinal nerve fiber layer. Invest Ophthalmol Vis Sci 51:2587–2600. https://doi.org/10.1167/iovs.09-3710
Dewundara SS, Wiggs JL, Sullivan DA, Pasquale LR (2016) Is estrogen a therapeutic target for glaucoma? SeminOphthalmol 31:140–146. https://doi.org/10.3109/08820538.2015.1114845
Dielemans I, Vingerling JR, Wolfs RC, Hofman A, Grobbee DE, de Jong PT (1994) The prevalence of primary open-angle glaucoma in a population-based study in The Netherlands. The Rotterdam Study. Ophthalmology 101:1851–1855. https://doi.org/10.1016/s0161-6420(94)31090-6
Eisner A (2015) Sex, eyes, and vision: male/female distinctions in ophthalmic disorders. Curr Eye Res 40:96–101. https://doi.org/10.3109/02713683.2014.975368
Eisner A, Demirel S (2011) Variability in short-wavelength automated perimetry among peri- or postmenopausal women: a dependence on phyto-oestrogen consumption? ActaOphthalmol 89:e217–224. https://doi.org/10.1111/j.1755-3768.2009.01799.x
Faria AF, de Souza MA, Geber S (2011) Vascular resistance of central retinal artery is reduced in postmenopausal women after use of estrogen. Menopause 18:869–872. https://doi.org/10.1097/gme.0b013e31820cc60c
Fautsch MP, Bahler CK, Jewison DJ, Johnson DH (2000) Recombinant TIGR/MYOC increases outflow resistance in the human anterior segment. Invest Ophthalmol Vis Sci 41:4163–4168
Feke GT, Pasquale LR (2008) Retinal blood flow response to posture change in glaucoma patients compared with healthy subjects. Ophthalmology 115:246–252. https://doi.org/10.1016/j.ophtha.2007.04.055
Feola AJ et al (2019) Menopause exacerbates visual dysfunction in experimental glaucoma. Exp Eye Res 186:107706. https://doi.org/10.1016/j.exer.2019.107706
Fingert JH et al (1998) Characterization and comparison of the human and mouse GLC1A glaucoma genes. Genome Res 8:377–384. https://doi.org/10.1101/gr.8.4.377
Foti MC (2007) Antioxidant properties of phenols. J Pharm Pharmacol 59:1673–1685. https://doi.org/10.1211/jpp.59.12.0010
Garbacz WG, Jiang M, Xie W (2017) Sex-dependent role of estrogen sulfotransferase and steroid sulfatase in metabolic homeostasis. AdvExp Med Biol 1043:455–469. https://doi.org/10.1007/978-3-319-70178-3_21
Gasser P, Flammer J (1991) Blood-cell velocity in the nailfold capillaries of patients with normal-tension and high-tension glaucoma. Am J Ophthalmol 111:585–588. https://doi.org/10.1016/s0002-9394(14)73703-1
Gherghel D, Hosking SL, Armstrong R, Cunliffe IA (2007) Autonomic dysfunction in unselected and untreated primary open angle glaucoma patients: a pilot study. Ophthalmic Physiol Opt 27:336–341. https://doi.org/10.1111/j.1475-1313.2007.00485.x
Gherghel D, Hosking SL, Cunliffe IA, Heitmar R (2010) Transient cardiac ischaemia and abnormal variations in systemic blood pressure in unselected primary open angle glaucoma patients. Ophthalmic Physiol Opt 30:175–181. https://doi.org/10.1111/j.1475-1313.2009.00704.x
Giordano C et al (2011) Oestrogens ameliorate mitochondrial dysfunction in Leber's hereditary optic neuropathy. Brain 134:220–234. https://doi.org/10.1093/brain/awq276
Giorgio A, Zhang J, Costantino F, De Stefano N, Frezzotti P (2018) Diffuse brain damage in normal tension glaucoma. Hum Brain Mapp 39:532–541. https://doi.org/10.1002/hbm.23862
Graham SL, Drance SM, Wijsman K, Douglas GR, Mikelberg FS (1995) Ambulatory blood pressure monitoring in glaucoma. The nocturnal dip. Ophthalmology 102:61–69. https://doi.org/10.1016/s0161-6420(95)31053-6
Guedes G, Tsai JC, Loewen NA (2011) Glaucoma and aging. Curr Aging Sci 4:110–117. https://doi.org/10.2174/1874609811104020110
Gupta PD, Johar K Sr, Nagpal K, Vasavada AR (2005) Sex hormone receptors in the human eye. SurvOphthalmol 50:274–284. https://doi.org/10.1016/j.survophthal.2005.02.005
Hajirahimkhan A, Dietz BM, Bolton JL (2013) Botanical modulation of menopausal symptoms: mechanisms of action? Planta Med 79:538–553. https://doi.org/10.1055/s-0032-1328187
Harris A, Harris M, Biller J, Garzozi H, Zarfty D, Ciulla TA, Martin B (2000) Aging affects the retrobulbar circulation differently in women and men. Arch Ophthalmol 118:1076–1080. https://doi.org/10.1001/archopht.118.8.1076
Harris-Yitzhak M, Harris A, Ben-Refael Z, Zarfati D, Garzozi HJ, Martin BJ (2000) Estrogen-replacement therapy: effects on retrobulbar hemodynamics. Am J Ophthalmol 129:623–628. https://doi.org/10.1016/s0002-9394(99)00468-7
Hayashi Y et al (2007) Neuroprotective effect of 17beta-estradiol against N-methyl-D-aspartate-induced retinal neurotoxicity via p-ERK induction. J Neurosci Res 85:386–394. https://doi.org/10.1002/jnr.21127
Hayreh SS, Zimmerman MB, Podhajsky P, Alward WL (1994) Nocturnal arterial hypotension and its role in optic nerve head and ocular ischemic disorders. Am J Ophthalmol 117:603–624. https://doi.org/10.1016/s0002-9394(14)70067-4
Heijl A, Leske MC, Bengtsson B, Hyman L, Bengtsson B, Hussein M, Early Manifest Glaucoma Trial G (2002) Reduction of intraocular pressure and glaucoma progression: results from the Early Manifest Glaucoma Trial. Arch Ophthalmol 120:1268–1279. https://doi.org/10.1001/archopht.120.10.1268
Hertz L, Peng L, Dienel GA (2007) Energy metabolism in astrocytes: high rate of oxidative metabolism and spatiotemporal dependence on glycolysis/glycogenolysis. J Cereb Blood Flow Metab 27:219–249. https://doi.org/10.1038/sj.jcbfm.9600343
Hollows FC, Graham PA (1966) Intra-ocular pressure, glaucoma, and glaucoma suspects in a defined population. Br J Ophthalmol 50:570–586. https://doi.org/10.1136/bjo.50.10.570
Hulsman CA et al (2001) Is open-angle glaucoma associated with early menopause? The Rotterdam Study. Am J Epidemiol 154:138–144. https://doi.org/10.1093/aje/154.2.138
Inagaki Y, Mashima Y, Fuse N, Ohtake Y, Fujimaki T, Fukuchi T (2006) Mitochondrial DNA mutations with Leber's hereditary optic neuropathy in Japanese patients with open-angle glaucoma. Jpn J Ophthalmol 50:128–134. https://doi.org/10.1007/s10384-005-0290-0
Iorga A, Cunningham CM, Moazeni S, Ruffenach G, Umar S, Eghbali M (2017) The protective role of estrogen and estrogen receptors in cardiovascular disease and the controversial use of estrogen therapy. Biol Sex Differ 8:33–33. https://doi.org/10.1186/s13293-017-0152-8
Ivanov D, Dvoriantchikova G, Nathanson L, McKinnon SJ, Shestopalov VI (2006) Microarray analysis of gene expression in adult retinal ganglion cells. FEBS Lett 580:331–335. https://doi.org/10.1016/j.febslet.2005.12.017
Iwase A et al (2004) The prevalence of primary open-angle glaucoma in Japanese: the Tajimi Study. Ophthalmology 111:1641–1648. https://doi.org/10.1016/j.ophtha.2004.03.029
Jansson I, Stoilov I, Sarfarazi M, Schenkman JB (2001) Effect of two mutations of human CYP1B1, G61E and R469W, on stability and endogenous steroid substrate metabolism. Pharmacogenetics 11:793–801
Jiang M, Ma X, Zhao Q, Li Y, Xing Y, Deng Q, Shen Y (2019) The neuroprotective effects of novel estrogen receptor GPER1 in mouse retinal ganglion cell degeneration. Exp Eye Res 189:107826. https://doi.org/10.1016/j.exer.2019.107826
Jojua T, Sumbadze TS, Papava M (2005) Secretion of sex hormones in patients with open angle glaucoma. Georgian Med News: 33–37
Jung Y, Han K, Park HYL, Lee SH, Park CK (2020) Metabolic health, obesity, and the risk of developing open-angle glaucoma: metabolically healthy obese patients versus metabolically unhealthy but normal weight patients. Diabetes Metab J 44:414–425. https://doi.org/10.4093/dmj.2019.0048
Kaiser HJ, Flammer J, Graf T, Stümpfig D (1993) Systemic blood pressure in glaucoma patients. Graefes Arch ClinExpOphthalmol 231:677–680. https://doi.org/10.1007/bf00919280
Kapetanakis VV, Chan MP, Foster PJ, Cook DG, Owen CG, Rudnicka AR (2016) Global variations and time trends in the prevalence of primary open angle glaucoma (POAG): a systematic review and meta-analysis. Br J Ophthalmol 100:86–93. https://doi.org/10.1136/bjophthalmol-2015-307223
Kaur K, Mandal AK, Chakrabarti S (2011) Primary congenital glaucoma and the involvement of CYP1B1 middle east. Afr J Ophthalmol 18:7–16. https://doi.org/10.4103/0974-9233.75878
Kerrigan LA, Zack DJ, Quigley HA, Smith SD, Pease ME (1997) TUNEL-positive ganglion cells in human primary open-angle glaucoma. Arch Ophthalmol 115:1031–1035. https://doi.org/10.1001/archopht.1997.01100160201010
Khachatryan N et al (2019) Primary Open-Angle African American Glaucoma Genetics (POAAGG) Study: gender and risk of POAG in African Americans. PLoS ONE 14:e0218804. https://doi.org/10.1371/journal.pone.0218804
Kim YK, Oh WH, Park KH, Kim JM, Kim DM (2010) Circadian blood pressure and intraocular pressure patterns in normal tension glaucoma patients with undisturbed sleep. Korean J Ophthalmol 24:23–28. https://doi.org/10.3341/kjo.2010.24.1.23
Kim HA, Han K, Lee YA, Choi JA, Park YM (2016) Differential association of metabolic risk factors with open angle glaucoma according to obesity in a Korean population. Sci Rep 6:38283. https://doi.org/10.1038/srep38283
Klein BE, Klein R, Sponsel WE, Franke T, Cantor LB, Martone J, Menage MJ (1992) Prevalence of glaucoma. The Beaver Dam Eye Study. Ophthalmology 99:1499–1504. https://doi.org/10.1016/s0161-6420(92)31774-9
Kolko M (2015) Present and new treatment strategies in the management of glaucoma open. Ophthalmol J 9:89–100. https://doi.org/10.2174/1874364101509010089
Kolko M, Horwitz A, Thygesen J, Jeppesen J, Torp-Pedersen C (2015) The prevalence and incidence of glaucoma in Denmark in a fifteen year period: a nationwide study. PLoS ONE 10:e0132048–e0132048. https://doi.org/10.1371/journal.pone.0132048
Koseki N, Kitaoka Y, Munemasa Y, Kumai T, Kojima K, Ueno S, Ohtani-Kaneko R (2012) 17beta-estradiol prevents reduction of retinal phosphorylated 14–3-3 zeta protein levels following a neurotoxic insult. Brain Res 1433:145–152. https://doi.org/10.1016/j.brainres.2011.11.034
Kosior-Jarecka E et al (2019) Estrogen receptor gene polymorphisms and their influence on clinical status of Caucasian patients with primary open angle glaucoma. Ophthalmic Genet 40:323–328. https://doi.org/10.1080/13816810.2019.1639201
Kubota R et al (1997) A novel myosin-like protein (myocilin) expressed in the connecting cilium of the photoreceptor: molecular cloning, tissue expression, and chromosomal mapping. Genomics 41:360–369. https://doi.org/10.1006/geno.1997.4682
Kumar DM et al (2005) Role of nonfeminizing estrogen analogues in neuroprotection of rat retinal ganglion cells against glutamate-induced cytotoxicity. Free RadicBiol Med 38:1152–1163. https://doi.org/10.1016/j.freeradbiomed.2004.12.007
Labrie F, Luu-The V, Bélanger A, Lin SX, Simard J, Pelletier G, Labrie C (2005) Is dehydroepiandrosterone a hormone? J Endocrinol 187:169–196. https://doi.org/10.1677/joe.1.06264
Lascaratos G, Garway-Heath DF, Willoughby CE, Chau K-Y, Schapira AHV (2012) Mitochondrial dysfunction in glaucoma: understanding genetic influences. Mitochondrion 12:202–212. https://doi.org/10.1016/j.mito.2011.11.004
Lavigne JA, Goodman JE, Fonong T, Odwin S, He P, Roberts DW, Yager JD (2001) The effects of catechol-O-methyltransferase inhibition on estrogen metabolite and oxidative DNA damage levels in estradiol-treated MCF-7 cells. Cancer Res 61:7488–7494
Lee AJ, Mitchell P, Rochtchina E, Healey PR, Blue Mountains Eye S (2003) Female reproductive factors and open angle glaucoma: the Blue Mountains Eye Study. Br J Ophthalmol 87:1324–1328. https://doi.org/10.1136/bjo.87.11.1324
Leske MC, Connell AM, Schachat AP, Hyman L (1994) The Barbados Eye Study. Prevalence of open angle glaucoma. Arch Ophthalmol 112:821–829. https://doi.org/10.1001/archopht.1994.01090180121046
Lin PW, Friedman M, Lin HC, Chang HW, Wilson M, Lin MC (2011) Normal tension glaucoma in patients with obstructive sleep apnea/hypopnea syndrome. J Glaucoma 20:553–558. https://doi.org/10.1097/IJG.0b013e3181f3eb81
Luft N et al (2016) Ocular blood flow measurements in healthy white subjects using laser speckle flowgraphy. PLoS ONE 11:e0168190–e0168190. https://doi.org/10.1371/journal.pone.0168190
Luu-The V, Labrie F (2010) The intracrine sex steroid biosynthesis pathways. Prog Brain Res 181:177–192. https://doi.org/10.1016/S0079-6123(08)81010-2
Mabuchi F, Sakurada Y, Kashiwagi K, Yamagata Z, Iijima H, Tsukahara S (2010) Estrogen receptor beta gene polymorphism and intraocular pressure elevation in female patients with primary open-angle glaucoma. Am J Ophthalmol 149:826–830. https://doi.org/10.1016/j.ajo.2009.12.030
Mallick J, Devi L, Malik PK, Mallick J (2016) Update on normal tension glaucoma. J Ophthalmic Vis Res 11:204–208. https://doi.org/10.4103/2008-322X.183914
Manthey D, Behl C (2006) From structural biochemistry to expression profiling: neuroprotective activities of estrogen. Neuroscience 138:845–850. https://doi.org/10.1016/j.neuroscience.2005.10.058
Masters SC, Fu H (2001) 14–3-3 proteins mediate an essential anti-apoptotic signal. J BiolChem 276:45193–45200. https://doi.org/10.1074/jbc.M105971200
Maxim P, Ettinger B, Spitalny GM (1995) Fracture protection provided by long-term estrogen treatment. OsteoporosInt 5:23–29. https://doi.org/10.1007/bf01623654
Melki R, Colomb E, Lefort N, Brézin AP, Garchon HJ (2004) CYP1B1 mutations in French patients with early-onset primary open-angle glaucoma. J Med Genet 41:647–651. https://doi.org/10.1136/jmg.2004.020024
Mitchell P, Smith W, Attebo K, Healey PR (1996) Prevalence of open-angle glaucoma in Australia. The Blue Mountains Eye Study. Ophthalmology 103:1661–1669. https://doi.org/10.1016/s0161-6420(96)30449-1
Monemi S et al (2005) Identification of a novel adult-onset primary open-angle glaucoma (POAG) gene on 5q22.1. Hum Mol Genet 14:725–733. https://doi.org/10.1093/hmg/ddi068
Mookherjee S, Acharya M, Banerjee D, Bhattacharjee A, Ray K (2012) Molecular basis for involvement of CYP1B1 in MYOC upregulation and its potential implication in glaucoma pathogenesis. PLoS ONE 7:e45077. https://doi.org/10.1371/journal.pone.0045077
Mroczkowska S, Benavente-Perez A, Negi A, Sung V, Patel SR, Gherghel D (2013) Primary open-angle glaucoma vs normal-tension glaucoma: the vascular perspective. JAMA Ophthalmology 131:36–43. https://doi.org/10.1001/2013.jamaophthalmol.1
Na KS, Jee DH, Han K, Park YG, Kim MS, Kim EC (2014) The ocular benefits of estrogen replacement therapy: a population-based study in postmenopausal Korean women. PLoS ONE 9:e106473. https://doi.org/10.1371/journal.pone.0106473
Nakazawa T (2016) Ocular blood flow and influencing factors for glaucoma. Asia Pac J Ophthalmol (Phila) 5:38–44. https://doi.org/10.1097/apo.0000000000000183
Nakazawa T, Takahashi H, Shimura M (2006) Estrogen has a neuroprotective effect on axotomized RGCs through ERK signal transduction pathway. Brain Res 1093:141–149. https://doi.org/10.1016/j.brainres.2006.03.084
Nevzati E, Shafighi M, Bakhtian KD, Treiber H, Fandino J, Fathi AR (2015) Estrogen induces nitric oxide production via nitric oxide synthase activation in endothelial cells. ActaNeurochirSuppl 120:141–145. https://doi.org/10.1007/978-3-319-04981-6_24
Newman-Casey PA, Talwar N, Nan B, Musch DC, Pasquale LR, Stein JD (2014) The potential association between postmenopausal hormone use and primary open-angle glaucoma. JAMA Ophthalmol 132:298–303. https://doi.org/10.1001/jamaophthalmol.2013.7618
Nirmalan PK, Katz J, Robin AL, Ramakrishnan R, Krishnadas R, Thulasiraj RD, Tielsch JM (2004) Female reproductive factors and eye disease in a rural South Indian population: the Aravind Comprehensive Eye Survey. Invest Ophthalmol Vis Sci 45:4273–4276. https://doi.org/10.1167/iovs.04-0285
Nixon E, Simpkins JW (2012) Neuroprotective effects of nonfeminizing estrogens in retinal photoreceptor neurons. Invest Ophthalmol Vis Sci 53:4739–4747. https://doi.org/10.1167/iovs.12-9517
Nuzzi R, Scalabrin S, Becco A, Panzica G (2018) Gonadal hormones and retinal disorders: a review. Front Endocrinol (Lausanne) 9:66–66. https://doi.org/10.3389/fendo.2018.00066
Oettli A, Gugleta K, Kochkorov A, Katamay R, Flammer J, Orgul S (2011) Rigidity of retinal vessel in untreated eyes of normal tension primary open-angle glaucoma patients. J Glaucoma 20:303–306. https://doi.org/10.1097/IJG.0b013e3181e666a1
Ondricek AJ, Kashyap AK, Thamake SI, Vishwanatha JK (2012) A comparative study of phytoestrogen action in mitigating apoptosis induced by oxidative stress. In Vivo 26:765–775
Pasquale LR, Kang JH (2011) Female reproductive factors and primary open-angle glaucoma in the Nurses' Health Study. Eye (Lond) 25:633–641. https://doi.org/10.1038/eye.2011.34
Pasquale LR, Rosner BA, Hankinson SE, Kang JH (2007) Attributes of female reproductive aging and their relation to primary open-angle glaucoma: a prospective study. J Glaucoma 16:598–605. https://doi.org/10.1097/IJG.0b013e318064c82d
Pasquale LR et al (2013) Estrogen pathway polymorphisms in relation to primary open angle glaucoma: an analysis accounting for gender from the United States. Mol Vis 19:1471–1481
Patel P et al (2018) Effects of sex hormones on ocular blood flow and intraocular pressure in primary open-angle glaucoma: a review. J Glaucoma 27:1037–1041. https://doi.org/10.1097/ijg.0000000000001106
Paterson GD, Miller SJ (1963) Hormonal influence in simple glaucoma. A preliminary report. Br J Ophthalmol 47:129–137. https://doi.org/10.1136/bjo.47.3.129
Peltoketo H, Vihko P, Vihko R (1998) Regulation of estrogen action: role of 17β-hydroxysteroid dehydrogenases. In: Litwack G (ed) Vitamins and hormones. Academic Press, San Diego, pp 353–398
Pemp B, Georgopoulos M, Vass C, Fuchsjäger-Mayrl G, Luksch A, Rainer G, Schmetterer L (2009) Diurnal fluctuation of ocular blood flow parameters in patients with primary open-angle glaucoma and healthy subjects. Br J Ophthalmol 93:486–491. https://doi.org/10.1136/bjo.2008.148676
Phelps CD, Corbett JJ (1985) Migraine and low-tension glaucoma. A case-control study. Invest Ophthalmol Vis Sci 26:1105–1108
Prokai-Tatrai K, Xin H, Nguyen V, Szarka S, Blazics B, Prokai L, Koulen P (2013) 17beta-estradiol eye drops protect the retinal ganglion cell layer and preserve visual function in an in vivo model of glaucoma. Mol Pharm 10:3253–3261. https://doi.org/10.1021/mp400313u
Quigley HA (2011) Glaucoma. Lancet 377:1367–1377. https://doi.org/10.1016/s0140-6736(10)61423-7
Quigley HA, Broman AT (2006) The number of people with glaucoma worldwide in 2010 and 2020. Br J Ophthalmol 90:262–267. https://doi.org/10.1136/bjo.2005.081224
Raghava N, Das BC, Ray SK (2017) Neuroprotective effects of estrogen in CNS injuries: insights from animal models. NeurosciNeuroecon 6:15–29. https://doi.org/10.2147/NAN.S105134
Revankar CM, Cimino DF, Sklar LA, Arterburn JB, Prossnitz ER (2005) A transmembrane intracellular estrogen receptor mediates rapid cell signaling. Science 307:1625–1630. https://doi.org/10.1126/science.1106943
Riccadonna M et al (2003) Autonomic system activity and 24-hour blood pressure variations in subjects with normal- and high-tension glaucoma. J Glaucoma 12:156–163. https://doi.org/10.1097/00061198-200304000-00011
Rudnicka AR, Mt-Isa S, Owen CG, Cook DG, Ashby D (2006) Variations in primary open-angle glaucoma prevalence by age, gender, and race: a Bayesian meta-analysis. Invest Ophthalmol Vis Sci 47:4254–4261. https://doi.org/10.1167/iovs.06-0299
Russo R et al (2008) 17Beta-estradiol prevents retinal ganglion cell loss induced by acute rise of intraocular pressure in rat. Prog Brain Res 173:583–590. https://doi.org/10.1016/S0079-6123(08)01144-8
Sator MO et al (1998) Reduction of intraocular pressure in a glaucoma patient undergoing hormone replacement therapy. Maturitas 29:93–95. https://doi.org/10.1016/s0378-5122(97)00091-1
Schmidl D, Schmetterer L, Garhofer G, Popa-Cherecheanu A (2015) Gender differences in ocular blood flow. Curr Eye Res 40:201–212. https://doi.org/10.3109/02713683.2014.906625
Siesky BA et al (2008) Comparison of visual function and ocular hemodynamics between pre- and post-menopausal women. Eur J Ophthalmol 18:320–323. https://doi.org/10.1177/112067210801800228
Simpkins JW, Yang SH, Sarkar SN, Pearce V (2008) Estrogen actions on mitochondria–physiological and pathological implications. Mol Cell Endocrinol 290:51–59. https://doi.org/10.1016/j.mce.2008.04.013
Stoilov I, Akarsu AN, Sarfarazi M (1997) Identification of three different truncating mutations in cytochrome P4501B1 (CYP1B1) as the principal cause of primary congenital glaucoma (Buphthalmos) in families linked to the GLC3A locus on chromosome 2p21. Hum Mol Genet 6:641–647. https://doi.org/10.1093/hmg/6.4.641
Stone EM et al (1997) Identification of a gene that causes primary open angle glaucoma. Science 275:668–670. https://doi.org/10.1126/science.275.5300.668
Su WW, Cheng ST, Ho WJ, Tsay PK, Wu SC, Chang SH (2008) Glaucoma is associated with peripheral vascular endothelial dysfunction. Ophthalmology 115:1173–1178.e1171. https://doi.org/10.1016/j.ophtha.2007.10.026
Tham Y-C, Li X, Wong TY, Quigley HA, Aung T, Cheng C-Y (2014) Global prevalence of glaucoma and projections of glaucoma burden through 2040: a systematic review and meta-analysis. Ophthalmology 121:2081–2090. https://doi.org/10.1016/j.ophtha.2014.05.013
Tielsch JM, Sommer A, Katz J, Royall RM, Quigley HA, Javitt J (1991) Racial variations in the prevalence of primary open-angle glaucoma. The Baltimore Eye Survey. JAMA 266:369–374
Tint NL, Alexander P, Tint KM, Vasileiadis GT, Yeung AM, Azuara-Blanco A (2010) Hormone therapy and intraocular pressure in nonglaucomatous eyes. Menopause 17:157–160. https://doi.org/10.1097/gme.0b013e3181b82fb4
Tobe LA et al (2012) Should men and women be managed differently in glaucoma? OphthalmolTher 1:1. https://doi.org/10.1007/s40123-012-0001-0
Toker E, Yenice O, Akpinar I, Aribal E, Kazokoglu H (2003a) The influence of sex hormones on ocular blood flow in women. ActaOphthalmolScand 81:617–624. https://doi.org/10.1111/j.1395-3907.2003.00160.x
Toker E, Yenice O, Temel A (2003b) Influence of serum levels of sex hormones on intraocular pressure in menopausal women. J Glaucoma 12:436–440
Tokunaga T, Kashiwagi K, Tsumura T, Taguchi K, Tsukahara S (2004) Association between nocturnal blood pressure reduction and progression of visual field defect in patients with primary open-angle glaucoma or normal-tension glaucoma. Jpn J Ophthalmol 48:380–385. https://doi.org/10.1007/s10384-003-0071-6
Topouzis F et al (2011) Risk factors for primary open-angle glaucoma and pseudoexfoliative glaucoma in the Thessaloniki Eye Study American. J Ophthalmol 152:219–228.e211. https://doi.org/10.1016/j.ajo.2011.01.032
Vajaranant TS, Grossardt BR, Maki PM, Pasquale LR, Sit AJ, Shuster LT, Rocca WA (2014) Risk of glaucoma after early bilateral oophorectomy. Menopause 21:391–398. https://doi.org/10.1097/GME.0b013e31829fd081
Vajaranant TS et al (2018) Racial differences in the effects of hormone therapy on incident open-angle glaucoma in a randomized trial. Am J Ophthalmol 195:110–120. https://doi.org/10.1016/j.ajo.2018.07.035
Vincent AL et al (2002) Digenic inheritance of early-onset glaucoma: CYP1B1, a potential modifier gene. Am J Hum Genet 70:448–460. https://doi.org/10.1086/338709
Vohra R, Aldana BI, Bulli G, Skytt DM, Waagepetersen H, Bergersen LH, Kolko M (2019) Lactate-mediated protection of retinal ganglion. Cells J MolBiol 431:1878–1888. https://doi.org/10.1016/j.jmb.2019.03.005
Wang X, Simpkins JW, Dykens JA, Cammarata PR (2003) Oxidative damage to human lens epithelial cells in culture: estrogen protection of mitochondrial potential, ATP, and cell viability. Invest Ophthalmol Vis Sci 44:2067–2075. https://doi.org/10.1167/iovs.02-0841
Wang L, Szklo M, Folsom AR, Cook NR, Gapstur SM, Ouyang P (2012) Endogenous sex hormones, blood pressure change, and risk of hypertension in postmenopausal women: the multi-ethnic study of atherosclerosis. Atherosclerosis 224:228–234. https://doi.org/10.1016/j.atherosclerosis.2012.07.005
Wang YE et al (2016) Oral contraceptive use and prevalence of self-reported glaucoma or ocular hypertension in the United States. Ophthalmology 123:729–736. https://doi.org/10.1016/j.ophtha.2015.11.029
Wensor MD, McCarty CA, Stanislavsky YL, Livingston PM, Taylor HR (1998) The prevalence of glaucoma in the Melbourne. Vis Impair Project Ophthalmol 105:733–739. https://doi.org/10.1016/s0161-6420(98)94031-3
Wickham LA, Gao J, Toda I, Rocha EM, Ono M, Sullivan DA (2000) Identification of androgen, estrogen and progesterone receptor mRNAs in the eye. Acta Ophthalmol Scand 78:146–153. https://doi.org/10.1034/j.1600-0420.2000.078002146.x
Wiermann A, Galambos P, Vafiadis J, Wagenfeld L, Richard G, Klemm M, Zeitz O (2007) Retrobulbarhaemodynamics in normal and high tension glaucoma patients: the diagnostic importance of tinnitus, migraine and Raynaud-like symptoms. KlinMonblAugenheilkd 224:396–400. https://doi.org/10.1055/s-2007-963118
Wilson MR (2002) Progression of visual field loss in untreated glaucoma patients and suspects in St Lucia, West Indies. Trans Am Ophthalmol Soc 100:365–410
Wong-Riley MT (2010) Energy metabolism of the visual system. Eye Brain 2:99–116. https://doi.org/10.2147/eb.S9078
Wu Q, Odwin-Dacosta S, Cao S, Yager JD, Tang W-y (2019) Estrogen down regulates COMT transcription via promoter DNA methylation in human breast cancer cells. Toxicol Appl Pharmacol 367:12–22. https://doi.org/10.1016/j.taap.2019.01.016
Yager JD (2015) Mechanisms of estrogen carcinogenesis: the role of E2/E1-quinone metabolites suggests new approaches to preventive intervention—a review. Steroids 99:56–60. https://doi.org/10.1016/j.steroids.2014.08.006
Yamashita H et al (2011) Functional and morphological effects of beta-estradiol in eyes with N-methyl-D-Aspartate-induced retinal neurotoxicity in rats. Exp Eye Res 93:75–81. https://doi.org/10.1016/j.exer.2011.04.006
Yamazaki Y, Drance SM (1997) The relationship between progression of visual field defects and retrobulbar circulation in patients with glaucoma. Am J Ophthalmol 124:287–295. https://doi.org/10.1016/s0002-9394(14)70820-7
Yanagida K et al (2015) Sex-related differences in ocular blood flow of healthy subjects using laser speckle flowgraphy. Invest Ophthalmol Vis Sci 56:4880–4890. https://doi.org/10.1167/iovs.15-16567
Yang SH et al (2004) Mitochondrial localization of estrogen receptor beta. Proc Natl Acad Sci USA 101:4130–4135. https://doi.org/10.1073/pnas.0306948101
Yu X et al (2004) Involvement of insulin/phosphoinositide 3-kinase/Akt signal pathway in 17 beta-estradiol-mediated neuroprotection. J Biol Chem 279:13086–13094. https://doi.org/10.1074/jbc.M313283200
Zorov DB, Juhaszova M, Sollott SJ (2014) Mitochondrial reactive oxygen species (ROS) and ROS-induced ROS release. Physiol Rev 94:909–950. https://doi.org/10.1152/physrev.00026.2013
Funding
The work is carried out as a part of the BRIDGE – Translational Excellence Programme (bridge.ku.dk) at the Faculty of Health and Medical Sciences, University of Copenhagen, funded by the Novo Nordisk Foundation (Grant Agreement No. NNF18SA0034956).
Author information
Authors and Affiliations
Contributions
Conceptualization: RV; Methodology: KF and RV; Validation: BSVT and MK; Investigation: KF, BSVT, MK, and RV; Writing—original draft preparation: KF, BSVT, and RV; Writing—review and editing: MK and RV.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflict of interest. The funders had no role in the design of the study; in the review or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fotesko, K., Thomsen, B.S.V., Kolko, M. et al. Girl Power in Glaucoma: The Role of Estrogen in Primary Open Angle Glaucoma. Cell Mol Neurobiol 42, 41–57 (2022). https://doi.org/10.1007/s10571-020-00965-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10571-020-00965-5