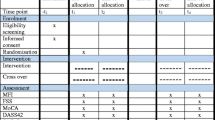
Objectives. To assess the efficacy and tolerance of Noofen in the treatment of chronic fatigue syndrome in patients with chronic cerebrovascular failure. Materials and methods. A total of 53 patients with cerebrovascular disease presenting active complaints of feelings of constant fatigue were studied; patients were randomized to form two groups. Patients of the study group (n = 33) received standard treatment and Noofen, while patients of the control group (n = 20) received only standard treatment. Treatment efficacy was assessed using the fatigue evaluation scale MFI-20, the Hospital Anxiety Scale HADS-A, and the Leeds Sleep Evaluation Questionnaire (LSEQ). The effectiveness of mental work was also assessed, using the Schulte test. Results and conclusions. Treatment with Noofen led to a marked decrease in the overall intensity of feelings of fatigue on the MFI-20 fatigue evaluation scale. Regression of fatigue intensity by 30–50% of baseline was seen in three quarters of the patients of the study group, and Noofen influenced reductions in all components of fatigue syndrome, including the mental components, and increased motivation. Reductions in the mental component of fatigue were combined with objective improvements in the effectiveness of mental work on the Schulte test. Thus, the effect of Noofen on the level of motivation and the mental component of fatigue can promote more effective cognitive training in patients with cerebrovascular failure.
Similar content being viewed by others
References
A. Lerdal, L. Bakken, S. Kouwenhoven, et al., “Poststroke fatigue: a review,” J. Pain Symptom Manage., 38, 928–949 (2009), https://doi.org/10.1016/j.jpainsymman.2009.04.028.
D. Christensen, S. P. Johnsen, T. Watt, et al., “Dimensions of post-stroke fatigue: a two-year follow-up study,” Cerebrovasc. Dis., 26, 134–141 (2008), https://doi.org/10.1159/000139660.
V. Schepers, A. Visser-Meily, M. Ketelaar, and E. Lindeman, “Post-stroke fatigue: course and its relation to personal and stroke-related factors,” Arch. Phys. Med. Rehabil., 87, 184–188 (2006), https://doi.org/10.1016/j.apmr.2005.10.005.
O. V. Vorob’eva, “Valdoxan in the treatment of depression in neurological practice: results of The Russian multicenter naturalistic study ‘Resonance,’” Neurosci. Behav. Physiol., 43, No. 9, 1126–1131 (2013), https://doi.org/10.1007/s11055-013-9860-7.
E. McGeough, A. Pollock, L. N. Smith, et al., “Interventions for post-stroke fatigue,” Cochrane Database Syst. Rev., 8, No. 3, CD007030 (2009), https://doi.org/10.1002/14651858.CD007030.pub2.
O. V. Vorob’eva and V. V. Rusaya, “Pharmacotherapy of anxiety disorders in patients with chronic cerebral ischemia,” Zh. Nevrol. Psikhiat., 116, No. 12, Iss. 2, 3–8 (2016), https://doi.org/10.17116/jnevro20161161223-8-2017.
E. M. A. Smets, B. Garssen, B. Bonke, and J. C. De Haes, “The multidimensional fatigue inventory (MFI) psychometric qualities of an instrument to assess fatigue,” J. Psychosom. Res., 39, No. 5, 315–325 (1995).
A. S. Zigmond and R. P. Snaith, “The Hospital Anxiety and Depression scale,” Acta Psychiatr. Scand., 67, 361–370 (1983), https://doi.org/10.1111/j1600-0447.
A. C. Parrott and I. Hindmarch, “Factor analysis of a sleep evaluation questionnaire,” Psychol. Med., 8, 325–329 (1978).
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Zhurnal Nevrologii i Psikhiatrii imeni S. S. Korsakova, Vol. 117, No. 11, Iss. 1, pp. 31–36, November, 2017.
Rights and permissions
About this article
Cite this article
Vorob’eva, O.V., Rusaya, V.V. Efficacy and Safety of Noofen in the Treatment of Chronic Fatigue Syndrome in Patients with Cerebrovascular Failure. Neurosci Behav Physi 49, 246–251 (2019). https://doi.org/10.1007/s11055-019-00722-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-019-00722-2