Abstract
Introduction
Glioblastoma multiforme (GBM) is a deadly brain tumor with a short expected median survival, despite current standard-of-care treatment. We explored the combination of intermediate stereotactic dose radiation therapy and immune checkpoint inhibitor therapy as a novel treatment strategy for GBM.
Methods
Glioma xenograft-bearing mice were exposed to high dose brain-directed radiation (10 Gy single exposure) as well as mouse anti-PD-1 antibody. The tumor-bearing animals were randomized to four groups: no treatment, radiation alone, anti-PD-1 alone, and radiation + anti-PD-1. Survival was followed, and tumor growth was monitored using MRI. Immunohistochemistry, gene expression arrays, and flow cytometry were used to characterize the treatment-induced effects. Pharmacologic inhibitors of T-lymphocytes, bone marrow derived macrophages, and microglia were used to assess the respective roles of different immune populations in observed treatment effects.
Results
We found the combined treatment with high dose radiation and immunotherapy to be highly effective with a 75% complete pathologic response and dramatically improved survival outcomes. We found both CD8+ T-cells and macrophages to be necessary for the full effect of combined therapy, with T lymphocytes appearing to play a role early on and macrophages mediating a later phase of the combined treatment effect. Radiation treatment appeared to trigger macrophage repolarization, increasing M1/M2 ratio.
Conclusions
These findings point to a novel immunologic mechanism underlying the interaction between radiotherapy and immunotherapy. They also provide the basis for clinical investigation of immunogenic dose radiation in combination with immune checkpoint blockade as a potential treatment approach for newly diagnosed high grade gliomas.
Similar content being viewed by others
Introduction
Glioblastoma multiforme (GBM) is the most aggressive of all brain tumors. It is also the most common, accounting for over 50% of primary brain cancers [1]. Current standard treatment with surgical resection followed by local fractionated radiation therapy and temozolomide yield a median survival of only about 14–16 months [2].
Previously, we showed in clinical studies that hypofractionated radiosurgery, also known as stereotactic radiotherapy (SRT), holds promise in improving local tumor control in the treatment of recurrent GBM [3,4,5]. We demonstrated superior local tumor control with this approach compared to treating the contrast-enhancing lesion only [3, 4]. This regimen has now been shown to result in significantly improved progression-free survival compared with the standard chemotherapeutic approach for recurrent GBM [5,6,7,8].
Recent studies have demonstrated that stereotactic dose RT can induce tumor immunogenicity and, strikingly, yield improved control of distant, unirradiated metastatic sites when administered in concert with immune checkpoint inhibitors in preclinical studies of several solid tumors outside the central nervous system [9,10,11,12]. The phenomenon of immune-mediated regression of unirradiated lesions, distant to the irradiated primary site, known as “abscopal effect”, has been reported both pre-clinically and clinically. The radiation-induced abscopal immune modulation was preferentially shown with “intermediate” stereotactic range radiation doses (8–10 Gy) rather than single high (> 18 Gy) doses [5].
Therefore, we hypothesized that the combined use of stereotactic dose RT and checkpoint blockade may cause immune phenomenon similar to the abscopal effect, but directed locally to eradicate the infiltrating GBM, rather than distant metastasis. To test this hypothesis, we evaluate the combined effects of SRT and anti-PD-1 blockade (aPD-1) in intracranial glioma-bearing mice.
Methods
Glioma mouse model system
Immunocompetent C57BL/6 mice were purchased from Charles River Breeding Lab (Wilmington, MA) and maintained on a 12:12 h light:dark cycle with food and water ad libitum. The GL261 cell is derived from a chemically-induced C57BL/6 murine astroglioma. The cells were transfected with an eGFP construct, generating the cell line GL261-eGFP, which has been characterized in an in vivo glioma model. Mice were transplanted stereotactically with the GL261-eGFP cells as previously described [13,14,15].
Mice were randomized to treatment groups on day 8 after tumor implantation. For survival studies, the mice were kept until death or maximum study duration of 90 days. For other studies, the mice were euthanized at the planned time points of experimental protocol or when they showed signs of neurologic deficits. To harvest the brain sample, mice were anesthetized with ketamine and xylazine before intracardiac perfusion with PBS followed by 4% PFA in PBS. The brains were removed and post-fixed in 4% PFA/PBS for 12 h followed by cryoprotection in 30% w/v sucrose for 48 h. All animal procedures were approved by the Stony Brook University Institutional Animal Care and Use Committee (IACUC).
Animal treatment
The randomized treatment groups were (1) control (no tumor), (2) sham treatment with tumor, (3) Radiation alone, (4) anti-PD-1 blockade only, (5) combined radiation and anti-PD-1 blockade. For radiation, a single dose radiation of 10 Gy to the brain on day 10 post-tumor implantation by using 100 kVp animal irradiator (Phillips RT-100). Immune check point inhibitor was given with 10 mg/kg of aPD-1, anti-mouse PD-1 antibody (clone RPM1-14, BioX Cell), by intraperitoneal injection immediately after radiation on day 10, and two more doses on day 12 and 14 post-tumor implantation. In order to inhibit lymphocyte trafficking, mice were also treated with 0.5 mg/kg of FTY720 i.p. every other day starting from day 8 during the study duration (ref). To deplete the bone marrow-derived macrophage mice were treated with 300 µg of anti CSF1-R (clone AFS98, BioXCell) i.p. every other day starting from day 8 during the study duration [16]. To inhibit microglial infiltration PLX5622 was formulated in an AIN-76 rodent diet at a dose of 1200 mg/kg standard chow provided by PLX5622 Inc.
MR imaging
The mice were imaged on days 15, 20 and on day 30 for surviving mice, by Bruker Biospec 7.0 T small animal MRI scanner with ADVANCE III hardware/software with 1H and X nuclide RF amplifiers and a 300 V/200A gradient power Copley amplifier. Various MR sequences including T1-weighted contrast and T2-weighed mages were used to measure the tumor volumes, and they were computed using standard analysis methods [17, 18].
Immunohistochemistry
The extracted brains were embedded in optimal cutting temperature compound (Tissue-Tek) and sectioned using Leica cryostat (Nussloch, Germany). Coronal Secttions (20-μm thick) throughout all tumor containing tissue were collected for analysis. The following primary antibodies were used: anti-Iba-1 (1:200; Wako Chemicals), CD8 (1:500, clone 53–7.6, eBioscience). Secondary antibodies against the appropriate species were incubated for 2 h at room temperature (Jackson, West Grove, PA, USA). 4,6-Diamidino-2-phenylindole (Sigma, 1 mg/ml) was used for 15 min to counterstain nuclei. For each section, random 40X confocal images within the center of the tumor were acquired with a Leica TCS SP8X confocal microscope and cell counting was performed using NIH Image J software.
ELISA
Blood samples from mice were collected at the time of cardiac puncture. After 30 min incubation at room temperature, the samples were centrifuged at 900 g for 10 min. Serum supernatant were analyzed by ELISA for mouse INF gamma (eBioscience, cat no 88-8314-22) according to the manufacturer’s instruction.
RNA extraction and gene expression assay
Tumor tissue was dissected at 11 and 15 days after tumor implant and RNA was isolated using Trizol reagent (Invitrogen) according to manufacturer’s instructions. Total RNA was further purified using a RNeasy Mini Kit and 0.5 ug of high quality total RNA (RIN > 7) was then reverse transcribed using the First Strand Synthesis Kit, and subsequently loaded on RT2 custom profiler array according to manufacturer’s instructions (Qiagen). Qiagen’s online web analysis tool was utilized to produce comparative heat maps and fold change was calculated by determining the ratio of mRNA levels to control values using the ΔCt method (2−ΔΔCt). All genes quantified are listed in Supplemental Table 1. Expression levels were normalized to the expression of housekeeping genes Gapdh and Tbp. PCR conditions used included a hold for 10 min at 95 °C, followed by 45 cycles of 15 s at 95 °C and 60 s at 60 °C.
Flow cytometry
Mouse brains were extracted, tumor tissue was micro-dissected and placed in ice cold FACS buffer (pH 7.40, 0.1 M PBS, 1 mM EDTA, 1% BSA, 50U/ml DNase I). Tissue was then subjected to digestion in papain (1 mg/ml) for 20 min at 37 °C followed by gentle trituration and 5 min centrifugation at 1500 rpm. The pellet was resuspended in 30% Percoll and spun for 10 min at 1500 rpm. The myelin debris containing top fraction was removed and 3× the volume of FACS buffer was added to the Percoll solution. Samples were spun for 15 min at 1500 rpm after which the pelleted fractions were resuspended in FACS buffer and passed through 40 μM cell strainer. The cells were blocked with anti-mouse CD16/32 (mouse BD Fc Block™) diluted in FACS buffer (1:50) for 30 min, and then were stained with fluorescent labeled antibodies for 30 min on ice. The antibody combination included macrophage lineage markers CD206-PE, CD11b-PE-Cy5, CD86-BV785 (BioLegend, 1:200); T cell markers CD3-BV605, CD4-PE-Cy7, CD8a-APC-Cy7 (BioLegend, 1:200), and PD-1-APC (BD Biosciences, 1:200), as well as leukocyte marker CD45(PerCP-Cy5.5 (BioLegend, 1:200). After incubation, the cells were washed with FACS buffer and fixed in 1% PFA. Samples were analyzed on a BD LSR Fortessa using BD FACSDiva software (BD Biosciences).
Statistical analysis
Survival data were analyzed by Kaplan–Meier curves with significance determined by long-rank test. For continuous outcomes, means were calculated and compared between experimental arms using ANOVA followed by Tukey’s post hoc t-test. Repeated ANOVA was used to analyze repeated measures over time. All data are presented as mean ± SEM of at least two independent experiments. P value less than 0.05 was considered as statistically significant.
Results
Combination of stereotactic dose RT and anti-PD-1 blockade results in markedly improved survival and pathologic complete response in glioma-bearing mice
There was a significant survival improvement in the group treated with combination of RT 10 Gy + anti-PD-1 blockade (aPD-1). The untreated glioma-bearing mice had a median survival of 22 days. Monotherapy with aPD-1 prolonged survival up to 30 days, and RT alone improved the median survival to 36 days. After combined RT and aPD-1 treatment, the median survival was not reached up to 60 days, and 75% of mice were alive at that time point. The Kaplan–Meier survival curves are shown in Fig. 1a. At the time of death and at the end of study on day 90, mice were sacrificed, and the whole mount brain samples were stained with H&E. The brain specimens of the surviving mice up to 60 days showed complete tumor disappearance with no microscopic evidence of disease after treatment with RT+ aPD-1 (Fig. 1c). MRI scans, taken at days 15, 22, and 30, showed significant delays in the average volumetric tumor growth in the RT+ aPD-1 groups, compared to tumor-bearing controls or other treatments groups (Fig. 1b and d).
Tumor cure and survival by high single dose radiation (RT 10 Gy) plus anti-PD-1 blockade. a Kaplan–Meier survival curves. Survival time was measured from the day of tumor implantation to death or maximum study duration of 60 days. Survival experiments were repeated twice independently with similar results, n = 6 CONTROL, n = 3 aPD-1, n = 8 RT and n = 7 RT+ aPD-1. Survival differences were determined by log-rank Mantel-Cox test. *P < 0.05. b Tumor growth delay by treatment groups. Tumors treated with SRT+ aPD1 showed significant reduction of the tumor volume compared to other treatment groups. Tumor volume was measured by T2-weighted MR image on days 15, 22, and 30 after tumor implantation. c Whole mount H&E stained brain sections at autopsy. The combined treatment with RT+ aPD-1 showed complete tumor disappearance on day 60 post-tumor implant in all the surviving mice. d Tumor growth delay curves with tumor volumes measured by MRI scan, n = 3–5 per group. Tumors treated with SRT+ aPD-1 showed significant reduction of the tumor volume. **P < 0.01 vs CONTROL by ANOVA followed by Tukey’s post hoc
Effects of radiation and anti-PD-1 blockade on CD8+ T-cell dynamics
We used IHC to examine the changes in immune effector cell dynamics. Non-tumor bearing controls did not exhibit any CD8+ staining. In the sham-treated tumor-bearing mice, there was an initial increase in the CD8+ T-cells induced by tumor growth on day 11 (24 h after treatment) which then remained at the same level until death. In the mice treated with aPD-1 alone, CD8+ T-cells did not significantly increase and followed a similar pattern to the sham-treated tumor-bearing controls. In contrast, radiation produced a delayed increase in CD8+ cells, suggesting influx of CD8+ cells to the tumor. By day 15 (5 days after treatment), the tumor infiltrating CD8+ T-cell populations in the mice treated with RT or RT+ aPD-1 rebounded with a fivefold increase compared to previous time point, and the CD8+ counts remained high in these groups at longer time points (Fig. 2a and b).
Role of immune effector cells in the intra-and peri-tumor environment in the brain. a Representative images of tumor CD8 IHC stain from brain sections collected on days 11 and 15 after tumor implant, scale bar = 100 µm. b Quantification of CD8+ cells in the brain sections by treatment groups on days 5, 8, 11, 15, 20 and 30 days after tumor implant, n = 6–8 per group. CD8+ T-cells were initially abrogated by radiation therapy (RT) alone or RT in combination with anti PD-1 blockade (RT+ aPD-1) on day 11 (P < 0.05 and P < 0.01 respectively), but restored in both groups on day 15
Gene expression array cluster analysis
Gene expression analysis on day 11 revealed results consistent with those of IHC. These are shown as a heatmap in Fig. 3a. Tumor growth by itself led to an up-regulation of CD8α expression. Treatment with aPD-1 alone did not yield additional CD8-α up-regulation. There was 1.5-fold up-regulation of CD8α in the RT alone group by gene expression analysis on day 11. Immunohistochemistry did not show CD8+ stained cells on day 11, but the CD8+ staining T-cells gradually increased at later time points (Fig. 2). Combined RT and anti-PD-1 showed 1.8-fold increase of CD8-α expression. Interestingly, FoxP3 expression was increased in RT alone group, but not in the RT+ aPD-1 group. In addition, the combined therapy induced up-regulation of Granzyme-b and Perforin-1, two key intermediaries of T cell cytotoxicity. The expression of the immune checkpoints PD-L1 and CTLA-4 was also increased by SRT alone as well as by the combined therapy.
a Gene expression heat map of selected immune markers. Heat map depicts the relative expression values in normal non-tumor-bearing brain tissue (NAÏVE), sham-treated GL261 tumor (CONTROL) and tumors treated with aPD-1 only, SRT only (RT) or combined therapy (RT+ aPD-1). Tissues were collected on 15 day after tumor implant. Scale bar represents the Z score value scaled by row. Each row corresponds to a different gene and n = 3 per group. b Western blot analysis of TBK1 phosphorylated at Ser172 and total TBK1 in whole cell lysates of control tumors and tumors dissected at various times after radiation (1–24 h, above lines). Extracts of THP-1 cells treated with LPS (1 mg/ml) was used as positive control, n = 3 per time point. c Western blot analysis of IRF phosphorylated at Ser396 and total IRF3 in whole cell lysates of control tumors and tumors dissected at various times after radiation (1–24 h, above lines). Extracts of A549 cells transfected with poly (I:C) was used as positive control, n = 3 per time point (d) QPCR analysis of different Interferon-responsive genes in controls tumors and tumors dissected 24 h after treatment with radiation or combined therapy (RT+ aPD-1), n = 3 per group. e Interferon-γ levels in serum on days 5, 8, 11, 15 and 30. INFγ significantly increased after SRT+ aPD-1. *P < 0.05 by Student’s t test, n = 12 CONTROL, n = 8 aPD-1, n = 19 RT and n = 18 RT+ aPD-1
Remarkably, RT alone elicited maximal changes in the expression of molecules important for the activation of immune cells, such as IFN-γ, MHC-II (H2-ab1), the MHC-II component CD74 and the co-stimulatory molecules CD40, CD80 and CD86. In addition, IFN-β was increased 1.5-fold in the combined RT+ aPD-1 group.
Because the actions of CD8+ T-lymphocytes are known to be mediated via IFN-γ, we also examined serum IFN-γ levels using ELISA. On day 11 (24 h after treatment) we observed an initial IFN-γ spike in mice receiving aPD-1 monotherapy, which disappeared by post-implant day 15 (Fig. 3b). However, by day 15 only those mice which had been treated with combination of SRT+ aPD-1 were found to have a sustained increase in serum IFN-γ level, corresponding with the improved tumor control and survival in this group. The serum IFN-γ levels appear to be even higher in those mice which were cured of their disease in the combined treatment group. In contrast, those mice which survived past day 30 after having been treated with SRT alone and ultimately succumbed to the glioma, did not show sustained increases in serum IFN-γ at later time points.
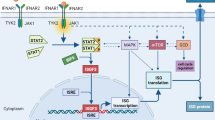
Previous studies showed that stereotactic high dose radiation and immune checkpoint blockade induced tumor cell release of IFN-beta and up-regulation of differential expression of interferon-stimulated genes (ISGs) mediated via IFN-β-dependent pathways, and irradiation resulted in cytoplasmic accumulation of tumor cell-derived double strand DNA. Cyclic GMP-AMP (cGAMP) synthase (cGAS), a sensor for cytoplasmic dsDNA, activated the downstream receptor STING via synthesis of 2′-3′- cGAMP leading to induction of ISGs [9,10,11]. Having observed a 1.5-fold increase in IFN-β expression levels after combined treatment in our model, we sought to investigate whether the cGAS-STING pathway and ISGs play a role in the therapeutic effect on glioma. To that end, we examined changes in ISG expression after RT as well as SRT+ aPD-1 treatments (Fig. 3c). Specifically, we looked at the ISGs that had been shown previously to be upregulated by SRT in other types of solid tumors [10, 11]. We also assessed for STING activation by checking the phosphorylation of its binding partners, TBK1 and IRF3 (Fig. 3d). These proteins are known to form a complex with STING upon activation with cGAS, and assessment of phosphorylated TBK1 and IRF3 has been identified as the most reliable way of detecting STING activation [19]. However, neither the gene expression studies of ISGs nor the co-IP to detect STING activation indicated any change with anti-PD-1 and RT treatment over untreated glioma-bearing mice, indicating that IFN-β-mediated pathways do not appear to play a role in our model system.
Proinflammatory effects induced by RT and anti-PD-1 on macrophages
Based on results of the gene expression array experiments, we sought to further examine the effects of RT and aPD-1 on macrophages and microglia in our glioma model system. Using IHC, we examined the distribution of cells positive for the macrophage/microglial marker Iba-1. Following treatment with combination of RT and aPD-1, we observed a distinct localization pattern of Iba-1-positive cells at the periphery of the tumor. Interestingly, the Iba-1+ cells displayed strong GFP signal within the cytoplasm, thus appearing to engulf the tumor cells. This finding strongly suggests phagocytosis. The microscopic images are shown in Fig. 4a and three-dimensional sections at higher magnification in Fig. 4b. Next, we used flow cytometry to assess the M1 (CD11b+CD86+) and M2 (CD11b+CD206+) macrophage dynamics. RT stimulated M1 but not M2, increasing the M1/M2 ratio (Fig. 4c and d).
Migration and polarization of macrophage after SRT and anti-PD-1 blockade treatment. a Representative 40× images Iba1 IHC stain (white) in brain sections collected on day 15 after tumor implant. Tumor cells are GFP+ (green). Scale bar = 100 µm. Note that the Iba-1 positive cells appear to engulf (red arrowheads) the GFP+ tumor cells in both SRT and SRT+ aPD-1 groups. b Higher magnification image (80X) of specimen from SRT+ aPD-1. Note that the GFP+ vesicles present within the cytoplasm of Iba-1 + macrophages on three-dimensional cross-sectional images. c The number of phagocytic-appearing macrophages from 10 microscopic fields with a 40X magnification objective, n = 3 per group, **P < 0.01 by ANOVA followed by Tukey’s post hoc. d The flow cytometry contour plots on day 15 post implantation show the differential expression of CD86 and CD206 in CD45+CD11b + macrophages. e Percentages of M1-like (CD86+) and M2-like (CD206+) macrophages and the ratio of M1/M2 in the treatment groups. SRT induced a significant increase of M1 macrophages, n = 6 per group, *P < 0.05 and **P < 0.01 by ANOVA followed by Tukey’s post hoc
Therapeutic effects of radiation and anti-PD-1 blockade: role of T-cells, macrophages, and microglia
We used FTY720, which is well-known to inhibit CNS infiltration of T-lymphocytes and has been previously studied in our laboratory [20]. To distinguish between bone marrow-derived macrophages and resident microglia, we used PLX5622 reagent which is known to inhibit only the microglia [16]. Conversely, we used CSF1R antibody that inhibits the bone-marrow derived macrophages but not the microglia [21]. As shown in Fig. 5a, all three inhibitors partially abrogated the survival outcome of combined therapeutic effects. The median survival time was > 60 days in the RT+ aPD-1 group without any inhibitors mirroring our initial findings. However, the median survival times were 34 days in the RT+ aPD-1 + FTY720 group, and 47.5 days in the RT+ aPD-1 + anti-CSF1R group as well as in the RT+ aPD-1 + PLX5622 group. This finding indicates that all three immune populations are required for full immune-mediated effect. From this differential survival time, we observe that the T-lymphocytes appear to play a role mediating an earlier phase of the survival time, and the macrophages mediating a later phase of the combined treatment effect. Using flow cytometry, we also accessed PD-1 expression on immune cell type. As can be seen in Fig. 5d and e, PD-1 expression was found uniquely on T-lymphocytes (CD45+CD3+) but not on macrophages/microglia (CD45+CD11b+). PD-1 expression on T-lymphocytes was not altered by RT, alone or combined with aPD-1.
Roles of immune effector cells on survival. a Kaplan-Meyer survival curves. Survival time was measured from the day of tumor implantation to death or maximum study duration of 60 days. There was significant decrease of survival in all 3 groups of the CD8-depleted (by FTY720), macrophage-depleted (by anti-CSF1R), and microglia-depleted (by PLX5622) groups. Survival experiments were repeated twice independently with similar results, n = 6 CONTROL, n = 8 RT and n = 7 RT+ aPD-1, n = 9 RT+ aPD-1 + FTY, n = 9 RT+ aPD-1 + aCSF1R and n = 6 RT+ aPD-1 + PLX5622. Survival differences were determined by log-rank Mantel-Cox test. b Flow cytometry histograms of PD-1 surface expression on T cells (CD45+ CD3+) and macrophages (CD45+CD11b+) isolated from the tumors. As a negative control, cells were not stained with the PD-1 antibody (fluorescence-minus-one [FMO]). c Percentages of PD-1 expression in T cells and macrophages n = 3 per group, ***P < 0.001 by two-way ANOVA
Discussion
The results of our study establish the role of macrophages in the therapeutic effect of combined radiation and anti-PD-1 treatment of intracranial glioma. Our experiments, using FTY720 to block T-lymphocytes, CSF1R antibody to block bone marrow-derived macrophages, and PLX5622 to block microglia, indicate that all three of these immune cell populations are necessary for full therapeutic effect. While the role of T-lymphocytes in mediating the effects of radiotherapy in combination with immunotherapy was previously reported by Zeng and colleagues [22], macrophages and microglia are identified as key mediators for the first time.
Inhibition of T-lymphocyte infiltration with FTY720 reduced the survival time similar to that of SRT alone. This finding again supports the role of T-lymphocytes in mediating the immune response. Equally important is that inhibition of macrophages with anti-CSF1R and inhibition of microglia with PLX5622 both abrogate the combined effects of RT+ anti-PD-1 in the longer-term survival. In fact, the degree to which the therapeutic effects were inhibited seemed to precisely correspond to the decrease seen in the target immune cell population with each of the inhibitors. PD-1 expression was found uniquely on T-lymphocytes (CD3+) but not on macrophages/microglia (CD45+). Since the effects of anti-PD-1 therapy are mediated primarily via T-lymphocytes, our survival studies indicate that T lymphocytes appear to play a role early on and macrophages mediate a later phase of the combined treatment effect. Of note, anti-PD-1 alone did not improve survival, while RT alone imparted a modest benefit. The additional survival benefit appears to be due macrophage-mediated effects, particularly those related to M1 macrophages. Since PD-1 expression was not from macrophages, it may be the downstream effect of radiation, rather than anti-PD-1 therapy. Our results also generate another hypothesis that macrophage-mediated immune response may contribute to the long-term survival.
Our results indicates that stereotactic dose RT plays a dual role: (1) improving tumor control and survival of glioma-bearing mice, and (2) synergistically potentiating the immune response by increasing influx of CD-8+ lymphocytes and macrophages, particularly increasing the M1/M2 ratio by the combined therapy with radiation and PD-1 checkpoint blockade. Future studies are needed to elucidate the specific immunological mechanisms and molecular signaling cascade of the participating immune cells. These results also provide the basis for evaluating the combined therapy with stereotactic dose RT and PD-1 blockade in early clinical protocols for GBM.
References
Ostrom QT, Gittleman H, Liao P, Vecchione-Koval T, Wolinsky Y, Kruchko C, Barnholtz-Sloan JS (2017) CBTRUS statistical report: Primary brain and other central nervous system tumors diagnosed in the United States in 2010–2014. Neuro Oncol 19(suppl_5):v1–v88
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJ, Belanger K, Brandes AA, Marosi C, Bogdahn U, Curschmann J, Janzer RC, Ludwin SK, Gorlia T, Allgeier A, Lacombe D, Cairncross JG, Eisenhauer E, Mirimanoff RO (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352:987–996
Patel M, Siddiqui F, Liu M, Scarpace L, Jin JY, Mikkelsen T, Movsas B, Ryu S (2009) Salvage radiosurgery of recurrent high grade glioma: Radiographic tumor control and clinical outcome. J Neuro-Oncol 92:185–191
Kim EY, Yechieli RL, Kim JK, Mikkelsen T, Kalkanis S, Rock JP, Ryu S (2014) Patterns of failure after radiosurgery to two different target volumes of enhancing lesions with and without FLAIR abnormalities in recurrent glioblastoma multiforme. J Neurooncol 116(2):291–297
Modh A, Bergman D, Siddiqui MS, Schultz L, Krozek, E, Scarpace L, Mikkelsen T, Ryu S (2018) Randomized prospective trial of stereotactic radiosurgery versus chemotherapy for recurrent malignant glioma after second-line chemotherapy , Abstract 505376 (RTHP-06), Annual meeting of society of Neurooncology 2018
Holt DE, Bernard ME, Quan K, Clump DA (2016) Salvage stereotactic radiosurgery for recurrent glioblastoma multiforme with prior radiation therapy. J Cancer Res Ther 12(4):1243–1248
Pollom EL, Fujimoto D, Wynne J, Seiger K (2017) Phase 1/2 trial of 5-fraction stereotactic radiosurgery with 5-mm margins with concurrent and adjuvant temozolomide in newly diagnosed supratentorial glioblastoma: health-related quality of life results. Int J Radiat Oncol Biol Phys 98(1):123–130
Greer L, Pannullo SC, Smith AW, Taube S (2017) Accelerated hypofractionated radiotherapy in the era of concurrent temozolomide chemotherapy in elderly patients with glioblastoma multiforme. Cureus 9(6):e1388
Vanpouille-Box C, Alard A, Aryankalayil MJ, Sarfraz Y (2017) DNA exonuclease Trex1 regulates radiotherapy-induced tumour immunogenicity. Nat Commun 8:15618
Motani K, Ito S, Nagata S (2015) DNA-mediated cyclic GMP-AMP synthase-dependent and -independent regulation of innate immune responses. J Immunol 194(10):4914–4923
Wang F, Alain T, Szretter KJ, Stephenson K (2016) S6K-STING interaction regulates cytosolic DNA-mediated activation of the transcription factor IRF3. Nat Immunol 17(5):514–522
Pépin G, Gantier MP (2017) cGAS-STING activation in the tumor microenvironment and its role in cancer immunity. Adv Exp Med Biol 1024:175–194
Zagzag D, Miller DC, Chiriboga L, Yee H, Newcomb EW (2003) Green fluorescent protein immunohistochemistry as a novel experimental tool for the detection of glioma cell invasion in vivo. Brain Pathol 13(1):34–37
Patel MA, Kim JE, Theodros D, Tam A, Velarde E, Kochel CM, Francica B, Nirschl TR, Ghasemzadeh A, Mathios D, Harris-Bookman S, Jackson CC, Jackson C, Ye X, Tran PT, Tyler B, Coric V, Selby M, Brem H, Drake CG, Pardoll DM, Lim M (2016) Agonist anti-GITR monoclonal antibody and stereotactic radiation induce immune-mediated survival advantage in murine intracranial glioma. J Immunother Cancer 4:28
Kim JE, Patel MA, Mangraviti A, Kim ES, Theodros D, Velarde E, Liu A, Sankey EW, Tam A, Xu H, Mathios D, Jackson CM, Harris-Bookman S, Garzon-Muvdi T, Sheu M, Martin AM, Tyler BM, Tran PT, Ye X, Olivi A, Taube JM, Burger PC, Drake CG, Brem H, Pardoll DM, Lim M (2017) Combination therapy with Anti-PD-1, Anti-TIM-3, and focal radiation results in regression of murine gliomas. Clin Cancer Res 23(1):124–136
Acharya MM, Green KN, Allen BD, Najafi AR, Syage A, Minasyan H, Le MT, Kawashita T, Giedzinski E, Parihar VK, West BL, Baulch JE, Limoli CL (2016) Elimination of microglia improves cognitive function following cranial irradiation. Sci Rep 6:31545
Brockmann MA, Ulmer S, Leppert J, Nadrowitz R, Wuestenberg R, Nolte I, Petersen D, Groden C, Giese A, Gottschalk S (2006) Analysis of mouse brain using a clinical 1.5 T scanner and a standard small loop surface coil. Brain Res 1068(1):138–142
Mitsuda M, Yamaguchi M, Furuta T, Nabetani A, Hirayama A, Nozaki A, Niitsu M, Fujii H (2011) Multiple-animal MR imaging using a 3T clinical scanner and multi-channel coil for volumetric analysis in a mouse tumor model. Magn Reson Med Sci 10(4):229–237
Wang F, Alain T, Szretter KJ, Stephenson K, Pol JG, Atherton MJ, Hoang HD, Fonseca BD, Zakaria C, Chen L, Rangwala Z, Hesch A, Chan ESY, Tuinman C, Suthar MS, Jiang Z, Ashkar AA, Thomas G, Kozma SC, Gale M Jr, Fitzgerald KA, Diamond MS, Mossman K, Sonenberg N, Wan Y, Lichty BD (2016) S6K-STING interaction regulates cytosolic DNA-mediated activation of the transcription factorIRF3. Nat Immunol 17(5):514–522
Stessin AM, Banu MA, Clausi MG, Berry N, Boockvar JA, Ryu S (2017) FTY720/fingolimod, an oral S1PR modulator, mitigates radiation induced cognitive deficits. Neurosci Lett 658:1–5
Priceman SJ, Sung JL, Shaposhnik Z, Burton JB, Torres-Collado AX, Moughon DL, Johnson M, Lusis AJ, Cohen DA, Iruela-Arispe ML, Wu L (2010) Targeting distinct tumor-infiltrating myeloid cells by inhibiting CSF-1 receptor: combating tumor evasion of antiangiogenic therapy. Blood 115(7):1461–1471
Zeng J, See AP, Phallen J, Jackson CM, Belcaid Z, Ruzevick J, Durham N, Meyer C, Harris TJ, Albesiano E, Pradilla G, Ford E, Wong J, Hammers HJ, Mathios D, Tyler B, Brem H, Tran PT, Pardoll D, Drake CG, Lim M (2013) Anti-PD-1 blockade and stereotactic radiation produce long-term survival in mice with intracranial gliomas. Int J Radiat Oncol Biol Phys 86(2):343–349
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no potential conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Stessin, A.M., Clausi, M.G., Zhao, Z. et al. Repolarized macrophages, induced by intermediate stereotactic dose radiotherapy and immune checkpoint blockade, contribute to long-term survival in glioma-bearing mice. J Neurooncol 147, 547–555 (2020). https://doi.org/10.1007/s11060-020-03459-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-020-03459-y