Abstract
Purpose
Sleep and sleep position have a significant impact on physical, cardiac and mental health, and have been evaluated in numerous studies particularly in terms of lateral sleeping positions and their association with diseases. We retrospectively examined the relationship between the sleeping position and position-specific apnea-hypopnea index (AHI) in obstructive sleep apnea-hypopnea (OSA) patients.
Methods
We assessed the sleeping body position and the body position-specific AHI score in patients who were referred for suspected OSA and underwent diagnostic nocturnal polysomnography. In order to eliminate inter-individual differences, only those who had a similar percentage of time spent in the LSSP and RSSP for each patient were enrolled. To provide this validity, only subjects that had a similar percentage of left and right lateral sleep time (±10%) were included in the analysis.
Results
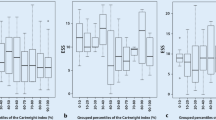
A total of 864 patients had nocturnal diagnostic PSG. Of them, 131 patients met the inclusion criteria. The percent rate spent in the supine sleeping position (SSP) was 31.3 ± 18.7%, in the LSSP was 31.8 ± 10% and in the RSSP was 32.6 ± 10.8%. Whereas the SSP-specific AHI score was the highest with 60.4 ± 36.2/h among all the sleeping position-specific AHI scores (p < 0.001), the LSSP-specific AHI score was statistically higher than that for RSSP (30.2 ± 32.6/h vs. 23.6 ± 30.1/h; p < 0.001). When comparing individuals sub-grouped based on OSA severity, there was a statistically significant difference between the LSSP-specific AHI score and RSSP-specific AHI score in patients with severe (p = 0.002) and moderate (p = 0.026), but not mild (p = 0.130) OSA.
Conclusion
We found that the sleeping position had a significant influence on apneic events and RSSP decreased the frequency of obstructive respiratory events in patients with moderate and severe disease.
Similar content being viewed by others
References
Roffwarg HP, Muzio JN, Dement WC (1966) Ontogenetic development of the human sleep-dream cycle. Science 152:604
Johnson HM, Swan TH, Wiegand AB (1930) In what positions do healthy people sleep? J Am Med Assoc 94:2058–2062
Dunkell S (1977) Sleep positions: the night language of the body. Heinemann, London
Pump B, Talleruphuus U, Chouristensen NJ, Warberg J, Norsk P (2002) Effects of supine, prone, and lateral positions on cardiovascular and renal variables in humans. Am J Physiol Regul Integr Comp Physiol 283:R174–R180
Naughton MT, Lorenzi-Filho G (2009) Sleep in heart failure. Prog Cardiovasc Dis 51:339–349
Palermo P, Cattadori G, Bussotti M, Apostolo A, Contini M, Agostoni P (2005) Lateral decubitus position generates discomfort and worsens lung function in chronic heart failure. Chest 128:1511–1516
Hallberg O, Johansson O (2010) Sleep on the right side—get cancer on the left? Pathophysiol 17:157–160
Phillips BA, Okeson J, Paesani D, Gilmore R (1986) Effect of sleep position on sleep apnea and parafunctional activity. Chest 90:424–429
D’Souza JM, D’Souza DH (2010) Sleeping position and the functioning of the brain: is there a link? Med Hypotheses 75:408
Pevernagie DA, Shepard JW Jr (1992) Relations between sleep stage, posture and effective nasal CPAP levels in OSA. Sleep 15:162–167
Jones AY (2004) Body position change and its effect on hemodynamic and metabolic status. Heart Lung 33:281–290
Banasik JL, Emerson RJ (2001) Effect of lateral positions on tissue oxygenation in the critically ill. Heart Lung 30:269–276
Backon J, Kullok S (1990) Why asthmatic patients should not sleep in the right lateral decubitus position. Br J Clin Pract 44:448–449
Khoury RM, Camacho-Lobato L, Katz PO, Castell DO (1999) Influence of spontaneous sleep positions on nighttime recumbent reflux in patients with gastroesophageal reflux disease. Am J Gastroenterol 94:2069–2073
Moreno MA, Furtner F (2009) Infant sleep position: back to sleep. Arch Pediatr Adolesc Med 163:1168
Farine D, Seaward PG (2007) When it comes to pregnant women sleeping, is left right? J Obstet Gynaecol Can 29:841–842
Domino G, Bohn SA (1980) Hypnagogic exploration: sleep positions and personality. J Clin Psychol 36:760–762
Sahlin C, Franklin KA, Stenlund H, Lindberg E (2009) Sleep in women: normal values for sleep stages and position and the effect of age, obesity, sleep apnea, smoking, alcohol and hypertension. Sleep Med 10:1025–1030
Cartwright R (1984) Effect of sleep position on sleep apnea severity. Sleep 7:110–114
Oksenberg A, Khamaysi I, Silverberg DS, Tarasiuk A (2000) Association of body position with severity of apneic events in patients with severe nonpositional obstructive sleep apnea. Chest 118:1018–1024
Elliott AR, Shea SA, Dijk DJ, Wyatt JK, Riel E, Neri DF, Czeisler CA, West JB, Prisk GK (2001) Microgravity reduces sleep disordered breathing in humans. Am J Respir Crit Care Med 164:478–485
Tanaka F, Nakano H, Sudo N, Kubo C (2009) Relationship between the body position-specific apnea-hypopnea index and subjective sleepiness. Respiration 78:185–190
Gouveris H, Selivanova O, Bausmer U, Goepel B, Mann W (2010) First-night-effect on polysomnographic respiratory sleep parameters in patients with sleep-disordered breathing and upper airway pathology. Eur Arch Otorhinolaryngol 267:1449–1453
The Report of an American Academy of Sleep Medicine Task Force (1999) Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. Sleep 22:667–689
Leung RS, Bowman ME, Parker JD, Newton GE (2003) Avoidance of the left lateral decubitus position during sleep in patients with heart failure: relationship to cardiac size and function. J Am Coll Cardiol 41:227–230
Fujita M, Miyamoto S, Sekiguchi H, Sasayama S (2000) Effects of posture on sympathetic nervous modulation in patients with chronic heart failure. Lancet 356:1822–1823
Chen GY, Kuo CD (1997) The effect of the lateral decubitus position on vagal tone. Anaesthesia 52:653–657
Stein P (1952) Tendency toward hypotension in left lateral recumbency. AMA Arch Intern Med 90:234–242
Lange RA, Katz J, McBride W, Moore DM Jr, Hillis LD (1988) Effects of supine and lateral positions on cardiac output and intracardiac pressures. Am J Cardiol 62:330–333
Shanoudy H, Soliman A, Raggi P, Liu JW, Russell DC, Jarmukli NF (1998) Prevalence of patent foramen ovale and its contribution to hypoxemia in patients with obstructive sleep apnea. Chest 113:91–96
Beelke M, Angeli S, Del Sette M, Gandolfo C, Cabano ME, Canovaro P, Nobili L, Ferrillo F (2003) Prevalence of patent foramen ovale in subjects with obstructive sleep apnea: a transcranial Doppler ultrasound study. Sleep Med 4:219–223
Beelke M, Angeli S, Del Sette M, De Carli F, Canovaro P, Nobili L, Ferrillo F (2002) Obstructive sleep apnea can be provocative for right-to-left shunting through a patent foramen ovale. Sleep 25:856–862
Chen GP, Goldberg SL, Gill EA Jr (2005) Patent foramen ovale and the platypnea-orthodeoxia syndrome. Cardiol Clin 23:85–89
Tada T, Fujita M, Goto T, Tamura T, Ono K, Kita T, Takahashi K, Osada H, Sakata R, Kimura T (2010) A case with sudden onset of position-dependent hypoxemia caused by reopening of foramen ovale. Journal of Cardiology Cases 1:e88–e91
Acknowledgment
We wish to thank all personnel of the Archive Section and our secretaries in the Cardiology Departmant, Mrs. Selda Avci Bal and Mrs. Arzu Eryigit, for their kind help with data collection.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ozeke, O., Erturk, O., Gungor, M. et al. Influence of the right- versus left-sided sleeping position on the apnea-hypopnea index in patients with sleep apnea. Sleep Breath 16, 617–620 (2012). https://doi.org/10.1007/s11325-011-0547-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-011-0547-4