Abstract
The study of upward spill over on parents of their offspring’s education is vital for understanding the family dynamics and role of adult children in the decisions of parents. Such association has widespread implication and application on ageing policies. We use pooled data from population-based cross-sectional health consumption surveys conducted by the National Sample Survey Organization in 2014 and 2018 (rounds 71 and 75, respectively) in this study. The analysis is restricted to individuals aged 60 and above, who are head of the household or their spouse and have children aged 25 years or above. The analysis is carried out for inpatient and outpatient cases separately. For inpatient analysis, the dependent variable is designed as a rank variable representing an increasing level of health care utilization. For the same partial proportional odds are calculated. For outpatient cases, the dependent variable is binary that takes the value 0 if the parents use public facilities and 1 if private facilities are used. Here, binary logistic regression is used for analysis. The odds of parents using a higher level of inpatient as well as outpatient health care are higher for those with better-educated children (inpatient: OR are 2.6 (p < 0.001, CI: 2.0–3.5); outpatient: OR are 1.5 (p < 0.001, CI: 1.1–2.2)). Education of children does influence the level of health care utilization among parents. Therefore, policy interventions can target offspring of working age group, who can assimilate information better and transfer it to their parents.


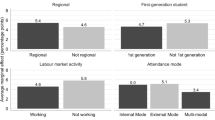
Source of data: NSSO rounds 71 (2014) and 75 (2018)
Similar content being viewed by others
Data availability
The data from National Sample Survey Organization is freely available on http://www.icssrdataservice.in/datarepository/index.php/catalog/MoSPI-NSS.
Code availability
STATA codes are available on request.
References
Lee R, Mason A. Population aging and the generational economy: a global perspective. East West Centre, Hawaii; 2011.
Dubow EF, Boxer P, Huesmann LR. Long-term effects of parents’ education on children’s educational and occupational success: mediation by family interactions, child aggression, and teenage aspirations. Merrill Palmer Q. 2009;55(3):224–49. https://doi.org/10.1353/mpq.0.0030.
Aslam M, Kingdon GG. Parental education and child health—understanding the pathways of impact in Pakistan. World Dev. 2012. CSAE Working Paper Series (40). https://doi.org/10.1016/j.worlddev.2012.05.007.
Kvaavik E, Glymour M, Klepp K, Tell G, Batty, G. Parental education as a predictor of offspring behavioural and physiological cardiovascular disease risk factors. Eur J Public Health. 2012. https://doi.org/10.1093/eurpub/ckr106.
Rowe M, Denmark N, Harden B, Stapleton L. The role of parent education and parenting knowledge in children’s language and literacy skills among White, Black, and Latino families. Infant Child Dev. 2016. https://doi.org/10.1002/icd.1924.
Caldwell J. Toward a restatement of demographic transition theory. Popul Dev Rev. 1976. https://doi.org/10.2307/1971615.
Chou KL. Parental repayment hypothesis in intergenerational financial transfers from adult children to elderly parents: evidence from Hong Kong. Educ Gerontol. 2008;34(9):788–99. https://doi.org/10.1080/03601270802095972.
Adamchak DJ, Wilson AO, Nyanguru A, Hampson J. Elderly support and intergenerational transfer in Zimbabwe: an analysis by gender, marital status, and place of residence. Gerontologist. 1991;31(4):505–13. https://doi.org/10.1093/geront/31.4.505.
Knodel J, Friedman J, Troung A, Bui C. Intergenerational exchanges in Vietnam: family size, sex composition, and the location of children. Popul Stud. 2000;54:89–104. https://doi.org/10.1080/713779067.
Lillard LA, Willis RJ. Motives for intergenerational transfers: evidence from Malaysia. Demography. 1997;34(1):115–34. https://doi.org/10.2307/2061663.
De Neve JW, Kawachi I. Spill overs between siblings and from offspring to parents are understudied: a review and future directions for research. Soc Sci Med. 2017;183:56–61. https://doi.org/10.1016/j.socscimed.2017.04.010.
Thoma B, Sudharsanan N, Karlsson O, Joe W, Subramanian SV, De Neve J. Children’s education and parental old-age health: evidence from a population-based, nationally representative study in India. Popul Stud. 2020;75(1):51–66. https://doi.org/10.1080/00324728.2020.1775873.
Lee C, Glei DA, Goldman N, Weinstein M. Children’s education and parents’ trajectories of depressive symptoms. J Health Soc Behav. 2017;58(1):86–101. https://doi.org/10.1177/0022146517690200.
Lee Y. Adult children’s educational attainment and the cognitive trajectories of older parents in South Korea. Soc Sci Med. 2018;209:76–85. https://doi.org/10.1016/j.socscimed.2018.05.026.
Sabater A, Graham E. The role of children’s education for the mental health of aging migrants in Europe. GeroPsych. 2016;29(2):81–92. https://doi.org/10.1024/1662-9647/a000145.
Zimmer Z, Liu X, Hermalin A, Chuang Y. Educational attainment and transitions in functional status among older Taiwanese. Demography. 1998;35(3):361–75.
Yahirun JJ, Sheehan CM, Hayward MD. Adult children’s education and parents’ functional limitations in Mexico. Res Aging. 2016;38(3):322–45. https://doi.org/10.1177/0164027515620240.
Friedman EM, Mare RD. The schooling of offspring and the survival of parents. Demography. 2014;51(4):1271–93. https://doi.org/10.1007/s13524-014-0303-z.
Jiang N. Adult children’s education and later-life health of parents in china: the intergenerational effects of human capital investment. Soc Ind Res. 2019;145(1):257–78. https://doi.org/10.1007/s11205-019-02109-9.
Zimmer Z, Martin LG, Ofstedal MB. Education of adult children and mortality of their elderly parents in Taiwan. Demography. 2007. https://doi.org/10.1353/dem.2007.0020.
Torssander J. From child to parent? The significance of children’s education for their parents’ longevity. Demography. 2013. https://doi.org/10.1007/s13524-012-0155-3.
Yang L, Martikainen P, Silventoinen K. Effects of individual, spousal, and offspring socioeconomic status on mortality among elderly people in China. J Epidemiol. 2016; 26(11):602–609. https://doi.org/10.2188/jea.JE20150252.
De Neve JW, Fink G. Children’s education and parental old age survival - quasi-experimental evidence on the intergenerational effects of human capital investment. J Health Econ. 2018;58:76–89. https://doi.org/10.1016/j.jhealeco.2018.01.008.
De Neve JW, Harling G. Offspring schooling associated with increased parental survival in rural KwaZulu-Natal, South Africa. Soc Sci Med. 2017;176:149–57. https://doi.org/10.1016/j.socscimed.2017.01.015.
Elo IT, Martikainen P, Aaltonen M. Children’s educational attainment, occupation, and income and their parents’ mortality. Popul Stud. 2018;72(1):53–73. https://doi.org/10.1080/00324728.2017.1367413.
World Health Organization. A conceptual framework for action on the social determinants of health. Discussion paper. WHO Document Production Services, Geneva; 2010.
Braveman P, Gottlieb L. The social determinants of health: it’s time to consider the causes of the causes. Public Health Rep. 2014;129(Suppl 2):19–31. https://doi.org/10.1177/00333549141291S206.
Donkin A, Goldblatt P, Allen J, Nathanson V, Marmot M. Global action on the social determinants of health. BMJ Glob Health. 2018. https://doi.org/10.1136/bmjgh-2017-000603.
Marmot M. Social determinants, capabilities and health inequalities: a response to Bhugra, Greco, Fennell and Venkatapuram. J Hum Dev Capabilities. 2018;19(4):575–7 . https://doi.org/10.1080/19452829.2018.1522044.
Andersen R. A behavioral model of families’ use of health services. Chicago: Center for Health Administration Studies, University of Chicago; 1968.
Gelberg L, Andersen RM, Leake BD. The behavioral model for vulnerable populations: application to medical care use and outcomes for homeless people. Health Serv Res. 2000;34(6):1273–302.
Davidson PL, Andersen RM, Wyn R, Brown ER. A framework for evaluating safety-net and other community-level factors on access for low-income populations. Inquiry. 2004;41(1):21–38. https://doi.org/10.5034/inquiryjrnl_41.1.21.
Ryvicker M. A conceptual framework for examining healthcare access and navigation: a behavioral-ecological perspective. Soc Theory Health. 2018;16(3):224–40. https://doi.org/10.1057/s41285-017-0053-2.
Peterson B, Harrell F. Partial proportional odds models for ordinal response variables. J R Stat Soc Ser C Appl Stat. 1990;39(2):205–17. https://doi.org/10.2307/2347760.
Williams R. Generalized ordered logit/partial proportional odds models for ordinal dependent variables. Stata J Promot Commun Stat Stata. 2006;6:58–82. https://doi.org/10.1177/1536867X0600600104.
Brant R. Assessing proportionality in the proportional odds model for ordinal logistic regression. Biometrics. 1990;46(4):1171–8.
Bamfo BA, Dogbe CSK. Factors influencing the choice of private and public hospitals: empirical evidence from Ghana. Int J Pharm Healthc Market. 2017;15(1):290. https://doi.org/10.1108/IJPHM-11-2015-0054.
Swain S. Do patients really perceive better quality of service in private hospitals than public hospitals in India? Benchmark Int J. 2019;26(2):590–613. https://doi.org/10.1108/BIJ-03-2018-0055.
Kwateng KO, Lumor R, Acheampong FO. Service quality in public and private hospitals: a comparative study on patient satisfaction. Int J Healthc Manag. 2019;12(4):251–8. https://doi.org/10.1080/20479700.2017.1390183.
Singh P. Comparison of service quality between private and public hospitals: empirical evidences from Varanasi District in up. Paradigm. 2013;17:37–46 . https://doi.org/10.1177/0971890720130105.
Kumar S. Private sector in healthcare delivery market in India: structure growth and implications. Inst Stud Ind Dev Work Paper. 2015;185:14–5.
Zeng Y, Brasher MS, Gu D, Vaupel JW. Older parents benefit more in health outcome from daughters’ than sons’ emotional care in China. J Aging Health. 2016;28(8):1426–47. https://doi.org/10.1177/0898264315620591.
Dwyer J, Coward RT. A multivariate comparison of the involvement of adult sons versus daughters in the care of impaired parents. J Gerontol. 1991;46(5):259–69. https://doi.org/10.1093/geronj/46.5.S259.
HelpAge India. Elderly abuse in India: role of family in caregiving. 2019. https://www.helpageindia.org/wp-content/uploads/2019/08/Newsletters-Apr.-2019-Jun.-2019.pdf.
Acknowledgements
The authors are thankful to the National Sample Survey Organization for providing the data for analysis.
Author information
Authors and Affiliations
Contributions
1. Conceptualization and design: SV and MA
2. Data acquisition and analysis: MA
3. Data interpretation: MA
4. Drafting of the manuscript: MA
5. Critical revisions to manuscript: WJ and SV
6. Overall supervision: SV and WJ
Corresponding author
Ethics declarations
The authors report no ethical issues.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Ambade, M., Joe, W. & Subramanian, S.V. Children’s education and level of health care utilization among parents: a pooled cross-sectional study from national population-based survey in India. GeroScience 43, 2497–2514 (2021). https://doi.org/10.1007/s11357-021-00415-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11357-021-00415-0