Abstract
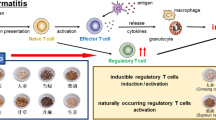
Orengedokuto (OGT) is a Kampo prescription that has been used for the treatment of inflammation, hypertension, gastrointestinal disorders, and liver and cerebrovascular diseases. It is also used for the treatment of skin diseases such as urticaria and atopic dermatitis. We previously studied its anti-allergic effects of OGT on the murine model of 2,4,6-trinitrochlorobenzene (TNCB)-induced contact hypersensitivity (CHS) and demonstrated that it significantly suppresses ear swelling in a dose-dependent manner. However, the mechanism underlying this activity remained unknown. Here, we sought to identify the mechanism involved. Using a murine model of TNCB-induced CHS, together with adoptive cell transfer experiments, we found that the anti-allergic effects of OGT may be due to the inhibition of effector T cell activation and not the induction and/or activation of regulatory T cells. Flow cytometry analysis revealed that oral administration of OGT suppressed the increase in CD8+CD44highCD62L+ cell number in draining lymph nodes (dLNs) of mice sensitized with 5% TNCB. Additionally, ex vivo experiments confirmed the suppressive effect of OGT on the activation of effector T cells, as interferon-γ (IFN-γ) production by cultured lymphocytes obtained from 5% TNCB-sensitized mice and stimulated with anti-CD3ε and anti-CD28 monoclonal antibodies was reduced by OGT administration. In conclusion, our finding suggests that OGT exerts anti-allergic effects by regulating the activation of effector T cells involved in inflammatory skin diseases such as atopic dermatitis.





Similar content being viewed by others
References
Hanifin JM, Rajika G (1980) Diagnostic features of atopic dermatitis. Acta Derm Venerol (Stockholm) Suppl 92:44 – 47
Cooper KD (1994) J Invest Dermatol 102:128–137
Kabashima K (2013) New concept of the pathogenesis of atopic dermatitis: interplay among the barrier, allergy, and pruritus as a trinity. J Dermatol Sci 70:3–11
Seegraber M, Srour J, Walter A, Knop M, Wollenberg A (2018) Dupilumab for treatment of atopic dermatitis. Expert Rev Clin Phramacoll 11, https://doi.org/10.1080/17512433.2018.1449462
Woo TE, Kuzel P (2019) Crisaborole 2% ointment (Eucrisa) for atopic dermatitis. Skin Therapy Lett 24:4–6
Nakagawa H, Nemoto O, Igarashi A, Saeki H, Kaino H Nagata T (2020) Delgocitinib ointment, a topical Janus kinase inhibitor, in adult patients with moderate to severe atopic dermatitis: A phase 3, randomized, double-blind, vehicle-controlled study and an open-label, long-term extension study. J Am Acad Dermatol 82:823–831
The ministry of Health, Labour and Welfare of Japan (2016) The Japanese pharmacopeia. The Ministry of Health, Labour and Welfare of Japan, Tokyo, pp 1752 – 1754
Li Y, Xie J, Li Y, Yang Y, Yang L (2019) Literature data-based systems pharmacology uncovers the essence of “body fire” in traditional Chinese medicine: a case by Huang–Lian–Jie–Du–Tang. J Ethnopharmacol 237:266–285
Nose M, Sakushima J, Harada D, Ogihara Y (1999) Comparison of immunopharmacological actions of 8 kinds of Kampo-hozais clinically used in atopic dermatitis on delayed-type hypersensitivity in mice. Biol Pharm Bull 22:48–54
Gao XK, Fuseda K, Shibata T, Tanaka H, Inagaki N, Nagai H (2005) Kampo medicines for mite antigen-induced allergic dermatitis in NC/Nga mice. Evid Based Complement Alternat Med 2:191–199
Nair AB, Jacob S (2016) A simple practice guide for dose conversion between animals and human. J Basic Clin Pharm 7:27–31
Camp RL, Scheyninus A, Johansson C, Pure E (1993) CD44 is necessary for optimal contact allergic responses but is not required for normal leukocyte extravasation. J Exp Med 178:497–507
Gonda A, Gal I, Szanto S, Sarraj B, Glant TT, Hunyadi J Mikecz K (2005) CD44, but not L-selectin, is critically involved in leukocyte migration into the skin in a murine model of allergic dermatitis. Exp Dermatol 14: 700–708
Nakashima D, Kabashima K, Sakabe J, Sugita K, Kobayashi T, Yoshiki R, Tokuda Y (2008) Impaired initiation of contact hypersensitivity by FT720. J Invest Dermatol 128:2833–2841
Salluso F, Lenig D, Forster R, Lipp M, Lanzavecchia A (1999) Two subsets of memory T lymphocytes with distinct homing potentials and effector functions. Nature 401:708–712
Wherry EJ, Teichgraber V, Becker TC, Masopust D, Kaech SM Antia R, Andrian UH, Ahmed R (2003) Lineage relationship and protective immunity of memory CD8 T cell subsets. Nat Immunol 4: 225–234
Takeda K, Gelfannd EW (2009) Mouse models of allergic diseases. Cur Opinion Immunol 21:660–665
Martel BC, Lovato P, Baümer W, Olivry, (2017) Translational animal model of atopic dermatitis for preclinical studies. Yale J Biol Med 90:389–402
Kim D, Kobayashi T, Nagao K (2019) Research techniques made simple: mouse models of atopic dermatitis. J Invest Dermatol 139:984–990
Vocanson M, Hennino A, Rozieres A, Poyet G, Nicolas JF (2009) Effector and regulatory mechanisms in allergic contact dermatitis. Allergy 64:1699–1714
Bouloc A, Cavani A, Katz SI (1998) Contact hypersensitivity in MHC class II-deficient mice depends on CD8 T lymphocytes primed by immunostimulating Langerhans cells. J Invest Dermatol 111:44–49
Wang B, Fujisawa H, Zhuang L, Freed I, Howell BG, Shiahid S, Shivji GM, Mak TW, Sauder DN (2000) CD4+ Th1 and CD8+ Type 1 cytosolic T cells both play a crucial role in the full development of contact hypersensitivity. J Immunol 165:6783–6790
Okazaki F, Kanzaki H, Fujii K, Arata J, Akiba H, Tsuji K, Iwatsuki K (2002) Initial recruitment of interferon-γ-producing CD8+ effector cells, followed by infiltration of CD4+ cells in 2, 4, 6-trinotro-1-chrolobenzene (TNCB)-induced murine contact hypersensitivity. J Dermatol 29:699–708
Christensen AD, Haase C (2011) Immunological mechanisms of contact hypersensitivity in mice. APMS 120:1–27
Chen Y, Xian YF, Loo S, Lai Z, Chan WY, Liu L, Lin ZX (2020) Huang-Lian-Jie-Du extract ameliorates atopic dermatitis-like skin lesions induced by 2,4-nitirobenzen in mice via suppression of MAPKs and NF-κB pathways. J Ethnopharmacol 249:112367
Chen Y, Xian Y, Lai Z, Loo S, Chain WY, Lin ZX (2016) Anti-inflammatory and anti-allergic effects of Huang–Lian–Jie–Du extract: implication for atopic dermatitis treatment. J Ethnopharmacol 185:41–52
Zeng H, Dou S, Zhao J, Fan S, Yuan X, Zhu S, Li L, Zhong W, Liu R (2011) The inhibitory activities of the components of Huang–Lian–Jie–Du–Tang (HLJIDT) on eicosanoid generation via lipoxygenase pathway. J Ethnopharmacol 135:561–568
Oshima N, Narukawa Y, Hada N, Kiuchi F (2013) Quantitative analysis of anti-inflammatory activity of orengedokuto: importance of combination of flavonoids in inhibition of PGE2 production in mouse macrophage-like cell line J774.1. J Nat Med 67:281–288
Oshima N, Shimizu T, Narukawa Y, Hada N, Kiuchi F (2018) Quantitative analysis of the anti-inflammatory activity of orengedokuto II: berberine is responsible for the inhibition of NO production. J Nat Med 72:706–714
Chi YS, Cheon BS, Kim HP (2001) Effect of wogonin, a plant flavone from Scutellariae Radix, on the suppression of cyclooxygenase-2 and the induction of inducible nitric oxide synthase in lipopolysaccharide-treated RAW264.7 cells. Biochem Pharmacol 61:1195–1203
Yoon SB, Lee YJ, Park SK, Kim HC, Bae H, Kim HM, Ko SG, Choi HY, Oh MS, Park W (2009) Anti-inflammatory effects of Scutellariae baicalensis water extract on LPS-activated RAW264.7 macrophages. J Ethnopharmacol 125:286–290
Akiyama H, Nose M, Takiguchi H, Sugiyama K, Tsutsui R, Hisaka S, Fuchino H, Inui T, Kawano N, Taguchi T, Kudo T, Kawahara N, Yoshimatsu K (2019) Mutagenetic and anti-allergic studies for evaluation of extracts of Coptis Rhizome produced by an artificial hydroponic system. J Nat Med 73:608–613
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tsuge, A., Watanabe, A., Kodama, Y. et al. Orengedokuto exerts anti-allergic effects via inhibition of effector T cell activation in a murine model of contact hypersensitivity. J Nat Med 76, 144–151 (2022). https://doi.org/10.1007/s11418-021-01566-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11418-021-01566-2