Abstract
Purpose
Ki-67 heterogeneity can impact on gastroenteropancreatic neuroendocrine tumor grade assignment, especially when tissue is scarce. This work is aimed at devising adequacy criteria for grade assessment in biopsy specimens.
Method
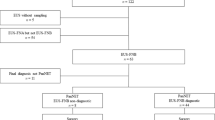
To analyze the impact of biopsy size on reliability, 360 virtual biopsies of different thickness and lengths were constructed. Furthermore, to estimate the mean amount of non-neoplastic tissue component present in biopsies, 28 real biopsies were collected, the non-neoplastic components (fibrosis and inflammation) quantified and the effective area of neoplastic tissue calculated for each biopsy.
Results
Heterogeneity of Ki-67 distribution, G2 tumors and biopsy size all play an important role in reducing the reliability of biopsy samples in Ki-67-based grade assignment. In particular in G2 cases, 59.9% of virtual biopsies downgraded the tumor and the smaller the biopsy, the more frequent downgrading occurs. In real biopsies the presence of non-neoplastic tissue reduced the available total area by a mean of 20%.
Conclusions
By coupling the results from these two different approaches we show that both biopsy size and non-neoplastic component must be taken into account for biopsy adequacy. In particular, we can speculate that if the minimum biopsy area, necessary to confidently (80% concordance) grade gastro-entero-pancreatic neuroendocrine tumors on virtual biopsies ranges between 15 and 30 mm2, and if real biopsies are on average composed of only 80% of neoplastic tissue, then biopsies with a surface area not <12 mm2 should be performed; using 18G needles, this corresponds to a minimum total length of 15 mm.

Similar content being viewed by others
Change history
19 August 2017
An erratum to this article has been published.
References
I.M. Modlin, K. Oberg, D.C. Chung, R.T. Jensen, W.W. de Herder, R.V. Thakker, M. Caplin, G. Delle Fave, G.A. Kaltsas, E.P. Krenning, S.F. Moss, O. Nilsson, G. Rindi, R. Salazar, P. Ruszniewski, A. Sundin, Gastroenteropancreatic neuroendocrine tumors. Lancet. Oncol. 9, 61–72 (2008)
G. Rindi, G. Klöeppel, H. Alhman, M. Caplin, A. Couvelard, W.W. de Herder, B. Eriksson, A. Falchetti, M. Falconi, P. Komminoth, M. Koerner, J.M. Lopes, A.M. McNicol, O. Nilsson, A. Perren, A. Scarpa, J.Y. Scoazec, B. Wiedenmann, all other Frascati Consensus Conference participants; European Neuroendocrine Tumor Society (ENETS), TNM staging of foregut (neuro)endocrine tumors: a consensus proposal including a grading system. Virchows. Arch. 449, 395–401 (2006)
G. Rindi, G. Klöppel, A. Couvelard, P. Komminoth, M. Koerner, J. M. Lopes, A. M. McNicol, O. Nilsson, A. Perren, A. Scarpa, J.Y. Scoazec, B. Wiedenmann, TNM staging of midgut and hindgut (neuro) endocrine tumors: a consensus proposal including a grading system. Virchows. Arch. 451, 757–762 (2007)
A. Perren, A. Couvelard, J.Y. Scoazec, F. Costa, I. Borbath, G. Delle Fave, V. Gorbounova, D. Gross, A. Grossma, R.T. Jense, M. Kulke, K. Oeberg, G. Rindi, H. Sorbye, S. Welin all other Antibes Consensus Conference participants ENETS consensus guidelines for the standards of care in neuroendocrine tumors: pathology: diagnosis and prognostic stratification. Neuroendocrinology (2017). doi:10.1159/000457956. [Epub ahead of print]
G. Rindi, R. Arnold, F.T. Bosman, C. Capella, D.S. Klimstra, G. Klöppel, P. Komminoth, E. Solcia, in Nomemclature and classification of neuroendocrine neoplasms of the digestive system. WHO Classification of Tumors of the Digestive System. eds. by F .T. Bosman, F. Carneiro, R. H. Hruban, N. D. Theise (IARC Press, Lyon, 2010), p. 13–14
C.M. McCall, C. Shi, T.C. Cornish, D.S. Klimstra, L.H. Tang, O. Basturk, L.J. Mun, T.A. Ellison, C.L. Wolfgang, M.A. Choti, R.D. Schulick, B.H. Edil, R.H. Hruban, Grading of well-differentiated pancreatic neuroendocrine tumors is improved by the inclusion of both Ki67 proliferative index and mitotic rate. Am. J. Surg. Pathol. 37, 1671–1677 (2013)
K. Öberg, U. Knigge, D. Kwekkeboom, A. Perren; on behalf of ESMO Guidelines Working Group, Neuroendocrine gastro-entero-pancreatic tumors: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann. Oncol. 23, vii124–vii130 (2012)
D.S. Klimstra, Reassessing the grade of gastroenteropancreatic neuroendocrine neoplasms. Endocrine 53, 4–6 (2016)
M. Milione, Prognostic factors for gastroenteropancreatic neuroendocrine neoplasms (GEP-NENs): what’s better? Endocrine (2017). doi:10.1007/s12020-017-1299-0. [Epub ahead of print]
A. Couvelard, L. Deschamps, P. Ravaud, G. Baron, A. Sauvanet, O. Hentic, N. Colnot, V. Paradis, J. Belghiti, P. Bedossa, P. Ruszniewski, Heterogeneity of tumor prognostic markers: a reproducibility study applied to liver metastases of pancreatic endocrine tumors. Mod. Pathol. 22, 273–281 (2009)
Z. Yang, L.H. Tang, D.S. Klimstra, Effect of tumor heterogeneity on the assessment of Ki67 labeling index in well-differentiated neuroendocrine tumors metastatic to the liver: implications for prognostic stratification. Am. J. Surg. Pathol. 35, 853–860 (2011)
A. Larghi, G. Capurso, A. Carnuccio, R. Ricci, S. Alfieri, D. Galasso, F. Lugli, A. Bianchi, F. Panzuto, L. De Marinis, M. Falconi, G. Delle Fave, G.B. Doglietto, G. Costamagna, G. Rindi, Ki-67 grading of nonfunctioning pancreatic neuroendocrine tumours on histologic samples obtained by EUS-guided fine-needle tissue acquisition: a prospective study. Gastrointest. Endosc. 76, 570–577 (2012)
V. Rebours, J. Cordova, A. Couvelard, M. Fabre, L. Palazzo, M.P. Vullierme, O. Hentic, A. Sauvanet, A. Aubert, P. Bedossa, P. Ruszniewski, Can pancreatic neuroendocrine tumour biopsy accurately determine pathological characteristics? Dig. Liver. Dis. 47, 973–977 (2015)
F. Grillo, M. Albertelli, M.P. Brisigotti, T. Borra, M. Boschetti, R. Fiocca, D. Ferone, L. Mastracci, Grade increases in gastroenteropancreatic neuroendocrine tumor metastases compared to the primary tumor. Neuroendocrinology. 103, 452–459 (2015)
F. Grillo, S. Pigozzi, P. Ceriolo, P. Calamaro, R. Fiocca, L. Mastracci, Factors affecting immunoreactivity in long-term storage of formalin-fixed paraffin-embedded tissue sections. Histochem. Cell. Biol. 144, 93–99 (2015)
A. Gambella, L. Porro, S. Pigozzi, R. Fiocca, F. Grillo, L. Mastracci, Section detachment in immunohistochemistry: causes, troubleshooting, and problem-solving. Cell. Biol. 148, 95–101 (2017)
M.D. Reid, P. Bagci, N. Ohike, B. Saka, I. Erbarut Seven, N. Dursun, S. Balci, H. Gucer, K.T. Jang, T. Tajiri, O. Basturk, S.Y. Kong, M. Goodman, G. Akkas, V. Adsay, Calculation of the Ki67 index in pancreatic neuroendocrine tumors: a comparative analysis of four counting methodologies. Mod. Pathol. 28, 686–694 (2015)
F. Grillo, M. Albertelli, F. Annunziata, M. Boschetti, A. Caff, S. Pigozzi, D. Ferone, L. Mastracci, Twenty years of gastroenteropancreatic neuroendocrine tumors: is reclassification worthwhile and feasible? Endocrine 53, 58–62 (2016)
S.M. Remes, V.J. Tuominen, H. Helin, J. Isola, J. Arola, Grading of neuroendocrine tumors with Ki-67 requires high-quality assessment practices. Am. J. Surg. Pathol. 36, 1359–1363 (2012)
B. Weynand, I. Borbath, V. Bernard, C. Sempoux, J.F. Gigot, C. Hubert, V. Lannoy, P.H. Deprez, A. Jouret-Mourin, Pancreatic neuroendocrine tumour grading on endoscopic ultrasound-guided fine needle aspiration: high reproducibility and inter-observer agreement of the Ki-67 labelling index. Cytopathology 25, 389–395 (2014)
L.H. Tang, M. Gonen, C. Hedvat, I.M. Modlin, D.S. Klimstra, Objective quantification of the Ki67 proliferative index in neuroendocrine tumors of the gastroenteropancreatic system: a comparison of digital image analysis with manual methods. Am. J. Surg. Pathol. 36, 1761–1770 (2012)
T. Hasegawa, K. Yamao, S. Hijioka, V. Bhatia, N. Mizuno, K. Hara, H. Imaoka, Y. Niwa, M. Tajika, S. Kondo, T. Tanaka, Y. Shimizu, T. Kinoshita, T. Kohsaki, I. Nishimori, S. Iwasaki, T. Saibara, W. Hosoda, Y. Yatabe, Evaluation of Ki-67 index in EUS-FNA specimens for the assessment of malignancy risk in pancreatic neuroendocrine tumors. Endoscopy 46, 32–38 (2014)
D.L. Aslan, H.E. Gulbahce, S.E. Pambuccian, J.C. Manivel, J. Jessurun, Ki-67 immunoreactivity in the differential diagnosis of pulmonary neuroendocrine neoplasms in specimens with extensive crush artifact. Am. J. Clin. Pathol. 123, 874–878 (2005)
Acknowledgements
We thank Miss Simona Pigozzi for technical support in immunohistochemistry.
Funding
This research did not receive any specific grant from any funding agency in the public, commercial or not-for-profit sector
Author contributions
Dr. Grillo devised the work, performed the Ki-67 counting and wrote the manuscript. Dr. Valle performed the Ki-67 counting and wrote the manuscript. Prof. Ferone, Dr. Albertelli, and Dr. Cittadini aided in devising the study. Dr. Brisigotti collected samples and performed Ki-67 counting. Prof. Fiocca and Dr. Vanoli critically reviewed the work and manuscript. Dr. Mastracci wrote and critically reviewed the work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
The original version of this article was revised: the first and surname of all the authors are corrected.
Federica Grillo and Luca Valle contributed equally to this work.
An erratum to this article is available at https://doi.org/10.1007/s12020-017-1389-z.
Rights and permissions
About this article
Cite this article
Grillo, F., Valle, L., Ferone, D. et al. KI-67 heterogeneity in well differentiated gastro-entero-pancreatic neuroendocrine tumors: when is biopsy reliable for grade assessment?. Endocrine 57, 494–502 (2017). https://doi.org/10.1007/s12020-017-1364-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-017-1364-8