Abstract
Background
Recent studies have identified an increased risk of hepatocellular carcinoma (HCC) in autoimmune hepatitis (AIH). Sex and regional disparities in incidence of HCC in AIH continue to be reported worldwide. Nevertheless, the magnitude of this gap remains unknown.
Method
We searched several databases including PubMed, Embase, Web of Science, Cochrane Library, Wanfang Data, CNKI and SinoMed. Incidence rates of HCC in AIH were combined and analyzed following the EBayes method. Incidence rate ratios were pooled to assess the sex differences. The impact of population difference, sex, age, cirrhotic condition was further analyzed with subgroup analysis and linear regression analysis.
Result
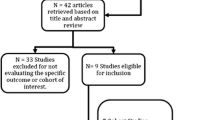
39 studies meeting our eligibility criteria were chosen for the analysis. The pooled incidence rate of HCC in AIH was 3.54 per 1000 person years (95% CI 2.76–4.55). Pooled IRR for the risk of HCC in male AIH patients compared to female was 2.16 (95% CI 1.25–3.75), with mild heterogeneity among studies. The pooled HCC incidence rate in AIH by continents was as follows: Europe 2.37 per 1000 person-years (95% CI 1.45–3.88), Asia 6.18 per 1000 person-years (95%CI 5.51–6.93), North America 2.97 per 1000 person-years (95%CI 2.40–3.68), Oceania 2.60 (95%CI 0.54–7.58). The pooled HCC incidence rate in AIH-related cirrhosis by continent was as follows: Europe 6.35 per 1000 person-years (95%CI 3.94–10.22), Asia 17.02 per 1000 person-years (95%CI 11.18–25.91), North America 10.89 per 1000 person-years (95%CI 6.69–17.74).
Conclusion
A higher HCC incidence in AIH was observed among male and in Asian populations. Cirrhosis status at AIH diagnosis is significantly associated with an increased incidence rate for HCC, and routine HCC surveillance is recommended for patients with AIH cirrhosis, especially for those in Asia.



Similar content being viewed by others
Data transparency
The manuscript's guarantors (L.-J.Y. and T.L.) affirm that the manuscript shows an honest, accurate, and transparent study; that no important aspects of the study have been omitted and that any discrepancies from the study have been explained.v
Abbreviations
- HCC:
-
Hepatocellular carcinoma
- HBV:
-
Hepatitis B virus
- HCV:
-
Hepatitis C virus
- AIH:
-
Autoimmune hepatitis
- SIR:
-
Standardized incidence rate
- SMR:
-
Standardized mortality rate
- NOS:
-
Newcastle–Ottawa scale
- CI:
-
Confidential interval
- IRR:
-
Incidence rate ratio
References
Latest global cancer data: Cancer burden rises to 19.3 million new cases and 10.0 million cancer deaths in 2020. https://www.iarc.fr/fr/news-events/latest-global-cancer-data-cancer-burden-rises-to-19-3-million-new-cases-and-10-0-million-cancer-deaths-in-2020/.
Liu KX, Hong JG, Wu R, et al. Clinical Benefit of Antiviral Agents for Hepatocellular Carcinoma Patients With Low Preoperative HBV-DNA Loads Undergoing Curative Resection: A Meta-Analysis. Front Oncol. 2021; 11:605648.
Yang JD, Ahmed F, Mara KC, et al. Diabetes Is Associated With Increased Risk of Hepatocellular Carcinoma in Patients With Cirrhosis From Nonalcoholic Fatty Liver Disease. Hepatology. 2020;71(3):907–16.
Zachou K, Muratori P, Koukoulis GK, et al. Review article: autoimmune hepatitis - current management and challenges. Aliment Pharmacol Ther. 2013;38(8):887–913.
Lv T, Li M, Zeng N, et al. Systematic review and meta-analysis on the incidence and prevalence of autoimmune hepatitis in Asian, European, and American population. J Gastroenterol Hepatol. 2019;34(10):1676–84.
Puustinen L, Barner-Rasmussen N, Pukkala E, Färkkilä M. Incidence, prevalence, and causes of death of patients with autoimmune hepatitis: A nationwide register-based cohort study in Finland. Dig Liver Dis. 2019;51(9):1294–9.
Arinaga-Hino T, Ide T, Miyajima I, et al. Risk of malignancies in autoimmune hepatitis type 1 patients with a long-term follow-up in Japan. Hepatol Res. 2018;48(3):E222–31.
Danielsson Borssén Å, Marschall HU, Bergquist A, et al. Epidemiology and causes of death in a Swedish cohort of patients with autoimmune hepatitis. Scand J Gastroenterol. 2017;52(9):1022–8.
Castro FA, Liu X, Forsti A, et al. Increased risk of hepatobiliary cancers after hospitalization for autoimmune disease. Clin Gastroenterol Hepatol. 2014;12(6):1038-1045.e1037.
Ngu JH, Gearry RB, Frampton CM, Stedman CAM. Mortality and the risk of malignancy in autoimmune liver diseases: A population-based study in Canterbury. New Zealand Hepatology. 2012;55(2):522–9.
Werner M, Almer S, Prytz H, et al. Hepatic and extrahepatic malignancies in autoimmune hepatitis. A long-term follow-up in 473 Swedish patients. Journal of Hepatology. 2009;50(2):388–393.
Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol. 2009;62(10):e1-34.
Macaron C, Hanouneh IA, Zein NN. Incidence and risk factors of hepatocellular carcinoma in patients with primary biliary cirrhosis. Hepatology. 2010;52(6):2240–2240.
El-Serag HB, Rudolph KL. Hepatocellular carcinoma: epidemiology and molecular carcinogenesis. Gastroenterology. 2007;132(7):2557–76.
Ioannou GN, Splan MF, Weiss NS, McDonald GB, Beretta L, Lee SP. Incidence and predictors of hepatocellular carcinoma in patients with cirrhosis. Clin Gastroenterol Hepatol. 2007;5(8):938–945, 945.e931–934.
Velázquez RF, Rodríguez M, Navascués CA, et al. Prospective analysis of risk factors for hepatocellular carcinoma in patients with liver cirrhosis. Hepatology. 2003;37(3):520–7.
Tansel A, Katz LH, El-Serag HB, et al. Incidence and Determinants of Hepatocellular Carcinoma in Autoimmune Hepatitis: A Systematic Review and Meta-analysis. Clin Gastroenterol Hepatol. 2017;15(8):1207-1217.e1204.
Parikh ND, Singal AG, Hutton DW, Tapper EB. Cost-Effectiveness of Hepatocellular Carcinoma Surveillance: An Assessment of Benefits and Harms. Am J Gastroenterol. 2020;115(10):1642–9.
Funding
This work was supported by the grants from the Taishan Scholars Program for Young Expert of Shandong Province (Grant No. tsqn20161064), National Natural Science Foundation of China (Grant Nos. 82073200 & 81874178), and founds for Independent Cultivation of Innovative Team from Universities in Jinan (Grant No.2020GXRC023).
Author information
Authors and Affiliations
Contributions
All authors had full access to the data in the study and take responsibility for the integrity and authenticity of the data. L-JY formulated the study objective, conceptualized the study, performed the statistical analysis, and interpreted the results; K-XL and G-XM designed the protocol of the systematic reviews; Z-RD, J-GH, Z-QC provided important guidance to the protocols and modified them; L-JY and S-YY assessed the availability of each study retrieved from online databases respectively and disagreements were identified and discussed with K-XL; H-CL, and Z-ND performed the methodology, data collection, and data validation; L-JY guided the task of formal statistical analysis and analysis of the data; L-JY and TL contributed to outlining the manuscript and drafting the manuscript; L-JY and TL verified the underlying data. TL supervised and coordinated the study. All authors have read and approved the final version.
Corresponding author
Ethics declarations
Conflicts of Interest
Lun-Jie Yan, Sheng-Yu Yao, Guang-Xiao Meng, Kai-Xuan Liu, Hai-Chao Li, Zi-Niu Ding, Zhao-Ru Dong, Jian-Guo Hong, Zhi-Qiang Chen and Tao Li declare no conflict of interests for this article.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.




Rights and permissions
About this article
Cite this article
Yan, LJ., Yao, SY., Meng, GX. et al. Sex and regional disparities in incidence of hepatocellular carcinoma in autoimmune hepatitis: a systematic review and meta-analysis. Hepatol Int 15, 1413–1420 (2021). https://doi.org/10.1007/s12072-021-10249-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12072-021-10249-9