Abstract
Objective
Studies suggest protein intake may be associated with lower body weight, but protein has also been associated with preservation of lean body mass. Understanding the role of protein in maintaining health for older adults is important for disease prevention among this population.
Design
Cross-sectional study of the relationship of dietary protein on body composition.
Setting
New York City community centers.
Participants
1,011 Black, White, and Latino urban men and women 60-99 years of age.
Measurements
Protein intake was assessed using two interviewer-administered 24-hour recalls, and body composition was assessed using bioelectrical impedance analysis (BIA) of fat mass (kg) (FM), fat free mass (kg) (FFM), and impedance resistance (Ohms).
Statistical Analysis
Indices of FM and FFM were calculated by dividing BIA measurements by height squared (m2), and percent FFM was calculated by dividing FFM by the sum of FM and FFM. Log linear models adjusting for age (continuous), race/ethnicity, education, physical activity (dichotomized at the median), hypertension, diabetes, and total calories (continuous).
Results
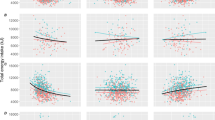
Just 33% of women and 50% of men reported meeting the RDA for protein. Both fat free mass index (FFMI) and fat mass index (FMI) were negatively associated with meeting the RDA for protein (Women: FFMI -1.78 95%CI [-2.24, -1.33], FMI -4.12 95% CI [-4.82, -3.42]; Men: FFMI -1.62 95% CI [-2.32, -0.93] FMI -1.80 95% CI [-2.70, -0.89]). After accounting for confounders, women and men consuming at least 0.8 g/kg/day had a 6.2% (95% CI: 5.0%, 7.4%) and a 3.2% (95% CI 1.1%, 5.3%) higher percent fat free mass, respectively.
Conclusions
FFM, FFMI, FM, and FMI were inversely related to meeting the RDA for protein. Meeting the RDA for protein of at least 0.8g/kg/day was associated with a higher percentage of fat free mass among older adults. These results suggest meeting the protein recommendations of at least 0.8 g/kg/day may help to promote lower overall body mass, primarily through loss of fat mass rather than lean mass.




Similar content being viewed by others
References
Phillips SM, Fulgoni VL, 3rd, Heaney RP, Nicklas TA, Slavin JL, Weaver CM. Commonly consumed protein foods contribute to nutrient intake, diet quality, and nutrient adequacy. Am. J. Clin. Nutr. 2015.
Fulgoni VL, 3rd. Current protein intake in America: analysis of the National Health and Nutrition Examination Survey, 2003-2004. Am. J. Clin. Nutr. 2008;87(5):1554S–1557S.
Pasiakos SM, Lieberman HR, Fulgoni VL. Higher-Protein Diets Are Associated with Higher HDL Cholesterol and Lower BMI and Waist Circumference in US Adults. J. Nutr. 2015;145(3):605–614.
Fukagawa NK. Protein requirements: methodologic controversy amid a call for change. Am. J. Clin. Nutr. 2014;99(4):761–762.
Deutz NE, Bauer JM, Barazzoni R, et al. Protein intake and exercise for optimal muscle function with aging: recommendations from the ESPEN Expert Group. Clin. Nutr. 2014;33(6):929–936.
Volpi E, Campbell WW, Dwyer JT, et al. Is the optimal level of protein intake for older adults greater than the recommended dietary allowance? J. Gerontol. A. Biol. Sci. Med. Sci. 2013;68(6):677–681.
Bauer J, Biolo G, Cederholm T, et al. Evidence-based recommendations for optimal dietary protein intake in older people: a position paper from the PROT-AGE Study Group. Journal of the American Medical Directors Association. 2013;14(8):542–559.
Kim IY, Schutzler S, Schrader A, et al. Quantity of dietary protein intake, but not pattern of intake, affects net protein balance primarily through differences in protein synthesis in older adults. American journal of physiology. Endocrinology and metabolism. 2015;308(1):E21–28.
Layman DK, Anthony TG, Rasmussen BB, et al. Defining meal requirements for protein to optimize metabolic roles of amino acids. Am. J. Clin. Nutr. 2015.
Rodriguez NR. Introduction to Protein Summit 2.0: continued exploration of the impact of high-quality protein on optimal health. Am. J. Clin. Nutr. 2015.
Franssen FM, Rutten EP, Groenen MT, Vanfleteren LE, Wouters EF, Spruit MA. New reference values for body composition by bioelectrical impedance analysis in the general population: results from the UK Biobank. Journal of the American Medical Directors Association. 2014;15(6):448 e441-446.
Bosy-Westphal A, Muller MJ. Identification of skeletal muscle mass depletion across age and BMI groups in health and disease—there is need for a unified definition. Int J Obes (Lond). 2015;39(3):379–386.
Heymsfield SB, Heo M, Thomas D, Pietrobelli A. Scaling of body composition to height: relevance to height-normalized indexes. Am. J. Clin. Nutr. 2011;93(4):736–740.
VanItallie TB, Yang MU, Heymsfield SB, Funk RC, Boileau RA. Height-normalized indices of the body’s fat-free mass and fat mass: potentially useful indicators of nutritional status. Am. J. Clin. Nutr. 1990;52(6):953–959.
Heymsfield SB, Gonzalez MC, Lu J, Jia G, Zheng J. Skeletal muscle mass and quality: evolution of modern measurement concepts in the context of sarcopenia. Proc. Nutr. Soc. 2015:1–12.
Jebb SA, Cole TJ, Doman D, Murgatroyd PR, Prentice AM. Evaluation of the novel Tanita body-fat analyser to measure body composition by comparison with a fourcompartment model. Br. J. Nutr. 2000;83(2):115–122.
Janssen I, Heymsfield SB, Baumgartner RN, Ross R. Estimation of skeletal muscle mass by bioelectrical impedance analysis. J Appl Physiol (1985). 2000;89(2):465–471.
Janssen I, Heymsfield SB, Ross R. Low relative skeletal muscle mass (sarcopenia) in older persons is associated with functional impairment and physical disability. J. Am. Geriatr. Soc. 2002;50(5):889–896.
Stewart AL, Mills KM, King AC, Haskell WL, Gillis D, Ritter PL. CHAMPS physical activity questionnaire for older adults: outcomes for interventions. Med. Sci. Sports Exerc. 2001;33(7):1126–1141.
Evenson KR, Morland KB, Wen F, Scanlin K. Physical activity and sedentary behavior among adults 60 years and older: New York City residents compared with a national sample. Journal of aging and physical activity. 2014;22(4):499–507.
Gregorio L, Brindisi J, Kleppinger A, et al. Adequate dietary protein is associated with better physical performance among post-menopausal women 60-90 years. The journal of nutrition, health & aging. 2014;18(2):155–160.
Wycherley TP, Moran LJ, Clifton PM, Noakes M, Brinkworth GD. Effects of energy-restricted high-protein, low-fat compared with standard-protein, low-fat diets: a meta-analysis of randomized controlled trials. Am. J. Clin. Nutr. 2012;96(6):1281–1298.
Paddon-Jones D, Leidy H. Dietary protein and muscle in older persons. Current opinion in clinical nutrition and metabolic care. 2014;17(1):5–11.
Wolfe RR. The role of dietary protein in optimizing muscle mass, function and health outcomes in older individuals. Br. J. Nutr. 2012;108 Suppl 2:S88–93.
Komar B, Schwingshackl L, Hoffmann G. Effects of leucine-rich protein supplements on anthropometric parameter and muscle strength in the elderly: a systematic review and meta-analysis. The journal of nutrition, health & aging. 2015;19(4):437–446.
Karelis AD, Messier V, Suppere C, Briand P, Rabasa-Lhoret R. Effect of cysteinerich whey protein (immunocal(R)) supplementation in combination with resistance training on muscle strength and lean body mass in non-frail elderly subjects: a randomized, double-blind controlled study. The journal of nutrition, health & aging. 2015;19(5):531–536.
Paddon-Jones D, Campbell WW, Jacques PF, et al. Protein and healthy aging. Am. J. Clin. Nutr. 2015.
Hickson M. Nutritional interventions in sarcopenia: a critical review. Proc. Nutr. Soc. 2015:1–9.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Beasley, J.M., Deierlein, A.L., Morland, K.B. et al. Is meeting the recommended dietary allowance (RDA) for protein related to body composition among older adults?: Results from the Cardiovascular Health of Seniors and Built Environment Study. J Nutr Health Aging 20, 790–796 (2016). https://doi.org/10.1007/s12603-015-0707-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-015-0707-5