Abstract
Background
People living with human immunodeficiency virus are ageing under combination antiretroviral treatments but data on drug exposure in serum and cerebrospinal fluid are limited. Dolutegravir is a widely used second-generation integrase strand transfer inhibitor: conflicting data suggest that neuropsychiatric side effects may present at a higher frequency in patients with higher dolutegravir serum concentrations.
Methods
We performed a retrospective analysis of our therapeutic drug monitoring registry identifying patients receiving once-daily dolutegravir without concomitant interacting drugs and significant clinical conditions. Data were analysed stratifying time after drug dose intake (maximum concentration 0.5–4 and trough concentration 21–27 h). Cerebrospinal fluid samples from patients enrolled in neurological studies and receiving dolutegravir were analysed for dolutegravir cerebrospinal fluid concentrations and cerebrospinal fluid-to-plasma ratios. Serum and cerebrospinal fluid concentrations were measured through validated chromatographic methods.
Results
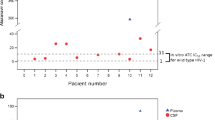
We included 207 (providing 457 serum samples) and 41 patients (providing 41 cerebrospinal fluid samples). Participants were mostly male (68.2–72.8%) of median age of 50 years (50–53 years). Non-significant changes in dolutegravir maximum concentration and trough concentration were observed with age at Spearman’s test (p values > 0.05); linear logistic regression showed a significant effect of age on dolutegravir trough concentration (p = 0.0013) (Fig. 1). Dolutegravir maximum concentration [3830 ng/mL (2311–5057) vs 4230 ng/mL (2919–5272), p = 0.311] and trough concentration [838 ng/mL (362–1587) vs 966 ng/mL (460–2085), p = 0.056] were non-significantly or borderline higher in patients aged > 50 years. Cerebrospinal dolutegravir concentrations were associated with plasma concentrations (ρ = 0.374, p = 0.016) and age (ρ = 0.537, p = 0.003); cerebrospinal fluid dolutegravir concentrations (13.8 vs 7.3 ng/mL, p = 0.015) and cerebrospinal fluid-to-plasma ratios (0.57 vs 0.32%, p = 0.017] were higher in participants aged > 50 years.
Conclusions
We observed an increase in dolutegravir exposure in serum and in cerebrospinal fluid in older patients living with human immunodeficiency virus.


Similar content being viewed by others
References
Kandel CE, Walmsley SL. Dolutegravir: a review of the pharmacology, efficacy, and safety in the treatment of HIV. Drug Des Dev Ther. 2015;9:3547–55.
Bollen P, Reiss P, Schapiro J, et al. Clinical pharmacokinetics and pharmacodynamics of dolutegravir used as a single tablet regimen for the treatment of HIV-1 infection. Expert Opin Drug Saf. 2015;14:1457–72.
Hoffmann C, Welz T, Sabranskiet M, et al. Higher rates of neuropsychiatric adverse events leading to dolutegravir discontinuation in women and older patients. HIV Med. 2017;18:56–63.
Bonfanti P, Madeddu G, Gulminetti R, et al. Discontinuation of treatment and adverse events in an Italian cohort of patients on dolutegravir. AIDS Lond Engl. 2017;31:455–7.
Greenberg L, Ryom L, Wandeleret G, et al. Uptake and discontinuation of integrase inhibitors (INSTIs) in a large cohort setting. J Acquir Immune Defic Syndr. 1999;83:240–50.
Parant F, Miailhes P, Brunel F, et al. Dolutegravir-related neurological adverse events: a case report of successful management with therapeutic drug monitoring. Curr Drug Saf. 2018;13:69–71. https://doi.org/10.2174/1574886313666180116124046.
Yagura H, Watanabe D, Kushidaet H, et al. Impact of UGT1A1 gene polymorphisms on plasma dolutegravir trough concentrations and neuropsychiatric adverse events in Japanese individuals infected with HIV-1. BMC Infect Dis. 2017;17:622.
Borghetti A, Calcagno A, Lombardi F et al. SLC22A2 variants and dolutegravir levels correlate with psychiatric symptoms in persons with HIV. J Antimicrob Chemother. 2019;74:1035–43.
Calcagno A, Nozza S, Mussi C et al. Ageing with HIV: a multidisciplinary review. Infection. 2015;43:509–22.
Winston A, Jose S, Gibbons S, et al. Effects of age on antiretroviral plasma drug concentration in HIV-infected subjects undergoing routine therapeutic drug monitoring. J Antimicrob Chemother. 2013;68:1354–9.
Courle P, Stader F, Guidiet M, et al. Pharmacokinetic profiles of boosted darunavir, dolutegravir and lamivudine in aging people living with HIV. AIDS. 2020;34:103–8.
Simiele M, Ariaudo A, De Nicolò A et al. UPLC-MS/MS method for the simultaneous quantification of three new antiretroviral drugs, dolutegravir, elvitegravir and rilpivirine, and other thirteen antiretroviral agents plus cobicistat and ritonavir boosters in human plasma. J Pharm Biomed Anal. 2017;138:223–30.
Cozzi V, Charbe N, Baldelli S et al. Development and validation of a chromatographic ultraviolet method for the simultaneous quantification of dolutegravir and rilpivirine in human plasma. Ther Drug Monit. 2016;38:407–13.
Zhang J, Hayes S, Sadler BM et al. Population pharmacokinetics of dolutegravir in HIV-infected treatment-naive patients. Br J Clin Pharmacol. 2015;80:502–14.
Barcelo C, Aouri M, Courletet P, et al. Population pharmacokinetics of dolutegravir: influence of drug-drug interactions in a real-life setting. J Antimicrob Chemother. 2019;74:2690–7.
Elliot ER, Wang X, Singh S et al. Increased dolutegravir peak concentrations in people living with human immunodeficiency virus aged 60 and over, and analysis of sleep quality and cognition. Clin Infect Dis. 2019;68:87–95.
Palazzo A, Trunfio M, Pirriatore V et al. Lower dolutegravir plasma concentrations in HIV-positive patients receiving valproic acid. J Antimicrob Chemother. 2018;73:826–7.
Capetti AF, Di Giambenedetto S, Latini A et al. Morning dosing for dolutegravir-related insomnia and sleep disorders. HIV Med. 2018;19:e62–e6363.
Stoquart-ElSankari S, Balédent O, Gondry-Jouet C et al. Aging effects on cerebral blood and cerebrospinal fluid flows. J Cereb Blood Flow Metab. 2007;27:1563–72.
Gelé T, Furlan V, Taburetet AM et al. Dolutegravir cerebrospinal fluid diffusion in HIV-1-infected patients with central nervous system impairment. Open Forum Infect Dis. 2019;6:ofz74.
De Francesco D, Wit FW, Bürkle A et al. Do people living with HIV experience greater age advancement than their HIV-negative counterparts? AIDS. 2019;33:259–68.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was carried out as part of our routine work.
Conflict of interest
Andrea Calcagno has received honoraria from Gilead, Insmed, Janssen-Cilag, MSD and Viiv and he is currently receiving research grants from Gilead and Viiv. Giovanni Di Perri and Stefano Bonora have received honoraria from Abbvie, BMS, Gilead, Janssen-Cilag, MSD and Viiv. José Moltó, Borghetti Alberto, Gervasoni Cristina, Maurizio Milesi, Marta Valle, Valeria Avataneo, Chiara Alcantarini, Francesc Pla-Junca, Trunfio Mattia, Antonio D’Avolio, Simona Di Giambenedetto and Dario Cattaneo have no conflicts of interest that are directly relevant to the content of this article.
Rights and permissions
About this article
Cite this article
Calcagno, A., Moltó, J., Borghetti, A. et al. Older Age is Associated with Higher Dolutegravir Exposure in Plasma and Cerebrospinal Fluid of People Living with HIV. Clin Pharmacokinet 60, 103–109 (2021). https://doi.org/10.1007/s40262-020-00916-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40262-020-00916-9