Abstract
Purpose
General and eating disorder (ED)-specific ruminations have been identified as key factors that may contribute to eating pathology. Positive beliefs about rumination (e.g., “Ruminating helps me to prevent future mistakes") may impact this association. However, the effect of positive beliefs about rumination on the links between rumination and ED symptom severity has not been investigated. This study sought to clarify relations between rumination and ED symptom severity and to evaluate the potential moderating effect of positive beliefs about rumination on these associations.
Methods
During a laboratory visit, undergraduate participants (N = 473, MAge = 18.90 ± 2.27, MBMI = 23.45 kg/m2 ± 4.31, 54.8% female) completed an online battery of questionnaires assessing general and ED-specific ruminative processes (e.g., brooding, reflection), positive beliefs about rumination, and global ED symptoms. Hierarchical multiple regression analyses assessed the unique contributions of specific ruminative processes, and the moderating effect of positive beliefs on associations between ruminative processes and ED symptom severity.
Results
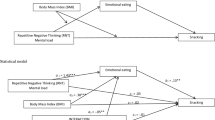
Hierarchical multiple regression results suggest that, after controlling for gender and BMI, ED-specific brooding, b = 1.32, SE = 0.13, β = 0.46, p < 0.0001, and reflection, b = 1.44, SE = 0.33, β = 0.19, p < 0.0001, accounted for unique variance in ED symptom severity. Moderation model results indicate that, at low levels of general reflection, b = − 0.06, SE = 0.02, β = − 0.51, p = 0.003, and ED-specific reflection, b = − 0.15, SE = 0.03, β = − 0.59, p < 0.0001, increased positive beliefs about rumination were associated with greater ED symptom severity.
Conclusion
Findings suggest ED-specific rumination accounts for ED symptom severity above and beyond general rumination, and that rumination-related expectancies influence the association between reflection and ED symptom severity.
Level of evidence
Level III, evidence obtained from a well-designed cohort study.

Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from Lisa M. Anderson (ande8936@umn.edu) upon reasonable request.
Code availability
Available upon reasonable request.
References
McEvoy P (2013) The relationship between worry, rumination, and comorbidity: evidence for repetitive negative thinking as a transdiagnostic construct. J Affect Disord 151(2013):313–320. https://doi.org/10.1016/j.jad.2013.06.014
Nolen-Hoeksema S, Watkins E (2011) A heuristic for developing transdiagnostic models of psychopathology: explaining multifinality and divergent trajectories. Perspect Psychol Sci 6(6):589–609. https://doi.org/10.1177/1745691611419672
Troop N, Holbrey A, Treasure J (1998) Stress, coping, and crisis support in eating disorders. Int J Eat Disord 24(2):157–166. https://doi.org/10.1002/(SICI)1098-108X(199809)24:2%3c157::AID-EAT5%3e3.0.CO;2-D
Nolen-Hoeksema S, Stice E, Wade E, Bohon C (2007) Reciprocal relations between rumination and bulimic, substance abuse, and depressive symptoms in female adolescents. J Abnorm Psychol 116(1):198–207. https://doi.org/10.1037/0021-843X.116.1.198
Naumann E, Tuschen-Caffier B, Voderholzer U, Caffier D, Svaldi J (2015) Rumination but not distraction increases eating-related symptoms in anorexia and bulimia nervosa. J Abnorm Psychol 124(2):412–420. https://doi.org/10.1037/abn0000046
Reilly E, Lavender J, Berner L, Brown T, Wierenga C, Kaye W (2019) Could repetitive negative thinking interfere with corrective learning? The example of anorexia nervosa. Int J Eat Disord 52:36–41. https://doi.org/10.1002/eat.22997
Treynor W, Gonzalez R, Nolen-Hoeksema S (2003) Rumination reconsidered: a psychometric analysis. Cogn Ther Res 27(3):247–259. https://doi.org/10.1023/A:1023910315561
Burwell R, Shirk S (2007) Subtypes of rumination in adolescence: Associations between brooding, reflection, depressive symptoms, and coping. J Clin Child Adolesc Psychol 36(1):56–65. https://doi.org/10.1080/15374410709336568
Schoofs H, Hermans D, Raes F (2010) Brooding and reflection as subtypes of rumination: Evidence from confirmatory factor analysis in nonclinical samples using the Dutch ruminative response scale. J Psychopathol Behav Assess 32(4):609–617. https://doi.org/10.1007/s10862-010-9182-9
Smith K, Mason T, Lavender J (2018) Rumination and eating disorder psychopathology: a meta-analysis. Clin Psychol Rev 61:9–23. https://doi.org/10.1016/j.cpr.2018.03.004
Naumann E, Tuschen-Caffier B, Voderholzer U, Schäfer J, Svaldi J (2016) Effects of emotional acceptance and rumination on media-induced body dissatisfaction in anorexia and bulimia nervosa. J Psychiatr Res 82:119–125. https://doi.org/10.1016/j.jpsychires.2016.07.021
Dondzilo L, Rieger E, Palermo R, Byrne S, Bell J (2016) Association between rumination factors and eating disorder behaviours in young women. Adv Eat Disord 4(1):84–98. https://doi.org/10.1080/21662630.2015.1118642
Jong-Meyer R, Beck B, Riede K (2009) Relationships between rumination, worry, intolerance of uncertainty and metacognitive beliefs. Personality Individ Differ 46(4):547–551. https://doi.org/10.1016/j.paid.2008.12.010
Papageorgiou C, Wells A (2001) Positive beliefs about depressive rumination: development and preliminary validation of a self-report scale. Behav Ther 32(1):13–26. https://doi.org/10.1016/S0005-7894(01)80041-1
Watkins E, Moulds M (2005) Positive beliefs about rumination in depression: a replication and extension. Personal Individ Differ 39(1):73–82. https://doi.org/10.1016/j.paid.2004.12.006
Wong Q, Moulds M (2010) Do socially anxious individuals hold positive metacognitive beliefs about rumination? Behav Chang 27(2):69–83. https://doi.org/10.1375/bech.27.2.69
Sütterlin S, Paap M, Babic S, Kübler A, Vögele C (2012) Rumination and age: some things get better. J Aging Res 2012:267327. https://doi.org/10.1155/2012/267327
Eisenberg D, Nicklett EJ, Roeder K (2011) Eating disorder symptoms among college students: prevalence, persistence, correlates, and treatment-seeking. J Am Coll Health 59(8):700–707. https://doi.org/10.1080/07448481.2010.546461
Ehrlich LE (2018) Perseverative thinking in eating pathology: do rumination patterns differ according to symptom type? [Master's Thesis, University at Albany]. ProQuest Dissertations and Theses Global.
Cowdrey F, Park R (2011) Assessing rumination in eating disorders: Principal component analysis of a minimally modified ruminative response scale. Eat Behav 12(4):321–324. https://doi.org/10.1016/j.eatbeh.2011.08.001
Stice E, Telch C, Rizvi S (2000) Development and validation of the eating disorder diagnostic scale: a brief self-report measure of anorexia, bulimia, and binge-eating disorder. Psychol Assess 12(2):123–131. https://doi.org/10.1037//1040-3590.12.2.123
Field A (2009) Discovering Statistics Using SPSS, Third Edition.
Hayes AF (2012) PROCESS: A versatile computational tool for observed variable mediation, moderation, and conditional process modeling. https://www.afhayes.com. Accessed 15 September 2020
Krabbenborg MA, Danner UN, Larsen JK et al (2012) The eating disorder diagnostic scale: psychometric features within a clinical population and a cut-off point to differentiate clinical patients from healthy controls. Eur Eat Disord Rev 20(4):315–320. https://doi.org/10.1002/erv.1144
Smith K, Schaumberg K, Reilly E et al (2020) The ecological validity of trait-level rumination measures among women with binge eating symptoms. Eat Weight Disord-Stud Anorexia Bulimia Obesity 26(1):181-190. https://doi.org/10.1007/s40519-019-00838-x
Watkins E, Scott J, Wingrove J et al. (2007) Rumination-focused cognitive behaviour therapy for residual depression: a case series. Behav Res Ther 45(9):2144–2154. https://doi.org/10.1016/j.brat.2006.09.018
Watkins E, Mullan E, Wingrove J et al. (2011) Rumination-focused cognitive–behavioural therapy for residual depression: Phase II randomised controlled trial. Br J Psychiatry 199(4):317–322. https://doi.org/10.1192/bjp.bp.110.090282
Acknowledgements
This work was supported by the National Institute of Mental Health of the National Institutes of Health under award numbers T32 MH082761 (L. Anderson), K23 MH123910 (L. Anderson), and K23 MH112867 (Haynos). It was additionally supported by the University of Minnesota Office of Undergraduate Research (Rich), Klarman Family Foundation (Haynos), and Hilda and Preston Davis Foundation (Haynos). This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Funding
This work was supported by the National Institute of Mental Health of the National Institutes of Health under award numbers T32 MH082761 (L. Anderson), K23 MH123910 (L. Anderson), and K23 MH112867 (Haynos). It was additionally supported by the University of Minnesota Office of Undergraduate Research (Rich), Klarman Family Foundation (Haynos), and Hilda and Preston Davis Foundation (Haynos). This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Data collection was conducted by LEE and DAA. Material preparation and data analysis were performed by ACR and LMA. The first draft of the manuscript was written by ACR and LMA, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflicts of interest to disclose
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
Participants signed informed consent regarding publishing their data.
Ethics approval
This study was approved by the University at Albany, State University of New York’s Institutional Review Board. Study procedures were performed in accordance with the Declaration of Helsinki.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rich, A.C., Haynos, A.F., Anderson, D.A. et al. The role of rumination and positive beliefs about rumination in eating pathology. Eat Weight Disord 27, 979–988 (2022). https://doi.org/10.1007/s40519-021-01209-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-021-01209-1