Abstract
Introduction
Obesity and chronic diseases disproportionately affect African-American women in the rural South (US) and may be influenced by adherence to a typical Southern-style diet. There is a need to examine dietary patterns of this population and to determine if consumption of nutritionally rich foods like nuts is associated with consumption of other nutritious foods. The objectives of this study were to identify (1) dietary patterns of overweight/obese African-American women in the rural South; (2) the role that nuts play in the diet; (3) and adherence to federal food group recommendations across dietary patterns.
Methods
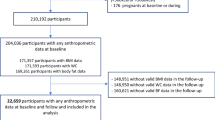
Secondary data analysis of two baseline 24-h dietary recalls was performed on 383 overweight/obese African-American women enrolled in a weight loss intervention in Alabama and Mississippi between 2011 and 2013. Cluster analysis identified dietary patterns. t tests and chi-square tests tested demographic and dietary differences across clusters. The proportion of women in each cluster who met federal recommendations for fruit, vegetable, nuts, added sugar, and sodium intake was calculated.
Results
Two dietary patterns were found. Nut intake frequency was higher in cluster 2 (P < .001), which was characterized by a higher intake frequency of fruits and vegetables, but high mean daily intake of added sugar (12.26 ± 7.67 tsp) and sodium (2800 ± 881 mg). Ninety-two percent of participants in this cluster consumed red/processed meats daily.
Conclusion
Even among women in this population who consume a more plant-based dietary pattern containing nuts, there is still a need to decrease intake of added sugar, sodium, and red meat.
Similar content being viewed by others
References
Befort CA, Nazir N, Perri MG. Prevalence of obesity among adults from rural and urban areas of the United States: findings from NHANES (2005-2008). J Rural Health. 2012;28(4):392–7.
Hill JL, You W, Zoellner JM. Disparities in obesity among rural and urban residents in a health disparate region. BMC Public Health. 2014;14:1051.
Centers for Disease Control and Prevention. Health of black or African-American non-Hispanic population. 2015. [cited 2015 July].
Friday L. Exploring the causes of black women’s obesity. 2012. Available from: https://www.bu.edu/today/2012/exploring-the-causes-of-black-womens-obesity/.
Food Research and Action Center. Obesity in the U.S. 2016. Available from: http://frac.org/initiatives/hunger-and-obesity/obesity-in-the-us/.
National Cancer Institute. Obesity and cancer risk. 2012. [cited 2015 July 15]; Available from: http://www.cancer.gov/about-cancer/causes-prevention/risk/obesity/obesity-fact-sheet.
American Cancer Society. Cancer facts and figures for African Americans, 2013–2014. 2013. Available from: http://www.cancer.org/acs/groups/content/@epidemiologysurveilance/documents/document/acspc-036921.pdf.
Mattes RD, Kris-Etherton PM, Foster GD. Impact of peanuts and tree nuts on body weight and healthy weight loss in adults. J Nutr. 2008;138(9):1741S–5S.
O’Neil CE, Fulgoni 3rd VL, Nicklas TA. Tree nut consumption is associated with better adiposity measures and cardiovascular and metabolic syndrome health risk factors in U.S. adults: NHANES 2005-2010. Nutr J. 2015;14:64.
Hu FS, Stampfer MJ, Manson JE, et al. Frequent nut consumption and risk of coronary heart disease in women: a prospective cohort study. BMJ. 1998;317.
Rajaram S, Sabate J. Nuts, body weight and insulin resistance. Br J Nutr. 2006;96(Suppl 2):S79–86.
Gadgil MD, et al. Dietary patterns are associated with metabolic risk factors in South Asians living in the United States. J Nutr. 2015;145(6):1211–7.
Kang MP, Park YH, Baik HW, Paik HY, Joung H. Grains, nuts and fruits dietary pattern is associated with reduced likelihood of having metabolic syndrome. FASEB J. 2012;26(SIb363).
Sabate J, Wien M. A perspective on vegetarian dietary patterns and risk of metabolic syndrome. Br J Nutr. 2015;113(Suppl 2):S136–43.
Tapsell LC. Foods and food components in the Mediterranean diet: supporting overall effects. BMC Med. 2014;12:100.
Weng LC, et al. A diet pattern with more dairy and nuts, but less meat is related to lower risk of developing hypertension in middle-aged adults: the atherosclerosis risk in communities (ARIC) study. Nutrients. 2013;5(5):1719–33.
United States Department of Agriculture. Dietary guidelines. 2015. [cited 2015 July 15]; Available from: http://www.choosemyplate.gov/dietary-guidelines.html.
King JC, Blumberg J, Ingwersen L, Jenab M, Tucker KL. Tree nuts and peanuts as components of a healthy diet. J Nutr. 2008;138(9):1736S–40S.
Jacobs Jr DR, Gross MD, Taspell LC. Food synergy: an operational concept for understanding nutrition. Am J Clin Nutr. 2009;89(5):1543S–8S.
Liu RH. Health benefits of fruit and vegetables are from additive and synergistic combinations of phytochemicals. Am J Clin Nutr. 2003;78(3 Suppl):517S–20S.
Judd SE, et al. Dietary patterns derived using exploratory and confirmatory factor analysis are stable and generalizable across race, region, and gender subgroups in the REGARDS study. Front Nutr. 2014;1:29.
Jiankang L, Hickson D, Musani S, et al. Dietary patterns, abdominal visceral adipose tissue and cardiometabolic risk factos in African Americans: the Jackson heart study. Obesity (Silver Spring). 2013;21(3):644–51.
Hernando Requejo O, Rubio Rodriguez MC. Nutrition and cancer. Nutr Hosp. 2015;32(Suppl 1):67–72.
Rouhani MH, et al. Is there a relationship between red or processed meat intake and obesity? A systematic review and meta-analysis of observational studies. Obes Rev. 2014;15(9):740–8.
Wang Y, Beydoun MA. Meat consumption is associated with obesity and central obesity among US adults. Int J Obes. 2009;33(6):621–8.
Ma Y, He FJ, MacGregor GA. High salt intake: independent risk factor for obesity? Hypertension. 2015;66(4):843–9.
Maioli TU, et al. High sugar and butter (HSB) diet induces obesity and metabolic syndrome with decrease in regulatory T cells in adipose tissue of mice. Inflamm Res. 2016;65(2):169–78.
He FJ, MacGregor GA. Salt and sugar: their effects on blood pressure. Pflugers Arch. 2015;467(3):577–86.
Stanhope KL. Sugar consumption, metabolic disease and obesity: the state of the controversy. Crit Rev Clin Lab Sci. 2016;53(1):52–67.
Diet Health. African-American diet. 2015. [cited 2015 July 15]; Available from: http://diet.com/g/africanamerican-diet.
African-American Registry. Soul food: a brief history. 2013. [cited 2015 July 15]; Available from: http://www.aaregistry.org/historic_events/view/soul-food-brief-history
Yang Y, et al. Favorite foods of older adults living in the Black Belt region of the United States. Influences of ethnicity, gender, and education. Appetite. 2013;63:18–23.
National Peanut Board. Peanut Country, U.S.A. 2014. Available from: http://nationalpeanutboard.org/the-facts/peanut-country-u-s-a/.
Brinegar J. Pecans—the South’s favorite nut. 2014. [cited 2015 July 15]; Available from: http://courier-tribune.com/thrive-magazine/pecans-south-s-favorite-nut.
Browne C. Pecan industry in Alabama. In: Encyclopedia of Alabama. 2008.
Carson TL, et al. A study of the relationship between food group recommendations and perceived stress: findings from black women in the Deep South. J Obes. 2015;2015:203164.
Hinton A, et al. The community health advisor program and the Deep South Network for Cancer Control: health promotion programs for volunteer community health advisors. Fam Community Health. 2005;28(1):20–7.
Lisovicz N, et al. The Deep South Network for Cancer Control. Building a community infrastructure to reduce cancer health disparities. Cancer. 2006;107(8 Suppl):1971–9.
National Cancer Institute. ASA24. 2015. [cited 2015 May 6]; Available from: http://epi.grants.cancer.gov/asa24/.
Bowman SA, Friday JE, Moshfegh AJ. MyPyramid equivalents database, 2.0 for USDA survey foods, 2003–2004 (online). Beltsville, MD: U.S. Department of Agriculture; 2008.
Fransen HP, et al. A posteriori dietary patterns: how many patterns to retain? J Nutr. 2014;144(8):1274–82.
Hu FB. Dietary pattern analysis: a new direction in nutritional epidemiology. Curr Opin Lipidol. 2002;13(1):3–9.
Parker R. Variable clustering in JMP. 2013. Available from: http://blogs.sas.com/content/jmp/2013/03/13/variable-clustering-in-jmp/
James DC. Cluster analysis defines distinct dietary patterns for African-American men and women. J Am Diet Assoc. 2009;109(2):255–62.
Ward Jr J. Hierarchical grouping to optimize an object function. J Am Stat Assoc. 2012;58(301):1963.
JMP. Hierarchical clustering. 2016. Available from: http://www.jmp.com/support/help/Hierarchical_Clustering.shtml.
Huang Z. Extensions to the k-means algorithm for clustering large data sets with categorical values. Data Min Knowl Disc. 1998;2:283–304.
Quatromoni PA, Copenhafer D, Demissie S, et al. The internal validity of a dietary pattern analysis. The Framingham nutrition studies. J Epidemiol Community Health. 2002;56(5):381–8.
United States Department of Health and Human Services. Summary of qualified health claims subject to enforcement discretion. 2014. [cited 2015 July 15]; Available from: http://www.fda.gov/Food/IngredientsPackagingLabeling/LabelingNutrition/ucm073992.htm#cardio.
United States Department of Agriculture. Salt and sodium: 10 tips to help you cut back. 2015. [cited 2015; Available from: http://www.choosemyplate.gov/food-groups/downloads/TenTips/DGTipsheet14SaltAndSodium.pdf.
SAS Institute, Inc. New features in JMP 12 and JMP Pro 12. [cited 2017 January 31]. Available from: http://www.jmp.com/content/dam/jmp/documents/en/software/jmp/jmp12/new-features-in-jmp-and-jmp-pro12.pdf.
Garcia-Garcia E, et al. Obesity and the metabolic syndrome as a public health problem: a reflection. Salud Publica Mex. 2008;50(6):530–47.
Zhou MS, Wang A, Yu H. Link between insulin resistance and hypertension: what is the evidence from evolutionary biology? Diabetol Metab Syndr. 2014;6(1):12.
Boada LD, Henriquez-Hernandez LA, Luzardo OP. The impact of red and processed meat consumption on cancer and other health outcomes: epidemiological evidences. Food Chem Toxicol. 2016;92:236–44.
Aykan NF. Red meat and colorectal cancer. Oncol Rev. 2015;9(1):288.
James DC. Factors influencing food choices, dietary intake, and nutrition-related attitudes among African Americans: application of a culturally sensitive model. Ethn Health. 2004;9(4):349–67.
Acknowledgements
The project described was supported by Grant Number 1U54CA153719 from the National Cancer Institute (NCI) Center to Reduce Cancer Health Disparities (CRCHD). Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the NCI or CRCHD. Recognition and appreciation is provided to all of the Deep South Network for Cancer Control staff (i.e., County Coordinators, Regional Coordinators, and Central Office personnel). A special thanks to the Community Health Advisors trained as Research Partners and study participants who helped to make all of the research possible.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
SS, SJ, BB, TLC, PCL, and MLB declare that they have no conflicts of interest.
Research Involving Human Participants
All procedures performed in this study involving human participants were in accordance with the ethical standards of the Institutional Review Board and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Sterling, S., Judd, S., Bertrand, B. et al. Dietary Patterns Among Overweight and Obese African-American Women Living in the Rural South. J. Racial and Ethnic Health Disparities 5, 141–150 (2018). https://doi.org/10.1007/s40615-017-0351-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40615-017-0351-3