Abstract
Objective
A 5% change in weight is a significant predictor for frailty and obesity. We ascertained how self-reported weight change over the lifespan impacts rates of frailty in older adults.
Methods
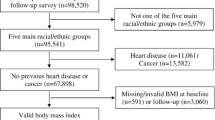
We identified 4,984 subjects ≥60 years with body composition measures from the National Health and Nutrition Examination Survey. An adapted version of Fried’s frailty criteria was used as the primary outcome. Self-reported weight was assessed at time current,1 and 10 years earlier and at age 25. Weight changes between each time point were categorized as ≥ 5%, ≤5% or neutral. Logistic regression assessed the impact of weight change on the outcome of frailty.
Results
Among 4,984 participants, 56.5% were female, mean age was 71.1 years, and mean BMI was 28.2kg/m2. A weight loss of ≥ 5% had a higher association with frailty compared to current weight, age 25 (OR 2.94 [1.72,5.02]), 10 years ago (OR 1.68 [1.05,2.69]), and 1 year ago (OR 1.55 [1.02,2.36]). Weight gain in the last year was associated with increased rate of frailty (1.59 [1.09,2.32]).
Conclusion
There is an association between frailty and reported weight loss over time while only weight gain in the last year has an association with frailty.

Similar content being viewed by others
Abbreviations
- BMI:
-
body mass index
- NHANES:
-
National Health and Nutrition Examination Survey
References
Chong E, Ho E, Baldevarona-Llego J, Chan M, Wu L, Tay L. Frailty and Risk of Adverse Outcomes in Hospitalized Older Adults: A Comparison of Different Frailty Measures. J Am Med Dir Assoc. 2017;18(7):638.e7–.e11.
Clegg A, Young J, Iliffe S, Rikkert MO, Rockwood K. Frailty in elderly people. Lancet. 2013;381(9868):752–62.
Fried LP, Tangen CM, Walston J, Newman AB, Hirsch C, Gottdiener J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56(3):M146–56.
Robinson TN, Wu DS, Stiegmann GV, Moss M. Frailty predicts increased hospital and six-month healthcare cost following colorectal surgery in older adults. Am J Surg. 2011;202(5):511–4.
Bock JO, Konig HH, Brenner H, Haefeli WE, Quinzler R, Matschinger H, et al. Associations of frailty with health care costs—results of the ESTHER cohort study. BMC Health Serv Res. 2016;16:128.
Makizako H, Shimada H, Doi T, Tsutsumimoto K, Suzuki T. Impact of physical frailty on disability in community-dwelling older adults: a prospective cohort study. BMJ Open. 2015;5(9):e008462.
Comans TA, Peel NM, Hubbard RE, Mulligan AD, Gray LC, Scuffham PA. The increase in healthcare costs associated with frailty in older people discharged to a post-acute transition care program. Age Ageing. 2016;45(2):317–20.
Avila-Funes JA, Amieva H, Barberger-Gateau P, Le Goff M, Raoux N, Ritchie K, et al. Cognitive impairment improves the predictive validity of the phenotype of frailty for adverse health outcomes: the three-city study. J Am Geriatr Soc. 2009;57(3):453–61.
Meltzer AA, Everhart JE. Unintentional weight loss in the United States. Am J Epidemiol. 1995;142(10):1039–46.
Willett WC. Weight loss in the elderly: cause or effect of poor health? Am J Clin Nutr. 1997;66(4):737–8.
Beaufrere B, Morio B. Fat and protein redistribution with aging: metabolic considerations. Eur J Clin Nutr. 2000;54 Suppl 3:S48–53.
Gallagher D, Visser M, De Meersman RE, Sepulveda D, Baumgartner RN, Pierson RN, et al. Appendicular skeletal muscle mass: effects of age, gender, and ethnicity. J Appl Physiol (1985). 1997;83(1):229–39.
Batsis JA, Mackenzie TA, Bartels SJ, Sahakyan KR, Somers VK, Lopez-Jimenez F. Diagnostic accuracy of body mass index to identify obesity in older adults: NHANES 1999–2004. Int J Obes (Lond). 2016;40(5):761–7.
Choi KM. Sarcopenia and sarcopenic obesity. Korean J Intern Med. 2016;31(6):1054–60.
Cauley JA. An Overview of Sarcopenic Obesity. J Clin Densitom. 2015;18(4):499–505.
Andres R, Muller DC, Sorkin JD. Long-term effects of change in body weight on all-cause mortality. A review. Ann Intern Med. 1993;119(7 Pt 2):737–43.
Oh TJ, Moon JH, Choi SH, Lim S, Park KS, Cho NH, et al. Body-Weight Fluctuation and Incident Diabetes Mellitus, Cardiovascular Disease, and Mortality: A 16-Year Prospective Cohort Study. J Clin Endocrinol Metab. 2019;104(3):639–46.
Payette H, Coulombe C, Boutier V, Gray-Donald K. Weight loss and mortality among free-living frail elders: a prospective study. J Gerontol A Biol Sci Med Sci. 1999;54(9):M440–5.
Somes GW, Kritchevsky SB, Shorr RI, Pahor M, Applegate WB. Body mass index, weight change, and death in older adults: the systolic hypertension in the elderly program. Am J Epidemiol. 2002;156(2):132–8.
Tully CL, Snowdon DA. Weight change and physical function in older women: findings from the Nun Study. J Am Geriatr Soc. 1995;43(12):1394–7.
Alibhai SM, Greenwood C, Payette H. An approach to the management of unintentional weight loss in elderly people. CMAJ. 2005;172(6):773–80.
Murphy RA, Patel KV, Kritchevsky SB, Houston DK, Newman AB, Koster A, et al. Weight change, body composition, and risk of mobility disability and mortality in older adults: a population-based cohort study. J Am Geriatr Soc. 2014;62(8):1476–83.
Dee A, Kearns K, O’Neill C, Sharp L, Staines A, O’Dwyer V, et al. The direct and indirect costs of both overweight and obesity: a systematic review. BMC Res Notes. 2014;7:242.
Visscher TL, Seidell JC. The public health impact of obesity. Annu Rev Public Health. 2001;22:355–75.
Hirani V, Naganathan V, Blyth F, Le Couteur DG, Seibel MJ, Waite LM, et al. Longitudinal associations between body composition, sarcopenic obesity and outcomes of frailty, disability, institutionalisation and mortality in community-dwelling older men: The Concord Health and Ageing in Men Project. Age Ageing. 2016.
Crow RS, Lohman MC, Titus AJ, Bruce ML, Mackenzie TA, Bartels SJ, et al. Mortality Risk Along the Frailty Spectrum: Data from the National Health and Nutrition Examination Survey 1999 to 2004. J Am Geriatr Soc. 2018;66(3):496–502.
Rippberger PL, Emeny RT, Mackenzie TA, Bartels SJ, Batsis JA. The association of sarcopenia, telomere length, and mortality: data from the NHANES 1999–2002. Eur J Clin Nutr. 2018;72(2):255–63.
Kulminski AM, Ukraintseva SV, Kulminskaya IV, Arbeev KG, Land K, Yashin AI. Cumulative deficits better characterize susceptibility to death in elderly people than phenotypic frailty: lessons from the Cardiovascular Health Study. J Am Geriatr Soc. 2008;56(5):898–903.
Jensen MD, Ryan DH, Apovian CM, Ard JD, Comuzzie AG, Donato KA, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. J Am Coll Cardiol. 2014;63(25 Pt B):2985–3023.
Painter SL, Ahmed R, Hill JO, Kushner RF, Lindquist R, Brunning S, et al. What Matters in Weight Loss? An In-Depth Analysis of Self-Monitoring. J Med Internet Res. 2017;19(5):e160.
Bieniek J, Wilczynski K, Szewieczek J. Fried frailty phenotype assessment components as applied to geriatric inpatients. Clin Interv Aging. 2016;11:453–9.
Stenholm S, Strandberg TE, Pitkala K, Sainio P, Heliovaara M, Koskinen S. Midlife obesity and risk of frailty in old age during a 22-year follow-up in men and women: the Mini-Finland Follow-up Survey. J Gerontol A Biol Sci Med Sci. 2014;69(1):73–8.
Strandberg TE, Sirola J, Pitkala KH, Tilvis RS, Strandberg AY, Stenholm S. Association of midlife obesity and cardiovascular risk with old age frailty: a 26-year follow-up of initially healthy men. Int J Obes (Lond). 2012;36(9):1153–7.
Batsis JA, Mackenzie TA, Lopez-Jimenez F, Bartels SJ. Sarcopenia, sarcopenic obesity, and functional impairments in older adults: National Health and Nutrition Examination Surveys 1999–2004. Nutr Res. 2015;35(12):1031–9.
Newman AB, Lee JS, Visser M, Goodpaster BH, Kritchevsky SB, Tylavsky FA, et al. Weight change and the conservation of lean mass in old age: the Health, Aging and Body Composition Study. Am J Clin Nutr. 2005;82(4):872–8; quiz 915–6.
Cederholm T. Overlaps between Frailty and Sarcopenia Definitions. Nestle Nutr Inst Workshop Ser. 2015;83:65–9.
Batsis JA, Petersen CL, Crow RS, Cook SB, Stevens CJ, Lillian SM, et al. Weight Change and Risk of Sarcopenia: Data from the National Health and Nutrition Examination Surveys 1999–2004 [Abstract]. 2018 International Frailty & Sarcopenia Conference, Miami Beach, FL, https://frailty-sarcopenia.com/docs/abstracts-2018pdf [accessed 18 September 2018]. 2018.
Flegal KM, Kit BK, Orpana H, Graubard BI. Association of all-cause mortality with overweight and obesity using standard body mass index categories: a systematic review and meta-analysis. JAMA. 2013;309(1):71–82.
Bowen ME. The relationship between body weight, frailty, and the disablement process. J Gerontol B Psychol Sci Soc Sci. 2012;67(5):618–26.
Villareal DT, Banks M, Siener C, Sinacore DR, Klein S. Physical frailty and body composition in obese elderly men and women. Obes Res. 2004;12(6):913–20.
Luo J, Thomson CA, Hendryx M, Tinker LF, Manson JE, Li Y, et al. Accuracy of self-reported weight in the Women’s Health Initiative. Public Health Nutr. 2019;22(6):1019–28.
Shamliyan T, Talley KM, Ramakrishnan R, Kane RL. Association of frailty with survival: a systematic literature review. Ageing Res Rev. 2013;12(2):719–36.
Fernandez-Garrido J, Ruiz-Ros V, Buigues C, Navarro-Martinez R, Cauli O. Clinical features of prefrail older individuals and emerging peripheral biomarkers: a systematic review. Arch Gerontol Geriatr. 2014;59(1):7–17.
Azur MJ, Stuart EA, Frangakis C, Leaf PJ. Multiple imputation by chained equations: what is it and how does it work? Int J Methods Psychiatr Res. 2011;20(1):40–9.
Acknowledgements
The authors would like to acknowledge Meaghan A. Kennedy MD, MPH who helped with editing and reviewing the transcript as well as support from the National Institute on Aging of the National Institutes of Health, Burroughs-Wellcome/Dartmouth Big Data in the Life Sciences Training Program, National Institute of Mental Health, Dartmouth Health Promotion and Disease Prevention Research Center, The Dartmouth Center for Health and Aging and the Dartmouth Hitchcock Medical Center Department of Medicine.
Funding
Funding: Dr. Batsis receives funding from the National Institute on Aging of the National Institutes of Health under Award Number K23AG051681. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. Dr. Batsis has also received honoraria from the Royal College of Physicians of Ireland, Endocrine Society, and Dinse, Knapp, McAndrew LLC, legal firm. Dr. Mackenzie: none. Dr. Cook: none. Alexander Titus’ research reported in this publication was supported in part by the National Institutes of Health under Award Number T32LM012204. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. Mr. Petersen’s research reported in this publication was supported by the Burroughs-Wellcome/Dartmouth Big Data in the Life Sciences Training Program. Dr. Crow’s research reported in this publication was supported by The Dartmouth Center for Health and Aging and the Department of Medicine. Dr. Stevens’ research is supported by National Institute of Mental Health (T32 MH073553, PI: Bruce, Fellow: Stevens). Support was also provided by the Dartmouth Health Promotion and Disease Prevention Research Center supported by Cooperative Agreement Number U48DP005018 from the Centers for Disease Control and Prevention. The findings and conclusions in this journal article are those of the authors and do not necessarily represent the official position of the Centers for Disease Control and Prevention. The authors acknowledge Friends of the Norris Cotton Cancer Center at Dartmouth and NCI Cancer Center Support Grant 5P30 CA023108-37 Developmental Funds.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures: There are no conflicts of interest pertaining to this manuscript
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Crow, R.S., Petersen, C.L., Cook, S.B. et al. Reported Weight Change in Older Adults and Presence of Frailty. J Frailty Aging 9, 74–81 (2020). https://doi.org/10.14283/jfa.2019.44
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.14283/jfa.2019.44