Abstract
Purpose
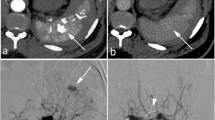
Non-operative management (NOM) of blunt splenic injury (BSI) uses angioembolization (AE) or observation (OBS). AE improves the success of NOM. However, how AE improves BSI is unknown. We hypothesized AE would decrease rate of pseudoaneurysm (PSA) presence, PSA size, PSA number, and rate of active extravasation.
Methods
We performed a retrospective review of computerized tomography (CT)-diagnosed BSI over a 2-year period. Patients undergoing NOM with an initial and repeat CT were included. Patients were excluded if they underwent primary splenectomy after BSI diagnosis or did not have repeat CT imaging.
Results
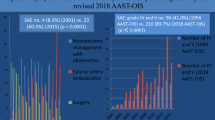
One hundred and fifteen patients with BSI had repeat CT imaging; 55/115 (47.8%) had AE; and 60/115 (52.2%) had OBS. On the initial CT, AE patients had more frequent PSA presence (52.7% vs. 6.7%, p < 0.001), higher median number of PSA (1.0 vs. 0, p < 0.001), higher median PSA size (1.15 mm vs. 0 mm, p < 0.001), and more frequent rates of active extravasation (10.9% vs. 0%, p = 0.01) compared with OBS patients. On repeat CT compared to the initial CT, AE patients had significant decrease in rate of PSA presence (21.8% vs. 52.7%, p < 0.001), median PSA size (0 mm vs. 1.15 mm, p < 0.001), median PSA number (p < 0.001), and rate of active extravasation (0% vs. 10.9%, p = 0.03). On repeat CT compared to the initial CT, OBS patients had an increase in rate of PSA presence (18.3% vs. 6.7%, p = 0.04).
Conclusions
AE significantly decreases PSA presence, number, and size as well as rates of active extravasation. AE should be standard practice in vascular injuries undergoing NOM to maximize splenic salvage.
Similar content being viewed by others
References
Davis KA, Fabian TC, Croce MA, et al. Improved success in nonoperative management of blunt splenic injuries: embolization of splenic artery pseudoaneurysms. J Trauma. 1998;44(6):1008–13 (discussion 1013–5).
Sabe AA, Claridge JA, Rosenblum DI, et al. The effects of splenic artery embolization on nonoperative management of blunt splenic injury: a 16-year experience. J Trauma. 2009;67(3):565–72 (discussion 571–2).
Moore EE, Cogbill TH, Jurkovich GJ, et al. Organ injury scaling: spleen and liver (1994 revision). J Trauma. 1995;38(3):323–4.
Crichton JCI, Naidoo K, Yet B, et al. The role of splenic angioembolization as an adjunct to nonoperative management of blunt splenic injuries: a systematic review and meta-analysis. J Trauma Acute Care Surg. 2017;83(5):934–43.
Zarzaur BL, Dunn JA, Leininger B, et al. Natural history of splenic vascular abnormalities after blunt injury: a western trauma association multicenter trial. J Trauma Acute Care Surg. 2017;83(6):999–1005.
Schurr MJ, Fabian TC, Gavant M, et al. Management of blunt splenic trauma: computed tomographic contrast blush predicts failure of nonoperative management. J Trauma. 1995;39(3):507–12 (discussion 512–3).
Stassen NA, Bhullar I, Cheng JD, et al. Selective nonoperative management of blunt splenic injury: an eastern association for the surgery of trauma practice management guideline. J Trauma Acute Care Surg. 2012;73(5 Suppl 4):S294–300.
Requarth JA. Distal splenic artery hemodynamic changes during transient proximal splenic artery occlusion in blunt splenic injury patients: a mechanism of delayed splenic hemorrhage. J Trauma. 2010;69(6):1423–6.
Banerjee A, Duane TM, Wilson SP, et al. Trauma center variation in splenic artery embolization and spleen salvage: a multicenter analysis. J Trauma Acute Care Surg. 2013;75(1):69–74 (discussion 74–5).
Harbrecht BG, Ko SH, Watson GA, et al. Angiography for blunt splenic trauma does not improve the success rate of nonoperative management. J Trauma. 2007;63(1):44–9.
Zarzaur BL, Kozar R, Myers JG, et al. The splenic injury outcomes trial: an American association for the surgery of trauma multi-institutional study. J Trauma Acute Care Surg. 2015;79(3):335–42.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Margaret Lauerman, Kathirkamanathan Shanmuganathan, Nana Simpson, Deborah Stein, and Thomas Scalea have no conflicts of interest to report. Megan Brenner is on the Clinical Advisory Board of Prytime Medical Inc.
Rights and permissions
About this article
Cite this article
Lauerman, M.H., Brenner, M., Simpson, N. et al. Angioembolization significantly improves vascular injuries in blunt splenic trauma. Eur J Trauma Emerg Surg 47, 99–103 (2021). https://doi.org/10.1007/s00068-019-01151-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-019-01151-z