Abstract
Purpose
The aim of the study was to investigate the oxidative damage and inflammatory effects of sepsis on the urogenital system in the Lipopolysaccharide (LPS)-induced sepsis model and ameliorating role of Pregabalin (PGB).
Methods
Twenty-four female Wistar Albino rats (12 months old) were divided into 3 groups as follows: Sepsis group (Group S) (5 mg/kg LPS, i.p, single dose); Sepsis+ PGB group (Group SP) (5 mg/kg LPS, i.p, single dose and 30 mg/kg PGB); Control group (Group C) (0.1 ml/oral and i.p. saline, single dose), 6 h after LPS administration, the animals were killed. Subsequently, analyses of urogenital tissue oxidant/antioxidant status, histopathological and immunohistochemical analyses were performed.
Results
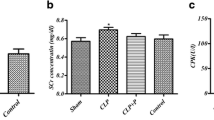
Total oxidative status (TOS) and oxidative stress index (OSI) values in the urogenital tissues were increased in Group S (Total anti-oxidative status (TAS) decreased) compared to the Control group (p < 0.05). PGB improved these values (p < 0.05). The immunohistochemical markers [Caspase-3, granulocyte colony-stimulating factor (G-CSF), interleukin-6 (IL-6), Serum Amyloid A (SAA) and inducible nitric oxide synthase (iNOS)] were significantly increased in Group S except for bladder (p < 0.001). Statistically significant immunohistochemical positiveness was found only for IL-6 in urinary bladder, though all the others values were negative. With the administration of PGB (Group SP), the expressions of these immunoreactions were markedly decreased (p < 0.001).
Conclusions
These findings demonstrated that sepsis caused oxidative stress and inflammation in the urogenital tissues. We have revealed that PGB ameliorated tissue damage caused by sepsis.






Similar content being viewed by others
References
Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M et al (2016) The third ınternational consensus definitions for sepsis and septic shock (Sepsis-3). JAMA 315(8):801–810. https://doi.org/10.1001/jama.2016.0287
Fleischmann C, Scherag A, Adhikari NKJ, Hartog CS, Tsaganos T, Schlattmann P, Angus DC, Reinhart K (2016) Assessment of global ıncidence and mortality of hospital-treated sepsis current estimates and limitations. Am J Respir Crit Care Med 193(3):259–272
Marshall JC, Vincent JL, Guyatt G, Angus DC, Abraham E, Bernard G, Bombardier C, Calandra T, Jørgensen HS, Sylvester R, Boers M (2005) Outcome measures for clinical research in sepsis: a report of the 2nd Cambridge Colloquium of the International Sepsis Forum. Crit Care Med 33(8):1708–1716. https://doi.org/10.1097/01.CCM.0000174478.70338.03
Tsiotou AG, Sakorafas GH, Anagnostopoulos G, Bramis J (2005) Septic shock; current pathogenetic concepts from a clinical perspective. Med Sci Monit 11(3):76–85
Ding Y, Lin Y, Zhu T, Huang M, Xu Q (2014) Interleukin 6 increases dysfunction of organs in sepsis rats through sirtuin 1. Int J Clin Exp Med 7(9):2593–2598
Bozza FA, D’Avila JC, Ritter C, Sonneville R, Sharshar T, Dal-Pizzol F (2013) Bioenergetics, mitochondrial dysfunction, and oxidative stress in the pathophysiology of septic encephalopathy. Shock 39(1):10–16. https://doi.org/10.1097/SHK.0b013e31828fade1
Perl M, Chung CS, Garber M, Huang X, Ayala A (2006) Contribution of anti-inflammatory/immune suppressive processes to the pathology of sepsis. Front Biosci 11:272–299. https://doi.org/10.2741/1797
Zhang HT, Tian EB, Chen YL, Deng HT, Wang QT (2015) Proteomic analysis for finding serum pathogenic factors and potential biomarkers in multiple myeloma. Chin Med J (Engl). https://doi.org/10.4103/0366-6999.155112
Naffaa M, Makhoul BF, Tobia A, Kaplan M, Aronson D, Azzam ZS, Saliba W (2014) Procalcitonin and interleukin 6 for predicting blood culture positivity in sepsis. Am J Emerg Med 32:448–451. https://doi.org/10.1016/j.ajem.2013.12.058
Kumar S, Gupta E, Srivastava VK, Kaushik S, Saxena J, Goyal LK, Mehta S, Jyoti A (2019) Nitrosative stress and cytokines are linked with the severity of sepsis and organ dysfunction. Br J Biomed Sci 76(1):29–34. https://doi.org/10.1080/09674845.2018.1543160
Chousterman BG, Arnaud M (2018) Is there a role for hematopoietic growth factors during sepsis? Front Immunol 21(9):1015. https://doi.org/10.3389/fimmu.2018.01015
Aşcı S, Demirci S, Aşcı H, Doğuç DK, Onaran İ (2016) Neuroprotective effects of pregabalin on cerebral ischemia and reperfusion. Balkan Med J 33(2):221–227. https://doi.org/10.5152/balkanmedj.2015
Celik M, Kose A, Kose D, Karakus E, Akpinar E, Calik M, Dostbil A, Calikoglu C, Aksoy M, Ozel L (2015) The double-edged sword:effects of pregabalin on experimentally induced sciatic nervetransection and crush injury in rats. Int J Neurosci 125(11):845–854. https://doi.org/10.3109/00207454.2014.978976
Ha KY, Carragee E, Cheng I, Kwon SE, Kim YH (2011) Pregabalin as neuroprotector after spinal cord injury in rats: biochemical analysis and effect on glial cells. J Korean Med Sci 26(3):404–411. https://doi.org/10.3346/jkms.2011.26.3.404
André V, Rigoulot MA, Koning E, Ferrandon A, Nehlig A (2003) Long term pregabalin treatment protects basal cortices and delays the occurrence of spontaneous seizures in the lithium-pilocarpine model in the rat. Epilepsia 44(7):893–903. https://doi.org/10.1046/j.1528-1157.2003.61802.x
Song Y, Jun JH, Shin EJ, Kwak YL, Shin JS, Shim JK (2017) Effect of pregabalin administration upon reperfusion in a rat model of hyperglycemic stroke: mechanistic insights associated with high-mobility group box 1. PLoS One 12(2):e0171147. https://doi.org/10.1371/journal.pone.0171147
Shamsi Meymandi M, Soltani Z, Sepehri G, Amiresmaili S, Farahani F, Moeini Aghtaei M (2018) Effects of pregabalin on brain edema, neurologic and histologic outcomes in experimental traumatic brain injury. Brain Res Bull 140:169–175. https://doi.org/10.1016/j.brainresbull.2018.05.001
Ozmen O, Topsakal S (2019) Pregabalin ameliorates lipopolysaccharide-induced pancreatic inflammation in aged rats. Endocr Metab Immune Disord Drug Targets. https://doi.org/10.2174/1871530319666190306095532
Karube N, Ito S, Sako S, Hirokawa J, Yokoyama T (2017) Sedative effects of oral pregabalin premedication on intravenous sedation using propofol target-controlled infusion. J Anesth 31(4):586–592. https://doi.org/10.1007/s00540-017-2366-7
Montgomery S, Chatamra K, Pauer L, Whalen E, Baldinetti F (2008) Efficacy and safety of pregabalin in elderly people with generalised anxiety disorder. Br J Psychiatry 193(5):389–394. https://doi.org/10.1192/bjp.bp.107.037788
Mathieson S, Kasch R, Maher CG, Pinto RZ, McLachlan AJ, Koes BW, Lin CC (2019) Combination drug therapy for the management of low back pain and sciatica: systematic review and meta-analysis. J Pain 20(1):1–15. https://doi.org/10.1016/j.jpain.2018.06.005
Loutochin O, Al Afraa T, Campeau L, Mahfouz W, Elzayat E, Corcos J (2012) Effect of the anticonvulsant medications pregabalin and lamotrigine on urodynamic parameters in an animal model of neurogenic detrusor overactivity. Neurourol Urodyn 31(7):1197–1202. https://doi.org/10.1002/nau.21214
Imai A, Matsunami K, Takagi H, Ichigo S (2013) New generation nonhormonal management for hot flashes. Gynecol Endocrinol 29(1):63–66. https://doi.org/10.3109/09513590.2012.705380
Edwards L (2015) Vulvodynia. Clin Obstet Gynecol 58(1):143–152. https://doi.org/10.1097/GRF.0000000000000093
Asgari Z, Rouholamin S, Nataj M, Sepidarkish M, Hosseini R, Razavi M (2017) Dose ranging effects of pregabalin on pain in patients undergoing laparoscopic hysterectomy: a randomized, double blinded, placebo controlled, clinical trial. J Clin Anesth 38:13–17. https://doi.org/10.1016/j.jclinane.2017.01.015
Di Cesare Mannelli L, Maresca M, Micheli L, Farina C, Scherz MW, Ghelardini C (2017) A rat model of FOLFOX-induced neuropathy: effects of oral dimiracetam in comparison with duloxetine and pregabalin. Cancer Chemother Pharmacol 80(6):1091–1103. https://doi.org/10.1007/s00280-017-3449-8
Meymandi MS, Sepehri G, Abdolsamadi M, Shaabani M, Heravi G, Yazdanpanah O, Aghtaei MM (2017) The effects of co-administration of pregabalin and vitamin E on neuropathic pain induced by partial sciatic nerve ligation in male rats. Inflammopharmacology 25(2):237–246. https://doi.org/10.1007/s10787-017-0325-4
Erel O (2004) A novel automated direct measurement method for total antioxidant capacity using a new generation, more stable ABTS radical cation. Clin Biochem 37(4):277–285. https://doi.org/10.1016/j.clinbiochem.2003.11.015
Aslankoc R, Savran M, Ozmen O, Asci S (2018) Hippocampus and cerebellum damage in sepsis induced by lipopolysaccharide in aged rats - Pregabalin can prevent damage. Biomed Pharmacother 108:1384–1392. https://doi.org/10.1016/j.biopha.2018.09.162
Riedemann NC, Neff TA, Guo RF, Bernacki KD, Laudes IJ, Sarma JV, Lambris JD, Ward PA (2003) Protective effects of IL-6 blockade in sepsis are linked to reduced C5a receptor expression. J Immunol 170(1):503–507. https://doi.org/10.4049/jimmunol.170.1.503
Rosengarten B, Wolff S, Klatt S, Schermuly RT (2009) Effects of inducible nitric oxide synthase inhibition or norepinephrine on the neurovascular coupling in an endotoxic rat shock model. Crit Care 13(4):R139. https://doi.org/10.1186/cc8020
Lorente L, Martín MM, Pérez-Cejas A, González-Rivero AF, López RO, Ferreres J, Solé-Violán J, Labarta L, Díaz C, Palmero S, Jiménez A (2018) Sustained high serum caspase-3 concentrations and mortality in septic patients. Eur J Clin Microbiol Infect Dis 37(2):281–288. https://doi.org/10.1007/s10096-017-3129-y
Metukuri MR, Reddy CM, Reddy PR, Reddanna P (2010) Bacterial LPS-mediated acute inflammation-induced spermatogenic failure in rats: role of stress response proteins and mitochondrial dysfunction. Inflammation 33(4):235–243. https://doi.org/10.1007/s10753-009-9177-4
Yuan H, Huang J, Lv B, Yan W, Hu G, Wang J, Shen B (2013) Diagnosis value of the serum amyloid A test in neonatal sepsis: a meta-analysis. Biomed Res Int 2013:520294. https://doi.org/10.1155/2013/520294
Fu Y, Chen J, Cai B, Zhang JL, Li LX, Wang LL (2012) Diagnostic values of procalcitonin, interleukin-6, C reactive protein and serum amyloid A in sepsis. Sichuan Da Xue Xue Bao Yi Xue Ban 43(5):702–705
Takatani Y, Ono K, Suzuki H, Inaba M, Sawada M, Matsuda N (2018) Inducible nitric oxide synthase during the late phase of sepsis is associated with hypothermia and immune cell migration.Lab Invest 98(5):629–639. https://doi.org/10.1038/s41374-018-0021-z
Kim J, Park EY, Kim O, Schilder JM, Coffey DM, Cho CH, Bast RC Jr (2018) Cell origins of high-grade serous ovarian cancer. Cancers (Basel). https://doi.org/10.3390/cancers10110433
Acknowledgements
The authors thank the participants of this study.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
GI contributed in the literature search, project development, manuscript writing/editing, data collection and interpretation, experimental rat study, rat killing and revised the article; SM contributed in biochemical analysis, statistical analysis, rat killing; OO contributed in histopathological and immunohistochemical analyses, management data analysis, and statistical analysis.
Corresponding author
Ethics declarations
Conflict of interest
We declare that we have no conflict of interest with respect to the authorship and publication of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gunyeli, I., Saygin, M. & Ozmen, O. The impact of the sepsis on female urogenital system: the role of pregabalin. Arch Gynecol Obstet 300, 1067–1082 (2019). https://doi.org/10.1007/s00404-019-05285-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-019-05285-8