Abstract
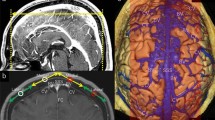
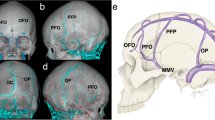
Preserving cortical frontal bridging veins draining into the superior sagittal sinus is a factor of good neurological outcome in anterior interhemispheric transcallosal approaches, classically performed to reach intraventricular tumors. Challenging the idea that veins are utterly variable, we propose a statistical analysis of 100 selective cerebral angiographies to determine where to place the craniotomy in order to expose the most probable vein-free area. The mean distance to the first pre-coronal vein was 6.66 cm (± 1.73, 1.80 to 13.00) and to the first post-coronal vein 0.94 cm (± 0.92, 0 to 3.00) (p < 0.001). The probability of absence of bridging veins was 92.0% at 4 cm anterior to the coronal suture versus 37.5% at 1 cm and 12.5% at 2 cm posteriorly. The length of the surgical corridor (distance between the first pre-coronal and post-coronal vein) was 7.60 cm (± 1.72, 3.00 to 14.10). Overall, the ideal centering point of the craniotomy was 2.86 cm (± 1.08, − 0.65 to 6.50) ahead of the coronal suture. The mean number of veins within 6 cm behind the coronal suture was 8.47 (± 2.11, from 3 to 15) versus 0.530 (± 0.82, from 0 to 3) ahead of the coronal suture (p < 0.001). These findings support a purely pre-coronal 5 cm craniotomy for interhemispheric approaches.


Similar content being viewed by others
References
Apuzzo MLJ (1993) Brain surgery: complication avoidance and management. Churchill Livingstone
Aryan HE, Ozgur BM, Jandial R, Levy ML (2006) Complications of interhemispheric transcallosal approach in children: review of 15 years experience. Clin Neurol Neurosurg 108:790–793. https://doi.org/10.1016/j.clineuro.2005.10.009
Brockmann C, Kunze SC, Schmiedek P, Groden C, Scharf J (2012) Variations of the superior sagittal sinus and bridging veins in human dissections and computed tomography venography. Clin Imaging 36:85–89. https://doi.org/10.1016/j.clinimag.2011.05.003
Greenberg MS Handbook of neurosurgery
Hassaneen W, Suki D, Salaskar AL, Levine NB, DeMonte F, Lang FF, McCutcheon IE, Dorai Z, Feiz-Erfan I, Wildrick DM, Sawaya R (2010) Immediate morbidity and mortality associated with transcallosal resection of tumors of the third ventricle. J Clin Neurosci 17:830–836. https://doi.org/10.1016/j.jocn.2009.12.007
Hernesniemi J, Romani R, Dashti R, Albayrak BS, Savolainen S, Ramsey C, Karatas A, Lehto H, Navratil O, Niemelä M (2008) Microsurgical treatment of third ventricular colloid cysts by interhemispheric far lateral transcallosal approach-experience of 134 patients. Surg Neurol 69:447–453. https://doi.org/10.1016/j.surneu.2007.11.005
McNatt SA, Sosa IJ, Krieger MD, McComb JG (2011) Incidence of venous infarction after sacrificing middle-third superior sagittal sinus cortical bridging veins in a pediatric population: clinical article. J Neurosurg Pediatr 7:224–228. https://doi.org/10.3171/2010.11.PEDS09261
Ohara K, Inoue T, Ono H, Kiyofuji S, Tamura A, Saito I (2017) Technique for rerouting a bridging vein that hinders the anterior interhemispheric approach: a technical note. Acta Neurochir (Wien) 159:1913–1918. https://doi.org/10.1007/s00701-017-3285-y
Oka K, Rhoton AL, Barry M, Rodriguez R (1985) Microsurgical anatomy of the superficial veins of the cerebrum. Neurosurgery 17:711–748. https://doi.org/10.1227/00006123-198511000-00003
Quiñones-Hinojosa A (2012) Schmidek and sweet operative neurosurgical techniques: indications, methods, and results: Sixth Edition. Elsevier Inc.
Rhoton AL, Yamamoto I, Peace DA (1981) Microsurgery of the third ventricle: Part II. Operative approaches. Neurosurgery 8:357–373. https://doi.org/10.1227/00006123-198103000-00007
Sakaki T, Kakizaki T, Takeshima T, Miyamoto K, Tsujimoto S (1995) Importance of prevention of intravenous thrombosis and preservation of the venous collateral flow in bridging vein injury during surgery: an experimental study. Surg Neurol 44:158–162. https://doi.org/10.1016/0090-3019(95)00160-3
Sampei T, Yasui N, Okudera T, Fukasawa H (1996) Anatomic study of anterior frontal cortical bridging veins with special reference to the frontopolar vein. Neurosurgery 38:971–975. https://doi.org/10.1097/00006123-199605000-00024
Sindou M (2009) Practical handbook of neurosurgery: from leading neurosurgeons. Springer-Verlag
Sindou MP, Auque J, Jouanneau E (2005) Neurosurgery and the intracranial venous system. Acta Neurochir Suppl 94:167–175. https://doi.org/10.1007/3-211-27911-3_27
Tsutsumi K, Shiokawa Y, Sakai T, Aoki N, Kubota M, Saito I (1991) Venous infarction following the interhemispheric approach in patients with acute subarachnoid hemorrhage. J Neurosurg 74:715–719. https://doi.org/10.3171/jns.1991.74.5.0715
Author information
Authors and Affiliations
Contributions
S.A. performed the analysis, drafted the manuscript, and approved the final version of the manuscript.
C.A. performed the analysis, drafted the manuscript, and approved the final version of the manuscript.
D.C. critically reviewed the manuscript and approved the final version of the manuscript.
C.L.G. critically reviewed the manuscript and approved the final version of the manuscript.
P.B. designed the study, performed the analysis, drafted the manuscript, and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval
Local committee approval.
Informed consent
Use of anonymized data, with patients’ consents
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Aldea, S., Apra, C., Chauvet, D. et al. Interhemispheric transcallosal approach: going further based on the vascular anatomy. Neurosurg Rev 44, 2831–2835 (2021). https://doi.org/10.1007/s10143-021-01480-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-021-01480-x