Abstract
Purpose
To determine the effect of human growth hormone (GH) supplementation during ovarian stimulation in women undergoing IVF/PGT-A cycles, who do not meet the Bologna criteria for poor ovarian response (POR).
Methods
This is a retrospective cohort study of 41 women with suboptimal outcomes in their first cycle of IVF/PGT-A including lower than expected number of MII oocytes, poor blastulation rate, and/or lower than expected number of euploid embryos for their age, who underwent a subsequent IVF/PGT-A cycle with the same fixed dose gonadotropin protocol and adjuvant GH treatment. Daily cotreatment with GH started with first gonadotrophin injection. The IVF cycle outcomes were compared between the control and GH cycle using the Wilcoxon-Signed Rank test.
Results
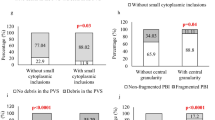
The total number of biopsied blastocysts (mean ± SD; 2.0 ± 1.6 vs 3.5 ± 3.2, p = 0.009) and euploid embryos (0.8 ± 1.0 vs 2.0 ± 2.8, p = 0.004) were significantly increased in the adjuvant GH cycle compared to the control cycle. The total number of MII oocytes also trended to be higher in the GH cycle (10.2 ± 6.3 vs 12.1 ± 8.3, p = 0.061). The overall blastulation and euploidy rate did not differ between the control and treatment cycle.
Conclusion
Our study uniquely investigated the use of adjuvant GH in IVF/PGT-A cycles in women without POR and without a priori suspicion for poor outcome based on their clinical parameters. Our study presents preliminary evidence that GH supplementation in these women is beneficial and is associated with an increased number of blastocysts for biopsy and greater number of euploid embryos for transfer.
Similar content being viewed by others
References
Homburg R, et al. Growth hormone facilitates ovulation induction by gonadotrophins. Clin Endocrinol. 1988;29(1):113–7.
Hart RJ, Rombauts L, Norman RJ. Growth hormone in IVF cycles: any hope? Curr Opin Obstet Gynecol. 2017;29(3):119–25.
Serafim MK, et al. Impact of growth hormone (GH) and follicle stimulating hormone (FSH) on in vitro canine preantral follicle development and estradiol production. Growth Hormon IGF Res. 2015;25(2):85–9.
Hull KL, Harvey S. Growth hormone and reproduction: a review of endocrine and autocrine/paracrine interactions. Int J Endocrinol. 2014;2014:234014.
Ipsa E, et al. Growth hormone and insulin-like growth factor action in reproductive tissues. Front Endocrinol (Lausanne). 2019;10:777.
Mendoza C, et al. Follicular fluid markers of oocyte developmental potential. Hum Reprod. 2002;17(4):1017–22.
Mendoza C, et al. Relationship between fertilization results after intracytoplasmic sperm injection, and intrafollicular steroid, pituitary hormone and cytokine concentrations. Hum Reprod. 1999;14(3):628–35.
Younis JS, et al. The effect of growth hormone supplementation on in vitro fertilization outcome: a prospective randomized placebo-controlled double-blind study. Fertil Steril. 1992;58(3):575–80.
Kolibianakis EM, et al. Addition of growth hormone to gonadotrophins in ovarian stimulation of poor responders treated by in-vitro fertilization: a systematic review and meta-analysis. Hum Reprod Update. 2009;15(6):613–22.
Duffy JM, et al. Growth hormone for in vitro fertilization. Cochrane Database Syst Rev. 2010;1:CD000099.
Ferraretti AP, et al. ESHRE consensus on the definition of ‘poor response’ to ovarian stimulation for in vitro fertilization: the Bologna criteria. Hum Reprod. 2011;26(7):1616–24.
Nardo LG, et al. Circulating basal anti-Müllerian hormone levels as predictor of ovarian response in women undergoing ovarian stimulation for in vitro fertilization. Fertil Steril. 2009;92(5):1586–93.
Reichman DE, Goldschlag D, Rosenwaks Z. Value of antimüllerian hormone as a prognostic indicator of in vitro fertilization outcome. Fertil Steril. 2014;101(4):1012–8.e1.
Moon KY, et al. Nomogram to predict the number of oocytes retrieved in controlled ovarian stimulation. Clin Exp Reprod Med. 2016;43(2):112–8.
Pantos K, et al. Influence of advanced age on the blastocyst development rate and pregnancy rate in assisted reproductive technology. Fertil Steril. 1999;71(6):1144–6.
Franasiak JM, et al. The nature of aneuploidy with increasing age of the female partner: a review of 15,169 consecutive trophectoderm biopsies evaluated with comprehensive chromosomal screening. Fertil Steril. 2014;101(3):656–663.e1.
Garcia-Velasco JA, et al. High doses of gonadotrophins combined with stop versus non-stop protocol of GnRH analogue administration in low responder IVF patients: a prospective, randomized, controlled trial. Hum Reprod. 2000;15(11):2292–6.
Cakmak H, et al. A novel “delayed start” protocol with gonadotropin-releasing hormone antagonist improves outcomes in poor responders. Fertil Steril. 2014;101(5):1308–14.
Ob’edkova K, et al. Growth hormone co-treatment in IVF/ICSI cycles in poor responders. Gynecol Endocrinol. 2017;33(sup1):15–7.
La Marca A, et al. Female age, serum antimüllerian hormone level, and number of oocytes affect the rate and number of euploid blastocysts in in vitro fertilization/intracytoplasmic sperm injection cycles. Fertil Steril. 2017;108(5):777–783.e2.
Polyzos NP, Sunkara SK. Sub-optimal responders following controlled ovarian stimulation: an overlooked group? Hum Reprod. 2015;30(9):2005–8.
Alvaro Mercadal B, et al. Characterization of a suboptimal IVF population and clinical outcome after two IVF cycles. Gynecol Endocrinol. 2018;34(2):125–8.
Funding
None
Funding
Not applicable
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
IRB approval was granted through the UT Austin Institutional Review Board.
Consent to participate
Not applicable
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Skillern, A., Leonard, W., Pike, J. et al. Growth hormone supplementation during ovarian stimulation improves oocyte and embryo outcomes in IVF/PGT-A cycles of women who are not poor responders. J Assist Reprod Genet 38, 1055–1060 (2021). https://doi.org/10.1007/s10815-021-02088-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-021-02088-2