Abstract
Purpose
Conventional magnetic resonance imaging (MRI) technics are insufficient in the differentiation of tumor progression from post-treatment changes in patients with treated glioblastoma. Previous studies have suggested that histogram analysis is a useful tool in the assessment of treatment response in different cancer types. The aim of the study was to to evaluate the effectiveness of MRI histogram analysis in the differentiation of tumor progression from pseudoprogression in patients with treated glioblastoma.
Methods
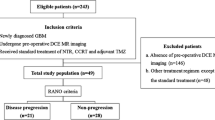
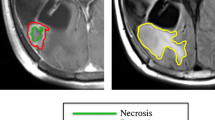
Forty-six patients with glioblastoma who newly developed enhancing lesions following chemoradiation treatment were included in this retrospective study. Histogram analysis was performed from new enhancing lesions on T1-weighted contrast-enhanced MRI. Histogram analysis findings of patients with progression (23) and pseudoprogression (23) were compared.
Results
Mean, minimum, median, maximum, standard deviation, variance, entropy, skewness, uniformity values were found to be significantly higher in progressive disease (p < 0.05). A receiver-operating characteristic (ROC) curve analysis was performed for mean value, and area under the curve (AUC) was found as 0.975. When the threshold value was selected as 528.86, two groups could be differentiated with 95.7% sensitivity and 87.0% specificity.
Conclusion
MRI histogram analysis can be used for the differentiation of progressive disease from pseudoprogression.




Similar content being viewed by others
References
Ohka F, Natsume A, Wakabayashi T (2012) Current trends in targeted therapies for glioblastoma multiforme. Neurol Res Int. 2012:878425. https://doi.org/10.1155/2012/878425
Thakkar JP, Dolecek TA, Horbinski C et al (2014) Epidemiologic and molecular prognostic review of Glioblastoma. Cancer Epidemiol Biomarkers Prev 23:1985–1985. https://doi.org/10.1158/1055-9965.EPI-14-0275
Stupp R, Hegi ME, Mason WP, van den Bent MJ, Taphoorn MJB, Janzer RC, Ludwin SK, Allgeier A, Fisher B, Belanger K, Hau P, Brandes AA, Gijtenbeek J, Marosi C, Vecht CJ, Mokhtari K, Wesseling P, Villa S, Eisenhauer E, Gorlia T, Weller M, Lacombe D, Cairncross JG, Mirimanof R-O (2009) Efects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. Lancet Oncol 10(5):459–466. https://doi.org/10.1016/S1470-2045(09)70025-7
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJB, Belanger K, Brandes AA, Marosi C, Bogdahn U, Curschmann J, Janzer RC, Ludwin SK, Gorlia T, Allgeier A, Lacombe D, Cairncross JG, Eisenhauer E, Mirimanof RO (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352(10):987–996. https://doi.org/10.1056/NEJMoa043330
Thust SC, van den Bent MJ, Smits M (2018) Pseudoprogression of brain tumors. J Magn Reson Imaging 48(3):571–589. https://doi.org/10.1002/jmri.26171
Melguizo-Gavilanes I, Bruner JM, Guha-Thakurta N, Hess KR, Puduvalli VK (2015) Characterization of pseudoprogression in patients with glioblastoma: is histology the gold standard? J Neurooncol 123(1):141–150. https://doi.org/10.1007/s11060-015-1774-5
Park YW, Han K, Ahn SS et al (2018) Whole-tumor histogram and texture analyses of DTI for evaluation of IDH1-mutation and 1p/19q-codeletion status in world health organization grade II gliomas. AJNR Am J Neuroradiol 39:693–698. https://doi.org/10.3174/ajnr.A5569
Yu H, Caldwell C, Mah K et al (2009) Automated radiation targeting in head-and-neck cancer using region-based texture analysis of PET and CT images. Int J Radiat Oncol Biol Phys 75:618–625. https://doi.org/10.1016/j.ijrobp.2009.04.043
Ganeshan B, Miles KA, Young RC, Chatwin CR (2009) Texture analysis in non-contrast enhanced CT: impact of malignancy on texture in apparently disease-free areas of the liver. Eur J Radiol 70:101–110. https://doi.org/10.1016/j.ejrad.2007.12.005
Suo ST, Zhuang ZG, Cao MQ et al (2016) Differentiation of pyogenic hepatic abscesses from malignant mimickers using multislice-based texture acquired from contrast-enhanced computed tomography. Hepatobiliary Pancreat Dis Int 15:391–398. https://doi.org/10.1016/s1499-3872(15)60031-5
Castellano G, Bonilha L, Li LM, Cendes F (2004) Texture analysis of medical images. Clin Radiol 59:1061–1069. https://doi.org/10.1016/j.crad.2004.07.008
Alic L, Niessen WJ, Veenland JF (2014) Quantification of heterogeneity as a biomarker in tumor imaging: a systematic review. PLoS ONE 9:e110300. https://doi.org/10.1371/journal.pone.0110300
Yang D, Rao G, Martinez J, Veeraraghavan A, Rao A (2015) Evaluation of tumor-derived MRI-texture features for discrimination of molecular subtypes and prediction of 12-month survival status in glioblastoma. Med Phys 42:6725–6735. https://doi.org/10.1118/1.4934373
Molina D, Perez-Beteta J, Luque B et al (2016) Tumour heterogeneity in glioblastoma assessed by MRI texture analysis: a potential marker of survival. Br J Radiol. https://doi.org/10.1259/bjr.20160242
Colombi D, Dinkel J, Weinheimer O et al (2015) Visual vs fully automatic histogram-based assessment of idiopathic pulmonary fibrosis (IPF) progression using sequential multidetector computed tomography (MDCT). PLoS ONE 10:e0130653. https://doi.org/10.1371/journal.pone.0130653
Young RJ, Gupta A, Shah AD, Graber JJ, Zhang Z, Shi W et al (2011) Potential utility of conventional MRI signs in diagnosing pseudoprogression in glioblasto-ma. Neurology 76:1918–1924. https://doi.org/10.1212/WNL.0b013e31821d74e7
Nelson DA, Tan TT, Rabson AB et al (2004) Hypoxia and defective apoptosis drive genomic instability and tumorigenesis. Genes Dev 18:2095–2107. https://doi.org/10.1101/gad.1204904
Peng SL, Chen CF, Liu HL et al (2013) Analysis of parametric histogram from dynamic contrast-enhanced MRI: application in evaluating brain tumor response to radiotherapy. NMR Biomed 26:443–450. https://doi.org/10.1002/nbm.2882
Liu Y, Zhang X, Feng N et al (2018) The effect of glioblastoma heterogeneity on survival stratification: a multimodal MR imaging texture analysis. Acta Radiol 59:1239–1246. https://doi.org/10.1177/0284185118756951
Yun TJ, Park C-K, Kim TM et al (2015) Glioblastoma treated with concurrent radiation therapy and temozolomide chemotherapy: differentiation of true progression from pseudoprogression with quantitative dynamic contrast-enhanced MR ımaging. Radiology. https://doi.org/10.1148/radiol.14132632
Ng F, Ganeshan B, Kozarski R et al (2013) Assessment of primary colorectal cancer heterogeneity by using whole-tumor texture analysis: contrast-enhanced CT texture as a biomarker of 5-year survival. Radiology 266:177–184. https://doi.org/10.1148/radiol.12120254
Law M, Young R, Babb J, et al (2007) Histogram analysis versus region of interest analysis of dynamic susceptibility contrast perfusion MR imaging data in the grading of cerebral gliomas. AJNR Am J Neuroradiol 28:761–66. http://www.ajnr.org/content/28/4/761.full
Beig N, Patel J, Prasanna P et al (2017) Radiogenomic analysis of hypoxia pathway reveals computerized MRI descriptors predictive of overall survival in glioblastoma. Med Imag. https://doi.org/10.1117/12.2255694
Kurtul N, Baykara M (2018) The association between MRI texture analysis and chemoradiotherapy outcomes in glioblastoma cases. Ann Med Res 25(4):1. https://doi.org/10.5455/annalsmedres.2018.09.191
Cao Y, Tsien CI, Nagesh V, Junck L, Ten Haken R, Ross BD et al (2006) Survival prediction in high-grade gliomas by MRI perfusion before and during early stage of RT. Int J Radiat Oncol Biol Phys 64:876–885. https://doi.org/10.1016/j.ijrobp.2005.09.001
Kong DS, Kim ST, Kim EH et al (2011) Diagnostic dilemma of pseudoprogression in the treatment of newly diagnosed glioblastomas: the role of assessing relative cerebral blood flow volume and oxygen-6-methylguanine-DNA methyltransferase promoter methylation status. AJNR Am J Neuroradiol 32:382–387. https://doi.org/10.3174/ajnr.A2286
Kim HS, Kim JH, Kim SH et al (2010) Posttreatment high-grade glioma: usefulness of peak height position with semiquantitative MR perfusion histogram analysis in an entire contrast-enhanced lesion for predicting volume fraction of recurrence. Radiology 256:906–915. https://doi.org/10.1148/radiol.10091461
Yoshii Y (2008) Pathological review of late cerebral radionecrosis. Brain Tumor Pathol 25:51–58. https://doi.org/10.1007/s10014-008-0233-9
Baek HJ, Kim HS, Kim N et al (2012) Percent change of perfusion skewness and kurtosis: a potential imaging biomarker for early treatment response in patients with newly diagnosed glioblastomas. Radiology 264:834–843. https://doi.org/10.1148/radiol.12112120
Chu HH, Choi SH, Ryoo I et al (2015) Differentiation of true progression from pseudoprogression in glioblastoma treated with radiation therapy and concomitant temozolomide: comparison study of standard and high-b-value diffusion-weighted ımaging. Radiology. https://doi.org/10.1148/radiol.13122024
Cha J, Kim ST, Kim H-J et al (2014) Differentiation of tumor progression from pseudoprogression in patients with posttreatment glioblastoma using multiparametric histogram analysis. AJNR Am J Neuroradiol 35(7):1309–1317. https://doi.org/10.3174/ajnr.A3876
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no confict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yildirim, M., Baykara, M. Differentiation of progressive disease from pseudoprogression using MRI histogram analysis in patients with treated glioblastoma. Acta Neurol Belg 122, 363–368 (2022). https://doi.org/10.1007/s13760-021-01607-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13760-021-01607-3