Abstract
Background
Using the Faroese Septuagenarian cohort, we aimed to describe the incidence of dementia and assess the validity of neurocognitive tests to predict subsequent dementia diagnosis.
Methods
In this population-based cohort, 713 Faroese septuagenarians aged 70–74 years without dementia, underwent clinical and neuropsychological examinations. After 10-years of follow-up, information was collected on all participants referred for cognitive evaluations and diagnosed with dementia. Incidence rates were calculated and presented with 95% confidence intervals (CIs), assuming a Poisson distribution. We then performed discriminant analysis to determine the best set of neuropsychological tests to identify those who would develop dementia.
Results
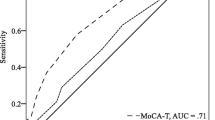
Over the 10-years, 65 participants (9.1%) were diagnosed with dementia, with a 10-year incidence rate of 1063 cases per 100,000 person years (95% CI 825, 1343). Women had a greater incidence than men (incidence rate ratio (IRR) = 1.58; 95% CI 0.93, 2.71). After stepwise selection, gender and six neuropsychological measures were selected to discriminate between those who would and would not develop dementia. Overall, the model was able to correctly identify 82% of those who would not develop dementia (specificity) and 71% of those who would (sensitivity).
Conclusions
These results indicate that among a greater number of tests covering a broad range of cognitive abilities, tests reflecting verbal and visual learning and recall, visuospatial function, attention, and encoding into and retrieval from long-term memory may be helpful in identifying patients in the pre-symptomatic phase of dementia. Thus, helping care-givers identify patients at a higher risk of developing dementia and adjusting management of care accordingly.

Similar content being viewed by others

References
Wu Y-T, Fratiglioni L, Matthews FE et al (2016) Dementia in western Europe: epidemiological evidence and implications for policy making. Lancet Neurol 15:116–124
Shah H, Albanese E, Duggan C et al (2016) Research priorities to reduce the global burden of dementia by 2025. Lancet Neurol 15:1285–1294
Prince M, Bryce R, Albanese E (2013) The global prevalence of dementia: a systematic review and metaanalysis. Alzheimer’s Dement 9:63–75
Guerchet M, Prina M, Prince M (2013) Policy brief for heads of government: the global impact of dementia 2013–2050. Policy Br Heads Gov Glob Impact Dement 2013–2050 Publ by Alzheimer’s Dis Int (ADI), London December 2013. 1–8.
Sposato LA, Kapral MK, Fang J et al (2015) Declining incidence of stroke and dementia: coincidence or prevention opportunity? JAMA Neurol 72:1529
Ahmadi-Abhari S, Guzman-Castillo M, Bandosz P et al (2017) Temporal trend in dementia incidence since 2002 and projections for prevalence in England and Wales to 2040: modelling study. BMJ. https://doi.org/10.1136/bmj.j2856
Grasset L, Brayne C, Joly P et al (2016) Trends in dementia incidence: evolution over a 10-year period in France. Alzheimer’s Dement 12:272–280
Prince M, Ali GC, Guerchet M (2016) Recent global trends in the prevalence and incidence of dementia, and survival with dementia. Alzheimer’s Res Ther. https://doi.org/10.1186/s13195-016-0188-8
Kivipelto M, Mangialasche F, Ngandu T (2018) Lifestyle interventions to prevent cognitive impairment, dementia and Alzheimer disease. Nat Rev Neurol 14:653–666
Norton S, Matthews FE, Barnes DE (2014) Potential for primary prevention of Alzheimer’s disease: an analysis of population-based data. Lancet Neurol 13:788–794
Santos CY, Snyder PJ, Wu WC (2017) Pathophysiologic relationship between Alzheimer’s disease, cerebrovascular disease, and cardiovascular risk: a review and synthesis. Alzheimer’s Dement. https://doi.org/10.1016/j.dadm.2017.01.005
Bratzke-Bauer LC, Pozehl BJ, Paul SM et al (2013) Neuropsychological patterns differ by type of left ventricle dysfunction in heart failure. Arch Clin Neuropsychol. https://doi.org/10.1093/arclin/acs101
Ylikoski R, Ylikoski A, Raininko R et al (2000) Cardiovascular diseases, health status, brain imaging findings and neuropsychological functioning in neurologically healthy elderly individuals. Arch Gerontol Geriatr. https://doi.org/10.1016/S0167-4943(00)00045-5
Verma M, Howard RJ (2012) Semantic memory and language dysfunction in early Alzheimer’s disease: a review. Int J Geriatr Psychiatry 27:1209–1217
Petersen MS, Debes F, Grandjean P, Weihe P (2019) Gender differences in cognitive performance and health status in the Faroese Septuagenarians cohort. Eur J Public Health. 29(1):79–81
Choi AL, Weihe P, Budtz-Jørgensen E et al (2009) Methylmercury exposure and adverse cardiovascular effects in Faroese Whaling men. Environ Health Perspect. https://doi.org/10.1289/ehp.11608
Salonen JT, Seppänen K, Lakka TA et al (2000) Mercury accumulation and accelerated progression of carotid atherosclerosis: a population-based prospective 4-year follow-up study in men in eastern Finland. Atherosclerosis. https://doi.org/10.1016/S0021-9150(99)00272-5
Petersen MS, Restorff M, Stórá T et al (2019) Trend in the incidence and prevalence of dementia in the Faroe Islands. J Alzheimer’s Dis. https://doi.org/10.3233/JAD-190341
Fernandez G (2002) Discriminant analysis, a powerful classification technique in data mining. Proceedings of the SAS Users International Conference, pp 247–56
SAS (2011) SAS/STAT 9.3. SAS Inst Inc, Cary, NC, 8640
Niu H, Álvarez-Álvarez I, Guillén-Grima F et al (2017) Prevalence and incidence of Alzheimer’s disease in Europe: a meta-analysis. Neurologia (English Ed). https://doi.org/10.1016/j.nrleng.2016.02.009
Van Cauwenberghe C, Van Broeckhoven C, Sleegers K (2016) The genetic landscape of Alzheimer disease: clinical implications and perspectives. Genet Med 18:421–430
Bondi MW, Jak AJ, Delano-Wood L et al (2008) Neuropsychological contributions to the early identification of Alzheimer’s disease. Neuropsychol Rev 18:73–90
Weintraub S, Wicklund AH, Salmon DP (2012) The neuropsychological profile of Alzheimer disease. Cold Spring Harb Perspect Med. https://doi.org/10.1101/cshperspect.a006171
Bastin C, Salmon E (2014) Early neuropsychological detection of Alzheimer’s disease. Eur J Clin Nutr 68:1192–1199
Belleville S, Fouquet C, Hudon C et al (2017) Neuropsychological measures that predict progression from mild cognitive impairment to Alzheimer’s type dementia in older adults: a systematic review and meta-analysis. Neuropsychol Rev 27:328–353
Buschke H (1973) Selective reminding for analysis of memory and learning. J Verbal Learn Verbal Behav 12:543–550
Buschke H, Fuld PA (1974) Evaluating storage, retention, and retrieval in disordered memory and learning. Neurology 24:1019–1019
Spreen O, Strauss EA (1998) A Compendium of neuropsychological Tests, 2nd edn. Oxford University Press, New York
Kaplan E, Goodglass H, Weintraub S (1983) The Boston naming test. Lea Febiger, Philadelphia
Williams BW, Mack W, Henderson VW (1989) Boston naming test in Alzheimer’s disease. Neuropsychologia 27:1073–1079
Katsumata Y, Mathews M, Abner EL et al (2015) Assessing the discriminant ability, reliability, and comparability of multiple short forms of the boston naming test in an Alzheimer’s disease center cohort. Dement Geriatr Cogn Disord 39:215–227
Raven J, Raven JC, Court J (1998) Manual for Raven’s progressive matrices and vocabulary scales. Cogn Psychol. https://doi.org/10.1006/cogp.1999.0735
Ambra FI, Iavarone A, Ronga B et al (2016) Qualitative patterns at Raven’s colored progressive matrices in mild cognitive impairment and Alzheimer’s disease. Aging Clin Exp Res 28:561–565
Chen P, Ratcliff G, Belle SH et al (2000) Cognitive tests that best discriminate between presymptomatic AD and those who remain nondemented. Neurology. https://doi.org/10.1212/WNL.55.12.1847
Roebuck-Spencer TM, Glen T, Puente AE et al (2017) Cognitive screening tests versus comprehensive neuropsychological test batteries: a national academy of neuropsychology education paper. Arch Clin Neuropsychol. https://doi.org/10.1093/arclin/acx021
Reul S, Lohmann H, Wiendl H et al (2017) Can cognitive assessment really discriminate early stages of Alzheimer’s and behavioural variant frontotemporal dementia at initial clinical presentation? Alzheimer’s Res Ther. https://doi.org/10.1186/s13195-017-0287-1
Acknowledgements
We would like to thank Arni Ludvig psychologist and Hildigunn Steinhólm, research coordinator for their contribution at the baseline examinations.
Funding
The study was supported by the Faroese Research Council, National Institute of Health (Grant Numbers ES013692 & F32ES028087) and the European Commission Sixth Framework Programme for RTD (Grant Number FOOD-CT-2006-016253, PHIME).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they do not have any conflict of interest.
Research involving human participants and/or animals
Yes, human subjects. All procedures have been approved by the Faroese Ethical Committee.
Informed consent
Informed consent was obtained from all study participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Paul, K.C., Debes, F., Eliasen, E. et al. Incidence, gender influence, and neuropsychological predictors of all cause dementia in the Faroe Islands—the Faroese Septuagenarian cohort. Aging Clin Exp Res 33, 105–114 (2021). https://doi.org/10.1007/s40520-020-01520-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-020-01520-4