Abstract
Objectives
Knowledge about self-perceived health can help us understand the health status and needs among migrants and ethnic minorities in the European Union (EU) which is essential to improve equity and integration. The objective was to examine and compare self-perceived health among migrant and ethnic minority groups in the EU countries.
Methods
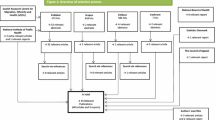
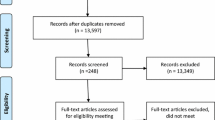
Publications were ascertained by a systematic search of PUBMED and EMBASE. Eligibility of studies was based on the abstracts and the full texts. Additional articles were identified via the references. The final number of studies included was 17.
Results
Publications were identified in 5 out of the 27 EU countries. In regard to self-perceived health, most migrants and ethnic minority groups appeared to be disadvantaged as compared to the majority population even after controlling for age, gender, and socioeconomic factors. Only limited cross-country comparisons could be carried out, still they revealed a parallel pattern of self-perceived health among similar migrant/ethnic minority groups.
Conclusions
Policies to improve social and health status, contextual factors, and access to healthcare among migrants and ethnic minorities are essential to reduce ethnic inequalities in health.

Similar content being viewed by others
References
Agyemang C, Denktas S, Bruijnzeels M, Foets M (2006) Validity of the single-item question on self-rated health status in first generation Turkish and Moroccans versus native Dutch in the Netherlands. Pub Health 120:543–550
Bhopal R (2004) Glossary of terms relating to ethnicity and race: for reflection and debate. J Epidemiol Community Health 58:441–445
Borrell C, Muntaner C, Sola J, Artazcoz L, Puigpinos R, Benach J, Noh S (2008) Immigration and self-reported health status by social class and gender: the importance of material deprivation, work organisation and household labour. J Epidemiol Community Health 62:e7
Bos V, Kunst AE, Keij-Deerenberg IM, Garssen J, Mackenbach JP (2004) Ethnic inequalities in age- and cause-specific mortality in the Netherlands. Int J Epidemiol 33:1112–1119
Burstrom B, Fredlund P (2001) Self-rated health: is it as good a predictor of subsequent mortality among adults in lower as well as in higher social classes? J Epidemiol Community Health 55:836–840
Cagney KA, Browning CR, Wen M (2005) Racial disparities in self-rated health at older ages: what differences does the neighborhood make? J Gerontol B Psychol Sci Soc Sci 60:S181–S190
Chandola T (2001) Ethnic and class differences in health in relation to British South Asians: using the new National Statistics Socio-Economic Classification. Soc Sci Med 52:1285–1296
Chandola T, Jenkinson C (2000) Validating self-rated health in different ethnic groups. Ethn Health 5:151–159
Cooper H (2002) Investigating socio-economic explanations for gender and ethnic inequalities in health. Soc Sci Med 54:693–706
Desesquelles AF, Egidi V, Salvatore MA (2009) Why do Italian people rate their health worse than French people do? An exploration of cross-country differentials of self-rated health. Soc Sci Med 68:1124–1128
European Community Health Indicators Monitoring (2008) Self-perceived health—definition of indicator
Fang J, Madhavan S, Alderman MH (1996) The association between birthplace and mortality from cardiovascular causes among black and white residents of New York City. N Engl J Med 335:1545–1551
Fylkesnes K (1993) Determinants of health care utilization—visits and referrals. Scand J Soc Med 21:40–50
Hjern A, Haglund B, Persson G, Rosen M (2001) Is there equity in access to health services for ethnic minorities in Sweden? Eur J Pub Health 11:147–152
Idler EL, Benyamini Y (1997) Self-rated health and mortality: a review of twenty-seven community studies. J Health Soc Behav 38:21–37
Iglesias E, Robertson E, Johansson SE, Engfeldt P, Sundquist J (2003) Women, international migration and self-reported health. A population-based study of women of reproductive age. Soc Sci Med 56:111–124
Jurges H (2007) True health vs response styles: exploring cross-country differences in self-reported health. Health Econ 16:163–178
Jylha M, Guralnik JM, Ferrucci L, Jokela J, Heikkinen E (1998) Is self-rated health comparable across cultures and genders? J Gerontol B Psychol Sci Soc Sci 53:S144–S152
Kaplan GA, Goldberg DE, Everson SA, Cohen RD, Salonen R, Tuomilehto J, Salonen J (1996) Perceived health status and morbidity and mortality: evidence from the Kuopio ischaemic heart disease risk factor study. Int J Epidemiol 25:259–265
Konig HH, Bernert S, Angermeyer MC, Matschinger H, Martinez M, Vilagut G, Haro JM, de Girolamo G, de Graaf G, Kovess V, Alonso J (2009) Comparison of population health status in six European countries: results of a representative survey using the EQ-5D questionnaire. Med Care 47:255–261
Koochek A, Montazeri A, Johansson SE, Sundquist J (2007) Health-related quality of life and migration: a cross-sectional study on elderly Iranians in Sweden. Health Qual Life Outcomes 5:60
Leao TS, Sundquist J, Johansson SE, Sundquist K (2009) The influence of age at migration and length of residence on self-rated health among Swedish immigrants: a cross-sectional study. Ethn Health 14:93–105
Lindstrom M, Sundquist J, Ostergren PO (2001) Ethnic differences in self-reported health in Malmo in southern Sweden. J Epidemiol Community Health 55:97–103
Lorant V, Van OH, Thomas I (2008) Contextual factors and immigrants’ health status: double jeopardy. Health Place 14:678–692
MEHO (2009) Migrant and Ethnic Minority Health Observatory. http://www.meho.eu.com
Mohseni M, Lindstrom M (2008) Ethnic differences in anticipated discrimination, generalised trust in other people and self-rated health: a population-based study in Sweden. Ethn Health 13:417–434
Padilla B, Miguel JP (2007) Health and migration in the EU: building a shared vision for action. Lisbon
Pudaric S, Sundquist J, Johansson SE (2003) Country of birth, instrumental activities of daily living, self-rated health and mortality: a Swedish population-based survey of people aged 55–74. Soc Sci Med 56:2493–2503
Robertson E, Iglesias E, Johansson SE, Sundquist J (2003) Migration status and limiting long-standing illness: a longitudinal study of women of childbearing age in Sweden. Eur J Pub Health 13:99–104
Singhammer J (2008) Ethnic minorities’ health. The Partnership, Region Midtjylland, pp 30–43
Stirbu I, Kunst AE, Bos V, Mackenbach JP (2006) Differences in avoidable mortality between migrants and the native Dutch in The Netherlands. BMC Pub Health 6:78
Stronks K, Ravelli AC, Reijneveld SA (2001) Immigrants in the Netherlands: equal access for equal needs? J Epidemiol Community Health 55:701–707
Sungurova Y, Johansson SE, Sundquist J (2006) East-west health divide and east-west migration: self-reported health of immigrants from Eastern Europe and the former Soviet Union in Sweden. Scand J Pub Health 34:217–221
Taloyan M, Johansson LM, Johansson SE, Sundquist J, Kocturk TO (2006) Poor self-reported health and sleeping difficulties among Kurdish immigrant men in Sweden. Transcult Psychiatry 43:445–461
Taloyan M, Johansson SE, Sundquist J, Kocturk TO, Johansson LM (2008) Psychological distress among Kurdish immigrants in Sweden. Scand J Pub Health 36:190–196
United Nations (2009) World Migrant Stock: The 2005 Revision Population Database
Villadsen SF, Mortensen LH, Andersen AM (2009) Ethnic disparity in stillbirth and infant mortality in Denmark 1981–2003. J Epidemiol Community Health 63:106–112
Wiking E, Johansson SE, Sundquist J (2004) Ethnicity, acculturation, and self-reported health. A population based study among immigrants from Poland, Turkey, and Iran in Sweden. J Epidemiol Community Health 58:574–582
Wild S, McKeigue P (1997) Cross sectional analysis of mortality by country of birth in England and Wales, 1970–92. BMJ 314:705–710
World Health Organisation (1946) WHO Constitution. http://www.who.int/governance/eb/constitution/en/index/html
Acknowledgments
This paper is a product of the EU-funded project Migrant and Ethnic Minority Health Observatory (MEHO) (http://www.meho.eu.com) from the work package “Healthcare utilization and self-perceived health”. Therefore, we would like to thank the project leader Marleen Foets, co-project leader Gerrit Koopmanns, and former leader Semiha Denktas (Erasmus Medical Centre, The Netherlands). Thanks also to Laura Cacciani, Emanuela Forcella, and Aldo Rosano (Agenzia di Sanità Pubblica della Regiona Lazio, Italy) for preparing a general survey for identification of registers and surveys in Europe. Also thanks to the other participants in the MEHO-project: Anton Kunst (University of Amsterdam), Johan Mackenbach and Irina Stirbu (Eramus Medical Centre, The Netherlands), Raj Bhopal and Snorri Bjorn Rafnsson (University of Edinburgh, Scotland), Oliver Razum, Jacob Spallek, and Anna Reeske (University of Bielefeld, Germany), Alexander Krämer, Manas Akmatov (University of Bielefeld, Germany), Kvetoslava Rimarova (University of Slovenia), and Dineke Zeegers (EUPHA).
Conflict of interest statement
The authors declare that they have no competing interests.
Author information
Authors and Affiliations
Corresponding author
Additional information
This paper belongs to the special issue “Health of ethnic minorities in Europe”.
Rights and permissions
About this article
Cite this article
Nielsen, S.S., Krasnik, A. Poorer self-perceived health among migrants and ethnic minorities versus the majority population in Europe: a systematic review. Int J Public Health 55, 357–371 (2010). https://doi.org/10.1007/s00038-010-0145-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00038-010-0145-4