Abstract
Purpose
The aim of this article is to present high-resolution magnetic resonance imaging (HR-MRI) findings of chronic stage spontaneous and unruptured intracranial artery dissection (ICAD).
Material and Methods
From March 2012 to April 2016 a total of 29 patients (15 male and14 female, age range 37–68 years) with chronic stage spontaneous and unruptured ICAD (vertebral artery 27, posterior inferior cerebellar artery 1 and middle cerebral artery 1) were retrospectively enrolled. Patients underwent HR-MRI more than 2 months (median interval 564 days, range 69–391 days) after symptom onset and were diagnosed at symptom onset or at the first imaging acquisition, which included luminal angiography and/or HR-MRI with clinical information. The HR-MRI findings were evaluated against those of luminal angiography on the basis of the lumen wall morphology, including thickening, contrast enhancement and residual dissection.
Results
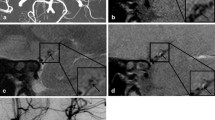
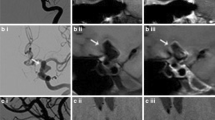
The HR-MRI findings were classified into complete normalization (normal lumen and wall with or without mild enhancement, n = 6), complete normalization with minimal wall changes (focal wall thickening with enhancement but normal luminal angiography, n = 8), incomplete normalization (focal wall thickening with enhancement with dilatation and stenosis on luminal angiography, n = 4), dissecting aneurysm (fusiform aneurysm with residual dissection findings, n = 8) and occlusion (small outer arterial diameter with diffuse contrast enhancement, n = 3).
Conclusion
The use of HR-MRI can demonstrate the distinguishing morphological features of chronic stage of spontaneous and unruptured ICAD as complete normalization, complete normalization with minimal wall changes, incomplete normalization, dissecting aneurysm and occlusion.







Similar content being viewed by others
References
Kim BM, Kim SH, Kim DI, Shin YS, Suh SH, Kim DJ, Park SI, Park KY, Ahn SS. Outcomes and prognostic factors of intracranial unruptured vertebrobasilar artery dissection. Neurology. 2011;76(20):1735–41.
Kim TW, Choi HS, Koo J, Jung SL, Ahn KJ, Kim BS, Shin YS, Lee KS. Intramural hematoma detection by susceptibility-weighted imaging in intracranial vertebral artery dissection. Cerebrovasc Dis. 2013;36(4):292–8.
Huang YC, Chen YF, Wang YH, Tu YK, Jeng JS, Liu HM. Cervicocranial arterial dissection: experience of 73 patients in a single center. Surg Neurol. 2009;72(Suppl 2):20–7, discussion S27
Takano K, Yamashita S, Takemoto K, Inoue T, Kuwabara Y, Yoshimitsu K. MRI of intracranial vertebral artery dissection: evaluation of intramural haematoma using a black blood, variable-flip-angle 3D turbo spin-echo sequence. Neuroradiology. 2013;55(7):845–51.
Mohan IV. Current optimal assessment and management of carotid and vertebral spontaneous and traumatic dissection. Angiology. 2014;65(4):274–83.
Naggara O, Louillet F, Touzé E, Roy D, Leclerc X, Mas JL, Pruvo JP, Meder JF, Oppenheim C. Added value of high-resolution MR imaging in the diagnosis of vertebral artery dissection. AJNR Am J Neuroradiol. 2010;31(9):1707–12.
Han M, Rim NJ, Lee JS, Kim SY, Choi JW. Feasibility of high-resolution MR imaging for the diagnosis of intracranial vertebrobasilar artery dissection. Eur Radiol. 2014;24(12):3017-24.
Wang Y, Lou X, Li Y, Sui B, Sun S, Li C, Jiang P, Siddiqui A, Yang X. Imaging investigation of intracranial arterial dissecting aneurysms by using 3 T high-resolution MRI and DSA: from the interventional neuroradiologists’ view. Acta Neurochir (Wien). 2014;156(3):515–25.
Arauz A, Márquez JM, Artigas C, Balderrama J, Orrego H. Recanalization of vertebral artery dissection. Stroke. 2010;41(4):717–21.
Mizutani T. Natural course of intracranial arterial dissections. J Neurosurg. 2011;114(4):1037–44.
Ono H, Nakatomi H, Tsutsumi K, Inoue T, Teraoka A, Yoshimoto Y, Ide T, Kitanaka C, Ueki K, Imai H, Saito N. Symptomatic recurrence of intracranial arterial dissections: follow-up study of 143 consecutive cases and pathological investigation. Stroke. 2013;44(1):126–31.
Krings T, Choi IS. The many faces of intracranial arterial dissections. Interv Neuroradiol. 2010;16(2):151–60.
Day AL, Gaposchkin CG, Yu CJ, Rivet DJ, Dacey RG Jr.. Spontaneous fusiform middle cerebral artery aneurysms: characteristics and a proposed mechanism of formation. J Neurosurg. 2003;99(2):228–40.
Ahn SS, Kim BM, Suh SH, Kim DJ, Kim DI, Shin YS, Ha SY, Kwon YS. Spontaneous symptomatic intracranial vertebrobasilar dissection: initial and follow-up imaging findings. Radiology. 2012;264(1):196–202.
Park KJ, Jung SC, Kim HS, Choi CG, Kim SJ, Lee DH, Suh DC, Kwon SU, Kang DW, Kim JS. Multi-contrast high-resolution magnetic resonance findings of spontaneous and unruptured intracranial vertebral artery dissection: qualitative and quantitative analysis according to stages. Cerebrovasc Dis. 2016;42(1–2):23–31.
Yoon W, Seo JJ, Kim TS, Do HM, Jayaraman MV, Marks MP. Dissection of the V4 segment of the vertebral artery: clinicoradiologic manifestations and endovascular treatment. Eur Radiol. 2007;17(4):983–93.
Sikkema T, Uyttenboogaart M, Eshghi O, de Keyser J, Brouns R, van Dijk JM, Luijckx GJ. Intracranial artery dissection. Eur J Neurol. 2014;21(6):820–6.
Habs M, Pfefferkorn T, Cyran CC, Grimm J, Rominger A, Hacker M, Opherk C, Reiser MF, Nikolaou K, Saam T. Age determination of vessel wall hematoma in spontaneous cervical artery dissection: a multi-sequence 3 T cardiovascular magnetic resonance study. J Cardiovasc Magn Reson. 2011;13:76.
Mizutani T, Miki Y, Kojima H, Suzuki H. Proposed classification of nonatherosclerotic cerebral fusiform and dissecting aneurysms. Neurosurgery. 1999;45(2):253–9, discussion 9–60.
Saliou G, Sacho RH, Power S, Kostynskyy A, Willinsky RA, Tymianski M, terBrugge KG, Rawal S, Krings T. Natural history and management of basilar trunk artery aneurysms. Stroke. 2015;46(4):948–53.
Kim SM, Ryu CW, Jahng GH, Kim EJ, Choi WS. Two different morphologies of chronic unilateral middle cerebral artery occlusion: evaluation using high-resolution MRI. J Neuroimaging. 2014;24(5):460–6.
Kim YJ, Lee DH, Kwon JY, Kang DW, Suh DC, Kim JS, Kwon SU. High resolution MRI difference between moyamoya disease and intracranial atherosclerosis. Eur J Neurol. 2013;20(9):1311–8.
Ryoo S, Cha J, Kim SJ, Choi JW, Ki CS, Kim KH, Jeon P, Kim JS, Hong SC, Bang OY. High-resolution magnetic resonance wall imaging findings of Moyamoya disease. Stroke. 2014;45(8):2457–60.
Yuan M, Liu ZQ, Wang ZQ, Li B, Xu LJ, Xiao XL. High-resolution MR imaging of the arterial wall in moyamoya disease. Neurosci Lett. 2015;584:77–82.
Acknowledgements
This study was supported by a grant from the Korea Healthcare Technology R&D Project, Ministry for Health, Welfare & Family Affairs, Republic of Korea (HI12C1847). The authors gratefully acknowledge technical support from Biomedical Imaging Infrastructure, Department of Radiology, Asan Medical Center.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interests
S.C. Jung, H.S. Kim, C.-G. Choi, S.J. Kim, S.U. Kwon, D.-W. Kang and J.S. Kim declare that they have no competing interests. This study was supported by a grant from the Korea Healthcare Technology R&D Project, Ministry for Health, Welfare & Family Affairs, Republic of Korea (HI12C1847).
This retrospective study was approved by our institutional review board and informed consent was waived. Patient information was anonymized and de-identified before making the assessments.
Rights and permissions
About this article
Cite this article
Jung, S.C., Kim, H.S., Choi, CG. et al. Spontaneous and Unruptured Chronic Intracranial Artery Dissection. Clin Neuroradiol 28, 171–181 (2018). https://doi.org/10.1007/s00062-016-0544-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00062-016-0544-x