Abstract
Aims/hypothesis
Glucagon-like peptide-1 (GLP-1) has various extra-pancreatic actions, in addition to its enhancement of insulin secretion from pancreatic beta cells. The GLP-1 receptor is produced in kidney tissue. However, the direct effect of GLP-1 on diabetic nephropathy remains unclear. Here we demonstrate that a GLP-1 receptor agonist, exendin-4, exerts renoprotective effects through its anti-inflammatory action via the GLP-1 receptor without lowering blood glucose.
Methods
We administered exendin-4 at 10 μg/kg body weight daily for 8 weeks to a streptozotocin-induced rat model of type 1 diabetes and evaluated their urinary albumin excretion, metabolic data, histology and morphometry. We also examined the direct effects of exendin-4 on glomerular endothelial cells and macrophages in vitro.
Results
Exendin-4 ameliorated albuminuria, glomerular hyperfiltration, glomerular hypertrophy and mesangial matrix expansion in the diabetic rats without changing blood pressure or body weight. Exendin-4 also prevented macrophage infiltration, and decreased protein levels of intercellular adhesion molecule-1 (ICAM-1) and type IV collagen, as well as decreasing oxidative stress and nuclear factor-κB activation in kidney tissue. In addition, we found that the GLP-1 receptor was produced on monocytes/macrophages and glomerular endothelial cells. We demonstrated that in vitro exendin-4 acted directly on the GLP-1 receptor, and attenuated release of pro-inflammatory cytokines from macrophages and ICAM-1 production on glomerular endothelial cells.
Conclusions/interpretation
These results indicate that GLP-1 receptor agonists may prevent disease progression in the early stage of diabetic nephropathy through direct effects on the GLP-1 receptor in kidney tissue.
Similar content being viewed by others
Introduction
The number of patients with diabetes is increasing dramatically throughout the world, while diabetic nephropathy is the leading cause of end-stage renal disease in developed countries. In addition, chronic kidney disease contributes to development of cardiovascular disease and leads to an increase in all-cause mortality rates [1, 2]. Therefore, prevention of renal insufficiency improves the prognosis of diabetic patients.
Numerous factors contribute to the development of diabetic nephropathy, such as glomerular hyperfiltration [3], which is mainly observed in early-stage nephropathy, oxidative stress [4], accumulation of AGEs [5], activation of protein kinase C [6], acceleration of the polyol pathway and overexpression of TGF-β [7]. Accumulating evidence also points to the critical role of the inflammatory process in the development of diabetic vascular complications, suggesting that microinflammation is a common mechanism in pathogenesis of diabetic nephropathy [8, 9]. Furuta et al. [10] reported that infiltration of mononuclear cells was prominent in the glomeruli of patients with diabetic nephropathy. Our group has also reported similar results, as well as observing an increase in the production of cell adhesion molecules in the kidney of diabetic patients [11]. We found that intercellular adhesion molecule-1 (ICAM-1) played a key role in promoting macrophage infiltration in glomeruli from a rat model of diabetes [12], and using mice deficient in ICAM-1, we also showed that blockade of ICAM-1 activation ameliorated diabetic nephropathy [13]. Additionally, we showed that methotrexate, an immunosuppressant, ameliorated diabetic nephropathy and that anti-inflammatory agents also had a beneficial effect on diabetic nephropathy [14]. Modulation of the inflammatory process prevents renal injury in animal models of diabetes, suggesting that microinflammation is a potential therapeutic target in diabetic nephropathy [14–17].
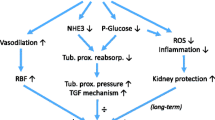
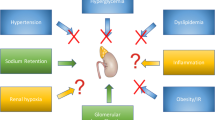
Glucagon-like peptide-1 (GLP-1) is a gut incretin hormone and currently considered an attractive agent for treatment of type 2 diabetes. It has various beneficial effects on pancreatic beta cells, such as enhancement of glucose-dependent insulin secretion [18], acceleration of beta cell proliferation and inhibition of beta cell apoptosis [19]. In the gut and hypothalamus, GLP-1 inhibits motility, gastric emptying [20] and central regulation of feeding [21], resulting in body weight loss [18]. However, native GLP-1 is rapidly degraded in the circulation by dipeptidylpeptidase-IV [22]. Today, dipeptidylpeptidase-IV-resistant, long-acting GLP-1 receptor (GLP-1R) agonists such as exendin-4 and liraglutide are available for type 2 diabetic patients. Previous reports have shown that GLP-1R is produced not only in the pancreas, gut and hypothalamus, but also in the kidney [23–25]. With respect to the effects of GLP-1 on the kidney, it has been reported that exendin-4 ameliorated hypertension by regulating sodium excretion in tubular cells [26] and attenuated renal injury by improving metabolic anomalies in a mouse model of type 2 diabetes [25]. From these results, the amelioration of hypertension and metabolic anomalies by GLP-1 would seem to have a beneficial effect on diabetic nephropathy. In the present study, we focused on the direct effect of GLP-1 through GLP-1R in the kidney, independently of the numerous other effects of GLP-1, including its glucose-lowering action.
Methods
Animals
Male Sprague–Dawley rats (5 weeks old; Charles River, Yokohama, Japan) were divided into the following groups: (1) non-diabetes (n = 5); (2) non-diabetes treated with exendin-4 (n = 6); (3) diabetes (n = 6); and (4) diabetes treated with exendin-4 (n = 6). At the age of 5 weeks, the groups allocated to be made diabetic received intravenous injections of streptozotocin (Sigma-Aldrich, St Louis, MO, USA) at 65 mg/kg body weight in citrate buffer (pH 4.5). We included only rats with blood glucose concentrations >16 mmol/l at 3 and 7 days after streptozotocin injection in the diabetes groups. The non-diabetic groups received injections of citrate buffer alone. The two groups treated with exendin-4 were given exendin-4 (Bachem, Bubendorf, Switzerland) intraperitoneally at 10 μg/kg body weight daily for 8 weeks, starting at 1 week after the streptozotocin or citrate buffer injections. The placebo groups were given water alone using the same schedule as in the exendin-4 treatment groups. All rats had free access to standard chow and tap water. All procedures were performed according to the Guidelines for Animal Experiments at Okayama University Medical School, the Japanese Government Animal Protection and Management Law and the Japanese Government Notification on Feeding and Safekeeping of Animals. All rats were killed at 9 weeks after induction of diabetes in the diabetes groups, and the kidneys were weighed and fixed in 10% (vol./vol.) formalin, or frozen in acetone cooled on dry ice.
Metabolic variables
Systolic BP was measured by tail-cuff plethysmography (Softron, Tokyo, Japan). HbA1c was measured by the HPLC method. Serum creatinine was measured by the 3-hydroxy-2,4,6-triiodobenzoic acid method. Food intake was calculated as the average over 3 days. Insulin concentration was measured by a rat insulin RIA kit (LincoResearch, St Charles, MO, USA). Urine samples were collected over a 24 h period in individual metabolism cages. Urinary albumin excretion was measured by nephelometry using anti-rat albumin antibody (ICN Pharmaceuticals, Aurora, OH, USA). Creatinine clearance (ml min−1 kg−1) was calculated as described previously [15].
Light microscopy
The glomerular tuft area and mesangial matrix index (ratio of the mesangial matrix area/glomerular tuft area) were measured using a software package (Lumina Vision; Mitani, Fukui, Japan) as described previously [13]. Periodic acid–Schiff’s reagent staining was used to observe the interstitium of the kidney. Quantitative analysis for all staining was performed in a blinded manner.
Immunoperoxidase staining
Immunoperoxidase staining was performed as described [12, 27]. Primary antibodies were macrophages mouse antibody (ED1, 1:50; Serotec, Oxford, UK), 8-hydroxydeoxyguanosin (8-OHdG) mouse antibody (1:10; JalCA, Shizuoka, Japan), NADPH oxidase 4 (NOX4) rabbit antibody (1:300; Novus Biologicals, Littleton, CO, USA) or GLP-1R rabbit antibody (ab39072, 1:200; Abcam, Tokyo, Japan), all of which were applied for 12 h at 4°C. Secondary antibodies were biotin-labelled anti-mouse or anti-rabbit IgG (Jackson ImmunoResearch, West Grove, PA, USA), which were applied for 60 min at room temperature. The average number of ED1-positive cells per glomerulus was used for the estimation. The ratio of the area stained positive with each of the above antibodies to the glomerular tuft area was calculated with a software package (Lumina Vision).
Immunofluorescence staining
Immunofluorescence staining was performed as described [12]. The primary antibodies were ICAM-1 mouse antibody (1:25; Abcam) or type IV collagen rabbit antibody (1:200; LSL, Tokyo, Japan), which were applied for 60 min at room temperature. Secondary antibodies were FITC-conjugated anti-mouse or anti-rabbit IgG (1:150; Zymed Laboratories, San Francisco, CA, USA), which were applied for 30 min at room temperature. Micrographic fluorescence photos were obtained with a laser-scanning confocal microscope (LSM-510; Carl Zeiss, Jena, Germany). The ICAM-1 and type IV collagen indexes were calculated as described [15].
Double immunofluorescence staining
The primary antibodies were GLP-1R rabbit antibody (1:200; Abcam) and rat endothelial cell antigen (RECA-1, 1:40; Monosan, Uden, the Netherlands), macrophages (ED1, 1:50) mouse antibody, or NOX4 rabbit antibody (1:300), which were applied for 12 h at 4°C. The secondary antibodies were Alexa-Fluor 488-labelled anti-rabbit and 546-labelled anti-mouse IgG (1:400; Invitrogen, Carlsbad, CA, USA), which were applied for 30 min at room temperature. Nuclei were stained with DAPI (Millipore, Tokyo, Japan). The sections were observed under a fluorescence microscope (BZ-800; Keyence, Osaka, Japan).
Quantitative real-time RT-PCR and gene expression
Total RNA was extracted from each sample (the rat renal cortex, glomeruli isolated by a previously reported mechanical sieving technique [28] and cultured cells) using a kit (RNeasy plus Mini; Qiagen, Valencia, CA, USA). Single-strand cDNA was synthesised from the individual samples of total RNA at 1 μg using a kit (GeneAmp RNA PCR-Core kit; Applied Biosystems, Foster City, CA, USA). After addition of each set of primers (final concentration 0.4 μmol/l) and template DNA to the master mix, quantitative real-time RT-PCR was performed with a LightCycler (Roche Diagnostics, Tokyo, Japan) and SYBR Premix-Ex-Taq (Takara Bio, Shiga, Japan). The PCR protocol was as follows: initial denaturation (95°C for 30 s), followed by 40 cycles of denaturation (95°C for 5 s), and annealing and extension (60°C for 20 s). The specific oligonucleotide primer sequences are shown in Electronic supplementary material (ESM) Table 1. To visualise gene expression, individual DNA fragments were electrophoresed on a 2% (wt./vol) agarose gel (Sigma-Aldrich) and treated with ethidium bromide. cDNAs of the human pancreas (Takara Bio) and of rat islet-cell tumour cells (RIN-5F; DS Pharma Biomedical, Osaka, Japan) were used as positive controls.
Urinary 8-OHdG excretion
8-OHdG is a marker of oxidative DNA damage [29]. Urinary 8-OHdG concentration in a 24 h urine collection was measured with a kit (8-OHdG ELISA; JalCA) according to the manufacturer’s instructions.
Nuclear factor-κB activation
Nuclear proteins of kidney tissues were extracted by a nuclear extract kit and nuclear factor-κB (NF-κB) p65 activity determined by ELISA using reagents (Active-Motif; Carlsbad, CA, USA) according to the manufacturer’s instructions. Absorbance was normalised to milligram cell protein.
Western blotting
Cells were lysed with cell lysis buffer containing 10 mmol/l TRIS (pH 7.4), 1% (vol./vol.) Triton X-100, 0.5% (vol./vol.) Nonidet P-40 and phosphatase inhibitor cocktail, 150 mmol/l NaCl, 1 mmol/l EDTA, 0.2 mmol/l EGTA, vanadate and phenylmethanesulfonyl fluoride. The cell lysates were subjected to 7.5% SDS-PAGE (Bio-Rad Japan, Tokyo, Japan). The separated proteins were transferred to polyvinylidene fluoride membranes (Bio-Rad) by electrotransfer. The blots were subsequently blocked with 5% (vol./vol.) skimmed milk (Nacalai Tesque, Kyoto, Japan) and then incubated with GLP-1R rabbit antibody (1:500; Abcam) and ICAM-1 mouse antibody (1:100; Abcam) for 12 h at 4°C, or with β-actin rabbit antibody (1:1,000; Sigma-Aldrich) for 1 h at room temperature. The membrane was incubated with horseradish-peroxidase-linked donkey anti-rabbit or anti-mouse IgG (1:5,000; GE Healthcare Japan, Tokyo, Japan) at room temperature for 2 h. The blots were then visualised with a western blotting detection system (ECL plus; GE Healthcare).
Culture
Human glomerular microvascular endothelial cells (hGECs) (ACBRI, Kirkland, WA, USA) were cultured in EGM-MV2 medium (Cambrex, East Rutherford, NJ, USA) supplemented with 19.4 mmol/l d-glucose, 10% (vol./vol.) FCS and growth factor within a gelatin-precoated flask in a 5% CO2 incubator at 37°C.
THP-1 cells (a human monocytic cell line; JCRB, Tokyo, Japan) were cultured in RPMI 1640 supplemented with 10 mmol/l d-glucose, 10% FCS and growth factor in a 5% CO2 incubator at 37°C.
Human circulating monocytes
The human circulating monocytes were extracted using lymphocyte separation medium (MP Biomedicals, Tokyo, Japan) according to the manufacturer’s instructions. After incubation in RPMI 1640 with 50 ng/ml phorbol myristate acetate (Sigma-Aldrich) for 24 h, total RNA was collected from the attaching cells as described above.
The effects of GLP-1 in THP-1 cells
THP-1 cells (1 × 106 cells/ml) were incubated for 24 h in six-well plates in RPMI 1640 medium supplemented with 1% FCS and 5.5 mmol/l d-glucose. THP-1 cells were exposed to the following conditions: (1) 5.5 mmol/l d-glucose (normal glucose); (2) 5.5 mmol/l d-glucose with 9.5 mmol/l mannitol (osmotic control); (3) 15 mmol/l d-glucose (high glucose); (4) high glucose with 2.5 nmol/l exendin-4; (5) high glucose with 10 nmol/l exendin-4; (6) high glucose with 100 nmol/l exendin-4; and (7) high glucose with 100 nmol/l exendin-4 and 1000 nmol/l GLP-1R antagonist (9-39) (Bachem). After incubation for 72 h, total RNA and supernatant fractions were collected from the cells. The supernatant fractions were measured using a human TNF-α and IL-1β immunoassay (Quantikine; R&D Systems, Minneapolis, MN, USA) according to the manufacturer’s instructions.
The effect of GLP-1 in hGECs
After starvation for 12 h, hGECs were exposed to the following conditions: (1) no TNF-α stimulation (control); (2) 100 pg/ml TNF-α alone; (3) TNF-α with 2.5 nmol/l exendin-4; (4) TNF-α with 10 nmol/l exendin-4; (5) TNF-α with 100 nmol/l exendin-4; and (6) TNF-α with 100 nmol/l exendin-4 and 1000 nmol/l GLP-1R antagonist (9-39). After incubation for 6 h, total RNA and protein were collected from cells as described above. Recombinant human TNF-α was purchased from R&D Systems.
Statistical analysis
All values are expressed as the means ± SEM. Differences between groups were examined for statistical significance using the Mann–Whitney test or one-way ANOVA followed by Scheffe’s test. Values of p < 0.05 were considered to indicate statistically significant differences.
Results
Metabolic variables and urinary albumin excretion
Body, organ weights and systolic BP
As seen in Table 1, body weights of the diabetic groups at 8 weeks after initiation of exendin-4 treatment were significantly lower than those of the non-diabetic groups. The kidney weights per body weight of the diabetic groups were significantly higher than those of the non-diabetic groups. There were no significant differences among the diabetic groups. Systolic BP was similar in all groups.
Food intake, HbA1c and insulin
Food intake and HbA1c were significantly elevated in the diabetic groups. However, there were no significant differences among the diabetic groups. Although GLP-1 has beta cell-protective effects, serum insulin concentration was not detectable in the diabetic groups in spite of the high blood glucose levels (data not shown).
Urinary albumin excretion and creatinine clearance
Urinary albumin excretion, which is a characteristic feature of the early stage of diabetic nephropathy, increased progressively in the diabetic groups during the study. Exendin-4 treatment significantly reduced urinary albumin excretion compared with that of the diabetes group at 8 weeks (Fig. 1a). In addition, exendin-4 treatment prevented diabetes-induced hyperfiltration (Fig. 1b).
a Time course of 24 h urinary albumin excretion. Urinary albumin excretion increased gradually over 8 weeks in the diabetic group. Exendin-4 resulted in a significantly lower level of urinary albumin excretion at 8 weeks than in the untreated diabetes group. *p < 0.05; **p < 0.01 vs non-diabetic and non-diabetic + exendin-4 groups. Black circles, non-diabetic group; white circles, non-diabetic + exendin-4; black squares, streptozotocin-induced diabetes group; white squares, diabetes + exendin-4 group. b Creatinine clearance. Hyperfiltration in the diabetic (DM) nephropathy group was significantly decreased by exendin-4 treatment (DM+EX) at 8 weeks. *p < 0.05 vs non-diabetic + exendin-4 (ND+EX); **p < 0.01 vs ND; † p < 0.05 vs DM. c–f Periodic acid–methenamine-silver (PAM) staining in glomeruli (original magnification ×200). g–j Periodic acid–Schiff’s reagent staining in the kidney (×100). k Glomerular size (tuft area). Glomerular hypertrophy was significantly greater in the DM group than in the ND groups. Exendin-4 treatment significantly suppressed glomerular hypertrophy. ***p < 0.001 vs ND and ND+EX; †† p < 0.01 vs DM. l Mesangial matrix index, calculated by the PAM-positive area in the tuft area, was significantly increased in the DM group. Exendin-4 treatment significantly reduced mesangial matrix expansion. ***p < 0.001 vs ND and ND+EX; ††† p < 0.001 vs DM. n = 5 animals in the untreated ND group; n = 6 animals per group in the three other groups. k, l Glomeruli: n = 30 from each rat kidney; n = 4 per group. Values are the means ± SEM
Kidney morphology
The level of glomerular hypertrophy was significantly higher in the diabetes group than in non-diabetic groups. In contrast, exendin-4 treatment inhibited glomerular hypertrophy (Fig. 1c–f, k) in diabetes. Quantitative analysis showed that mesangial matrix index, which was used as an index of mesangial expansion, was significantly increased in the diabetes group. However, exendin-4 treatment significantly reduced mesangial matrix expansion (Fig. 1l). The renal interstitium showed a significantly higher level of tubular hypertrophy in the diabetic groups than in non-diabetic groups. However, there was no remarkable difference among the diabetic groups. In addition, no histological change of fibrosis in the renal interstitium was seen in any of the groups (Fig. 1g–j).
Microinflammation in the kidney
To evaluate the anti-inflammatory effect of exendin-4 in the kidney, we examined gene expression of Cd14, which is regarded as a cell surface marker of macrophages, as well as expression of Icam1 and Tgfb1 in the cortex. Cd14, Icam1 and Tgfb1 were significantly upregulated in the diabetes group and significantly downregulated by exendin-4 treatment (Fig. 2a–c). Regarding the glomeruli, we evaluated macrophage infiltration, and ICAM-1 and type IV collagen levels in glomeruli. The number of macrophages in glomeruli was significantly elevated in the diabetic compared with the non-diabetic groups. In contrast, exendin-4 treatment significantly prevented glomerular macrophage infiltration (Fig. 2d–g, p) in diabetes. The ICAM-1 level was significantly increased in the diabetic groups, but was significantly reduced by exendin-4 treatment (Fig. 2h–k, q). The type IV collagen level, which is an important component in the mesangial matrix, was significantly increased in the diabetes group and significantly reduced by exendin-4 treatment (Fig. 2l–o, r).
Exendin-4 treatment suppressed the inflammatory axis in the kidney. a Quantification of Cd14, (b) Icam1 and (c) Tgfb1 gene expression by real-time RT-PCR in the renal cortex. All three genes were significantly downregulated by exendin-4 treatment. Values (means ± SEM) are presented as fold relative to Actb and expressed as 1 in ND; n = 4 per group. Each experiment was performed three times. **p < 0.01 and ***p < 0.001 vs non-diabetic (ND) and ND + exendin-4 (EX); † p < 0.05 and ††† p < 0.001 vs diabetes (DM). d–g Immunoperoxidase staining for macrophages (ED1-positive cells), indicated by arrows. h–k Immunofluorescence staining for ICAM-1 and (l–o) for type IV collagen. Magnification, all images ×200. p Quantification of the number of macrophages per glomerulus, which was significantly increased in the diabetic groups. Exendin-4 treatment significantly prevented glomerular macrophage infiltration in diabetes. ***p < 0.001 vs ND and ND+EX; ††† p < 0.001 vs DM. q Quantification of glomerular ICAM-1 staining per glomerulus, which was significantly increased in the diabetic groups and significantly reduced vs DM by exendin-4 treatment. ***p < 0.001 vs ND and ND+EX; ††† p < 0.001 vs DM. r Quantification of type IV collagen staining per glomerulus. Type IV collagen was significantly increased in the DM group and significantly reduced by exendin-4 treatment. ***p < 0.001 vs ND and ND+EX; ††† p < 0.001 vs DM. p–r Values are the means ± SEM; n = 20 glomeruli from each rat kidney; n = 4 per group. Each experiment was repeated three times
Influence of exendin-4 on oxidative stress
To evaluate oxidative stress, we focused on 8-OHdG and NOX4. Urinary excretion of 8-OHdG was significantly increased in the diabetic groups compared with the non-diabetic groups. Exendin-4 treatment significantly decreased urinary excretion of 8-OHdG in diabetes (Fig. 3a). Immunoperoxidase staining for 8-OHdG revealed a significant abundance of 8-OHdG in glomeruli in the diabetic groups, which was significantly reduced by exendin-4 treatment (Fig. 3b–e, j). Nox4 gene expression in the cortex was significantly upregulated in the diabetes group and significantly downregulated by exendin-4 treatment (Fig. 3k). We demonstrated the presence of NOX4 in glomerular endothelial cells in the rat kidney (ESM Fig. 1h–k). Immunoperoxidase staining for NOX4 revealed a significant abundance of NOX4 in the diabetic kidney. However, exendin-4 treatment significantly reduced the level of NOX4 in diabetes (Fig. 3f–i, l).
Exendin-4 treatment suppressed oxidative stress and NF-κB activation. a Urinary 8-OHdG concentration in a 24 h urine collection. Urinary 8-OHdG excretion was significantly increased in the diabetic groups (DM). However, exendin-4 treatment (EX) significantly decreased urinary 8-OHdG excretion; n = 5 per group. The experiment was repeated twice. *p < 0.05 vs non-diabetic (ND)+EX; **p < 0.01 vs ND; ***p < 0.001 vs ND and ND+EX; †† p < 0.01 vs DM. b–e Immunoperoxidase staining for 8-OHdG and (f–i) NOX4 in glomeruli. Magnification, all images ×200. j Quantification of 8-OHdG content (μm2/μm2) as staining per glomerulus. Glomerular 8-OHdG content was significantly increased in the diabetic groups and significantly reduced by exendin-4 treatment. Values are means ± SEM; n = 20 glomeruli from each rat kidney; n = 4 per group. ***p < 0.001 vs ND and ND+EX; ††† p < 0.001 vs DM. k Quantification of Nox4 by real-time RT-PCR in the renal cortex. Nox4 expression was significantly downregulated by exendin-4 treatment. Values (means ± SEM) are presented as fold relative to Actb and expressed as 1 in ND; n = 4 per group. Each experiment was repeated three times. *p < 0.05 vs ND and ND+EX; † p < 0.05 vs DM. l Quantification of NOX4 content (μm2/μm2) as staining per glomerulus. NOX4 content was significantly increased in the diabetic groups and significantly suppressed by exendin-4 treatment. Values are means ± SEM; n = 20 glomeruli from each rat kidney; n = 4 per group. **p < 0.01 and ***p < 0.001 vs ND and ND+EX; ††† p < 0.001 vs DM. m NF-kB p65 DNA-binding activity. NF-κB p65DNA-binding activity was significantly increased in the DM group. Exendin-4 treatment significantly decreased NF-κB p65 DNA-binding activity. Values are the means ± SEM; n = 5 per group. The experiment was repeated twice. *p < 0.05 vs ND and ND+EX; † p < 0.05 vs DM
NF-κB activation in the kidney
The activation of NF-κB p65 DNA-binding activity was significantly enhanced in the diabetes compared with the non-diabetic groups. Exendin-4 treatment significantly inhibited NF-κB p65 DNA-binding activity in diabetes (Fig. 3m).
GLP-1R in rat glomeruli
We demonstrated the existence of GLP-1R in rat glomeruli (Fig. 4a, d). Double immunofluorescence staining revealed production of GLP-1R on glomerular endothelial cells (Fig. 4e–h). In addition, we ascertained that GLP-1R was produced on macrophages in rat glomeruli (Fig. 4i–l). The GLP-1R levels in glomeruli were not significantly different among the groups (ESM Fig. 1a–g).
The production of GLP-1R in rat glomeruli. a Glp1r gene expression in rat glomeruli. r-P: rat positive control (RIN-5F: rat islet-cell tumour). b Immunoperoxidase staining for GLP-1R, with negative control in rat pancreas islet cells, (c) positive control in rat pancreas islet cells and (d) rat glomeruli. e–h Double immunofluorescence staining for GLP-1R and glomerular endothelial cells as labelled. RECA-1, rat endothelial cell antigen. i–l Double immunofluorescence staining for GLP-1R and macrophages
GLP-1R in human macrophages and hGECs
We identified the existence of GLP-1R in THP-1 cells and hGECs (Figs 5a, b and 6a, b). In addition, we examined GLP1R gene expression in human circulating monocytes. We demonstrated that the GLP-1R gene was not only expressed in the THP-1 cell line, but also in human circulating monocytes (Fig. 5a).
The direct effects of exendin-4 on THP-1 cells. a GLP1R gene expression in human circulating monocytes (hCM) and THP-1 cells. h-P, human positive control (human pancreas). b GLP-1R protein production in THP-1 cells by western blotting. c Quantification of TNF and (d) IL1B mRNA expression in THP-1 by real-time RT-PCR. THP-1 cells stimulated with 15 mmol/l high glucose (HG; 15.0 mmol/l d-glucose) for 72 h showed significantly enhanced TNF and IL1B expression. Exendin-4 (EX) significantly and dose-dependently suppressed TNF and IL1B gene expression. GLP-1R antagonist (anti-EX; 1,000 nmol/l) significantly inhibited the suppressive effects of exendin-4 (100 nmol/l) on TNF and IL1B expression. Values (means ± SEM) are presented as fold relative to GAPDH and expressed as 1 in normal glucose (NG; 5.5 mmol/l d-glucose), n = 5 per group. The experiment was repeated three times. ***p < 0.001 vs NG and 5.5 mmol/l d-glucose with 9.5 mmol/l mannitol (HM); † p < 0.05 and †† p < 0.01 vs HG; ‡‡ p < 0.01 and ‡‡‡ p < 0.001 vs HG+EX (100 nmol/l; EX100). e Quantification of TNF-α and (f) IL-1β secretion (pg/ml) from THP-1 by ELISA. Stimulation of THP-1 cells with HG for 72 h significantly promoted TNF-α and IL-1β secretion. Exendin-4 significantly suppressed TNF-α and IL-1β secretion. GLP-1R antagonist (anti-EX; 1,000 nmol/l) significantly inhibited the suppressive effects of exendin-4 (100 nmol/l) on TNF-α and IL-1β secretion. Values are the means ± SEM; n = 5 per group. The experiment was repeated twice. ***p < 0.001 vs NG and HM; † p < 0.05 and ††† p < 0.001 vs HG; ‡ p < 0.05 and ‡‡‡ p < 0.001 vs HG+EX100. EX2.5, 2.5 nmol/l exendin-4; EX10, 10 nmol/l exendin-4
The direct effects of exendin-4 on hGECs. a GLP1R gene expression in hGECs. h-P, human positive control (human pancreas). b GLP-1R protein production in hGECs by western blotting. c Quantification of ICAM1 expression in hGECs by real-time RT-PCR. hGECs stimulated with TNF-α (100 pg/ml) for 6 h showed significantly enhanced ICAM1 expression. Exendin-4 (EX) significantly and dose-dependently suppressed ICAM1 gene expression. GLP-1R antagonist (1,000 nmol/l; anti-EX) significantly inhibited the suppressive effect of 100 nmol/l exendin-4 (EX100) on ICAM1 expression. Values (means ± SEM) are presented as fold relative to ACTB and expressed as 1 in control (no TNF-α stimulation); n = 5 per group. The experiment was repeated three times. **p < 0.01 vs control; † p < 0.05 vs TNF-α stimulation; ‡ p < 0.05 vs TNF-α + 100 nmol/l EX (EX100). d ICAM-1 production in hGECs by western blotting analysis, with (e) quantification. hGECs stimulated with TNF-α (100 pg/ml) for 6 h significantly promoted ICAM-1 production. Exendin-4 significantly suppressed ICAM-1 production. Anti-EX significantly inhibited the suppressive effect of EX100 on ICAM-1 production. Values (means ± SEM) are presented as fold relative to β-actin and expressed as 1 in control (no TNF-α stimulation); n = 5 per group. The experiment was repeated twice. ***p < 0.01 vs control; † p < 0.05 vs TNF-α stimulation; ‡ p < 0.05 vs TNF-α + EX100. EX2.5, 2.5 nmol/l exendin-4; EX10, 10 nmol/l exendin-4
The effects of GLP-1 through GLP-1R on THP-1 cells and hGECs
THP-1 cells stimulated with a high concentration of glucose for 72 h showed significantly enhanced levels of TNF and IL1B gene expression. Exendin-4 significantly and dose-dependently attenuated TNF and IL1B gene expression. Additionally, the effects of exendin-4 were significantly blocked by a GLP-1R antagonist (Fig. 5c, d). Similarly, exendin-4 significantly suppressed TNF-α and IL-1β secretion from THP-1, effects that were also significantly blocked by the GLP-1R antagonist (Fig. 5e, f).
hGECs stimulated with TNF-α for 6 h showed significantly enhanced ICAM1 gene expression. Exendin-4 significantly and dose-dependently attenuated ICAM1 gene expression. In addition, the effect of exendin-4 was significantly blocked by the GLP-1R antagonist (Fig. 6c). Likewise, exendin-4 significantly suppressed TNF-α-induced ICAM-1 production on hGECs, an effect that, again, was also significantly blocked by the GLP-1R antagonist (Fig. 6d, e).
Discussion
In the present study, we showed that exendin-4 exerted renoprotective effects through anti-inflammatory actions without lowering the blood glucose level in a streptozotocin-induced rat model of type 1 diabetes. In addition, exendin-4 inhibited NF-κB activity in the kidney, which is known to contribute to cross-talk between inflammation and oxidative stress. We also found that GLP-1R was produced in rat, and in cultured macrophages and glomerular endothelial cells. Exendin-4 acted directly on GLP-1R and attenuated production of pro-inflammatory cytokines and ICAM-1 in vitro. This is the first report of a GLP-1R agonist directly contributing, via its anti-inflammatory effects, to amelioration of characteristic features of diabetic nephropathy, such as increased urinary albumin excretion, glomerular hypertrophy and mesangial matrix expansion.
The current results suggest that exendin-4 alleviated the above-mentioned features by suppressing: (1) ICAM-1 production; (2) macrophage infiltration; (3) NF-κB activation; (4) oxidative stress; and (5) Tgfb1 mRNA expression and type IV collagen accumulation in the kidney.
An increase in the level of ICAM-1 on glomerular endothelial cells promotes macrophage infiltration into glomeruli [12, 14]. In our study, exendin-4 prevented macrophage infiltration into glomeruli. The mechanism underlying this effect was thought to be the suppression of ICAM-1 production on glomerular endothelial cells and direct inhibition of cytokine release from macrophages, which breaks the vicious cycle between macrophages and glomerular endothelial cells that gives rise to microinflammation. In HUVECs, treatment with liraglutide, a long-acting GLP-1 analogue, has also been shown to inhibit TNF-α or hyperglycaemia-mediated induction of ICAM-1 gene and protein [30]. These reports support our present findings. In our study, high glucose (15 mmol/l) stimulation for a period of 24 to 72 h did not significantly enhance ICAM1 gene expression in hGECs (data not shown).
Macrophages play a critical role in the development of diabetic nephropathy. In vitro, the culture supernatant fraction of macrophages has been shown to stimulate mesangial cells to produce fibronectin [31], while macrophages directly secrete TGF-β [32]. Both of these processes play a central role in the enhancement of glomerular extracellular matrix production in diabetic nephropathy [33, 34]. Based on these previous and our present findings, we conclude that the inhibition of macrophage infiltration by exendin-4 has a beneficial effect on suppressing progression of diabetic nephropathy.
In the diabetic state, many factors contribute to elevated NF-κB activation [35]. NF-κB is also the most important transcription factor regulating ICAM-1 production [36]. Arakawa et al. [37] reported that exendin-4 suppressed NF-κB activation of lipopolysaccharide-induced macrophages, suggesting that exendin-4 reduced direct NF-κB activation in macrophages. The reduction of NF-κB activity by exendin-4 may lead to inhibition of ICAM-1 levels and suppression of pro-inflammatory cytokines derived from macrophages.
Oxidative stress and inflammation are closely related to each other and create a vicious cycle in the diabetic state. Gorin et al. [38] showed that NADPH oxidase, and especially the NOX4 component of NADPH in the kidney, is important as the major source of oxidative stress in streptozotocin-induced diabetic nephropathy. Although many stimuli activate NOX4 production, cytokines and shear stress are important factors in the diabetic state [39]. NOX4 has been reported to be produced on epithelial cells [40] and mesangial cells [27], and was confirmed to be produced on endothelial cells in this study. In our study, exendin-4 suppressed NOX4 levels in the kidney. We speculate that reducing the release of pro-inflammatory cytokines from macrophages and normalising hyperfiltration by exendin-4 treatment may have contributed to the suppression of NOX4 production. Etoh et al. [27] reported that localisation and levels of NOX4 were in parallel with those of 8-OHdG. Therefore, the reduction of NOX4 level by exendin-4 treatment would contribute to a decrease in 8-OHdG production in glomeruli. Park et al. [25] also reported similar results in regard to 8-OHdG reduction by exendin-4 in a mouse model of type 2 diabetes. We speculate that exendin-4 contributes to an attenuation of oxidative stress and that this helps ameliorate diabetic vascular complications.
It is well known that GLP-1 signalling through GLP-1R enhances cyclic AMP as a second messenger [41]. Previous reports have revealed that an increase in activity of the cyclic AMP/protein kinase A pathway suppresses NF-κB activity in THP-1 cells and HUVECs [42], and inhibits NADPH oxidase [43]. These findings support our finding that exendin-4 modulated the inflammatory vicious cycle in the kidney.
In our model, exendin-4 did not affect blood glucose levels, blood pressure, food intake or body weight as it has been shown to do in models of type 2 diabetes. To determine that the effects of exendin-4 occurred without lowering of blood glucose, we started exendin-4 treatment at 1 week after the streptozotocin injections and confirmed that exendin-4 did not restore insulin secretion in our model. A much higher dose than that used in our study would have been necessary to reduce blood pressure in diabetic rats [26]. GLP-1 inhibits food intake and results in weight loss [18, 20, 21]. In the present study, the non-diabetic group treated with exendin-4 had decreased food intake and weight loss compared with the control group, but there were no significant differences. It is difficult to differentiate the effect of exendin-4 from the significant weight reduction that is generally seen in the model of type 1 diabetes.
In this study, the ratio of kidney weight to body weight in the diabetic groups was significantly increased in diabetic rats compared with the non-diabetic groups. However, exendin-4 treatment did not affect them. As periodic acid–Schiff’s reagent staining revealed, exendin-4 did not ameliorate tubular hypertrophy. Tubular hypertrophy may be the main factor contributing to kidney weight, and we need to investigate a longer period to appreciate the effect of exendin-4 on tubular hypertrophy and interstitial fibrosis. Additionally, exendin-4 prevented diabetes-induced hyperfiltration. Previous reports have revealed that hyperfiltration was improved by exendin-4 treatment in obese diabetic patients [44] and the db/db mouse model [25]. There has been no report that exendin-4 affects creatinine clearance in a later stage of diabetic nephropathy.
The inflammatory process is involved in the mechanism of obesity-related insulin resistance [45] and in the pathogenesis of atherosclerosis [46]. Moreover, there is also a close relationship between chronic renal insufficiency and the cardiorenal syndrome, through several pathways including inflammation [47, 48]. GLP-1R agonists might be beneficial for these diseases through their anti-inflammatory effects. Recently, Arakawa et al. [37] reported an anti-inflammatory effect of exendin-4 in an animal model of atherosclerosis. Their report also pointed out the importance of exendin-4 as a potential therapeutic agent for cardiovascular disease in diabetes.
In conclusion, we have shown that exendin-4 exerts renoprotective effects through anti-inflammatory actions without lowering blood glucose in a streptozotocin-induced rat model of type 1 diabetes. Furthermore, exendin-4 directly acted on GLP-1R and suppressed production of pro-inflammatory cytokines and ICAM-1. This study may provide the first evidence that GLP-1R agonists directly contribute to the prevention of diabetic nephropathy via an anti-inflammatory effect.
Abbreviations
- GLP-1:
-
Glucagon-like peptide-1
- GLP-1R:
-
Glucagon-like peptide-1 receptor
- hGECs:
-
Human glomerular microvascular endothelial cells
- ICAM-1:
-
Intercellular adhesion molecule-1
- NOX4:
-
NADPH oxidase 4
- NF-κB:
-
Nuclear factor-κB
- 8-OHdG:
-
8-Hydroxydeoxyguanosine
References
de Zeeuw D, Parving HH, Henning RH (2006) Microalbuminuria as an early marker for cardiovascular disease. J Am Soc Nephrol 17:2100–2105
Go AS, Chertow GM, Fan D, McCulloch CE, Hsu CY (2004) Chronic kidney disease and the risks of death, cardiovascular events, and hospitalization. N Engl J Med 351:1296–1305
Magee GM, Bilous RW, Cardwell CR, Hunter SJ, Kee F, Fogarty DG (2009) Is hyperfiltration associated with the future risk of developing diabetic nephropathy? A meta-analysis. Diabetologia 52:691–697
Baynes JW (1991) Role of oxidative stress in development of complications in diabetes. Diabetes 40:405–412
Brownlee M, Cerami A, Vlassara H (1988) Advanced glycosylation end products in tissue and the biochemical basis of diabetic complications. N Engl J Med 318:1315–1321
Koya D, Jirousek MR, Lin YW, Ishii H, Kuboki K, King GL (1997) Characterization of protein kinase C beta isoform activation on the gene expression of transforming growth factor-beta, extracellular matrix components, and prostanoids in the glomeruli of diabetic rats. J Clin Invest 100:115–126
Ziyadeh FN, Sharma K, Ericksen M, Wolf G (1994) Stimulation of collagen gene expression and protein synthesis in murine mesangial cells by high glucose is mediated by autocrine activation of transforming growth factor-beta. J Clin Invest 93:536–542
Nelson CL, Karschimkus CS, Dragicevic G et al (2005) Systemic and vascular inflammation is elevated in early IgA and type 1 diabetic nephropathies and relates to vascular disease risk factors and renal function. Nephrol Dial Transplant 20:2420–2426
Saraheimo M, Teppo AM, Forsblom C, Fagerudd J, Groop PH (2003) Diabetic nephropathy is associated with low-grade inflammation in type 1 diabetic patients. Diabetologia 46:1402–1407
Furuta T, Saito T, Ootaka T et al (1993) The role of macrophages in diabetic glomerulosclerosis. Am J Kidney Dis 21:480–485
Hirata K, Shikata K, Matsuda M et al (1998) Increased expression of selectins in kidneys of patients with diabetic nephropathy. Diabetologia 41:185–192
Sugimoto H, Shikata K, Hirata K et al (1997) Increased expression of intercellular adhesion molecule-1 (ICAM-1) in diabetic rat glomeruli: glomerular hyperfiltration is a potential mechanism of ICAM-1 upregulation. Diabetes 46:2075–2081
Okada S, Shikata K, Matsuda M et al (2003) Intercellular adhesion molecule-1-deficient mice are resistant against renal injury after induction of diabetes. Diabetes 52:2586–2593
Yozai K, Shikata K, Sasaki M et al (2005) Methotrexate prevents renal injury in experimental diabetic rats via anti-inflammatory actions. J Am Soc Nephrol 16:3326–3338
Tone A, Shikata K, Sasaki M et al (2005) Erythromycin ameliorates renal injury via anti-inflammatory effects in experimental diabetic rats. Diabetologia 48:2402–2411
Ohga S, Shikata K, Yozai K et al (2007) Thiazolidinedione ameliorates renal injury in experimental diabetic rats through anti-inflammatory effects mediated by inhibition of NF-kappaB activation. Am J Physiol Renal Physiol 292:F1141–F1150
Usui H, Shikata K, Matsuda M et al (2003) HMG-CoA reductase inhibitor ameliorates diabetic nephropathy by its pleiotropic effects in rats. Nephrol Dial Transplant 18:265–272
Baggio LL, Drucker DJ (2007) Biology of incretins: GLP-1 and GIP. Gastroenterology 132:2131–2157
Farilla L, Hui H, Bertolotto C et al (2002) Glucagon-like peptide-1 promotes islet cell growth and inhibits apoptosis in Zucker diabetic rats. Endocrinology 143:4397–4408
Nauck MA, Niedereichholz U, Ettler R et al (1997) Glucagon-like peptide 1 inhibition of gastric emptying outweighs its insulinotropic effects in healthy humans. Am J Physiol 273:E981–E988
Turton MD, O'Shea D, Gunn I et al (1996) A role for glucagon-like peptide-1 in the central regulation of feeding. Nature 379:69–72
Orskov C, Wettergren A, Holst JJ (1993) Biological effects and metabolic rates of glucagon like peptide-1 7-36 amide and glucagon like peptide-1 7-37 in healthy subjects are indistinguishable. Diabetes 42:658–661
Bullock BP, Heller RS, Habener JF (1996) Tissue distribution of messenger ribonucleic acid encoding the rat glucagon-like peptide-1 receptor. Endocrinology 137:2968–2978
Schlatter P, Beglinger C, Drewe J, Gutmann H (2007) Glucagon-like peptide 1 receptor expression in primary porcine proximal tubular cells. Regul Pept 141:120–128
Park CW, Kim HW, Ko SH et al (2007) Long-term treatment of glucagon-like peptide-1 analog exendin-4 ameliorates diabetic nephropathy through improving metabolic anomalies in db/db mice. J Am Soc Nephrol 18:1227–1238
Hirata K, Kume S, Araki S et al (2009) Exendin-4 has an anti-hypertensive effect in salt-sensitive mice model. Biochem Biophys Res Commun 380:44–49
Etoh T, Inoguchi T, Kakimoto M et al (2003) Increased expression of NAD(P)H oxidase subunits, NOX4 and p22phox, in the kidney of streptozotocin-induced diabetic rats and its reversibity by interventive insulin treatment. Diabetologia 46:1428–1437
Fong JS, Drummond KN (1968) Method for preparation of glomeruli for metabolic studies. J Lab Clin Med 71:1034–1039
Shigenaga MK, Gimeno CJ, Ames BN (1989) Urinary 8-hydroxy-2′-deoxyguanosine as a biological marker of in vivo oxidative DNA damage. Proc Natl Acad Sci U S A 86:9697–9701
Liu H, Dear AE, Knudsen LB, Simpson RW (2009) A long-acting glucagon-like peptide-1 analogue attenuates induction of plasminogen activator inhibitor type-1 and vascular adhesion molecules. J Endocrinol 201:59–66
Pawluczyk IZ, Harris KP (1997) Macrophages promote prosclerotic responses in cultured rat mesangial cells: a mechanism for the initiation of glomerulosclerosis. J Am Soc Nephrol 8:1525–1536
Leonarduzzi G, Scavazza A, Biasi F et al (1997) The lipid peroxidation end product 4-hydroxy-2,3-nonenal up-regulates transforming growth factor beta1 expression in the macrophage lineage: a link between oxidative injury and fibrosclerosis. Faseb J 11:851–857
Ziyadeh FN, Hoffman BB, Han DC et al (2000) Long-term prevention of renal insufficiency, excess matrix gene expression, and glomerular mesangial matrix expansion by treatment with monoclonal antitransforming growth factor-beta antibody in db/db diabetic mice. Proc Natl Acad Sci U S A 97:8015–8020
Sharma K, Ziyadeh FN (1995) Hyperglycemia and diabetic kidney disease. The case for transforming growth factor-beta as a key mediator. Diabetes 44:1139–1146
Guijarro C, Egido J (2001) Transcription factor-kappa B (NF-kappa B) and renal disease. Kidney Int 59:415–424
Roebuck KA, Finnegan A (1999) Regulation of intercellular adhesion molecule-1 (CD54) gene expression. J Leukoc Biol 66:876–888
Arakawa M, Mita T, Azuma K et al (2010) Inhibition of monocyte adhesion to endothelial cells and attenuation of atherosclerotic lesion by a glucagon-like peptide-1 receptor agonist, exendin-4. Diabetes 59:1030–1037
Gorin Y, Block K, Hernandez J et al (2005) Nox4 NAD(P)H oxidase mediates hypertrophy and fibronectin expression in the diabetic kidney. J Biol Chem 280:39616–39626
Frey RS, Ushio-Fukai M, Malik AB (2009) NADPH oxidase-dependent signaling in endothelial cells: role in physiology and pathophysiology. Antioxid Redox Signal 11:791–810
Sharma K, Ramachandrarao S, Qiu G et al (2008) Adiponectin regulates albuminuria and podocyte function in mice. J Clin Invest 118:1645–1656
Doyle ME, Egan JM (2007) Mechanisms of action of glucagon-like peptide 1 in the pancreas. Pharmacol Ther 113:546–593
Ollivier V, Parry GC, Cobb RR, de Prost D, Mackman N (1996) Elevated cyclic AMP inhibits NF-kappaB-mediated transcription in human monocytic cells and endothelial cells. J Biol Chem 271:20828–20835
Kim JS, Diebold BA, Babior BM, Knaus UG, Bokoch GM (2007) Regulation of Nox1 activity via protein kinase A-mediated phosphorylation of NoxA1 and 14-3-3 binding. J Biol Chem 282:34787–34800
Gutzwiller JP, Tschopp S, Bock A et al (2004) Glucagon-like peptide 1 induces natriuresis in healthy subjects and in insulin-resistant obese men. J Clin Endocrinol Metab 89:3055–3061
Xu H, Barnes GT, Yang Q et al (2003) Chronic inflammation in fat plays a crucial role in the development of obesity-related insulin resistance. J Clin Invest 112:1821–1830
Ross R (1999) Atherosclerosis—an inflammatory disease. N Engl J Med 340:115–126
Bongartz LG, Cramer MJ, Doevendans PA, Joles JA, Braam B (2005) The severe cardiorenal syndrome: ‘Guyton revisited’. Eur Heart J 26:11–17
Nakamura A, Shikata K, Hiramatsu M et al (2005) Serum interleukin-18 levels are associated with nephropathy and atherosclerosis in Japanese patients with type 2 diabetes. Diabetes Care 28:2890–2895
Acknowledgements
This study was supported in part by a Grant-in-Aid for Scientific Research from the Ministry of Education, Science, Culture, Sports and Technology (C21591031 to K. Shikata), and the Ministry of Health, Labour and Welfare of Japan.
Duality of interest
The authors declare that there is no duality of interest associated with this manuscript.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM Table 1
(PDF 68 kb)
ESM Fig. 1
a Quantification of Glp1r gene expression in the renal cortex and (b) glomeruli by real-time RT-PCR. c–f Immunoperoxidase staining for GLP-1R in glomeruli. Magnification ×200. g Quantification of GLP-1R staining per glomerulus. The glomerular GLP-1R contents were not significantly different among the glomerular groups. Values (means ± SEM) are presented relative to Actb and expressed as 1 in ND group; n = 5 per group. The experiment was repeated twice. h–k Double immunofluorescence staining for NOX4 and glomerular endothelial cells as labelled. ND, non-diabetic; ND+EX, non-diabetic plus exendin-4 treatment; DM, diabetic; DM+EX, diabetic + exendin-4 treatment; RECA, rat endothelial cell antigen (PDF 16529 kb)
Rights and permissions
About this article
Cite this article
Kodera, R., Shikata, K., Kataoka, H.U. et al. Glucagon-like peptide-1 receptor agonist ameliorates renal injury through its anti-inflammatory action without lowering blood glucose level in a rat model of type 1 diabetes. Diabetologia 54, 965–978 (2011). https://doi.org/10.1007/s00125-010-2028-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-010-2028-x