Abstract
Purpose
Studies on dynamic intraligamentary stabilization (DIS) of acute anterior cruciate ligament (ACL) ruptures reported failure rates similar to those of conventional ACL reconstruction. This study aimed to determine whether surgeon experience with DIS is associated with revision rates or patient-reported outcomes. The hypothesis was that more experienced surgeons achieved better outcomes following DIS due to substantial learning curve.
Methods
The authors prospectively enrolled 110 consecutive patients that underwent DIS and evaluated them at a minimum of 2 years. The effects of independent variables (surgeon experience, gender, age, adjuvant procedures, tear location, preinjury Tegner score, time from injury to surgery, and follow-up) on four principal outcomes (revision ACL surgery, any re-operation, IKDC and Lysholm score) were analyzed using univariable and multivariable regressions.
Results
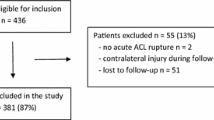
From the 110 patients enrolled, 14 patients (13%) were lost to follow-up. Of the remaining 96 patients, 11 underwent revision ACL surgery, leaving 85 patients for clinical assessment at a mean of 2.2 ± 0.4 years (range 2.0–3.8). Arthroscopic reoperations were performed in 26 (27%) patients, including 11 (11%) revision ACL surgeries. Multivariable regressions revealed: (1) no associations between the reoperation rate and the independent variables, (2) better IKDC scores for ‘designer surgeons’ (b = 10.7; CI 4.9–16.5; p < 0.001), higher preinjury Tegner scores (b = 2.5, CI 0.8–4.2; p = 0.005), and younger patients (b = 0.3, CI 0.0–0.6; p = 0.039), and (3) better Lysholm scores for ‘designer surgeons’ (b = 7.8, CI 2.8–12.8; p = 0.005) and preinjury Tegner score (b = 1.9, CI 0.5–3.4; p = 0.010).
Conclusion
Surgeon experience with DIS was not associated with rates of revision ACL surgery or general re-operations. Future, larger-scaled studies are needed to confirm these findings. Patients operated by ‘designer surgeons’ had slightly better IKDC and Lysholm scores, which could be due to better patient selection and/or positively biased attitudes of both surgeons and patients.
Level of evidence
Level II, prospective comparative study.

Similar content being viewed by others
Change history
25 August 2018
The original version of this article unfortunately contains mistake in Table 4.
25 August 2018
The original version of this article unfortunately contains mistake in Table 4.
25 August 2018
The original version of this article unfortunately contains mistake in Table 4.
25 August 2018
The original version of this article unfortunately contains mistake in Table 4.
25 August 2018
The original version of this article unfortunately contains mistake in Table 4.
25 August 2018
The original version of this article unfortunately contains mistake in Table 4.
25 August 2018
The original version of this article unfortunately contains mistake in Table 4.
25 August 2018
The original version of this article unfortunately contains mistake in Table 4.
References
Andernord D, Desai N, Bjornsson H, Ylander M, Karlsson J, Samuelsson K (2015) Patient predictors of early revision surgery after anterior cruciate ligament reconstruction: a cohort study of 16,930 patients with 2-year follow-up. Am J Sports Med 43:121–127
Anderson MJ, Browning WM 3rd, Urband CE, Kluczynski MA, Bisson LJ (2016) A systematic summary of systematic reviews on the topic of the anterior cruciate ligament. Orthop J Sports Med 4:2325967116634074
Ateschrang A, Ahmad SS, Stockle U, Schroeter S, Schenk W, Ahrend MD (2017) Recovery of ACL function after dynamic intraligamentary stabilization is resultant to restoration of ACL integrity and scar tissue formation. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-017-4656-x
Barrett GR, Luber K, Replogle WH, Manley JL (2010) Allograft anterior cruciate ligament reconstruction in the young, active patient: Tegner activity level and failure rate. Arthroscopy 26:1593–1601
Biau DJ, Tournoux C, Katsahian S, Schranz PJ, Nizard RS (2006) Bone-patellar tendon-bone autografts versus hamstring autografts for reconstruction of anterior cruciate ligament: meta-analysis. BMJ 332:995–1001
Bieri KS, Scholz SM, Kohl S, Aghayev E, Staub LP (2017) Dynamic intraligamentary stabilization versus conventional ACL reconstruction: a matched study on return to work. Injury. https://doi.org/10.1016/j.injury.2017.03.004
Borchers JR, Pedroza A, Kaeding C (2009) Activity level and graft type as risk factors for anterior cruciate ligament graft failure: a case-control study. Am J Sports Med 37:2362–2367
Buchler L, Regli D, Evangelopoulos DS, Bieri K, Ahmad SS, Krismer A et al (2016) Functional recovery following primary ACL repair with dynamic intraligamentary stabilization. Knee 23:549–553
Collins NJ, Misra D, Felson DT, Crossley KM, Roos EM (2011) Measures of knee function: International Knee Documentation Committee (IKDC) Subjective Knee Evaluation Form, Knee Injury and Osteoarthritis Outcome Score (KOOS), Knee Injury and Osteoarthritis Outcome Score Physical Function Short Form (KOOS-PS), Knee Outcome Survey Activities of Daily Living Scale (KOS-ADL), Lysholm Knee Scoring Scale, Oxford Knee Score (OKS), Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), Activity Rating Scale (ARS), and Tegner Activity Score (TAS). Arthritis Care Res (Hoboken) 63(Suppl 11):S208-228
Dunn WR, Lyman S, Lincoln AE, Amoroso PJ, Wickiewicz T, Marx RG (2004) The effect of anterior cruciate ligament reconstruction on the risk of knee reinjury. Am J Sports Med 32:1906–1914
Eggli S, Roder C, Perler G, Henle P (2016) Five year results of the first ten ACL patients treated with dynamic intraligamentary stabilisation. BMC Musculoskelet Disord 17:105
Fithian DC, Paxton EW, Stone ML, Luetzow WF, Csintalan RP, Phelan D et al (2005) Prospective trial of a treatment algorithm for the management of the anterior cruciate ligament-injured knee. Am J Sports Med 33:335–346
Frobell RB, Roos EM, Roos HP, Ranstam J, Lohmander LS (2010) A randomized trial of treatment for acute anterior cruciate ligament tears. N Engl J Med 363:331–342
Grindem H, Eitzen I, Engebretsen L, Snyder-Mackler L, Risberg MA (2014) Nonsurgical or surgical treatment of ACL injuries: knee function, sports participation, and knee reinjury: the Delaware-Oslo ACL cohort study. J Bone Jt Surg Am 96:1233–1241
Guo S, Dipietro LA (2010) Factors affecting wound healing. J Dent Res 89:219–229
Haberli J, Henle P, Acklin YP, Zderic I, Gueorguiev B (2016) Knee joint kinematics with dynamic augmentation of primary anterior cruciate ligament repair—a biomechanical study. J Exp Orthop 3:29
Haeberli J, Jaberg L, Bieri KS, Eggli S, Henle P (2017) Reinterventions after dynamic intraligamentary stabilization in primary anterior cruciate ligament repair. Knee. https://doi.org/10.1016/j.knee.2018.01.003
Henle P, Bieri KS, Brand M, Aghayev E, Bettfuehr J, Haeberli J et al (2017) Patient and surgical characteristics that affect revision risk in dynamic intraligamentary stabilization of the anterior cruciate ligament. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-017-4574-y
Henle P, Roder C, Perler G, Heitkemper S, Eggli S (2015) Dynamic intraligamentary stabilization (DIS) for treatment of acute anterior cruciate ligament ruptures: case series experience of the first three years. BMC Musculoskelet Disord 16:27
Herrington L (2013) Functional outcome from anterior cruciate ligament surgery: a review. OA Orthop 1:12
Kaeding CC, Pedroza AD, Reinke EK, Huston LJ, Consortium M, Spindler KP (2015) Risk factors and predictors of subsequent ACL injury in either knee after ACL reconstruction: prospective analysis of 2488 primary ACL reconstructions from the MOON cohort. Am J Sports Med 43:1583–1590
Kartus J, Magnusson L, Stener S, Brandsson S, Eriksson BI, Karlsson J (1999) Complications following arthroscopic anterior cruciate ligament reconstruction. A 2-5-year follow-up of 604 patients with special emphasis on anterior knee pain. Knee Surg Sports Traumatol Arthrosc 7:2–8
Kohl S, Evangelopoulos D, Schär M, Bieri K, Müller T, Ahmad S (2016) Dynamic intraligamentary stabilisation. Bone Jt J 98:793–798
Kohl S, Evangelopoulos DS, Schar MO, Bieri K, Muller T, Ahmad SS (2016) Dynamic intraligamentary stabilisation: initial experience with treatment of acute ACL ruptures. Bone Jt J 98-B:793–798
Kosters C, Herbort M, Schliemann B, Raschke MJ, Lenschow S (2015) Dynamic intraligamentary stabilization of the anterior cruciate ligament: Operative technique and short-term clinical results. Unfallchirurg 118:364–371
Krismer AM, Gousopoulos L, Kohl S, Ateschrang A, Kohlhof H, Ahmad SS (2017) Factors influencing the success of anterior cruciate ligament repair with dynamic intraligamentary stabilisation. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-017-4445-6
Meister M, Koch J, Amsler F, Arnold MP, Hirschmann MT (2017) ACL suturing using dynamic intraligamentary stabilisation showing good clinical outcome but a high reoperation rate: a retrospective independent study. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-017-4726-0
Noyes FR, Barber SD (2010) Noyes’ knee disorders: surgery, rehabilitation, clinical outcomes. Elsevier, Philadelphia, pp 213–256
Nyland J, Gamble C, Franklin T, Caborn DNM (2017) Permanent knee sensorimotor system changes following ACL injury and surgery. Knee Surg Sports Traumatol Arthrosc 25:1461–1474
Schliemann B, Glasbrenner J, Rosenbaum D, Lammers K, Herbort M, Domnick C et al (2017) Changes in gait pattern and early functional results after ACL repair are comparable to those of ACL reconstruction. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-017-4618-3
Schlumberger M, Schuster P, Schulz M, Immendorfer M, Mayer P, Bartholoma J et al (2015) Traumatic graft rupture after primary and revision anterior cruciate ligament reconstruction: retrospective analysis of incidence and risk factors in 2915 cases. Knee Surg Sports Traumatol Arthrosc 25(5):1535–1541
Shelbourne KD, Gray T, Haro M (2009) Incidence of subsequent injury to either knee within 5 years after anterior cruciate ligament reconstruction with patellar tendon autograft. Am J Sports Med 37:246–251
Sullivan GM, Artino AR Jr (2013) Analyzing and interpreting data from likert-type scales. J Grad Med Educ 5:541–542
Tegner Y, Lysholm J (1985) Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res 198:43–49
Tejwani SG, Chen J, Funahashi TT, Love R, Maletis GB (2015) Revision risk after allograft anterior cruciate ligament reconstruction: association with graft processing techniques, patient characteristics, and graft type. Am J Sports Med 43:2696–2705
Toy BJ, Yeasting RA, Morse DE, McCann P (1995) Arterial supply to the human anterior cruciate ligament. J Athl Train 30:149–152
van Melick N, van Cingel RE, Brooijmans F, Neeter C, van Tienen T, Hullegie W et al (2016) Evidence-based clinical practice update: practice guidelines for anterior cruciate ligament rehabilitation based on a systematic review and multidisciplinary consensus. Br J Sports Med 50:1506–1515
Webster KE, Feller JA (2016) Exploring the high reinjury rate in younger patients undergoing anterior cruciate ligament reconstruction. Am J Sports Med 44:2827–2832
Acknowledgements
The authors thank Mo Saffarini (ReSurg SA) for editorial assistance.
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors have received reimbursements or funding from Mathys AG Bettlach, Switzerland, in the past 5 years. The authors are not compensated for this work.
Ethical approval
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from the participants included in this study.
Rights and permissions
About this article
Cite this article
Henle, P., Bieri, K.S., Haeberli, J. et al. Surgeon experience with dynamic intraligamentary stabilization does not influence risk of failure. Knee Surg Sports Traumatol Arthrosc 26, 2978–2985 (2018). https://doi.org/10.1007/s00167-018-4847-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-4847-0