Abstract
Introduction and hypothesis
Understanding the clustering of pelvic floor disorders (PFDs) within families is important because it may suggest underlying risk factors that may be environmental, genetic or both. The objective of this study was to describe clinical characteristics observed in familial cases with PFDs and compare them with strictly defined controls.
Methods
Women evaluated and treated for PFDs were recruited as part of a larger genetic study. Here, we define familial cases as those with bothersome symptoms or treatment for a PFD (pelvic organ prolapse [POP], stress urinary incontinence [SUI], and overactive bladder [OAB]) and who had a first-degree relative with bothersome symptoms or treatment for the same pelvic floor defect. We assigned clinical characteristics to probands and their relatives using standardized symptom questions (PFDI), examination, and review of treatment records, if any.
Results
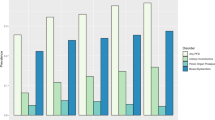
We identified 126 familial POP cases, 183 familial SUI cases, and 101 familial OAB cases. Familial cases were more likely to have bothersome symptoms for more than one PFD. Among familial POP cases, bothersome SUI (71 %), OAB (54 %), and a combination of all three disorders (48 %) were common. Among familial SUI cases, bothersome OAB (60 %), POP (59 %), and combinations of all disorders (40 %) were common. Among familial OAB cases, bothersome SUI (88 %), POP (66 %), and combinations of all three disorders (59 %) were common.
Conclusions
Familial cases of POP, SUI, and OAB are more likely to have more than one pelvic floor defect. It is likely that underlying genetic factors contribute to more than one pelvic floor defect.
Similar content being viewed by others
References
Jelosvek E, Maher C, Barber M (2007) Pelvic organ prolapse. Lancet 369:1027–1382
Altman D, Forsman M, Falconer C, Lichtenstein P (2008) Genetic influence on stress urinary incontinence and pelvic organ prolapse. Eur Urol 54(4):918–922
Allen-Brady K, Allen-Brady KL, Norton PA, Farnham JM, Teerlink C, Cannon-Albright LA (2009) Significant linkage evidence for a predisposition gene for pelvic floor disorder. Am J Hum Genet 84(5):678–682
Norton P, Allen-Brady K, Cannon-Albright L (2013) Familiality of pelvic organ prolapse in the Utah Population Database. Int Urogynecol J 24(3):413–418
Barber M, Walters M, Bump R (2005) Short form versions of two condition-specific quality-of-life questionnaires for women with pelvic floor disorders. Am J Obstet Gynecol 193(1):103–107
Ghasemi A, Gorouhi F, Rashighi-Firoozabadi M, Jafarian S, Firooz A (2007) Striae gravidarum: associated factors. J Eur Acad Dermatol Venereol 21(6):743–746
Remvig L, Jensen DV, Ward RC (2007) Epidemiology of general joint hypermobility and basis for the proposed criteria for benign joint hypermobility syndrome: review of the literature. J Rheumatol 34(4):804–809
Bump R, Mattiasson A, Bo K, Brubaker L, DeLancey J, Klarsov P, Shull B, Smith A (1996) The standardization of terminology in female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175(1):10–17
Nygaard I, Shaw J, Egger MJ (2012) Exploring the association between lifetime physical activity and pelvic floor disorders: study and design challenges. Contemp Clin Trials 33(4):819–827
Ross S, Soroka D, Karahalios A, Glazener CM, Hay-Smith EJ, Drutz HP (2006) Incontinence-specific quality of life measures used in trials of treatments for female urinary incontinence: a systematic review. Int Urogynecol J Pelvic Floor Dysfunct 17(3):272–285
Simmonds J, Keer R (2007) Hypermobility and the hypermobility syndrome. Man Ther 12(4):298–309
Tung JY, Kiefer AK, Mullins M, Francke U, Eriksson N (2013) Genome-wide association analysis implicates elastic microfibrils in the development of nonsyndromic striae distensae. J Invest Dermatol 133(11):2628–2631
Osman H, Rubeiz N, Tamim H, Nassar AH (2007) Risk factors for the development of striae gravidarum. Am J Obstet Gynecol 196(1):62.e1–5
Ahn C (1997) An evaluation of methods for the estimation of sensitivity and specificity of site-specific diagnostic tests. Biom J 39(7):793–807
Sternberg MR, Hadgu A (2001) A GEE approach to estimating sensitivity and specificity and coverage properties of the confidence intervals. Stat Med 20(9–10):1529–1539
Leisenring W, Pepe MS, Longton G (1997) A marginal regression modelling framework for evaluating medical diagnostic tests. Stat Med 16(11):1263–1281
Wu J, Ward R, Allen-Brady K, Edwards T, Norton P, Hartmann K, Hauser E, Velez-Edwards D (2013) Phenotyping clinical disorders: lessons learned from pelvic organ prolapse. Am J Obstet Gynecol 208:360
Aydeniz A, Dikensoy E, Cebesoy B, Altindağ O, Gürsoy S, Balat O (2010) The relation between genitourinary prolapse and joint hypermobility in Turkish women. Arch Gynecol Obstet 281(2):301–304
Lawrence J, Lukacz E, Nager C, Hsu J, Luber C (2008) Prevalence and co-occurrence of pelvic floor disorders in community-dwelling women. Obstet Gynecol 111(3):678–685
Wu JM, Visco AG, Grass EA et al (2012) Comprehensive analysis of LAMC1 genetic variants in advanced pelvic organ prolapse. Am J Obstet Gynecol 206:447.e1–447.e6
Budatha M, Roshanravan S, Zheng Q et al (2011) Extracellular matrix proteases contribute to progression of pelvic organ prolapse in mice and humans. J Clin Invest 121:2048–2059
Liu X, Zhao Y, Pawlyk B, Damaser M, Li T (2006) Failure of elastic fiber homeostasis leads to pelvic floor disorders. Am J Pathol 168:519–528
Rahn DD, Acevedo JF, Roshanravan S et al (2009) Failure of pelvic organ support in mice deficient in fibulin-3. Am J Pathol 174:206–215
Drewes PG, Yanagisawa H, Starcher B et al (2007) Pelvic organ prolapse in fibulin-5 knockout mice: pregnancy-induced changes in elastic fiber homeostasis in mouse vagina. Am J Pathol 170:578–589
Legro RS (2000) Is there a male phenotype in polycystic ovary syndrome families? Pediatr Endocrinol Metab 13 [Suppl 5]:1307–1309
Buchsbaum GM, Duecy EE, Kerr LA, Huang LS, Perevich M, Guzick DS (2006) Pelvic organ prolapse in nulliparous women and their parous sisters. Obstet Gynecol 108(6):1388–1393
Allen-Brady K, Cannon-Albright L, Farnham J, Teerlink C, Vierhout M, van Kempen L, Kluivers K, Norton P (2011) Genome-wide association analysis identifies six loci associated with pelvic organ prolapse. Obstet Gynecol 118(6):1345–1353
Acknowledgements
Partial support for all data sets within the Utah Population Database (UPDB) was provided by Huntsman Cancer Institute, University of Utah and the Huntsman Cancer Institute's Cancer Center Support grant, P30 CA42014 from National Cancer Institute. Data collection for this publication was supported by NIH grant Number R01 HD061821 from the Eunice Kennedy Shriver National Institute of Child Health and Human Development (Lisa Cannon Albright and Peggy Norton).
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Norton, P.A., Allen-Brady, K., Wu, J. et al. Clinical characteristics of women with familial pelvic floor disorders. Int Urogynecol J 26, 401–406 (2015). https://doi.org/10.1007/s00192-014-2513-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-014-2513-8