Abstract
Summary
This study evaluated the benefits of ZOL versus placebo on health-related quality of life (HRQoL) among patients from HORIZON–RFT. At month 24 and end of the study visit, ZOL significantly improved patients’ overall health state compared to placebo as assessed by the EQ-5D VAS.
Introduction
To evaluate the benefits of zoledronic acid (ZOL) versus placebo on health-related quality of life (HRQoL) among patients from The Health Outcomes and Reduced Incidence With Zoledronic Acid Once Yearly Recurrent Fracture Trial (HORIZON–RFT).
Methods
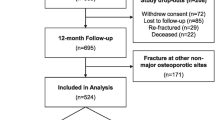
In this randomized, double-blind, placebo-controlled trial, 2,127 patients were randomized to receive annual infusion of ZOL 5 mg (n = 1,065) or placebo (n = 1,062) within 90 days after surgical repair of low-trauma hip fracture. HRQoL was measured using EQ-5D Visual Analogue Scale (VAS) and utility scores (EuroQol instrument) at months 6, 12, 24, 36, and end of the study visit. Analysis of covariance model included baseline EQ-5D value, region, and treatment as explanatory variables.
Results
At baseline, patients (mean age 75 years; 24% men and 76% women) were well matched between treatment groups with mean EQ-5D VAS of 65.82 in ZOL and 65.70 in placebo group. At the end of the study, mean change from baseline in EQ-5D VAS was greater for ZOL vs. placebo in all patients (7.67 ± 0.56 vs. 5.42 ± 0.56), and in subgroups of patients experiencing clinical vertebral fractures (8.86 ± 4.91 vs. −1.69 ± 3.42), non-vertebral fractures (5.03 ± 2.48 vs. −1.07 ± 2.16), and clinical fractures (5.19 ± 2.25 vs. −0.72 ± 1.82) with treatment difference significantly in favor of ZOL. EQ-5D utility scores were comparable for ZOL and placebo groups, but more patients on placebo consistently had extreme difficulty in mobility (1.74% for ZOL vs. 2.13% for placebo; p = 0.6238), self-care (4.92% vs. 6.69%; p = 0.1013), and usual activities (10.28% vs. 12.91%; p = 0.0775).
Conclusion
ZOL significantly improves HRQoL in patients with low-trauma hip fracture.


Similar content being viewed by others
References
Adachi JD, Ioannidis G, Pickard L, Berger C, Prior JC, Joseph L, Hanley DA, Olszynski WP, Murray TM, Anastassiades T, Hopman W, Brown JP, Kirkland S, Joyce C, Papaioannou A, Poliquin S, Tenenhouse A, Papadimitropoulos EA (2003) The association between osteoporotic fractures and health-related quality of life as measured by the Health Utilities Index in the Canadian Multicentre Osteoporosis Study (CaMos). Osteoporos Int 14:895–904
Papaioannou A, Kennedy CC, Ioannidis G, Sawka A, Hopman WM, Pickard L, Brown JP, Josse RG, Kaiser S, Anastassiades T, Goltzman D, Papadimitropoulos M, Tenenhouse A, Prior JC, Olszynski WP, Adachi JD (2009) The impact of incident fractures on health-related quality of life: 5 years of data from the Canadian Multicentre Osteoporosis Study. Osteoporos Int 20:703–714
Oleksik AM, Ewing S, Shen W, van Schoor NM, Lips P (2005) Impact of incident vertebral fractures on health related quality of life (HRQOL) in postmenopausal women with prevalent vertebral fractures. Osteoporos Int 16:861–870
Lips P, Jameson K, Bianchi ML, Goemaere S, Boonen S, Reeve J, Stepan J, Johnell O, van Schoor NM, Dennison E, Kanis JA, Cooper C (2009) Validation of the IOF quality of life questionnaire for patients with wrist fracture. Osteoporos Int 21:61–70
Tosteson AN, Gabriel SE, Grove MR, Moncur MM, Kneeland TS, Melton LJ 3rd (2001) Impact of hip and vertebral fractures on quality-adjusted life years. Osteoporos Int 12:1042–1049
Ioannidis G, Papaioannou A, Hopman WM, Akhtar-Danesh N, Anastassiades T, Pickard L, Kennedy CC, Prior JC, Olszynski WP, Davison KS, Goltzman D, Thabane L, Gafni A, Papadimitropoulos EA, Brown JP, Josse RG, Hanley DA, Adachi JD (2009) Relation between fractures and mortality: results from the Canadian Multicentre Osteoporosis Study. CMAJ 181:265–271
Cummings SR, Melton LJ (2002) Epidemiology and outcomes of osteoporotic fractures. Lancet 359:1761–1767
Boonen S, Autier P, Barette M, Vanderschueren D, Lips P, Haentjens P (2004) Functional outcome and quality of life following hip fracture in elderly women: a prospective controlled study. Osteoporos Int 15:87–94
Haentjens P, Autier P, Barette M, Boonen S (2001) The economic cost of hip fractures among elderly women. A one-year, prospective, observational cohort study with matched-pair analysis. Belgian Hip Fracture Study Group. J Bone Joint Surg Am 83-A:493–500
Osnes EK, Lofthus CM, Meyer HE, Falch JA, Nordsletten L, Cappelen I, Kristiansen IS (2004) Consequences of hip fracture on activities of daily life and residential needs. Osteoporos Int 15:567–574
Magaziner J, Hawkes W, Hebel JR, Zimmerman SI, Fox KM, Dolan M, Felsenthal G, Kenzora J (2000) Recovery from hip fracture in eight areas of function. J Gerontol A Biol Sci Med Sci 55:M498–M507
Sawka AM, Thabane L, Papaioannou A, Gafni A, Ioannidis G, Papadimitropoulos EA, Hopman WM, Cranney A, Hanley DA, Pickard L, Adachi JD (2005) Health-related quality of life measurements in elderly Canadians with osteoporosis compared to other chronic medical conditions: a population-based study from the Canadian Multicentre Osteoporosis Study (CaMos). Osteoporos Int 16:1836–1840
Papaioannou A, Kennedy CC, Ioannidis G, Brown JP, Pathak A, Hanley DA, Josse RG, Sebaldt RJ, Olszynski WP, Tenenhouse A, Murray TM, Petrie A, Goldsmith CH, Adachi JD (2006) Determinants of health-related quality of life in women with vertebral fractures. Osteoporos Int 17:355–363
Silverman SL, Cranney A (1997) Quality of life measurement in osteoporosis. J Rheumatol 24:1218–1221
Silverman SL, Minshall ME, Shen W, Harper KD, Xie S (2001) The relationship of health-related quality of life to prevalent and incident vertebral fractures in postmenopausal women with osteoporosis: results from the Multiple Outcomes of Raloxifene Evaluation Study. Arthritis Rheum 44:2611–2619
The EuroQol Group (1990) EuroQol—a new facility for the measurement of health-related quality of life. Health Policy 16:199–208
Brooks R (1996) EuroQol: the current state of play. Health Policy 37:53–72
Brazier JE, Walters SJ, Nicholl JP, Kohler B (1996) Using the SF-36 and Euroqol on an elderly population. Qual Life Res 5:195–204
Dhillon V, Hurst N, Hannan J, Nuki G (2005) Association of low general health status, measured prospectively by Euroqol EQ5D, with osteoporosis, independent of a history of prior fracture. Osteoporos Int 16:483–489
Lyles KW, Colon-Emeric CS, Magaziner JS, Adachi JD, Pieper CF, Mautalen C, Hyldstrup L, Recknor C, Nordsletten L, Moore KA, Lavecchia C, Zhang J, Mesenbrink P, Hodgson PK, Abrams K, Orloff JJ, Horowitz Z, Eriksen EF, Boonen S (2007) Zoledronic acid and clinical fractures and mortality after hip fracture. N Engl J Med 357:1799–1809
Colon-Emeric CS, Caminis J, Suh TT, Pieper CF, Janning C, Magaziner J, Adachi J, Rosario-Jansen T, Mesenbrink P, Horowitz ZD, Lyles KW (2004) The HORIZON Recurrent Fracture Trial: design of a clinical trial in the prevention of subsequent fractures after low trauma hip fracture repair. Curr Med Res Opin 20:903–910
Rosen CJ, Brown S (2003) Severe hypocalcemia after intravenous bisphosphonate therapy in occult vitamin D deficiency. N Engl J Med 348:1503–1504
Guyatt GH, Feeny DH, Patrick DL (1993) Measuring health-related quality of life. Ann Intern Med 118:622–629
Dolan P (1997) Modeling valuations for EuroQol health states. Med Care 35:1095–1108
Oleksik A, Lips P, Dawson A, Minshall ME, Shen W, Cooper C, Kanis J (2000) Health-related quality of life in postmenopausal women with low BMD with or without prevalent vertebral fractures. J Bone Miner Res 15:1384–1392
Silverman SL, Piziak VK, Chen P, Misurski DA, Wagman RB (2005) Relationship of health related quality of life to prevalent and new or worsening back pain in postmenopausal women with osteoporosis. J Rheumatol 32:2405–2409
Meunier PJ, Roux C, Ortolani S, Diaz-Curiel M, Compston J, Marquis P, Cormier C, Isaia G, Badurski J, Wark JD, Collette J, Reginster JY (2009) Effects of long-term strontium ranelate treatment on vertebral fracture risk in postmenopausal women with osteoporosis. Osteoporos Int 20:1663–1673
Marquis P, Cialdella P, De la Loge C (2001) Development and validation of a specific quality of life module in post-menopausal women with osteoporosis: the QUALIOST. Qual Life Res 10:555–566
Acknowledgments
The authors thank Dr. Nandita Adhikary (Novartis Healthcare Pvt. Ltd.) for her assistance in writing the manuscript and incorporating authors’ comments into subsequent revisions. Dr. Boonen is a senior clinical investigator of the Fund for Scientific Research, Flanders, Belgium (F.W.O.-Vlaanderen) and holder of the Leuven University Chair in Gerontology and Geriatrics. This research was sponsored by Novartis Pharma AG, Basel, Switzerland.
Conflicts of interest
Dr. Adachi reports receiving consulting fees from Amgen, AstraZeneca, Eli Lilly, GlaxoSmithKline, Merck, Novartis, Pfizer, Procter & Gamble, Roche, Sanofi-Aventis, and Servier and grant support from Amgen, Eli Lilly, GlaxoSmithKline, Merck, Novartis, Pfizer, Procter & Gamble, and Roche.
Dr. Lyles, receiving grant support from Novartis, the Alliance for Better Bone Health (Sanofi-Aventis and Procter & Gamble), and Amgen, consulting fees from Novartis, Procter & Gamble, Merck, Amgen, GTx, GlaxoSmithKline, Eli Lilly, and Bone Medical, and being listed as an inventor on a U.S. patent application (20050272707) covering methods for preventing or reducing secondary fractures after hip fracture and on another provisional patent application for medication kits and formulations for preventing, treating, or reducing secondary fractures after a previous fracture.
Dr. Colón-Emeric, receiving consulting fees from Novartis, Amgen, and research grants from Novartis, Pfizer, and the Alliance for Better Bone Health.
Dr. Boonen, receiving consulting fees and research support from Novartis.
Dr. Pieper, receiving research support from Novartis.
Dr. Mautalen, receiving consulting and advisory board fees from Novartis.
Dr. Hyldstrup, receiving advisory board fees from Novartis, Eli Lilly, and Nycomed, lecture fees from Merck, Eli Lilly, Nycomed, Novartis, Novo Nordisk, and Servier, and grant support from Eli Lilly, Novartis, Pfizer, Nycomed, Roche, and GlaxoSmithKline.
Dr. Recknor, receiving consulting fees from Procter & Gamble, Roche, and Eli Lilly, lecture fees from Procter & Gamble, Eli Lilly, Roche, GlaxoSmithKline, Merck, and Aventis, and grant support from Procter & Gamble.
Dr. Nordsletten, receiving consulting and advisory board fees from Novartis and DePuy, lecture fees from Wyeth, and grant support from Biomet.
Dr. Bucci-Rechtweg and Dr. Su, being employees of and owning stock in Novartis.
Dr. Eriksen (now an employee of Oslo University, Oslo, Norway), being an employee of Novartis during the design and initiation of the study, and receiving advisory board fees from Novartis, Eli Lilly and Amgen.
Dr. Magaziner, receiving consulting fees from Amgen, Merck, Eli Lilly and Novartis, and grant support from Novartis and Merck.
Ms. Moore, no disclosures.
Author information
Authors and Affiliations
Corresponding author
Additional information
ClinicalTrials.gov registration number
NCT00046254
Rights and permissions
About this article
Cite this article
Adachi, J.D., Lyles, K.W., Colón-Emeric, C.S. et al. Zoledronic acid results in better health-related quality of life following hip fracture: the HORIZON–Recurrent Fracture Trial. Osteoporos Int 22, 2539–2549 (2011). https://doi.org/10.1007/s00198-010-1514-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-010-1514-9