Abstract
Purpose
Although different forms of lidocaine are used for migraine attack headaches, the effect of intravenous lidocaine is still limited. This study aimed to investigate the effects of intravenous lidocaine infusion for the treatment of migraine attack headaches.
Methods
A hundred patients with migraine attacks, aged between 18 and 65, were randomly divided into two groups. The lidocaine group (n = 50) received a 1.5 mg/kg lidocaine bolus and a 1 mg/kg infusion (first 30 min), followed by a 0.5 mg/kg infusion for a further 30 min intravenously. The non-steroidal anti-inflammatory drug (NSAID) group (n = 50) received 50 mg dexketoprofen trometamol and saline at the same volume as the lidocaine at the same time intervals intravenously. The Visual Analog Scale (VAS) pain scores, additional analgesia requirement, side effects, and revisits to the emergency department were recorded.
Results
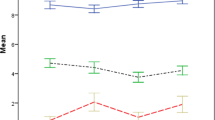
The VAS score was significantly lower in the lidocaine group than in the NSAID group for the first 20th and 30th minutes (p = 0.014 and p = 0.024, respectively). There was no difference between the VAS scores for the remaining evaluation times (p > 0.05). In terms of secondary outcomes, rescue medication requirement was not different between the two groups at both the 60th and 90th minutes (p > 0.05). However, the number of patients revisiting ED within 48–72 h was statistically less in the lidocaine group than in the NSAID group (1/50 vs. 8/50; p = 0.031).
Conclusion
Intravenous lidocaine may be an alternative treatment method for patients with migraine attack headaches in the emergency department.

Similar content being viewed by others
References
Becker WJ (2015) Acute migraine treatment in adults. Headache 55(6):778–793. https://doi.org/10.1111/head.12550
Robblee J, Grimsrud KW (2020) Emergency department and inpatient management of headache in adults. Curr Neurol Neurosci Rep 20(4):7. https://doi.org/10.1007/s11910-020-01030-w
Ong JJY, De Felice M (2018) Migraine treatment: current acute medications and their potential mechanisms of action. Neurotherapeutics 15(2):274–290. https://doi.org/10.1007/s13311-017-0592-1
Bilhimer MH, Groth ME, Holmes AK (2020) Ketamine for migraine in the emergency department. Adv Emerg Nurs J 42(2):96–102. https://doi.org/10.1097/tme.0000000000000296
Benish T, Villalobos D, Love S, Casmaer M, Hunter CJ, Summers SM, April MD (2019) The THINK (Treatment of Headache with Intranasal Ketamine) trial: a randomized controlled trial comparing intranasal ketamine with intravenous metoclopramide. J Emerg Med 56(3):248-257.e241. https://doi.org/10.1016/j.jemermed.2018.12.007
Beaussier M, Delbos A, Maurice-Szamburski A, Ecoffey C, Mercadal L (2018) Perioperative use of intravenous lidocaine. Drugs 78(12):1229–1246. https://doi.org/10.1007/s40265-018-0955-x
Ates İ, Aydin ME, Ahiskalioglu A, Ahiskalioglu EO, Kaya Z, Gozeler MS (2020) Postoperative analgesic efficacy of perioperative intravenous lidocaine infusion in patients undergoing septorhinoplasty: a prospective, randomized, double-blind study. Eur Arch Otorhinolaryngol 277(4):1095–1100. https://doi.org/10.1007/s00405-020-05801-6
Forster C, Vanhaudenhuyse A, Gast P, Louis E, Hick G, Brichant JF, Joris J (2018) Intravenous infusion of lidocaine significantly reduces propofol dose for colonoscopy: a randomised placebo-controlled study. Br J Anaesth 121(5):1059–1064. https://doi.org/10.1016/j.bja.2018.06.019
Ates I, Aydin ME, Albayrak B, Disci E, Ahiskalioglu EO, Celik EC, Baran O, Ahiskalioglu A (2020) Pre-procedure intravenous lidocaine administration on propofol consumption for ERCP: a prospective, randomized, double-blind study. J Gastroenterol Hepatol. https://doi.org/10.1111/jgh.15356
Akhgar A, Pouryousefi T, Nejati A, Rafiemanesh H, Hossein-Nejad H (2020) The efficacy of intravenous lidocaine and its side effects in comparison with intravenous morphine sulfate in patients admitted to the ED with right upper abdominal pain suspected of biliary colic. Am J Emerg Med. https://doi.org/10.1016/j.ajem.2020.04.010
Chinn E, Friedman BW, Naeem F, Irizarry E, Afrifa F, Zias E, Jones MP, Pearlman S, Chertoff A, Wollowitz A, Gallagher EJ (2019) Randomized trial of intravenous lidocaine versus hydromorphone for acute abdominal pain in the emergency department. Ann Emerg Med 74(2):233–240. https://doi.org/10.1016/j.annemergmed.2019.01.021
Johnson M, Strait L, Ata A, Bartscherer A, Miller C, Chang A, Stain SC, Tafen M (2020) Do lidocaine patches reduce opioid use in acute rib fractures? Am Surg 86(9):1153–1158. https://doi.org/10.1177/0003134820945224
Miller ACC, Faza C, Bigalli AAC, Khan AM, Sewell KA, King A, Vahedian-Azimi A, Zehtabchi S (2020) Intravenous amide anesthetics to treat pain associated with renal colic in the emergency department: a systematic review. Arch Acad Emerg Med 8(1):e27
Kandil E, Melikman E, Adinoff B (2017) Lidocaine infusion: a promising therapeutic approach for chronic pain. J Anesth Clin Res 8(1) https://doi.org/10.4172/2155-6148.1000697
Karadaş Ö, Gül HL, Inan LE (2013) Lidocaine injection of pericranial myofascial trigger points in the treatment of frequent episodic tension-type headache. J Headache Pain 14(1):44. https://doi.org/10.1186/1129-2377-14-44
Avcu N, Doğan N, Pekdemir M, Yaka E, Yılmaz S, Alyeşil C, Akalın LE (2017) Intranasal lidocaine in acute treatment of migraine: a randomized controlled trial. Ann Emerg Med 69(6):743–751. https://doi.org/10.1016/j.annemergmed.2016.09.031
Williams DR, Stark RJ (2003) Intravenous lignocaine (lidocaine) infusion for the treatment of chronic daily headache with substantial medication overuse. Cephalalgia 23(10):963–971. https://doi.org/10.1046/j.1468-2982.2003.00623.x
Matharu MS, Cohen AS, Goadsby PJ (2004) SUNCT syndrome responsive to intravenous lidocaine. Cephalalgia 24(11):985–992. https://doi.org/10.1111/j.1468-2982.2004.00886.x
Berk T, Silberstein SD (2018) The use and method of action of intravenous lidocaine and its metabolite in headache disorders. Headache 58(5):783–789. https://doi.org/10.1111/head.13298
Bell R, Montoya D, Shuaib A, Lee MA (1990) A comparative trial of three agents in the treatment of acute migraine headache. Ann Emerg Med 19(10):1079–1082. https://doi.org/10.1016/s0196-0644(05)81507-0
Masic D, Liang E, Long C, Sterk EJ, Barbas B, Rech MA (2018) Intravenous lidocaine for acute pain: a systematic review. Pharmacotherapy 38(12):1250–1259. https://doi.org/10.1002/phar.2189
Ayulo MA Jr, Phillips KE, Tripathi S (2018) Safety and efficacy of IV lidocaine in the treatment of children and adolescents with status migraine. Pediatr Crit Care Med 19(8):755–759. https://doi.org/10.1097/pcc.0000000000001629
Reutens DC, Fatovich DM, Stewart-Wynne EG, Prentice DA (1991) Is intravenous lidocaine clinically effective in acute migraine? Cephalalgia 11(6):245–247. https://doi.org/10.1046/j.1468-2982.1991.1106245.x
Kaube H, Hoskin KL, Goadsby PJ (1994) Lignocaine and headache: an electrophysiological study in the cat with supporting clinical observations in man. J Neurol 241(7):415–420. https://doi.org/10.1007/bf00900958
Orlando R, Piccoli P, De Martin S, Padrini R, Palatini P (2003) Effect of the CYP3A4 inhibitor erythromycin on the pharmacokinetics of lignocaine and its pharmacologically active metabolites in subjects with normal and impaired liver function. Br J Clin Pharmacol 55(1):86–93. https://doi.org/10.1046/j.1365-2125.2003.01718.x
Daykin H (2017) The efficacy and safety of intravenous lidocaine for analgesia in the older adult: a literature review. Br J Pain 11(1):23–31. https://doi.org/10.1177/2049463716676205
Gungor F, Akyol KC, Kesapli M, Celik A, Karaca A, Bozdemir MN, Eken C (2016) Intravenous dexketoprofen vs placebo for migraine attack in the emergency department: a randomized, placebo-controlled trial. Cephalalgia 36(2):179–184. https://doi.org/10.1177/0333102415584604
Rodríguez MJ, Arbós RM, Amaro SR (2008) Dexketoprofen trometamol: clinical evidence supporting its role as a painkiller. Expert Rev Neurother 8(11):1625–1640. https://doi.org/10.1586/14737175.8.11.1625
Kelley NE, Tepper DE (2012) Rescue therapy for acute migraine, part 3: opioids, NSAIDs, steroids, and post-discharge medications. Headache 52(3):467–482. https://doi.org/10.1111/j.1526-4610.2012.02097.x
Author information
Authors and Affiliations
Contributions
ST Akgol Gur, EO Ahiskalioglu: Planning, data collection, sample analysis, writing the first draft, evaluating and modifying the final manuscript. ME Aydin, AO Kocak: Data collection and evaluating subsequent drafts and the final manuscript. P. Aydin: Sample analysis, writing and the final manuscript. A. Ahiskalioglu: Writing and the final manuscript, supervisor.
Corresponding author
Ethics declarations
Ethic approval and patient consent
This study was conducted at the Ataturk University Faculty of Medicine, Erzurum, Turkey. It was approved by the local ethics board approval (B30.2ATA.0.01.00/462) and followed the Helsinki statement, and signed consent was obtained from all participants before the experiment.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gur, S.T.A., Ahiskalioglu, E.O., Aydin, M.E. et al. Intravenous lidocaine vs. NSAIDs for migraine attack in the ED: a prospective, randomized, double-blind study. Eur J Clin Pharmacol 78, 27–33 (2022). https://doi.org/10.1007/s00228-021-03219-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-021-03219-5