Abstract
Introduction
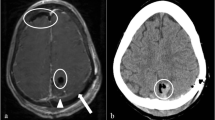
Syndrome of the trephined (ST) is a post-craniectomy complication. It is characterized by the appearance of new neurological symptoms following the craniectomy, which are relieved after cranioplasty. The purpose of our work was to identify radiological signs and imaging biomarkers of the ST.
Methods
CT images of 32 patients were retrospectively analyzed (ST = 13, controls = 19). While the shapes of craniectomy flap were qualitatively assessed, deviation of the midline structures, relative intracranial cerebrospinal fluid (CSF) volume, and the 3rd ventricle’s volume were quantitatively measured.
Results
We did not find between-group differences in the mean age or number of post-craniectomy days. ST was diagnosed during the second post-craniectomy month. The occurrence of a sunken skin flap sign was similar in both groups (69.23 % in ST group, 57.89 % in control group). Occurrence of paradoxical herniation and deviation of the midline structures were not significantly different between groups. Mean relative intracranial CSF volume was significantly smaller in ST patients (ST = 5.59 %, controls = 8.12 %, p = 0.01). ST patients, compared to controls, had also significantly smaller mean 3rd ventricle volumes (ST = 1748 mm3, controls = 2772.97 mm3, p = 0.03).
Conclusions
ST is an infrequent and delayed post-craniectomy complication. The most common radiological findings (paradoxical herniation, deviation of the midline structures, and sunken skin flap sign) might not be specific for ST. Significantly lower 3rd ventricle, and relative intracranial CSF volumes, suggest that altered biophysical CSF properties underlie ST pathophysiology. Therefore, volume measurements of 3rd ventricle could be useful for identification of patients who have higher probability of developing the ST.





Similar content being viewed by others
References
Grant FC, Norcross NC (1939) Repair of cranial defects by cranioplasty. Ann Surg 110(4):488–512
Annan M, Martin C, Dejobert M, de Toffol B, Hommet C, Mondon K (2014) Deterioration following craniectomy. Pract Neurol 14(4):266–267. doi:10.1136/practneurol-2013-000704
Carota A, Pintucci M, Zanchi F, D’Ambrosio E, Calabrese P (2011) ‘Cognitive’ sinking skin flap syndrome. Eur Neurol 66(4):227–228. doi:10.1159/000331939
Corallo F, Calabro RS, Leo A, Bramanti P (2015) Can cranioplasty be effective in improving cognitive and motor function in patients with chronic disorders of consciousness? A case report. Turk Neurosurg 25(1):193–196. doi:10.5137/1019-5149.JTN.10618-14.2
Dujovny M, Agner C, Aviles A (1999) Syndrome of the trephined: theory and facts. Crit Rev Neurosurg 9(5):271–278
Kumar GS, Chacko AG, Rajshekhar V (2004) Unusual presentation of the “syndrome of the trephined”. Neurol India 52(4):504–505
Richaud J, Boetto S, Guell A, Lazorthes Y (1985) Effects of cranioplasty on neurological function and cerebral blood flow. Neuro-Chirurgie 31(3):183–188
Schorl M (2009) Sinking skin flap syndrome (SSFS)—clinical spectrum and impact on rehabilitation. Cent Eur Neurosurg 70(2):68–72. doi:10.1055/s-0028-1093355
Stiver SI, Wintermark M, Manley GT (2008) Reversible monoparesis following decompressive hemicraniectomy for traumatic brain injury. J Neurosurg 109(2):245–254. doi:10.3171/JNS/2008/109/8/0245
Yamaura A, Makino H (1977) Neurological deficits in the presence of the sinking skin flap following decompressive craniectomy. Neurol Med Chir 17(1 Pt 1):43–53
Gottlob I, Simonsz-Toth B, Heilbronner R (2002) Midbrain syndrome with eye movement disorder: dramatic improvement after cranioplasty. Strabismus 10(4):271–277
Romero FR, Zanini MA, Ducati LG, Gabarra RC (2013) Sinking skin flap syndrome with delayed dysautonomic syndrome—an atypical presentation. Int J Surg Case Rep 4(11):1007–1009. doi:10.1016/j.ijscr.2013.08.013
Janzen C, Kruger K, Honeybul S (2012) Syndrome of the trephined following bifrontal decompressive craniectomy: implications for rehabilitation. Brain Inj 26(1):101–105. doi:10.3109/02699052.2011.635357
Fodstad H, Love JA, Ekstedt J, Friden H, Liliequist B (1984) Effect of cranioplasty on cerebrospinal fluid hydrodynamics in patients with the syndrome of the trephined. Acta Neurochir 70(1–2):21–30
Segal DH, Oppenheim JS, Murovic JA (1994) Neurological recovery after cranioplasty. Neurosurgery 34(4):729–731, discussion 731
Suzuki N, Suzuki S, Iwabuchi T (1993) Neurological improvement after cranioplasty. Analysis by dynamic CT scan. Acta Neurochir 122(1–2):49–53
Archavlis E, Carvi YNM (2012) The impact of timing of cranioplasty in patients with large cranial defects after decompressive hemicraniectomy. Acta Neurochir 154(6):1055–1062. doi:10.1007/s00701-012-1333-1
Ropper AH (1986) Lateral displacement of the brain and level of consciousness in patients with an acute hemispheral mass. New Eng J Med 314(15):953–958. doi:10.1056/NEJM198604103141504
Yushkevich PA, Piven J, Hazlett HC, Smith RG, Ho S, Gee JC, Gerig G (2006) User-guided 3D active contour segmentation of anatomical structures: significantly improved efficiency and reliability. NeuroImage 31(3):1116–1128. doi:10.1016/j.neuroimage.2006.01.015
Zweckberger K, Juettler E, Bosel J, Unterberg WA (2014) Surgical aspects of decompression craniectomy in malignant stroke: review. Cerebrovasc Dis 38(5):313–323. doi:10.1159/000365864
Sarov M, Guichard JP, Chibarro S, Guettard E, Godin O, Yelnik A, George B, Bousser MG, Vahedi K, investigators D (2010) Sinking skin flap syndrome and paradoxical herniation after hemicraniectomy for malignant hemispheric infarction. Stroke 41(3):560–562. doi:10.1161/STROKEAHA.109.568543
Choi JJ, Cirivello MJ, Neal CJ, Armonda RA (2011) Paradoxical herniation in wartime penetrating brain injury with concomitant skull-base trauma. J Craniofac Surg 22(6):2163–2167. doi:10.1097/SCS.0b013e3182323fd5
Fields JD, Lansberg MG, Skirboll SL, Kurien PA, Wijman CA (2006) “Paradoxical” transtentorial herniation due to CSF drainage in the presence of a hemicraniectomy. Neurology 67(8):1513–1514. doi:10.1212/01.wnl.0000242889.02957.b6
Isago T, Nozaki M, Kikuchi Y, Honda T, Nakazawa H (2004) Sinking skin flap syndrome: a case of improved cerebral blood flow after cranioplasty. Ann Plast Surg 53(3):288–292
Maeshima S, Kagawa M, Kishida Y, Kobayashi K, Makabe T, Morita Y, Kunishio K, Matsumoto A, Tsubahara A (2005) Unilateral spatial neglect related to a depressed skin flap following decompressive craniectomy. Eur Neurol 53(3):164–168. doi:10.1159/000086129
Nakamura T, Takashima T, Isobe K, Yamaura A (1980) Rapid neurological alteration associated with concave deformity of the skin flap in a craniectomized patient. Case report. Neurol Med Chir 20(1):89–93
Sinclair AG, Scoffings DJ (2010) Imaging of the post-operative cranium. Radiographics 30(2):461–482. doi:10.1148/rg.302095115
Stiver SI (2009) Complications of decompressive craniectomy for traumatic brain injury. Neurosurg Focus 26(6), E7. doi:10.3171/2009.4.FOCUS0965
Vilela MD (2008) Delayed paradoxical herniation after a decompressive craniectomy: case report. Surg Neurol 69(3):293–296. doi:10.1016/j.surneu.2007.01.027, discussion 296
Winkler PA, Stummer W, Linke R, Krishnan KG, Tatsch K (2000) Influence of cranioplasty on postural blood flow regulation, cerebrovascular reserve capacity, and cerebral glucose metabolism. J Neurosurg 93(1):53–61. doi:10.3171/jns.2000.93.1.0053
Yang XF, Wen L, Shen F, Li G, Lou R, Liu WG, Zhan RY (2008) Surgical complications secondary to decompressive craniectomy in patients with a head injury: a series of 108 consecutive cases. Acta Neurochir 150(12):1241–1247. doi:10.1007/s00701-008-0145-9, discussion 1248
Chalouhi N, Teufack S, Fernando Gonzalez L, Rosenwasser RH, Jabbour PM (2012) An extreme case of the syndrome of the trephined requiring the use of a novel titanium plate. Neurologist 18(6):423–425. doi:10.1097/NRL.0b013e318272f7be
Joseph V, Reilly P (2009) Syndrome of the trephined. J Neurosurg 111(4):650–652. doi:10.3171/2009.3.JNS0984
Ng D, Dan NG (1997) Cranioplasty and the syndrome of the trephined. J Clin Neurosci 4(3):346–348
Mokri B (2010) Orthostatic headaches in the syndrome of the trephined: resolution following cranioplasty. Headache 50(7):1206–1211. doi:10.1111/j.1526-4610.2010.01715.x
Sakamoto S, Eguchi K, Kiura Y, Arita K, Kurisu K (2006) CT perfusion imaging in the syndrome of the sinking skin flap before and after cranioplasty. Clin Neurol Neurosurg 108(6):583–585. doi:10.1016/j.clineuro.2005.03.012
Schiffer J, Gur R, Nisim U, Pollak L (1997) Symptomatic patients after craniectomy. Surg Neurol 47(3):231–237
Feigin VL, Theadom A, Barker-Collo S, Starkey NJ, McPherson K, Kahan M, Dowell A, Brown P, Parag V, Kydd R, Jones K, Jones A, Ameratunga S, Group BS (2013) Incidence of traumatic brain injury in New Zealand: a population-based study. Lancet Neurol 12(1):53–64. doi:10.1016/S1474-4422(12)70262-4
Akins PT, Guppy KH (2008) Sinking skin flaps, paradoxical herniation, and external brain tamponade: a review of decompressive craniectomy management. Neurocrit Care 9(2):269–276. doi:10.1007/s12028-007-9033-z
Hodozuka A, Takebayashi S, Nakai H, Hashizume K, Tanaka T (2000) A case of the syndrome of the sinking skin flap: case report. No shinkei Geka 28(3):245–249
Kemmling A, Duning T, Lemcke L, Niederstadt T, Minnerup J, Wersching H, Marziniak M (2010) Case report of MR perfusion imaging in sinking skin flap syndrome: growing evidence for hemodynamic impairment. BMC Neurol 10:80. doi:10.1186/1471-2377-10-80
Tabaddor K, LaMorgese J (1976) Complication of a large cranial defect. Case report. J Neurosurg 44(4):506–508. doi:10.3171/jns.1976.44.4.0506
Gschwind M, Michel P, Siclari F (2012) Life-threatening sinking skin flap syndrome due to CSF leak after lumbar puncture—treated with epidural blood patch. Eur J Neurol 19(5), e49. doi:10.1111/j.1468-1331.2012.03672.x
Han PY, Kim JH, Kang HI, Kim JS (2008) “Syndrome of the sinking skin-flap” secondary to the ventriculoperitoneal shunt after craniectomy. J Korean Neurosurg Soc 43(1):51–53. doi:10.3340/jkns.2008.43.1.51
Kwon SM, Cheong JH, Kim JM, Kim CH (2012) Reperfusion injury after autologous cranioplasty in a patient with sinking skin flap syndrome. J Korean Neurosurg Soc 51(2):117–119. doi:10.3340/jkns.2012.51.2.117
Oyelese AA, Steinberg GK, Huhn SL, Wijman CA (2005) Paradoxical cerebral herniation secondary to lumbar puncture after decompressive craniectomy for a large space-occupying hemispheric stroke: case report. Neurosurgery 57(3):E594, discussion E594
Klarica M, Rados M, Erceg G, Petosic A, Jurjevic I, Oreskovic D (2014) The influence of body position on cerebrospinal fluid pressure gradient and movement in cats with normal and impaired craniospinal communication. PloS One 9(4), e95229. doi:10.1371/journal.pone.0095229
Langfitt TW (1969) Increased intracranial pressure. Clin Neurosurg 16:436–471
Kelley GR, Johnson PL (2004) Sinking brain syndrome: craniotomy can precipitate brainstem herniation in CSF hypovolemia. Neurology 62(1):157
Komotar RJ, Mocco J, Ransom ER, Mack WJ, Zacharia BE, Wilson DA, Naidech AM, McKhann GM 2nd, Mayer SA, Fitzsimmons BF, Connolly ES Jr (2005) Herniation secondary to critical postcraniotomy cerebrospinal fluid hypovolemia. Neurosurgery 57(2):286–292, discussion 286–292
Mackenzie A, Shann F, Barnes G (1989) Clinical signs of dehydration in children. Lancet 2(8678–8679):1529–1530
Marin-Padilla M (2012) The human brain intracerebral microvascular system: development and structure. Front Neuroanat 6:38. doi:10.3389/fnana.2012.00038
Oreskovic D, Klarica M (2010) The formation of cerebrospinal fluid: nearly a hundred years of interpretations and misinterpretations. Brain Res Rev 64(2):241–262. doi:10.1016/j.brainresrev.2010.04.006
Guido LJ, Patterson RH Jr (1976) Focal neurological deficits secondary to intraoperative CSF drainage: successful resolution with an epidural blood patch. Report of two cases. J Neurosurg 45(3):348–351. doi:10.3171/jns.1976.45.3.0348
Zhao J, Li G, Zhang Y, Zhu X, Hou K (2015) Sinking skin flap syndrome and paradoxical herniation secondary to lumbar drainage. Clin Neurol Neurosurg 133:6–10. doi:10.1016/j.clineuro.2015.03.010
George AE, Morantz RA, Abad RM, Rovit RL, Chase N (1974) Neuroradiology of the posthemicraniectomy patient with special emphasis on the radiology of unilateral atrophy. Radiology 111(3):627–631. doi:10.1148/111.3.627
Probst MA, Baraff LJ, Hoffman JR, Wolfson AB, Ourian AJ, Mower WR (2009) Can patients with brain herniation on cranial computed tomography have a normal neurologic exam? Acad Emerg Med 16(2):145–150. doi:10.1111/j.1553-2712.2008.00312.x
Schmidt JH 3rd, Reyes BJ, Fischer R, Flaherty SK (2007) Use of hinge craniotomy for cerebral decompression. Technical note. J Neurosurg 107(3):678–682. doi:10.3171/JNS-07/09/0678
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
We declare that all human and animal studies have been approved by the Swiss Ethics Committees on research involving humans and have therefore been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. We declare that due to retrospective nature of this study, informed consent was waived.
Conflict of interest
We declare that we have no conflict of interest.
Additional information
Lana Vasung and Marion Hamard are joint first authors.
Rights and permissions
About this article
Cite this article
Vasung, L., Hamard, M., Soto, M.C.A. et al. Radiological signs of the syndrome of the trephined. Neuroradiology 58, 557–568 (2016). https://doi.org/10.1007/s00234-016-1651-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-016-1651-8