Abstract
Purpose
A major concern for patients undergoing reverse total shoulder arthroplasty (RTSA) is managing toileting after surgery. The goals of this systematic review of RTSA studies were to determine the following: (1) the percentage of patients who can manage toileting, (2) their degree of difficulty with toileting, and (3) the percentage of patients who can manage toileting after bilateral versus unilateral RTSA.
Methods
Medline, EMBASE, Google Scholar, and the Cochrane Central Register of Controlled Trials were searched for studies reporting the ability to manage toileting after RTSA. Six studies with at least 12 months of follow-up were included, yielding 183 patients (105 unilateral RTSA, 78 bilateral RTSA). We pooled patient data and calculated the weighted mean proportion of patients able to manage toileting, those who reported difficulty, and those able to manage toileting after unilateral versus bilateral RTSA. Statistical significance was set at P < 0.05.
Results
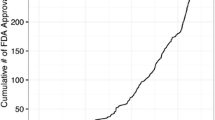
Most patients (92%; 95% confidence interval, 87–95%) were able to manage toileting after RTSA. Some degree of difficulty with toileting was reported for 20% of all shoulders. Almost all patients with bilateral RTSA were able to manage toileting with at least one arm (weighted mean proportion 97%; 95% confidence interval, 88–99%). There was no significant difference in the proportion of patients able to manage toileting after unilateral versus bilateral RTSA (P = 0.08). Only 3% of all papers published on the clinical results of RTSA by June 2017 reported upon toileting after the procedure.
Conclusions
With the available evidence, most patients were able to manage toileting after RTSA, although one-fifth reported some degree of difficulty. Ability to manage toileting was similar after unilateral versus bilateral RTSA. In the future, this variable should be a standard question after shoulder arthroplasty.
Level of evidence
IV

Similar content being viewed by others
References
Boileau P, Watkinson D, Hatzidakis AM, Hovorka I (2006) Neer Award 2005: the Grammont reverse shoulder prosthesis: results in cuff tear arthritis, fracture sequelae, and revision arthroplasty. Journal of Shoulder and Elbow Surgery/American Shoulder and Elbow Surgeons [et al] 15 5:527–540. doi:https://doi.org/10.1016/j.jse.2006.01.003
Favard L, Katz D, Colmar M, Benkalfate T, Thomazeau H, Emily S (2012) Total shoulder arthroplasty—arthroplasty for glenohumeral arthropathies: results and complications after a minimum follow-up of 8 years according to the type of arthroplasty and etiology. Orthopaedics & Traumatology, Surgery & Research: OTSR 98 4 Suppl:S41–47. doi:https://doi.org/10.1016/j.otsr.2012.04.003
Wall B, Nove-Josserand L, O'Connor DP, Edwards TB, Walch G (2007) Reverse total shoulder arthroplasty: a review of results according to etiology. J Bone Joint Surg Am 89(7):1476–1485. https://doi.org/10.2106/jbjs.f.00666
Roy JS, Macdermid JC, Goel D, Faber KJ, Athwal GS, Drosdowech DS (2010) What is a successful outcome following reverse total shoulder arthroplasty? The Open Orthopaedics Journal 4:157–163. https://doi.org/10.2174/1874325001004010157
Torrens C, Guirro P, Santana F (2016) The minimal clinically important difference for function and strength in patients undergoing reverse shoulder arthroplasty. J Shoulder Elb Surg 25(2):262–268. https://doi.org/10.1016/j.jse.2015.07.020
Chen AL, Bain EB, Horan MP, Hawkins RJ (2007) Determinants of patient satisfaction with outcome after shoulder arthroplasty. Journal of Shoulder and Elbow Surgery/American Shoulder and Elbow Surgeons [et al] 16 1:25–30. doi:https://doi.org/10.1016/j.jse.2006.04.013
Triplet JJ, Everding NG, Levy JC, Moor MA (2015) Functional internal rotation after shoulder arthroplasty: a comparison of anatomic and reverse shoulder arthroplasty. J Shoulder Elb Surg 24(6):867–874. https://doi.org/10.1016/j.jse.2014.10.002
Mellano CR, Kupfer N, Thorsness R, Chalmers PN, Feldheim TF, O'Donnell P, Cole BJ, Verma NN, Romeo AA, Nicholson GP (2017) Functional results of bilateral reverse total shoulder arthroplasty. J Shoulder Elb Surg 26(6):990–996. https://doi.org/10.1016/j.jse.2016.10.011
Grassi FA, Murena L, Valli F, Alberio R (2009) Six-year experience with the Delta III reverse shoulder prosthesis. Journal of Orthopaedic Surgery (Hong Kong) 17(2):151–156
Stevens CG, Struk AM, Wright TW (2014) The functional impact of bilateral reverse total shoulder arthroplasty. J Shoulder Elb Surg 23(9):1341–1348. https://doi.org/10.1016/j.jse.2013.12.012
Wiater BP, Boone CR, Koueiter DM, Wiater JM (2013) Early outcomes of staged bilateral reverse total shoulder arthroplasty: a case-control study. The Bone & Joint Journal 95-B(9):1232–1238. https://doi.org/10.1302/0301-620x.95b9.31445
Namdari S, Yagnik G, Ebaugh DD, Nagda S, Ramsey ML, Williams GR Jr, Mehta S (2012) Defining functional shoulder range of motion for activities of daily living. J Shoulder Elb Surg 21(9):1177–1183. https://doi.org/10.1016/j.jse.2011.07.032
Vasen AP, Lacey SH, Keith MW, Shaffer JW (1995) Functional range of motion of the elbow. The Journal of Hand Surgery 20(2):288–292. https://doi.org/10.1016/s0363-5023(05)80028-0
Mallon WJ, Herring CL, Sallay PI, Moorman CT, Crim JR (1996) Use of vertebral levels to measure presumed internal rotation at the shoulder: a radiographic analysis. J Shoulder Elb Surg 5(4):299–306. https://doi.org/10.1016/S1058-2746(96)80057-7
Ginn KA, Cohen ML, Herbert RD (2006) Does hand-behind-back range of motion accurately reflect shoulder internal rotation? J Shoulder Elb Surg 15(3):311–314. https://doi.org/10.1016/j.jse.2005.08.005
Edwards TB, Bostick RD, Greene CC, Baratta RV, Drez D (2002) Interobserver and intraobserver reliability of the measurement of shoulder internal rotation by vertebral level. J Shoulder Elb Surg 11(1):40–42. https://doi.org/10.1067/mse.2002.119853
Wakabayashi I, Itoi E, Minagawa H, Kobayashi M, Seki N, Shimada Y, Okada K (2006) Does reaching the back reflect the actual internal rotation of the shoulder? J Shoulder Elb Surg 15(3):306–310. https://doi.org/10.1016/j.jse.2005.08.022
Michener LA, McClure PW, Sennett BJ (2002) American Shoulder and Elbow Surgeons Standardized Shoulder Assessment Form, patient self-report section: reliability, validity, and responsiveness. Journal of Shoulder and Elbow Surgery/American Shoulder and Elbow Surgeons [et al] 11 6:587–594. doi:https://doi.org/10.1067/mse.2002.127096
Leggin BG, Michener LA, Shaffer MA, Brenneman SK, Iannotti JP, Williams GR Jr (2006) The Penn shoulder score: reliability and validity. The Journal of Orthopaedic and Sports Physical Therapy 36(3):138–151. https://doi.org/10.2519/jospt.2006.36.3.138
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med 6(7):e1000100. https://doi.org/10.1371/journal.pmed.1000100
Kemp AL, King JJ, Farmer KW, Wright TW (2016) Reverse total shoulder arthroplasty in wheelchair-dependent patients. J Shoulder Elb Surg 25(7):1138–1145. https://doi.org/10.1016/j.jse.2015.11.006
Maier MW, Zeifang F, Caspers M, Dreher T, Klotz MC, Rettig O, Wolf SI, Kasten P (2015) Can reverse shoulder arthroplasty in post-traumatic revision surgery restore the ability to perform activities of daily living? Orthopaedics & Traumatology, Surgery & Research: OTSR 101(2):191–196. https://doi.org/10.1016/j.otsr.2014.12.007
Morris BJ, Haigler RE, O'Connor DP, Elkousy HA, Gartsman GM, Edwards TB (2015) Outcomes of staged bilateral reverse shoulder arthroplasties for rotator cuff tear arthropathy. J Shoulder Elb Surg 24(3):474–481. https://doi.org/10.1016/j.jse.2014.08.008
Wright JG, Swiontkowski MF, Heckman JD (2003) Introducing levels of evidence to the journal. J Bone Joint Surg Am 85(1):1–3
Guyatt G, Oxman AD, Akl EA, Kunz R, Vist G, Brozek J, Norris S, Falck-Ytter Y, Glasziou P, DeBeer H, Jaeschke R, Rind D, Meerpohl J, Dahm P, Schunemann HJ (2011) GRADE guidelines: 1. Introduction-GRADE evidence profiles and summary of findings tables. J Clin Epidemiol 64(4):383–394. https://doi.org/10.1016/j.jclinepi.2010.04.026
Funding
There was no external source of funding for this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
For this type of study, formal consent is not required.
Informed consent
Not applicable.
Rights and permissions
About this article
Cite this article
Rojas, J., Joseph, J., Liu, B. et al. Can patients manage toileting after reverse total shoulder arthroplasty? A systematic review. International Orthopaedics (SICOT) 42, 2423–2428 (2018). https://doi.org/10.1007/s00264-018-3900-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-3900-4