Abstract
Background
Endoscopic thyroidectomy has comparable surgical outcomes and superior cosmetic satisfaction to open thyroidectomy. However, steep learning curve is a concern. This study evaluated the learning curve of endoscopic thyroidectomy using various parameters and statistical methods.
Methods
A total of 90 consecutive patients who underwent endoscopic thyroidectomy using bilateral axillo-breast approach (BABA) between March 2016 and April 2020 were enrolled. Operative time, postoperative drainage amount, and blood loss were assessed by cumulative sum (CUSUM) analysis and moving average to evaluate the learning curve.
Results
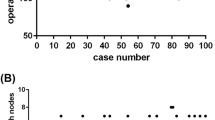
Using the CUSUM analysis, the peak point of both operative time and drainage amount occurred at the 30th case. No clear single peak was identified in the CUSUM plot for blood loss. The moving average also showed significant reduction in operative time and drainage amount after, approximately, the first 30 cases. The blood loss decreased after the 25th case. We therefore divided the patients into 2 phases: phase 1 (1–30 cases) and phase 2 (31–90 cases). The operative time, drainage amount, and blood loss decreased significantly in the phase 2 compared with phase 1. Lower pain score in first postoperative day and shorter hospital stay were also observed in the phase 2. Although the reduction in transient hypoparathyroidism did not reach statistical significance, no permanent hypoparathyroidism was noted in the phase 2.
Conclusions
The learning curve for endoscopic thyroidectomy is approximately 30 cases. Aside from the operative time, drainage amount may also serve as a surrogate for the learning curve evaluation.






Similar content being viewed by others
References
Johri G, Chand G, Mishra A et al (2020) Endoscopic versus conventional thyroid surgery: a comparison of quality of life, cosmetic outcomes and overall patient satisfaction with treatment. World J Surg 44(12):4118–4126
Cho MJ, Park KS, Cho MJ et al (2015) A comparative analysis of endoscopic thyroidectomy versus conventional thyroidectomy in clinically lymph node negative thyroid cancer. Ann Surg Treat Res 88:69–76
ImKoo doPaeng HJHJC et al (2012) Evaluation of surgical completeness in endoscopic thyroidectomy compared with open thyroidectomy with regard to remnant ablation. Clin Nucl Med 37:148–151
BaeKoo doChoi DSHJY et al (2014) Current status of robotic thyroid surgery in South Korea: a web-based survey. World J Surg 38:2632–2639
Yu J, Rao S, Lin Z et al (2019) The learning curve of endoscopic thyroid surgery for papillary thyroid microcarcinoma: CUSUM analysis of a single surgeon’s experience. Surg Endosc 33:1284–1289
Lee DY, Oh DJ, Kang KR et al (2016) Comparison of learning curves for retroauricular and transaxillary endoscopic hemithyroidectomy. Ann Surg Oncol 23:4023–4028
Luo JH, Xiang C, Wang P et al (2020) The learning curve for transoral endoscopic thyroid surgery: a single surgeon’s 204 case experience. J Laparoendosc Adv Surg Tech A 30:163–169
Razavi CR, Vasiliou E, Tufano RP et al (2018) Learning curve for transoral endoscopic thyroid lobectomy. Otolaryngol Head Neck Surg 159:625–629
Liu S, Qiu M, Jiang DZ et al (2009) The learning curve for endoscopic thyroidectomy: a single surgeon’s experience. Surg Endosc 23:1802–1806
Lee J, Yun JH, Choi UJ et al (2012) Robotic versus endoscopic thyroidectomy for thyroid cancers: a multi-institutional analysis of early postoperative outcomes and surgical learning curves. J Oncol 2012:734541
Kim WW, Jung JH, Park HY (2015) A single surgeon’s experience and surgical outcomes of 300 robotic thyroid surgeries using a bilateral axillo-breast approach. J Surg Oncol 111:135–140
Liao HJ, Dong C, Kong FJ et al (2014) The CUSUM analysis of the learning curve for endoscopic thyroidectomy by the breast approach. Surg Innov 21:221–228
Kassite I, Bejan-Angoulvant T, Lardy H et al (2019) A systematic review of the learning curve in robotic surgery: range and heterogeneity. Surg Endosc 33:353–365
Kim WW, Jung JH, Park HY (2015) The learning curve for robotic thyroidectomy using a bilateral axillo-breast approach from the 100 cases. Surg Laparosc Endosc Percutan Tech 25:412–416
Choi JY, Lee KE, Chung KW et al (2012) Endoscopic thyroidectomy via bilateral axillo-breast approach (BABA): review of 512 cases in a single institute. Surg Endosc 26:948–955
Zhu H, Wu L, Yuan R et al (2018) Learning curve for performing choledochotomy bile duct exploration with primary closure after laparoscopic cholecystectomy. Surg Endosc 32:4263–4270
Liu SY, Kim JS (2017) Bilateral axillo-breast approach robotic thyroidectomy: review of evidences. Gland Surg 6:250–257
Lira RB, Ramos AT, Nogueira RMR et al (2020) Transoral thyroidectomy (TOETVA): complications, surgical time and learning curve. Oral Oncol 110:104871
Anuwong A, Ketwong K, Jitpratoom P et al (2018) Safety and outcomes of the transoral endoscopic thyroidectomy vestibular approach. JAMA Surg 153:21–27
Russell JO, Razavi CR, Al Khadem MG et al (2018) Anterior cervical incision-sparing thyroidectomy: comparing retroauricular and transoral approaches. Laryngoscope Investig Otolaryngol 3:409–414
Lee HS, Chai YJ, Kim SJ et al (2016) Influence of body habitus on the surgical outcomes of bilateral axillo-breast approach robotic thyroidectomy in papillary thyroid carcinoma patients. Ann Surg Treat Res 91:1–7
Liang TJ, Liu SI, Mok KT et al (2016) Associations of volume and thyroidectomy outcomes: a nationwide study with systematic review and meta-analysis. Otolaryngol Head Neck Surg 155:65–75
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liang, TJ., Tsai, CY., Liu, SI. et al. Multidimensional Analyses of the Learning Curve of Endoscopic Thyroidectomy. World J Surg 45, 1446–1456 (2021). https://doi.org/10.1007/s00268-021-05953-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-021-05953-4