Abstract
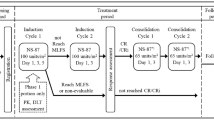
High-dose chemotherapy with autologous transplantation of in vivo purged PBSC is a novel investigational approach to treating chronic myelogenous leukemia (CML) patients not responsive to conventional therapy with interferon-α (IFN-α) and not eligible for allogeneic transplantation. PBSC mobilization using either '5+2/7+3'-type chemotherapy or 'mini-ICE/ICE' chemotherapy was investigated in 43 patients with advanced phases of Philadelphia (Ph)-positive CML. Thirty patients were in late chronic phase (>12 months post diagnosis) and 13 patients in accelerated phase (AP) or blast crisis (BC). Contamination with Ph-positive cells was evaluated in harvests from 37/43 patients. The outcome of PBSC mobilization was dependent on the type of chemotherapy administered: a complete or major cytogenetic response (<35% Ph-positive metaphases) in leukapheresis collections was obtained in ten of 15 patients treated with 'mini-ICE/ICE' but in only three of 28 patients treated with '5+2/7+3' chemotherapy. One patient (1/43) in blast crisis died during mobilization therapy (2%). Twenty-five patients underwent PBSC transplantation and all of them engrafted successfully. Transplantation-related mortality was 0%. The data show that in advanced phases of CML the chance of harvesting Ph-negative peripheral blood stem cells depends on the type of chemotherapy used for mobilization.
Similar content being viewed by others
Author information
Authors and Affiliations
Additional information
Received: February 6, 1998 / Accepted: May 19, 1998
Rights and permissions
About this article
Cite this article
Fischer, T., Neubauer, A., Mohm, J. et al. Outcome of peripheral blood stem cell mobilization in advanced phases of CML is dependent on the type of chemotherapy applied. Ann Hematol 77, 21–26 (1998). https://doi.org/10.1007/s002770050406
Issue Date:
DOI: https://doi.org/10.1007/s002770050406