Abstract
Purpose
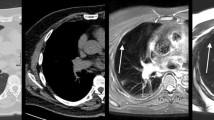
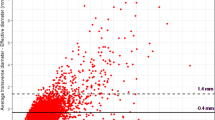
To evaluate MRI for lung cancer screening comparing LDCT- and MRI-derived Lung-RADS categories in the first two screening rounds.
Materials and methods
224 participants in a lung cancer screening study were examined with MRI and low-dose CT (LDCT). Acquired MRI sequences were T2, balanced, T1 and DWI. MRI was prospectively analysed regarding nodules. Minimum nodule size was 4 mm. Nodules were assigned a Lung-RADS score based on appearance and size at baseline and after 3, 6 and 12 months. MRI findings were correlated with LDCT.
Results
The early recall rate dropped from 13.8% at baseline to 1.9% in the second screening round with biopsy rates of 3.6% in the first round and 0.5% in the second round. Histology revealed lung cancer in 8/9 participants undergoing biopsy/surgery. All eight cancers were accurately depicted by MRI. The following categories were assigned on MRI (results of LDCT in parentheses): 4B/4X in 10 (10) cases, 4A in 16 (15) cases, 3 in 13 (12) cases, 2 in 77 (92) cases and 1 in 140 (126) cases. Lung-RADS scoring correlated significantly between MRI and CT. The score was overestimated by MRI in one case for category 4A, in two cases for category 3 and in five cases for category 2. MRI-based Lung-RADS score was underestimated for category 1 in 20 cases.
Conclusion
Lung-RADS might be applied for lung cancer screening with MRI, since findings correlated with LDCT. Relevant findings with a Lung-RADS score of 3 and higher were never missed or underestimated by MRI
Key Points
• MRI performed comparably to low-dose CT in a lung cancer-screening programme.
• Lung-RADS might be applied for lung cancer screening with MRI.
• Lung-RADS findings score of 3 and higher were never missed by MRI.





Similar content being viewed by others
Abbreviations
- DWI:
-
Diffusion-weighted imaging
- LDCT:
-
Low-dose computed tomography
- Lung-RADS:
-
Lung Screening Reporting and Data System
- MVXD:
-
MultiVane XD (Philips Healthcare, Best, The Netherlands)
- NSCLC:
-
Non-small cell lung cancer
- SCLC:
-
Small cell lung cancer
- THRIVE T1:
-
High Resolution Isotropic Volume Excitation (Philips Healthcare)
References
National Lung Screening Trial Research Team, Aberle DR, Adams AM et al (2011) Reduced lung-cancer mortality with low-dose computed tomographic screening. N Engl J Med 365(5):395–409
American College of Radiology. Lung CT Screening Reporting and Data System (Lung-RADS). Available at: http://www.acr.org/ Quality-Safety/Resources/LungRADS. Accessed 30 Nov 2017
McKee BJ, Regis SM, McKee AB, Flacke S, Wald C (2016) Performance of ACR Lung-RADS in a clinical CT lung screening program. J Am Coll Radiol 13(2 Suppl):R25–R29. https://doi.org/10.1016/j.jacr.2015.12.009
Wielpütz M, Kauczor HU (2012) MRI of the lung: state of the art. Diagn Interv Radiol 18(4):344–353
Wild JM, Marshall H, Bock M et al (2012) MRI of the lung (1/3): methods. Insights Imaging 3(4):345–353
Biederer J, Beer M, Hirsch W et al (2012) MRI of the lung (2/3). Why … when … how? Insights Imaging 3(4):355–371
Biederer J, Ohno Y, Hatabu H et al (2017) Screening for lung cancer: Does MRI have a role? Eur J Radiol 86:353–360
Sommer G, Tremper J, Koenigkam-Santos M et al (2014) Lung nodule detection in a high-risk population: comparison of magnetic resonance imaging and low-dose computed tomography. Eur J Radiol 83(3):600–605
Meier-Schroers M, Homsi R, Skowasch D, Buermann J, Zipfel M, Schild HH, Thomas D (2017) Lung cancer screening with MRI: results of the first screening round. J Cancer Res Clin Oncol. https://doi.org/10.1007/s00432-017-2521-4
Becker N, Motsch E, Gross ML et al (2012) Randomized study on early detection of lung cancer with MSCT in Germany: study design and results of the first screening round. J Cancer Res Clin Oncol 138(9):1475–1486
Gierada DS, Pinsky P, Nath H, Chiles C, Duan F, Aberle DR (2014) Projected outcomes using different nodule sizes to define a positive CT lung cancer screening examination. J Natl Cancer Inst 106(11):dju284. https://doi.org/10.1093/jnci/dju284
Cieszanowski A, Lisowska A, Dabrowska M et al (2016) MR imaging of pulmonary nodules: detection rate and accuracy of size estimation in comparison to computed tomography. PLoS One 11(6):e0156272
Koyama H, Ohno Y, Seki S et al (2013) Magnetic resonance imaging for lung cancer. J Thorac Imaging 28(3):138–150
Bruegel M, Gaa J, Woertler K et al (2007) MRI of the lung: value of different turbo spin-echo, single-shot turbo spinecho, and 3D gradient-echo pulse sequences for the detection of pulmonary metastases. J Magn Reson Imaging 25(1):73–81
MacMahon H, Naidich DP, Goo JM et al (2017) Guidelines for management of incidental pulmonary nodules detected on CT images: From the Fleischner Society 2017. Radiology 284(1):228–243
Becker N, Motsch E, Gross ML et al (2015) Randomized study on early detection of lung cancer with MSCT in Germany: Results of the first 3 years of follow-up after randomization. J Thorac Oncol 10(6):890–896
Grabler P, Sighoko D, Wang L, Allgood K, Ansell D (2017) Recall and cancer detection rates for screening mammography: Finding the sweet spot. AJR Am J Roentgenol 208(1):208–213
Callister ME, Baldwin DR, Akram AR et al (2015) British Thoracic Society guidelines for the investigation and management of pulmonary nodules. Thorax 70(Suppl 2):ii1–ii54
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Daniel Thomas.
Conflict of interest
One co-author of this manuscript, Jürgen Gieseke, is an employee of Philips Healthcare Germany. However, he did not have any influence on the study design, evaluation or interpretation of results. His main contribution was optimising the MR sequences and reviewing the manuscript.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was obtained from all patients in this study.
Ethical approval
Institutional Review Board approval was obtained.
Study subjects or cohorts overlap
All study subjects are participants of our lung cancer screening program. The performance of MRI regarding the detection of lung nodules in the first screening round were published in 2017 (Meier-Schroers M, Homsi R, Skowasch D, Buermann J, Zipfel M, Schild HH, Thomas D. Lung cancer screening with MRI: results of the first screening round. J Cancer Res Clin Oncol. 2017 Sep 20. [Epub ahead of print]). The current study reports on the first two screening rounds including all follow-ups and on the applicability of the Lung-RADS classification.
Methodology
• prospective
• diagnostic study
• performed at one institution
Electronic supplementary material
ESM 1
(DOCX 3557 kb)
Rights and permissions
About this article
Cite this article
Meier-Schroers, M., Homsi, R., Gieseke, J. et al. Lung cancer screening with MRI: Evaluation of MRI for lung cancer screening by comparison of LDCT- and MRI-derived Lung-RADS categories in the first two screening rounds. Eur Radiol 29, 898–905 (2019). https://doi.org/10.1007/s00330-018-5607-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-018-5607-8