Abstract
Purpose
This study aimed to develop a prediction model to identify risk factors for post-operative acute pancreatitis (POAP) in children with pancreaticobiliary maljunction (PBM) by pre-operative analysis of patient variables.
Methods
Logistic regression (LR), support vector machine (SVM), and extreme gradient boosting (XGBoost) models were established using the prospectively collected databases of patients with PBM undergoing surgery which was reviewed in the period comprised between August 2015 and August 2022, at the Children’s Hospital of Soochow University. Primarily, the area beneath the receiver-operating curves (AUC), accuracy, sensitivity, and specificity were used to evaluate the model performance. The model was finally validated using the nomogram and clinical impact curve.
Results
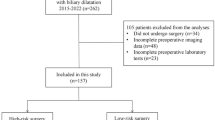
In total, 111 children with PBM met the inclusion criteria, and 21 children suffered POAP. In the validation dataset, LR models showed the highest performance. The risk nomogram and clinical effect curve demonstrated that the LR model was highly predictive.
Conclusion
The prediction model based on the LR with a nomogram could be used to predict the risk of POAP in patients with PBM. Protein plugs, age, white blood cell count, and common bile duct diameter were the most relevant contributing factors to the models.







Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Kamisawa T, Ando H, Hamada Y, Fujii H, Koshinaga T, Urushihara N, Itoi T, Shimada H (2014) Diagnostic criteria for pancreaticobiliary maljunction 2013. J Hepatobiliary Pancreat Sci 21:159–161. https://doi.org/10.1002/jhbp.57
Shimotakahara A, Yamataka A, Yanai T, Kobayashi H, Okazaki T, Lane GJ, Miyano T (2005) Roux-en-Y hepaticojejunostomy or hepaticoduodenostomy for biliary reconstruction during the surgical treatment of choledochal cyst: which is better? Pediatr Surg Int 21:5–7. https://doi.org/10.1007/s00383-004-1252-1
Shi LB, Peng SY, Meng XK, Peng CH, Liu YB, Chen XP, Ji ZL, Yang DT, Chen HR (2001) Diagnosis and treatment of congenital choledochal cyst: 20 years’ experience in China. World J Gastroenterol 7:732–734. https://doi.org/10.3748/wjg.v7.i5.732
Li L, Feng W, Jing-Bo F, Qi-Zhi Y, Gang L, Liu-Ming H, Yu L, Jun J, Ping W (2004) Laparoscopic-assisted total cyst excision of choledochal cyst and Roux-en-Y hepatoenterostomy. J Pediatr Surg 39:1663–1666. https://doi.org/10.1016/j.jpedsurg.2004.07.01
Roberts SE, Morrison-Rees S, John A, Williams JG, Brown TH, Samuel DG (2017) The incidence and aetiology of acute pancreatitis across Europe. Pancreatology 17:155–165. https://doi.org/10.1016/j.pan.2017.01.005
Deo RC (2015) Machine learning in medicine. Circulation 132:1920–1930. https://doi.org/10.1161/CIRCULATIONAHA.115.001593
Jiang F, Jiang Y, Zhi H, Dong Y, Li H, Ma S, Wang Y, Dong Q, Shen H, Wang Y (2017) Artificial intelligence in healthcare: past, present and future. Stroke Vasc Neurol 2(4):230–243. https://doi.org/10.1136/svn-2017-000101
Rajkomar A, Dean J, Kohane I (2019) Machine learning in medicine. N Engl J Med 380:1347–1358. https://doi.org/10.1056/NEJMra1814259
Lecun Y, Bengio Y, Hinton G (2015) Deep learning. Nature 521:436–444. https://doi.org/10.1038/nature14539
Han X, Geng J, Zhang XX, Zhao L, Wang J, Guo WL (2022) Using machine learning models to predict acute pancreatitis in children with pancreaticobiliary maljunction. Surg Today. https://doi.org/10.1007/s00595-022-02571-y
Todani T, Watanabe Y, Narusue M, Tabuchi K, Okajima K (1977) Congenital bile duct cysts: classification, operative procedures, and review of thirty-seven cases including cancer arising from choledochal cyst. Am J Surg 134:263–269. https://doi.org/10.1016/0002-9610(77)90359-2
Morinville VD, Husain SZ, Bai H, Barth B, Alhosh R, Durie PR, Freedman SD, Himes R, Lowe ME, Pohl J et al (2012) Definitions of pediatric pancreatitis and survey of present clinical practices. J Pediatr Gastroenterol Nutr 55:261–265. https://doi.org/10.1097/MPG.0b013e31824f1516
Yuan KC, Tsai LW, Lee KH, Cheng YW, Hsu SC, Lo YS, Chen RJ (2020) The development anartificial intelligence algorithm for early sepsis diagnosis in the intensive care unit. Int J Med Inform 141:104176. https://doi.org/10.1016/j.ijmednf.2020.104176
Sidey-Gibbons J, Sidey-Gibbons CJ (2019) Machine learning in medicine: a practical introduction. BMC Med Res Methodol 19:64. https://doi.org/10.1186/s12874-019-0681-4
Yamataka A, Ohshiro K, Okada Y, Hosoda Y, Fujiwara T, Kohno S, Sunagawa M, Futagawa S, Sakakibara N, Miyano T (1997) Complications after cyst excision with hepaticoenterostomy for choledochal cysts and their surgical management in children versus adults. J Pediatr Surg 32:1097–1102. https://doi.org/10.1016/s0022-3468(97)90407-3
Miyano T, Yamataka A, Kato Y, Segawa O, Lane G, Takamizawa S, Kohno S, Fujiwara T (1996) Hepaticoenterostomy after excision of choledochal cyst in children: a 30-year experience with 180 cases. J Pediatr Surg 31:1417–1421. https://doi.org/10.1016/s0022-3468(96)90843-x
Gross V, Leser HG, Heinisch A, Schölmerich J (1993) Inflammatory mediators and cytokines–new aspects of the pathophysiology and assessment of severity of acute pancreatitis? Hepatogastroenterology 40:522–530. https://doi.org/10.1055/s-2008-1066049
Afzal S, Kleinhenz J (2021) Acute pancreatitis in children. Pediatr Ann 50:e330–e335. https://doi.org/10.3928/19382359-20210713-01
Qiu Q, Nian YJ, Guo Y, Tang L, Lu N, Wen LZ, Wang B, Chen DF, Liu KJ (2019) Development and validation of three machine-learning models for predicting multiple organ failure in moderately severe and severe acute pancreatitis. BMC Gastroenterol 19:118. https://doi.org/10.1186/s12876-019-1016-y
Lan L, Guo Q, Zhang Z, Zhao W, Yang X, Lu H, Zhou Z, Zhou X (2020) Classification of infected necrotizing pancreatitis for surgery within or beyond 4 weeks using machine learning. Front Bioeng Biotechnol 8:541. https://doi.org/10.3389/fbioe.2020.00541
Diao M, Li L, Li Q, Ye M, Cheng W (2014) Challenges and strategies for single-incision laparoscopic Roux-en-Y hepaticojejunostomy in managing giant choledochal cysts. Int J Surg 12:412–417. https://doi.org/10.1016/j.ijsu.2014.03.007
Wu S, Wu H, Xu G, Zhao Y, Xue F, Dong S, Han L, Wang Z, Wu Z (2022) Risk factors and clinical impacts of post-pancreatectomy acute pancreatitis after pancreaticoduodenectomy: a single-center retrospective analysis of 298 patients based on the ISGPS definition and grading system. Front Surg 9:916486. https://doi.org/10.3389/fsurg.2022.916486
Li SL, Zhang DR, Li YC, Li ZD, Niu AG (2000) Prevention and treatment for pancreatic duct injury during the excision of choledochal cyst. Chin J Pediatr Surg 21:211–213. https://doi.org/10.3760/cma.j.issn.0253-3006.2000.04.007
Czerwonko ME, Pekolj J, Uad P, Mazza O, Sanchez-Claria R, Arbues G, de Santibañes E, de Santibañes M, Palavecino M (2018) Acute pancreatitis after laparoscopic transcystic common bile duct exploration: an analysis of predisposing factors in 447 patients. World J Surg 42:3134–3142. https://doi.org/10.1007/s00268-018-4611-0
Acknowledgements
This work was partially supported by National Natural Science Foundation of China (No. 81971685), Scientific Research Project of Jiangsu Provincial Health Commission (No. ZD2022015), Science and Technology Development Project of Suzhou (SKY2022054), Suzhou Clinical Medical Center (SZLCYXZX202104), and Suzhou Key Discipline of Medicine (SZXK202105).
Funding
This work was supported by the National Natural Science Foundation of China, under Grant No. 81971685.
Author information
Authors and Affiliations
Contributions
WG Study conception and design. TC, YY and HM Data acquisition. SH, TC and WG Analysis and data interpretation. TC, HM, YY and SH Drafting of the manuscript. TC and WG Critical revision.
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cai, Tn., Huang, Sg., Yang, Y. et al. Prediction of post-operative acute pancreatitis in children with pancreaticobiliary maljunction using machine learning model. Pediatr Surg Int 39, 158 (2023). https://doi.org/10.1007/s00383-023-05441-x
Accepted:
Published:
DOI: https://doi.org/10.1007/s00383-023-05441-x